Author Interviews, Orthopedics, Surgical Research / 23.03.2020
Complication Rates Vary Between Hip Surgery Approaches
MedicalResearch.com Interview with:
[caption id="attachment_53608" align="alignleft" width="200"] Dr. Pincus[/caption]
Pincus MD PhD
Division of Orthopaedic Surgery, Department of Surgery
University of Toronto
Sunnybrook Health Sciences Centre, Division of Orthopaedic Surgery
ICES, Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: Controversy exists among arthroplasty surgeons and patients about the best surgical approach for total hip arthroplasty (THA) - one of the most common operations performed worldwide. In the last few years, the direct anterior approach has become increasingly popular compared to posterior and lateral approaches, partially as a result of advertising to patients. We sought to determine whether a direct anterior surgical approach was associated with lower surgical complications compared to lateral and posterior approaches.
Dr. Pincus[/caption]
Pincus MD PhD
Division of Orthopaedic Surgery, Department of Surgery
University of Toronto
Sunnybrook Health Sciences Centre, Division of Orthopaedic Surgery
ICES, Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: Controversy exists among arthroplasty surgeons and patients about the best surgical approach for total hip arthroplasty (THA) - one of the most common operations performed worldwide. In the last few years, the direct anterior approach has become increasingly popular compared to posterior and lateral approaches, partially as a result of advertising to patients. We sought to determine whether a direct anterior surgical approach was associated with lower surgical complications compared to lateral and posterior approaches.
 Dr. Pincus[/caption]
Pincus MD PhD
Division of Orthopaedic Surgery, Department of Surgery
University of Toronto
Sunnybrook Health Sciences Centre, Division of Orthopaedic Surgery
ICES, Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: Controversy exists among arthroplasty surgeons and patients about the best surgical approach for total hip arthroplasty (THA) - one of the most common operations performed worldwide. In the last few years, the direct anterior approach has become increasingly popular compared to posterior and lateral approaches, partially as a result of advertising to patients. We sought to determine whether a direct anterior surgical approach was associated with lower surgical complications compared to lateral and posterior approaches.
Dr. Pincus[/caption]
Pincus MD PhD
Division of Orthopaedic Surgery, Department of Surgery
University of Toronto
Sunnybrook Health Sciences Centre, Division of Orthopaedic Surgery
ICES, Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study?
Response: Controversy exists among arthroplasty surgeons and patients about the best surgical approach for total hip arthroplasty (THA) - one of the most common operations performed worldwide. In the last few years, the direct anterior approach has become increasingly popular compared to posterior and lateral approaches, partially as a result of advertising to patients. We sought to determine whether a direct anterior surgical approach was associated with lower surgical complications compared to lateral and posterior approaches.























 Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
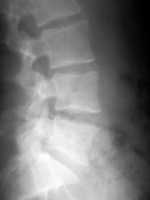
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.
Dr. Schneider[/caption]
Dr. Michael Schneider DC, PhD
Associate Professor
School of Health and Rehabilitation Sciences
University of Pittsburgh
MedicalResearch.com: What is the background for this study?
Response: Lumbar spinal stenosis (LSS) is one of the fastest growing problems in the country due to its aging population. One third of Medicare users have the condition, and it is the number one reason for spine surgery in this population. Existing research evaluates the benefits of nonsurgical treatment options compared to surgery, but there was no existing research that compared the available nonsurgical options to each other to determine the best course of treatment for each patient.
We studied three nonsurgical treatments for LSS: medical management with medications and/or epidural injections, individualized care with a physical therapist or chiropractor, and group exercise. We assessed each of these treatment methods with a questionnaire, a walking distance test, and a physical activity monitor.

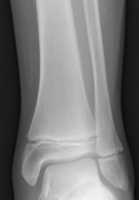
 Dr. Duren[/caption]
Dana L. Duren, PhD
Professor, Director of Orthopaedic Research
Director of Skeletal Morphology Laboratory
Thompson Laboratory for Regenerative Orthopaedics
Department of Orthopaedic Surgery
Missouri Orthopaedic Institute, University of Missouri
Columbia, MO 6521
MedicalResearch.com: What is the background for this study? What are the main findings?
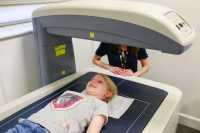
Response: The motivation for this study is the apparent accelerated maturity in children in the United States.
[caption id="attachment_46650" align="alignleft" width="139"]
Dr. Duren[/caption]
Dana L. Duren, PhD
Professor, Director of Orthopaedic Research
Director of Skeletal Morphology Laboratory
Thompson Laboratory for Regenerative Orthopaedics
Department of Orthopaedic Surgery
Missouri Orthopaedic Institute, University of Missouri
Columbia, MO 6521
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The motivation for this study is the apparent accelerated maturity in children in the United States.
[caption id="attachment_46650" align="alignleft" width="139"]