From Clicks to Care: How Online Platforms Are Speeding Up Patient Service
Enhancing Patient Engagement Through Strategic Digital Integration
[caption id="attachment_61969" align="alignleft" width="200"] Photo from Pexels[/caption]
Photo from Pexels[/caption]
Leveraging SEO for Improved Patient Information Accessibility
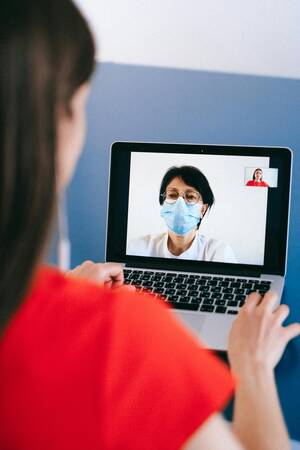
The strategic use of digital platforms in healthcare, particularly through search engine optimization (SEO), significantly enhances how medical practices engage with patients. SEO is crucial in making educational content easily discoverable online, thereby ensuring that when patients seek information about their conditions or potential treatments, the resources provided by advanced platforms like CheckedUp are readily available.Pre-Visit Patient Education via Optimized Content
Digital platforms not only facilitate direct patient education but also play a pivotal role in how this content is structured and presented online. By optimizing content for search engines, practices can ensure higher visibility and accessibility, allowing patients to obtain necessary medical knowledge before their consultations. This approach not only improves the efficiency of in-person visits but also empowers patients, making them proactive participants in their healthcare journey.US Healthcare Staffing Market to be Worth $26.97 Billion by 2031
The Rise in Demand for Healthcare Professionals
 The booming healthcare staffing market is driven by an increasing demand for medical practitioners. The US is grappling with a shortage of healthcare workers, including doctors, nurses, and allied health professionals - over 340,000 combined professionals are needed, including doctors and nurses. The issue is, that as more baby boomers retire, they often become more reliant on medical services, putting pressure on an already understaffed industry.
But the issue also is that the demand for healthcare staff isn't being met. The US and the UK both use overseas staff to fill the numbers. The people training to be nurses in the US are becoming travel nurses, aesthetic practitioners, and basically avoiding the main healthcare system. Well, not all of them, but a big chunk are. The US has no choice but to rely on outsourced agencies like physician staffing companies.
The booming healthcare staffing market is driven by an increasing demand for medical practitioners. The US is grappling with a shortage of healthcare workers, including doctors, nurses, and allied health professionals - over 340,000 combined professionals are needed, including doctors and nurses. The issue is, that as more baby boomers retire, they often become more reliant on medical services, putting pressure on an already understaffed industry.
But the issue also is that the demand for healthcare staff isn't being met. The US and the UK both use overseas staff to fill the numbers. The people training to be nurses in the US are becoming travel nurses, aesthetic practitioners, and basically avoiding the main healthcare system. Well, not all of them, but a big chunk are. The US has no choice but to rely on outsourced agencies like physician staffing companies.
How COVID-19 Has Changed Medical Research in Global Health
 COVID-19 is a virus that devastated the healthcare systems around the globe. The main reason for this devastation was the speed of the spreading. Because it was spreading so fast, hospitals weren’t able to accommodate so many patients.
We needed to figure out a better approach to dealing with the pandemic. So, this is where most of the people on Earth stood together by being apart. We were in lockdown, but our scientists and governments collaborated more on finding the right solution.
COVID-19 is a virus that devastated the healthcare systems around the globe. The main reason for this devastation was the speed of the spreading. Because it was spreading so fast, hospitals weren’t able to accommodate so many patients.
We needed to figure out a better approach to dealing with the pandemic. So, this is where most of the people on Earth stood together by being apart. We were in lockdown, but our scientists and governments collaborated more on finding the right solution.
What Was the COVID-19 Impact on Research Priorities?
One of the major impacts of the pandemic was the speed of research. Because of the urgency and the need for a quick response, research was focused on the COVID-19 virus and therapy and vaccine development for it. The development of vaccines was heavily prioritized, but this does not imply that it is not being done presently. Epidemiology and therapeutic regimens continue to see some initiatives. However, research remains a priority with ongoing trials on many things you can participate in (link to site). This required a lot of funding and resources, so governments, private sectors, and international organizations collaborated and helped out the research process. We’ve proven that we can adapt in no time, and respond to great threats effectively and swiftly.5 Reasons Why Pursuing Medical Administrative Credentials is Worthwhile
Working in the healthcare sector, even in an administrative capacity, allows you to make a meaningful impact on patient care...
DDW2024: SonarMD Program Reduced ER Visits and Health Care Costs for IBD Patients
 Dr. Kosinski[/caption]
Dr. Larry Kosinski, MD
Gastroenterologist and SonarMD Founder & Board Member
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by the IBD group of diseases?
Response: Affecting up to 70 million Americans, the U.S. spends $136 billion each year on digestive health as these conditions are complex to predict, treat and manage. Inflammatory Bowel Disease (IBD) includes people specifically diagnosed with either ulcerative colitis or Crohn’s disease, and these conditions require close monitoring to reduce the risk for complications that lead to lengthy hospital stays and significant medical spend. In addition to providing a holistic health program, the SonarMD digital platform risk stratifies patients and performs continuous symptom checks to identify deteriorating symptoms sooner and communicate changes to physicians, meaning that care teams can intervene faster to keep patients healthier and lower the overall cost of care.
The two large, longitudinal studies that we presented at Digestive Disease Week 2024 evaluated several major drivers of medical costs in people living with IBD and enrolled in the SonarMD end-to-end, digital care coordination program to determine if SonarMD’s program reduced healthcare utilization and concurrently produced better health outcomes. To assess this, we looked at Emergency Department visits and In-patient Admissions compared to risk-matched control groups.
Dr. Kosinski[/caption]
Dr. Larry Kosinski, MD
Gastroenterologist and SonarMD Founder & Board Member
MedicalResearch.com: What is the background for this study? Would you briefly explain what is meant by the IBD group of diseases?
Response: Affecting up to 70 million Americans, the U.S. spends $136 billion each year on digestive health as these conditions are complex to predict, treat and manage. Inflammatory Bowel Disease (IBD) includes people specifically diagnosed with either ulcerative colitis or Crohn’s disease, and these conditions require close monitoring to reduce the risk for complications that lead to lengthy hospital stays and significant medical spend. In addition to providing a holistic health program, the SonarMD digital platform risk stratifies patients and performs continuous symptom checks to identify deteriorating symptoms sooner and communicate changes to physicians, meaning that care teams can intervene faster to keep patients healthier and lower the overall cost of care.
The two large, longitudinal studies that we presented at Digestive Disease Week 2024 evaluated several major drivers of medical costs in people living with IBD and enrolled in the SonarMD end-to-end, digital care coordination program to determine if SonarMD’s program reduced healthcare utilization and concurrently produced better health outcomes. To assess this, we looked at Emergency Department visits and In-patient Admissions compared to risk-matched control groups.
Ongoing education is the backbone of a robust safety culture. Regular safety training sessions ensure that all employees are up-to-date...
Leading with Empathy in the Healthcare Sector
The Impact of Technological Advancements
 As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing HR challenges in behavioral health. Understanding the unique nature of these challenges, and the emotional toll they can take on staff, is crucial for leaders who strive to create a supportive work environment. This deeper understanding can drive the implementation of effective solutions, fostering a workplace where empathy and professionalism thrive together.
As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing HR challenges in behavioral health. Understanding the unique nature of these challenges, and the emotional toll they can take on staff, is crucial for leaders who strive to create a supportive work environment. This deeper understanding can drive the implementation of effective solutions, fostering a workplace where empathy and professionalism thrive together.
UCLA Study Finds Patients Treated By Female Physicians Have Better Outcomes and Fewer Readmissions
 Dr. Tsugawa[/caption]
Yusuke Tsugawa, MD, PhD
Associate Professor of Medicine & Health Policy and Management, UCLA
Director of Data Core, UCLA Department of Medicine Statistics Core
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: Prior studies have found that female and male physicians practice medicine differently. For example, female physicians are, on average, more likely to abide by clinical guidelines and spend more time listening to patients. However, evidence was limited as to whether such differences have clinically meaningful impact on patients’ health outcomes, which was the aim of this study.
Dr. Tsugawa[/caption]
Yusuke Tsugawa, MD, PhD
Associate Professor of Medicine & Health Policy and Management, UCLA
Director of Data Core, UCLA Department of Medicine Statistics Core
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA 90024
MedicalResearch.com: What is the background for this study?
Response: Prior studies have found that female and male physicians practice medicine differently. For example, female physicians are, on average, more likely to abide by clinical guidelines and spend more time listening to patients. However, evidence was limited as to whether such differences have clinically meaningful impact on patients’ health outcomes, which was the aim of this study.
 When you visit your doctor, you expect to receive accurate diagnoses and appropriate treatment. However, medical professionals can sometimes make mistakes that have serious consequences for patients. If you believe you have been the victim of a misdiagnosis in Virginia, you may be wondering about your legal options. Can you sue your doctor for a wrong diagnosis?
Consider the hypothetical case of Sarah, a hardworking professional plagued by persistent fatigue and headaches. After a series of tests with ambiguous results, her physician diagnoses her with chronic fatigue syndrome. Feeling a sense of relief at finally having an answer, Sarah diligently follows the recommended treatment plan and makes significant lifestyle changes. Despite her efforts, her health continues to deteriorate. Seeking a second opinion, Sarah discovers that she actually has a tumor which, while treatable, has gone undetected and caused substantial harm. Sarah's story illustrates the potentially devastating impact of a misdiagnosis, leaving her with both emotional trauma and severe medical issues.
When you visit your doctor, you expect to receive accurate diagnoses and appropriate treatment. However, medical professionals can sometimes make mistakes that have serious consequences for patients. If you believe you have been the victim of a misdiagnosis in Virginia, you may be wondering about your legal options. Can you sue your doctor for a wrong diagnosis?
Consider the hypothetical case of Sarah, a hardworking professional plagued by persistent fatigue and headaches. After a series of tests with ambiguous results, her physician diagnoses her with chronic fatigue syndrome. Feeling a sense of relief at finally having an answer, Sarah diligently follows the recommended treatment plan and makes significant lifestyle changes. Despite her efforts, her health continues to deteriorate. Seeking a second opinion, Sarah discovers that she actually has a tumor which, while treatable, has gone undetected and caused substantial harm. Sarah's story illustrates the potentially devastating impact of a misdiagnosis, leaving her with both emotional trauma and severe medical issues.
Enhancing Accuracy and Precision
 Skilled medical scribing entails meticulous transcription of patient encounters, procedures, or treatment plans from spoken word into written text, capturing every detail and nuance. Transcription is a pivotal tool for ensuring that the physician follows the proper procedure and that medical records, reports, and documentation have perfect levels of accuracy.
Medical scribing is a skilled profession that requires solid knowledge of the worker's chosen healthcare field. Any misinterpretation of patient information has the potential to lead to ill-informed future decisions regarding a patient's health.
Healthcare organisations must also adhere to strict guidelines regarding the documentation of patient care, billing processes, and confidentiality protocols. Skilled medical scribes with specialised knowledge and expertise in their industry can protect organisations from costly lawsuits and ensure that patients are treated with the correct level of integrity.
In today's world, time is money. Successful medical scribes improve efficiency and take the burden off physicians having to personally record data, enabling them to see more patients and listen more attentively, ultimately contributing to reaching the healthcare company's overall productivity and financial aims.
One study found that medical scribes cut costs by $31.15 per hour, with no risk added risk to patient safety.
Skilled medical scribing entails meticulous transcription of patient encounters, procedures, or treatment plans from spoken word into written text, capturing every detail and nuance. Transcription is a pivotal tool for ensuring that the physician follows the proper procedure and that medical records, reports, and documentation have perfect levels of accuracy.
Medical scribing is a skilled profession that requires solid knowledge of the worker's chosen healthcare field. Any misinterpretation of patient information has the potential to lead to ill-informed future decisions regarding a patient's health.
Healthcare organisations must also adhere to strict guidelines regarding the documentation of patient care, billing processes, and confidentiality protocols. Skilled medical scribes with specialised knowledge and expertise in their industry can protect organisations from costly lawsuits and ensure that patients are treated with the correct level of integrity.
In today's world, time is money. Successful medical scribes improve efficiency and take the burden off physicians having to personally record data, enabling them to see more patients and listen more attentively, ultimately contributing to reaching the healthcare company's overall productivity and financial aims.
One study found that medical scribes cut costs by $31.15 per hour, with no risk added risk to patient safety.
Remote Patient Monitoring for Effective Heart Disease Management
Quality Care Revolutionaries
 The seminal Institute of Medicine's “To Err Is Human” publication sounded alarms in 1999 about the silent epidemic of American medical errors contributing to nearly 98,000 annual deaths. With time, the stakes intensified for systemic improvement. Nurse leadership emerged, accelerating cultural transformations and pioneering processes that saved countless lives.
Take Children’s Hospital Solutions for Patient Safety Network (SPS), for example. Founded by nurse scientist Marlene Miller in 2001, it aims to unite children’s hospitals to develop evidence-based harm reduction tactics and tools.
By adopting the best practices across their network, their hospitals are making significant strides in preventing serious harm. As of November 2023, this nationwide network of child healthcare has spared over 25,000 children from harm, resulting in an estimated cost savings of $500 million.
Similarly, medical experts around the world credit ICU nurses’ relentless systems analysis and testing of solutions during the COVID-19 pandemic for lifting outcomes.
The seminal Institute of Medicine's “To Err Is Human” publication sounded alarms in 1999 about the silent epidemic of American medical errors contributing to nearly 98,000 annual deaths. With time, the stakes intensified for systemic improvement. Nurse leadership emerged, accelerating cultural transformations and pioneering processes that saved countless lives.
Take Children’s Hospital Solutions for Patient Safety Network (SPS), for example. Founded by nurse scientist Marlene Miller in 2001, it aims to unite children’s hospitals to develop evidence-based harm reduction tactics and tools.
By adopting the best practices across their network, their hospitals are making significant strides in preventing serious harm. As of November 2023, this nationwide network of child healthcare has spared over 25,000 children from harm, resulting in an estimated cost savings of $500 million.
Similarly, medical experts around the world credit ICU nurses’ relentless systems analysis and testing of solutions during the COVID-19 pandemic for lifting outcomes.
New study finding $14.2 million in undisclosed conflicts of interest in the “bible” of psychiatry (DSM-5-TR) published in the British Medical Journal
 Lauren C. Davis, MBS
Department of Medical Education
Geisinger Commonwealth School of Medicine
Scranton, PA 19409
MedicalResearch.com: What is the background for this study?
Response: Financial conflicts of interest (COIs) resulting from ties between academia and industry have been under scrutiny for their potential to hinder the integrity of medical research. COIs can lead to implicit bias, compromise the research process, and erode public trust (1-6). The American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM), standardizes symptom criteria and codifies psychiatric disorders. This manual contributes to the approval of new drugs, extensions of patent exclusivity, and can influence payers and mental health professionals seeking third-party reimbursements. Given the implications of the DSM on public health, it is paramount that it is free of industry influence. Previous research has shown a high prevalence of industry ties among panel and task force members of the DSM-IV-TR and DSM-5, despite the implementation of a disclosure policy for the DSM-5 (7,8). This study (9) determined the extent and type of COIs received by panel and task-force members of the DSM-5-TR (2022) (10). As the DSM-5-TR did not disclose COI, we used the Center for Medicare and Medicaid Services Open Payments (OP) database (11) to quantify them.
Lauren C. Davis, MBS
Department of Medical Education
Geisinger Commonwealth School of Medicine
Scranton, PA 19409
MedicalResearch.com: What is the background for this study?
Response: Financial conflicts of interest (COIs) resulting from ties between academia and industry have been under scrutiny for their potential to hinder the integrity of medical research. COIs can lead to implicit bias, compromise the research process, and erode public trust (1-6). The American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM), standardizes symptom criteria and codifies psychiatric disorders. This manual contributes to the approval of new drugs, extensions of patent exclusivity, and can influence payers and mental health professionals seeking third-party reimbursements. Given the implications of the DSM on public health, it is paramount that it is free of industry influence. Previous research has shown a high prevalence of industry ties among panel and task force members of the DSM-IV-TR and DSM-5, despite the implementation of a disclosure policy for the DSM-5 (7,8). This study (9) determined the extent and type of COIs received by panel and task-force members of the DSM-5-TR (2022) (10). As the DSM-5-TR did not disclose COI, we used the Center for Medicare and Medicaid Services Open Payments (OP) database (11) to quantify them.
AI Has Ability To Speed Up Medical Literature Searches, But Not All Information Reliable
Pharmacy Forecast: Paradigm Shifts in Breakthrough Therapeutics Will Challenge Existing Payment Models
 Dr. DiPiro[/caption]
Joseph T. DiPiro, Pharm.D
Associate Vice President, Faculty Affairs
Virginia Commonwealth University
Dr. DiPiro is an editor for Pharmacotherapy: A Pathophysiologic Approach
MedicalResearch.com: What is the background for this study?
Response: The ASHP/ASHP Foundation Pharmacy Forecast Report is constructed from a survey of health-system pharmacy leaders who were asked to rate the likelihood of events, scenarios, and trends occurring in the next five years. The purpose is for health-system pharmacists and pharmacy leaders to inform their strategic planning efforts. The Pharmacy Forecast is not intended to predict future events. Rather, the report is intended to be a provocative stimulant for the thinking, discussion, and planning that must take place in every health system. Leaders must be informed of potential developments to help position their organizations to care for patients, enhance population health, and improve medication outcomes.
Dr. DiPiro[/caption]
Joseph T. DiPiro, Pharm.D
Associate Vice President, Faculty Affairs
Virginia Commonwealth University
Dr. DiPiro is an editor for Pharmacotherapy: A Pathophysiologic Approach
MedicalResearch.com: What is the background for this study?
Response: The ASHP/ASHP Foundation Pharmacy Forecast Report is constructed from a survey of health-system pharmacy leaders who were asked to rate the likelihood of events, scenarios, and trends occurring in the next five years. The purpose is for health-system pharmacists and pharmacy leaders to inform their strategic planning efforts. The Pharmacy Forecast is not intended to predict future events. Rather, the report is intended to be a provocative stimulant for the thinking, discussion, and planning that must take place in every health system. Leaders must be informed of potential developments to help position their organizations to care for patients, enhance population health, and improve medication outcomes.
New Alzheimer Drug Lecanemab and its Ancillary Services Could Cost Medicare up to 5 billion Annually
 Julia Cave Arbanas[/caption]
Julia Cave Arbanas
Project Manager and
Julia Cave Arbanas[/caption]
Julia Cave Arbanas
Project Manager and
 John N. Mafi, MD, MPH
Associate Professor of Medicine
General Internal Medicine & Health Services Research
David Geffen School of Medicine at UCLA
MedicalResearch.com: What is the background for this study? What is lecanemab used for and how well does it work?
Response: Lecanemab is a treatment for mild cognitive impairment and mild dementia that was approved in January 2023 as part of the Food and Drug Administration’s (FDA) accelerated approval program. The results from a recent phase 3 clinical trial show a modest clinical benefit: the rate of cognitive decline by 27% in an 18-month study involving participants experiencing the early stage of Alzheimer’s, with an 0.45-point absolute difference in cognitive testing scores. However, due to the risk of brain swelling and bleeding (also known as amyloid-related imaging abnormalities), treatment with lecanemab involves frequent MRIs and neurology or geriatrics appointments to monitor for these abnormalities, which can be life threatening. So far, three patient deaths have potentially been tied to lecanemab.
It is likely that the FDA will grant is lecanemab traditional approval later this year, prompting Medicare to reconsider its current coverage restrictions and potentially enabling widespread use.
John N. Mafi, MD, MPH
Associate Professor of Medicine
General Internal Medicine & Health Services Research
David Geffen School of Medicine at UCLA
MedicalResearch.com: What is the background for this study? What is lecanemab used for and how well does it work?
Response: Lecanemab is a treatment for mild cognitive impairment and mild dementia that was approved in January 2023 as part of the Food and Drug Administration’s (FDA) accelerated approval program. The results from a recent phase 3 clinical trial show a modest clinical benefit: the rate of cognitive decline by 27% in an 18-month study involving participants experiencing the early stage of Alzheimer’s, with an 0.45-point absolute difference in cognitive testing scores. However, due to the risk of brain swelling and bleeding (also known as amyloid-related imaging abnormalities), treatment with lecanemab involves frequent MRIs and neurology or geriatrics appointments to monitor for these abnormalities, which can be life threatening. So far, three patient deaths have potentially been tied to lecanemab.
It is likely that the FDA will grant is lecanemab traditional approval later this year, prompting Medicare to reconsider its current coverage restrictions and potentially enabling widespread use.
Disparity and Diversity in Non-Small Cell Lung Cancer Imaging and Genomics
 Dr. Kohan[/caption]
Andres Kohan MD
MHSc. in Translational Research
Joint Department of Medical Imaging
University Health Network
Mount Sinai Hospital and Women's College Hospital
University of Toronto
Toronto, Canada
MedicalResearch.com: What is the background for this study?
Response: Inequalities in access to healthcare for oncologic patients and its impact on quality of life and survival have been previously described. However, there also exists reports pointing out that when factors contributing to socioeconomic inequality are accounted for differences in outcome between races remain identifiable.
In this context, we sought to evaluate the presence of disparities in imaging in a selected population of patients with non-small cell lung cancer (NSCLC) within AACRs Project GENIE Biopharma Consortium (BPC) dataset v 1.1. This database is the largest in existence that has not only the patients’ imaging and clinical staging/follow-up, but also the genetic profile of the patients’ tumors.
Dr. Kohan[/caption]
Andres Kohan MD
MHSc. in Translational Research
Joint Department of Medical Imaging
University Health Network
Mount Sinai Hospital and Women's College Hospital
University of Toronto
Toronto, Canada
MedicalResearch.com: What is the background for this study?
Response: Inequalities in access to healthcare for oncologic patients and its impact on quality of life and survival have been previously described. However, there also exists reports pointing out that when factors contributing to socioeconomic inequality are accounted for differences in outcome between races remain identifiable.
In this context, we sought to evaluate the presence of disparities in imaging in a selected population of patients with non-small cell lung cancer (NSCLC) within AACRs Project GENIE Biopharma Consortium (BPC) dataset v 1.1. This database is the largest in existence that has not only the patients’ imaging and clinical staging/follow-up, but also the genetic profile of the patients’ tumors.
ChatGPT Provided Surprising Empathetic Answers to Patient Queries
ACC23: Encouraging Findings on Mortality After Acute Heart Attack
 Dr. Ditah Chobufo[/caption]
Dr. Muchi Ditah Chobufo MD MPH
Cardiology Fellow
West Virginia University
MedicalResearch.com: What is the background for this study?
Response: Ischemic heart diseases are a significant cause of morbidity and mortality in the USA. Also, there exists alarming ethnic disparities in mortality rates following acute myocardial infarction. To this effect, significant efforts have been deployed over the years to curb its burden and reduce extant disparities. It is in this light that we set out to analyze general and ethnic specific trends in acute myocardial infarction related age adjusted mortality rates (AAMR) in the entire USA from 1999-2020.
Dr. Ditah Chobufo[/caption]
Dr. Muchi Ditah Chobufo MD MPH
Cardiology Fellow
West Virginia University
MedicalResearch.com: What is the background for this study?
Response: Ischemic heart diseases are a significant cause of morbidity and mortality in the USA. Also, there exists alarming ethnic disparities in mortality rates following acute myocardial infarction. To this effect, significant efforts have been deployed over the years to curb its burden and reduce extant disparities. It is in this light that we set out to analyze general and ethnic specific trends in acute myocardial infarction related age adjusted mortality rates (AAMR) in the entire USA from 1999-2020. Patients Associate Green Scrub Color With Surgeons
 Casey Hribar[/caption]
Casey Hribar
Fourth-year medical student
University of North Carolina
MedicalResearch.com: What is the background for this study?
Response: Several great pieces of literature already exist about patient perception of doctors wearing white coats, formal attire, business attire, and the like. But recently, scrubs are garnering favor, especially as a result of the COVID-19 pandemic.
While there has been some interest in what is worn over scrubs (jackets, vests, name tags, etc.), to our knowledge, there has not been any investigation into scrub color. Scrubs are a highly variable article of clothing, from fit, to pockets, pattern, and color, and it makes sense that these variations could have their own associated perceptions. Our study served as a way to open up the conversation around scrubs and the potential impact of their color on patients.
Casey Hribar[/caption]
Casey Hribar
Fourth-year medical student
University of North Carolina
MedicalResearch.com: What is the background for this study?
Response: Several great pieces of literature already exist about patient perception of doctors wearing white coats, formal attire, business attire, and the like. But recently, scrubs are garnering favor, especially as a result of the COVID-19 pandemic.
While there has been some interest in what is worn over scrubs (jackets, vests, name tags, etc.), to our knowledge, there has not been any investigation into scrub color. Scrubs are a highly variable article of clothing, from fit, to pockets, pattern, and color, and it makes sense that these variations could have their own associated perceptions. Our study served as a way to open up the conversation around scrubs and the potential impact of their color on patients.
Physician Weekly Work Hours Fall Especially for Doctor Fathers
 Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
Dr. Goldman[/caption]
Anna L. Goldman, M.D., M.P.A., M.P.H
Assistant Professor of Medicine
General Internal Medicine
Boston University Chobanian & Avedisian School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Experts on the healthcare labor market have long debated the existence and magnitude of a physician shortage. Physician work hours are a major contributor to physician supply issues, but little research is available on recent trends in work hours by physicians. In addition, no available studies have rigorously estimated changes in the physician workforce size during the pandemic.
Non-Clinical Medical Careers are Soaring: Here is What You Need to Know
Healthcare is one of the largest industries in the country, and it is also outpacing other industries in terms of...
Covid: Safety Net Hospitals Experienced Greater Financial Losses During Pandemic
Allison Witman PhD Assistant Professor of Economics Economics & Finance Cameron School of Business University of North Carolina, Wilmington
Yu Wang PhD Assistant Professor Congdon School of Supply Chain, Business Analytics, & Information Systems Cameron School of Business University of North Carolina Wilmington David Cho PhD Assistant Professor of Management California State University, Fullerton
MedicalResearch.com: What is the background for this study? Response: The COVID-19 pandemic placed tremendous financial pressure on hospitals. Beginning in March of 2020, hospitals cancelled outpatient and elective procedures to accommodate surges in demand from COVID-19 patients. As these procedures account for more than 60% of an average hospital’s revenue, cancellation posed serious challenges to the financial health of hospitals. Revenue from COVID-19 patients may have partially offset these effects, but the American Hospital Association estimated a total loss of $202.6 billion by American hospitals between March and June 2020. In response, the U.S. government created large federal assistance programs aimed to stabilize hospitals’ financial situation as their ability to maintain operations was critical to the health of the nation. Due to differences in hospital characteristics, certain hospitals such as rural hospitals and those serving a higher share of Medicaid and uninsured patients (e.g., safety net hospitals) may have been more financially susceptible to the effects of the pandemic. These hospitals that serve vulnerable patient populations historically have had lower profit margins and were candidates for targeted COVID relief funding (e.g., Safety Net Hospitals Payments, a $10 billion component of the Provider Relief Fund).Private Equity and Health Care: More Patients, More Charges
 Dr. Zhu[/caption]
Jane M. Zhu, M.D., M.P.P., M.S.H.P.
Assistant Professor of Medicine
Division of General Internal Medicine and Geriatrics
School of Medicine
Oregon Health & Science University
Portland, Oregon
MedicalResearch.com: What is the background for this study?
Response: Private equity (PE) acquisitions of physician practices are accelerating across many specialties, but there is still little robust evidence on the effects of these acquisitions. Concerns about PE involvement is predicated on the fact that these firms expect high annual returns, which require either reducing costs or increasing revenue, or both. Using PE acquisition data from 2016-2020, linked to commercial claims data, we sought to understand what common mechanisms of revenue generation were being adopted after private equity acquisition of physician practices.
Dr. Zhu[/caption]
Jane M. Zhu, M.D., M.P.P., M.S.H.P.
Assistant Professor of Medicine
Division of General Internal Medicine and Geriatrics
School of Medicine
Oregon Health & Science University
Portland, Oregon
MedicalResearch.com: What is the background for this study?
Response: Private equity (PE) acquisitions of physician practices are accelerating across many specialties, but there is still little robust evidence on the effects of these acquisitions. Concerns about PE involvement is predicated on the fact that these firms expect high annual returns, which require either reducing costs or increasing revenue, or both. Using PE acquisition data from 2016-2020, linked to commercial claims data, we sought to understand what common mechanisms of revenue generation were being adopted after private equity acquisition of physician practices.
Financially Distressed Hospitals Found to Benefit from System Affiliation
 Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.
Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.
Geisinger Study Found 79 Physician Contributors to UpToDate and DynaMed with Potential Conflicts of Interest of Nearly $8 Million
 SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
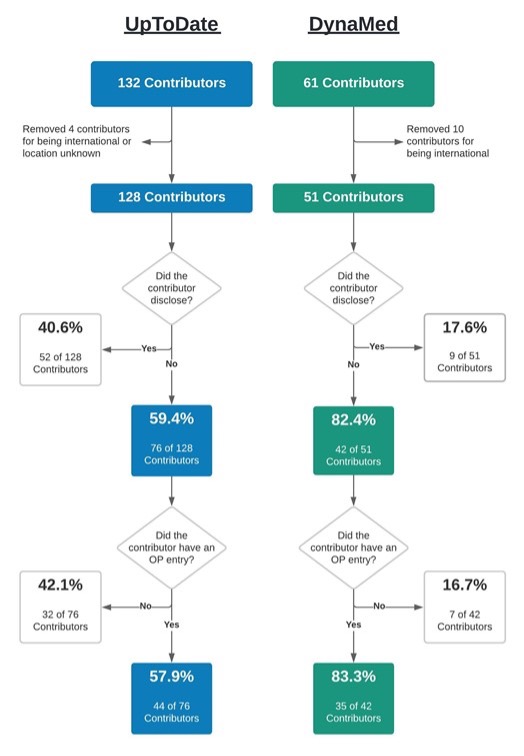
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
Expensive New Drugs Often Provide Little Substantial Benefit Over Existing Medications
 Dr. Rome[/caption]
Benjamin N. Rome MD
Instructor, Harvard Medical School
Internal Medicine
Division of Pharmacoepidemiology and Pharmacoeconomics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
What are the main findings?
Response: Manufacturers of brand-name drugs are granted periods, free from direct competition, during which they can set and raise prices as they choose.
We found that the prices for newly marketed brand-name drugs increased by 20% per year from 2008 to 2021. In 2020 and 2021, nearly half of new drugs were launched at a price greater than $150,000 per year, compared with 9% of drugs in 2008-2013. These dramatic trends are only partly explained by changes in the types of drugs coming to market.
Dr. Rome[/caption]
Benjamin N. Rome MD
Instructor, Harvard Medical School
Internal Medicine
Division of Pharmacoepidemiology and Pharmacoeconomics
Brigham and Women’s Hospital
MedicalResearch.com: What is the background for this study?
What are the main findings?
Response: Manufacturers of brand-name drugs are granted periods, free from direct competition, during which they can set and raise prices as they choose.
We found that the prices for newly marketed brand-name drugs increased by 20% per year from 2008 to 2021. In 2020 and 2021, nearly half of new drugs were launched at a price greater than $150,000 per year, compared with 9% of drugs in 2008-2013. These dramatic trends are only partly explained by changes in the types of drugs coming to market.