Author Interviews, Gout, JAMA, Kidney Disease / 06.06.2022
Study Evaluates Association of Uric Acid Lowering Medications with Chronic Kidney Disease
MedicalResearch.com Interview with:
[caption id="attachment_16840" align="alignleft" width="124"] Dr. .Kovesdy[/caption]
Csaba P Kovesdy MD FASN
Fred Hatch Professor of Medicine
Director, Clinical Outcomes and Clinical Trials Program
Division of Nephrology, University of Tennessee Health Science Center
Nephrology Section Chief, Memphis VA Medical Center
Memphis TN, 38163
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Hyperuricemia has unfavorable metabolic effects and has been associated with higher risk of progressive kidney disease and mortality. Despite this, earlier clinical trials have failed to prove a beneficial impact on kidney disease progression from uric acid lowering therapy in patients with preexisting CKD.
The effect of uric acid lowering therapy on the development of new onset CKD in patients with normal kidney function has not been well studied. In our large observational study we did not find a beneficial association between newly initiated uric acid lowering therapy (the majority of which was in the form of allopurinol).
On the contrary, uric acid lowering therapy was associated with a slightly higher risk of new onset low eGFR and new onset albuminuria, especially in patients with less elevated baseline serum acid levels.
Dr. .Kovesdy[/caption]
Csaba P Kovesdy MD FASN
Fred Hatch Professor of Medicine
Director, Clinical Outcomes and Clinical Trials Program
Division of Nephrology, University of Tennessee Health Science Center
Nephrology Section Chief, Memphis VA Medical Center
Memphis TN, 38163
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Hyperuricemia has unfavorable metabolic effects and has been associated with higher risk of progressive kidney disease and mortality. Despite this, earlier clinical trials have failed to prove a beneficial impact on kidney disease progression from uric acid lowering therapy in patients with preexisting CKD.
The effect of uric acid lowering therapy on the development of new onset CKD in patients with normal kidney function has not been well studied. In our large observational study we did not find a beneficial association between newly initiated uric acid lowering therapy (the majority of which was in the form of allopurinol).
On the contrary, uric acid lowering therapy was associated with a slightly higher risk of new onset low eGFR and new onset albuminuria, especially in patients with less elevated baseline serum acid levels.
 Dr. .Kovesdy[/caption]
Csaba P Kovesdy MD FASN
Fred Hatch Professor of Medicine
Director, Clinical Outcomes and Clinical Trials Program
Division of Nephrology, University of Tennessee Health Science Center
Nephrology Section Chief, Memphis VA Medical Center
Memphis TN, 38163
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Hyperuricemia has unfavorable metabolic effects and has been associated with higher risk of progressive kidney disease and mortality. Despite this, earlier clinical trials have failed to prove a beneficial impact on kidney disease progression from uric acid lowering therapy in patients with preexisting CKD.
The effect of uric acid lowering therapy on the development of new onset CKD in patients with normal kidney function has not been well studied. In our large observational study we did not find a beneficial association between newly initiated uric acid lowering therapy (the majority of which was in the form of allopurinol).
On the contrary, uric acid lowering therapy was associated with a slightly higher risk of new onset low eGFR and new onset albuminuria, especially in patients with less elevated baseline serum acid levels.
Dr. .Kovesdy[/caption]
Csaba P Kovesdy MD FASN
Fred Hatch Professor of Medicine
Director, Clinical Outcomes and Clinical Trials Program
Division of Nephrology, University of Tennessee Health Science Center
Nephrology Section Chief, Memphis VA Medical Center
Memphis TN, 38163
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Hyperuricemia has unfavorable metabolic effects and has been associated with higher risk of progressive kidney disease and mortality. Despite this, earlier clinical trials have failed to prove a beneficial impact on kidney disease progression from uric acid lowering therapy in patients with preexisting CKD.
The effect of uric acid lowering therapy on the development of new onset CKD in patients with normal kidney function has not been well studied. In our large observational study we did not find a beneficial association between newly initiated uric acid lowering therapy (the majority of which was in the form of allopurinol).
On the contrary, uric acid lowering therapy was associated with a slightly higher risk of new onset low eGFR and new onset albuminuria, especially in patients with less elevated baseline serum acid levels.


 Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace.
Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace. 
 Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000.
Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000. 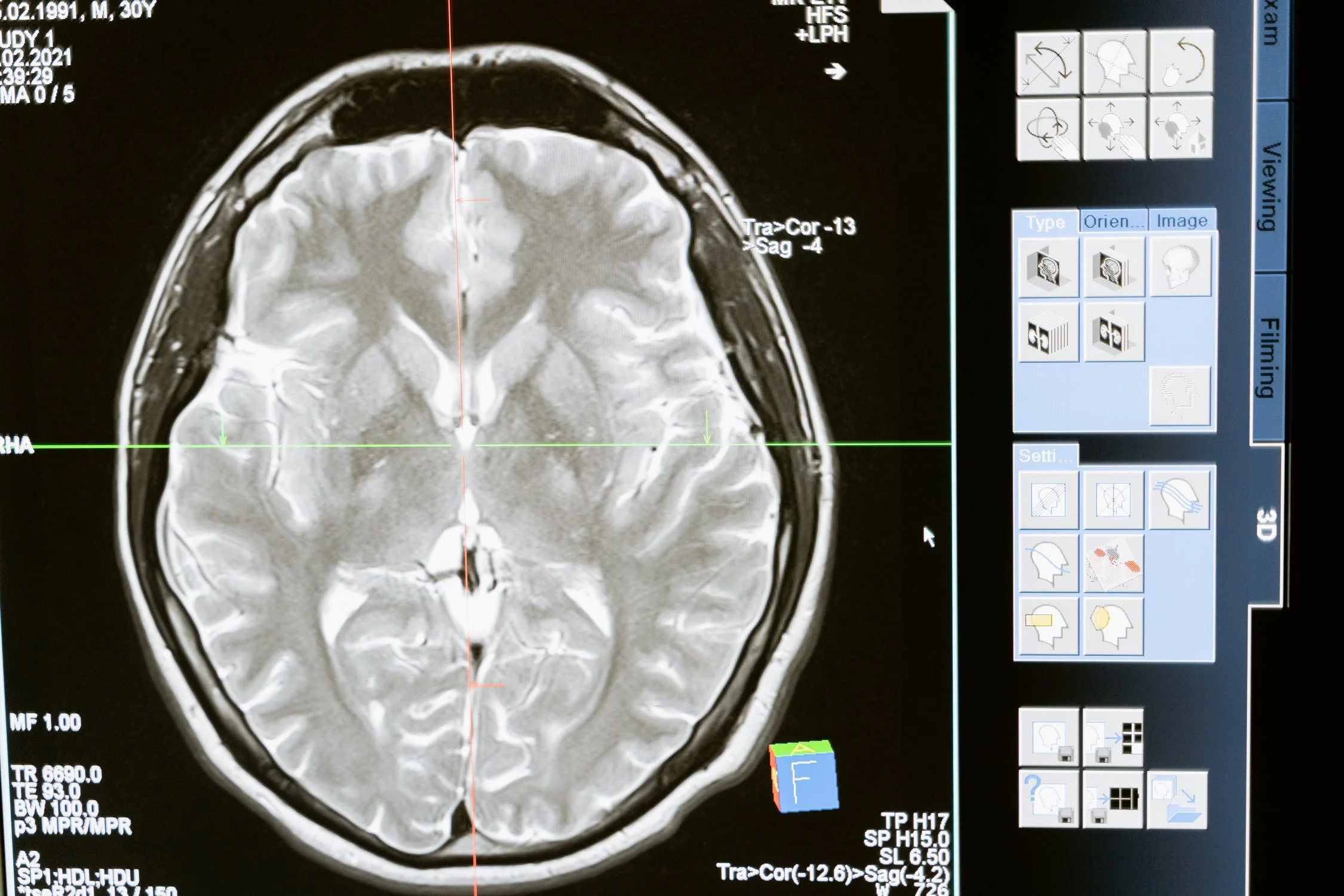

 Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.
Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.

 Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
 Dr. Wong[/caption]
Susan P. Y. Wong, MD MS
Assistant Professor
Division of Nephrology
University of Washington
VA Puget Sound Health Care System
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Very little is known about the care and outcomes of patients who reach the end stages of kidney disease and do not pursue dialysis. We conducted a systematic review of longitudinal studies on patients with advanced kidney disease who forgo dialysis to determine their long-term outcomes.
We found that many patients survived several years and experienced sustained quality of life until late in the illness course. However, use of acute care services was common and there was a high degree of variability in access to supportive care services near the end of life.
Dr. Wong[/caption]
Susan P. Y. Wong, MD MS
Assistant Professor
Division of Nephrology
University of Washington
VA Puget Sound Health Care System
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Very little is known about the care and outcomes of patients who reach the end stages of kidney disease and do not pursue dialysis. We conducted a systematic review of longitudinal studies on patients with advanced kidney disease who forgo dialysis to determine their long-term outcomes.
We found that many patients survived several years and experienced sustained quality of life until late in the illness course. However, use of acute care services was common and there was a high degree of variability in access to supportive care services near the end of life.


 Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.
Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.


 Dr. Thakrar[/caption]
Ashish Thakrar, MD
Internal Medicine & Addiction Medicine
National Clinician Scholars Program
University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: About 1.8 million Americans are currently incarcerated, more than any other country in the world per capita. Of those 1.8 million, about 1 in 7 suffers from opioid addiction, putting them at high risk of overdose and death, particularly in the weeks following release.
Opioid use disorder is a treatable condition, particularly with the medications buprenorphine or methadone, but historically, prisons and jails have not offered treatment. Over the past five years, a few states and municipalities have enacted policies to provide access for OUD treatment. We examined whether these policies were actually improving access to treatment.
Dr. Thakrar[/caption]
Ashish Thakrar, MD
Internal Medicine & Addiction Medicine
National Clinician Scholars Program
University of Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: About 1.8 million Americans are currently incarcerated, more than any other country in the world per capita. Of those 1.8 million, about 1 in 7 suffers from opioid addiction, putting them at high risk of overdose and death, particularly in the weeks following release.
Opioid use disorder is a treatable condition, particularly with the medications buprenorphine or methadone, but historically, prisons and jails have not offered treatment. Over the past five years, a few states and municipalities have enacted policies to provide access for OUD treatment. We examined whether these policies were actually improving access to treatment. 
 Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.




 Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.
Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.

 Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.
Dr. Pierce[/caption]
John Pierce, PhD
Professor Emeritus
Department of Family Medicine and Public Health
Moores Cancer Center Director for Population Sciences
Co-leader of the Cancer Prevention program
UC San Diego
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Graphic Warning Labels are to be implemented in the US in July 2022, depending on litigation. This will be about 10 years after they were first proposed. Meanwhile, 120 other countries have implemented them already.
The FDA states that their purpose for the warnings is to provide a constant reminder to smokers about the health consequences of smoking, not to force them to quit.
In our study, 3 months of having cigarettes repackaged into graphic warning packs was associated with smokers thinking more about quitting and not getting as much pleasure out of their cigarettes. However, thinking about quitting is only the first step to conquering a nicotine addiction.


 Dr. Strauss[/caption]
David Strauss, MD, PhD
Director, Division of Applied Regulatory Science
[caption id="attachment_57763" align="alignleft" width="150"]
Dr. Strauss[/caption]
David Strauss, MD, PhD
Director, Division of Applied Regulatory Science
[caption id="attachment_57763" align="alignleft" width="150"] Dr. Keire[/caption]
David Keire, PhD
Director, Office of Testing and Research
U.S. Food and Drug Administration
Center for Drug Evaluation and Research
MedicalResearch.com: What is the background for this study?
Response: In 2019, the US Food and Drug Administration (FDA) received a citizen petition indicating that ranitidine, a widely used prescription and over-the-counter drug, contained the probable human carcinogen N-nitrosodimethylamine (NDMA). In addition, the petitioner proposed that ranitidine could convert to NDMA in humans; however, this was based on a small clinical study with limitations and an in vitro study that included high level of supplemental nitrite. In response, the FDA immediately alerted the public and began an investigation.
The FDA’s initial research found that the procedures previously used to quantify NDMA were not appropriate for assessing its presence in ranitidine, owing to the use of high temperatures that could convert ranitidine to NDMA during that analysis. New lower-temperature analytical methods found that the amounts of NDMA contained in ranitidine products were 3,000-fold lower than those reported in the citizen petition; however, these lower amounts of NDMA were still above the FDA-acceptable level and could increase over time, prompting the FDA to request the market withdrawal of ranitidine products.
The FDA noted, however, that if ranitidine products could be manufactured to control NDMA amounts, they could be allowed back on the market—but additional information would first be needed to understand whether NDMA could form in vivo from ranitidine in humans.
Dr. Keire[/caption]
David Keire, PhD
Director, Office of Testing and Research
U.S. Food and Drug Administration
Center for Drug Evaluation and Research
MedicalResearch.com: What is the background for this study?
Response: In 2019, the US Food and Drug Administration (FDA) received a citizen petition indicating that ranitidine, a widely used prescription and over-the-counter drug, contained the probable human carcinogen N-nitrosodimethylamine (NDMA). In addition, the petitioner proposed that ranitidine could convert to NDMA in humans; however, this was based on a small clinical study with limitations and an in vitro study that included high level of supplemental nitrite. In response, the FDA immediately alerted the public and began an investigation.
The FDA’s initial research found that the procedures previously used to quantify NDMA were not appropriate for assessing its presence in ranitidine, owing to the use of high temperatures that could convert ranitidine to NDMA during that analysis. New lower-temperature analytical methods found that the amounts of NDMA contained in ranitidine products were 3,000-fold lower than those reported in the citizen petition; however, these lower amounts of NDMA were still above the FDA-acceptable level and could increase over time, prompting the FDA to request the market withdrawal of ranitidine products.
The FDA noted, however, that if ranitidine products could be manufactured to control NDMA amounts, they could be allowed back on the market—but additional information would first be needed to understand whether NDMA could form in vivo from ranitidine in humans.


 Dr. Seifi[/caption]
Ali Seifi, MD, FACP, FNCS, FCCM
Associate Professor
Director of Neuro Critical Care,
Fellowship Director, CAST Neurosurgery Critical Care
Department of Neurosurgery, Neurology, Anesthesiology and Medicine
The University of Texas Health Science Center at San Antonio
MedicalResearch.com: What is the background for this study?
Dr. Seifi[/caption]
Ali Seifi, MD, FACP, FNCS, FCCM
Associate Professor
Director of Neuro Critical Care,
Fellowship Director, CAST Neurosurgery Critical Care
Department of Neurosurgery, Neurology, Anesthesiology and Medicine
The University of Texas Health Science Center at San Antonio
MedicalResearch.com: What is the background for this study?


 Dr. Wong[/caption]
John B. Wong, M.D.
Chief Scientific Officer
Vice chair for Clinical Affairs
Chief of the Division of Clinical Decision Making and
Primary care Clinician
Department of Medicine at Tufts Medical Center
MedicalResearch.com: What is the background for this study?
Response: Hypertension affects nearly half of all adults in the United States and is a major risk factor for many serious health conditions. Fortunately, by screening all adults for hypertension, clinicians can improve their patient’s health. The Task Force continues to recommend screening all adults for hypertension so that they can get the care they need to help prevent health conditions such as heart attack, stroke, and kidney failure.
Dr. Wong[/caption]
John B. Wong, M.D.
Chief Scientific Officer
Vice chair for Clinical Affairs
Chief of the Division of Clinical Decision Making and
Primary care Clinician
Department of Medicine at Tufts Medical Center
MedicalResearch.com: What is the background for this study?
Response: Hypertension affects nearly half of all adults in the United States and is a major risk factor for many serious health conditions. Fortunately, by screening all adults for hypertension, clinicians can improve their patient’s health. The Task Force continues to recommend screening all adults for hypertension so that they can get the care they need to help prevent health conditions such as heart attack, stroke, and kidney failure.

 Dr. Yun Liu[/caption]
Yun Liu, PhD
Google Health
Palo Alto, California
MedicalResearch.com: What is the background for this study? Would you describe the system? Does it use dermatoscopic images?
Response: Dermatologic conditions are extremely common and a leading cause of morbidity worldwide. Due to limited access to dermatologists, patients often first seek help from non-specialists. However, non-specialists have been reported to have lower diagnostic accuracies compared to dermatologists, which may impact the quality of care.
In this study, we built upon prior work published in
Dr. Yun Liu[/caption]
Yun Liu, PhD
Google Health
Palo Alto, California
MedicalResearch.com: What is the background for this study? Would you describe the system? Does it use dermatoscopic images?
Response: Dermatologic conditions are extremely common and a leading cause of morbidity worldwide. Due to limited access to dermatologists, patients often first seek help from non-specialists. However, non-specialists have been reported to have lower diagnostic accuracies compared to dermatologists, which may impact the quality of care.
In this study, we built upon prior work published in 
 Dr. McPeek Hinz[/caption]
Eugenia McPeek Hinz MD MS FAMIA
Associate CMIO - DHTS
Duke University Health System
MedicalResearch.com: What is the background for this study?
Response: Clinician burnout rates have hovered around 50% for much of the past decade. Burnout is a significant concern in healthcare for its effects on care givers and associated downstream adverse implications on patient care for quality and safety. The ubiquitous presence of Electronic Health Records (EHR) along with the increased clerical components and after hours use has been a significant concern for contributing to provider burnout.
Dr. McPeek Hinz[/caption]
Eugenia McPeek Hinz MD MS FAMIA
Associate CMIO - DHTS
Duke University Health System
MedicalResearch.com: What is the background for this study?
Response: Clinician burnout rates have hovered around 50% for much of the past decade. Burnout is a significant concern in healthcare for its effects on care givers and associated downstream adverse implications on patient care for quality and safety. The ubiquitous presence of Electronic Health Records (EHR) along with the increased clerical components and after hours use has been a significant concern for contributing to provider burnout. 