[caption id="attachment_73364" align="aligncenter" width="500"]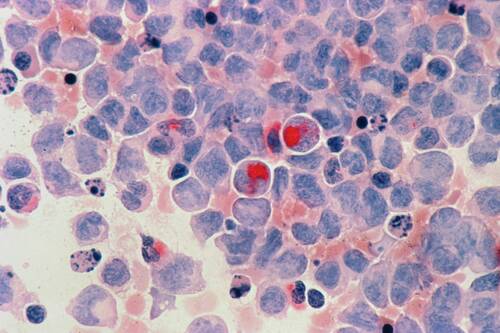 Source[/caption]
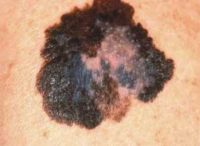
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
 Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.

 Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology
Dr. Koh[/caption]
Andrew Y. Koh, M.D.
Associate Professor, Pediatrics and Microbiology













![MedicalResearch.com Interview with: Cole Wayant Oklahoma State University Center for Health Sciences ‐ Analytical and Institutional Research Tulsa, OK MedicalResearch.com: What is the background for this study? What are the main findings? Response: New FDA-approved oncology drugs are essential to oncology practice. These drugs may immediately change clinical care by offering better treatments for common, lethal forms of cancer. But, new FDA-approved oncology drugs are expensive and have been shown to have variable efficacy. Given the importance of new FDA-approved oncology drugs to patients and physicians, the trials that underpin the FDA-approval of these drugs must be free from bias and transparent. Therefore, we investigated the financial relationships between oncologist-authors of clinical trials that underpin FDA-approvals. MedicalResearch.com: What should readers take away from your report? Response: The key takeaway from our study is that oncologist-authors often do not fully disclose their financial relationships with pharmaceutical companies. Financial disclosures are important for the reasons of transparency and trust between physicians and other stakeholders, such as patients. Disclosing conflicts of interest helps readers interpret the findings of a research study, especially given the fact that drug companies finance their own drug trials. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: In the future, beyond recommending that authors fully disclose all financial relationships with the sponsor of the trial, I recommend that journals use the Open Payments Database to verify the accuracy and completeness of author disclosure statements. Doing so is a small first step toward mitigating the potential for financial bias in the oncology literature.” Disclosures: I do not have anything else to add. None of the authors have conflicts of interest - financial or otherwise. Citation: Financial Conflicts of Interest Among Oncologist Authors of Reports of Clinical Drug Trials [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/Cole-Wayant.jpg)