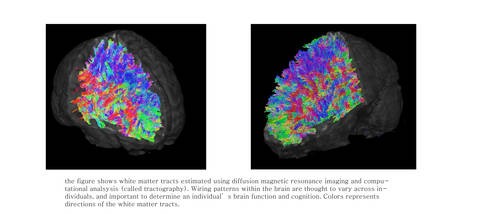
Author Interviews, Breast Cancer, NIH, OBGYNE / 27.12.2018
Breast Cancer Risk Remains Elevated 20-30 years After Childbirth
MedicalResearch.com Interview with:
[caption id="attachment_46711" align="alignleft" width="133"] Dr. Sandler[/caption]
Dale P. Sandler, Ph.D.
Chief, Epidemiology Branch
National Institute of Environmental Health Sciences
NIH
MedicalResearch.com: What is the background for this study?
Response: Not having children is a well-established risk factor for breast cancer, but most of this evidence comes from studies of postmenopausal women since breast cancer before menopause is relatively uncommon. There is growing evidence that some risk factors differ for premenopausal and postmenopausal breast cancer – for example obesity which increases risk for breast cancer after menopause but appears to be protective before menopause.
There was some evidence that breast cancer risk increased shortly after pregnancy. It was thought that this risk lasted for 5 to ten years. Studies were unable to fully characterize the duration of this increase in risk or evaluate factors such as breast feeding, age at birth, or family history of breast cancer that could modify the relationship between recent pregnancy and breast cancer risk. Breast cancer before menopause or age 55 is relatively rare, and few individual studies are large enough to answer these questions.
To answer these questions, we formed the Breast Cancer Collaborative Group, a pooling project involving 20 prospective cohort studies. We included 890,000 women from 15 of these long-term studies across three continents, including over 18,000 incident breast cancer cases.
Dr. Sandler[/caption]
Dale P. Sandler, Ph.D.
Chief, Epidemiology Branch
National Institute of Environmental Health Sciences
NIH
MedicalResearch.com: What is the background for this study?
Response: Not having children is a well-established risk factor for breast cancer, but most of this evidence comes from studies of postmenopausal women since breast cancer before menopause is relatively uncommon. There is growing evidence that some risk factors differ for premenopausal and postmenopausal breast cancer – for example obesity which increases risk for breast cancer after menopause but appears to be protective before menopause.
There was some evidence that breast cancer risk increased shortly after pregnancy. It was thought that this risk lasted for 5 to ten years. Studies were unable to fully characterize the duration of this increase in risk or evaluate factors such as breast feeding, age at birth, or family history of breast cancer that could modify the relationship between recent pregnancy and breast cancer risk. Breast cancer before menopause or age 55 is relatively rare, and few individual studies are large enough to answer these questions.
To answer these questions, we formed the Breast Cancer Collaborative Group, a pooling project involving 20 prospective cohort studies. We included 890,000 women from 15 of these long-term studies across three continents, including over 18,000 incident breast cancer cases.
 Dr. Sandler[/caption]
Dale P. Sandler, Ph.D.
Chief, Epidemiology Branch
National Institute of Environmental Health Sciences
NIH
MedicalResearch.com: What is the background for this study?
Response: Not having children is a well-established risk factor for breast cancer, but most of this evidence comes from studies of postmenopausal women since breast cancer before menopause is relatively uncommon. There is growing evidence that some risk factors differ for premenopausal and postmenopausal breast cancer – for example obesity which increases risk for breast cancer after menopause but appears to be protective before menopause.
There was some evidence that breast cancer risk increased shortly after pregnancy. It was thought that this risk lasted for 5 to ten years. Studies were unable to fully characterize the duration of this increase in risk or evaluate factors such as breast feeding, age at birth, or family history of breast cancer that could modify the relationship between recent pregnancy and breast cancer risk. Breast cancer before menopause or age 55 is relatively rare, and few individual studies are large enough to answer these questions.
To answer these questions, we formed the Breast Cancer Collaborative Group, a pooling project involving 20 prospective cohort studies. We included 890,000 women from 15 of these long-term studies across three continents, including over 18,000 incident breast cancer cases.
Dr. Sandler[/caption]
Dale P. Sandler, Ph.D.
Chief, Epidemiology Branch
National Institute of Environmental Health Sciences
NIH
MedicalResearch.com: What is the background for this study?
Response: Not having children is a well-established risk factor for breast cancer, but most of this evidence comes from studies of postmenopausal women since breast cancer before menopause is relatively uncommon. There is growing evidence that some risk factors differ for premenopausal and postmenopausal breast cancer – for example obesity which increases risk for breast cancer after menopause but appears to be protective before menopause.
There was some evidence that breast cancer risk increased shortly after pregnancy. It was thought that this risk lasted for 5 to ten years. Studies were unable to fully characterize the duration of this increase in risk or evaluate factors such as breast feeding, age at birth, or family history of breast cancer that could modify the relationship between recent pregnancy and breast cancer risk. Breast cancer before menopause or age 55 is relatively rare, and few individual studies are large enough to answer these questions.
To answer these questions, we formed the Breast Cancer Collaborative Group, a pooling project involving 20 prospective cohort studies. We included 890,000 women from 15 of these long-term studies across three continents, including over 18,000 incident breast cancer cases. 

 Josephine Funck Bilsteen, MSc
Department of Pediatrics, Hvidovre University Hospital, Hvidovre,
Section of Epidemiology, Department of Public Health
University of Copenhagen
Copenhagen, Denmark
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background of this study is that there is increasing recognition of the longer-term health and social outcomes associated with preterm birth such as independent living, quality of life, self-perception and socioeconomic achievements. However, much less is known about differences in education and income among adults born at different gestational weeks in the term period.
In this study shorter gestational duration, even within the term range, was associated with lower chances of having a high personal income and having completed a secondary or tertiary education at age 28 years. This is the first study to show that adults born at 37 and 38 completed weeks of gestation had slightly lower chances of having a high income and educational level than adults born at 40 completed weeks of gestation.
Josephine Funck Bilsteen, MSc
Department of Pediatrics, Hvidovre University Hospital, Hvidovre,
Section of Epidemiology, Department of Public Health
University of Copenhagen
Copenhagen, Denmark
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background of this study is that there is increasing recognition of the longer-term health and social outcomes associated with preterm birth such as independent living, quality of life, self-perception and socioeconomic achievements. However, much less is known about differences in education and income among adults born at different gestational weeks in the term period.
In this study shorter gestational duration, even within the term range, was associated with lower chances of having a high personal income and having completed a secondary or tertiary education at age 28 years. This is the first study to show that adults born at 37 and 38 completed weeks of gestation had slightly lower chances of having a high income and educational level than adults born at 40 completed weeks of gestation. 




 Dr. Ray[/caption]
Joel Ray MD, MSc, FRCPC
Institute of Health Policy, Management and Evaluation
Faculty of Medicine
University of Toronto, Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many women who die within childbirth or soon thereafter experience rapid onset of morbidity/illness before succumbing. Thus, severe maternal morbidity (SMM) offers a detectable (or set of detectable) conditions that might be dealt with before they progress to a fatality. Even so, severe maternal morbidity alone can be non-fatal, but create disability for a new mother (e.g., a stroke), or prolong separation of mother and newborn.
So, we showed that, as the number of severe maternal morbidity indicators rises, so does the probability of maternal death. This relation was exponential in nature.
Dr. Ray[/caption]
Joel Ray MD, MSc, FRCPC
Institute of Health Policy, Management and Evaluation
Faculty of Medicine
University of Toronto, Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many women who die within childbirth or soon thereafter experience rapid onset of morbidity/illness before succumbing. Thus, severe maternal morbidity (SMM) offers a detectable (or set of detectable) conditions that might be dealt with before they progress to a fatality. Even so, severe maternal morbidity alone can be non-fatal, but create disability for a new mother (e.g., a stroke), or prolong separation of mother and newborn.
So, we showed that, as the number of severe maternal morbidity indicators rises, so does the probability of maternal death. This relation was exponential in nature. 
 Dr Sarah Myers PhD
Honorary Research Associate
UCL Department of Anthropology
MedicalResearch.com: What is the background for this study?
Response: Postnatal or postpartum depression is unfortunately common after giving birth; a figure often quoted is 15%, but some studies have found much higher numbers. Postnatal depression is associated with a range of poorer outcomes for mothers and their infants, and the financial costs of treating maternal mental ill health put health services under considerable strain. Studies have found that providing additional emotional support to at risk mothers, for instance via peer support programmes or regular phone calls with health visitors, can reduce the likelihood of them developing the condition. Therefore, it is really important that we understand the full range of risk factors that put women at greater risk of becoming depressed after giving birth.
There is increasing evidence for a link between inflammation and depression, with factors that trigger an inflammatory immune response also increasing the likelihood of depressive symptoms. The opens up the possibility of finding new risk factors for postnatal depression based on known associations with inflammation.
Dr Sarah Myers PhD
Honorary Research Associate
UCL Department of Anthropology
MedicalResearch.com: What is the background for this study?
Response: Postnatal or postpartum depression is unfortunately common after giving birth; a figure often quoted is 15%, but some studies have found much higher numbers. Postnatal depression is associated with a range of poorer outcomes for mothers and their infants, and the financial costs of treating maternal mental ill health put health services under considerable strain. Studies have found that providing additional emotional support to at risk mothers, for instance via peer support programmes or regular phone calls with health visitors, can reduce the likelihood of them developing the condition. Therefore, it is really important that we understand the full range of risk factors that put women at greater risk of becoming depressed after giving birth.
There is increasing evidence for a link between inflammation and depression, with factors that trigger an inflammatory immune response also increasing the likelihood of depressive symptoms. The opens up the possibility of finding new risk factors for postnatal depression based on known associations with inflammation.

 Dr. McLaughlin[/caption]
Ryan J. McLaughlin, PhD
Assistant Professor
Department of Integrative Physiology & Neuroscience
College of Veterinary Medicine
Washington State University
Pullman, WA 99164-7620
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of cannabis during pregnancy is a growing health concern, yet the long-term cognitive ramifications for developing offspring remain largely unknown. Human studies exploring the long-term effects of maternal cannabis use have been sparse for several reasons, including the length and cost of such studies, as well as the fact that experimentally assigning mothers to smoke cannabis during pregnancy is obviously ethically impractical. Animal models of maternal cannabis use have been advantageous in this respect, but they have been limited by the drugs used (synthetic cannabinoids vs. THC vs. cannabis plant) and the way that they are administered. In our study, we used a more translationally relevant animal model of maternal cannabis use that exposes pregnant rat dams to whole plant cannabis extracts using the intra-pulmonary route of administration that is most common to human users. Our preliminary data indicate that twice-daily exposure to a high-dose cannabis extract during pregnancy may produce deficits in cognitive flexibility in adult rat offspring. Importantly, these rats did not experience general learning deficits, as they performed comparably to non-exposed offspring when required to follow a cue in their environment that dictate reinforcer delivery. Instead, deficits were observed only when rats were required to disregard this previous cue-based strategy and adopt a new egocentric spatial strategy in order to continue receiving the sugar reinforcers.
Dr. McLaughlin[/caption]
Ryan J. McLaughlin, PhD
Assistant Professor
Department of Integrative Physiology & Neuroscience
College of Veterinary Medicine
Washington State University
Pullman, WA 99164-7620
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of cannabis during pregnancy is a growing health concern, yet the long-term cognitive ramifications for developing offspring remain largely unknown. Human studies exploring the long-term effects of maternal cannabis use have been sparse for several reasons, including the length and cost of such studies, as well as the fact that experimentally assigning mothers to smoke cannabis during pregnancy is obviously ethically impractical. Animal models of maternal cannabis use have been advantageous in this respect, but they have been limited by the drugs used (synthetic cannabinoids vs. THC vs. cannabis plant) and the way that they are administered. In our study, we used a more translationally relevant animal model of maternal cannabis use that exposes pregnant rat dams to whole plant cannabis extracts using the intra-pulmonary route of administration that is most common to human users. Our preliminary data indicate that twice-daily exposure to a high-dose cannabis extract during pregnancy may produce deficits in cognitive flexibility in adult rat offspring. Importantly, these rats did not experience general learning deficits, as they performed comparably to non-exposed offspring when required to follow a cue in their environment that dictate reinforcer delivery. Instead, deficits were observed only when rats were required to disregard this previous cue-based strategy and adopt a new egocentric spatial strategy in order to continue receiving the sugar reinforcers.











 Ali Khashan, PhD
Senior Lecturer in Epidemiology
School of Public Health & INFANT Centre
University College Cork
Cork, Ireland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There is some evidence to suggest an increased likelihood of neurodevelopmental disorders in relation to hypertensive disorders in pregnancy, however consensus is lacking. Considering hypertensive disorders in pregnancy are among the most common prenatal complication, we decided to synthesise the published literature on this topic by conducting a comprehensive systematic review and meta-analysis.
Our main findings suggest that hypertensive disorders in pregnancy are associated with about 30% increase in the likelihood of autism spectrum disorders (ASD) and ADHD in the offspring, compared to offspring not exposed to hypertensive disorders in pregnancy.
Ali Khashan, PhD
Senior Lecturer in Epidemiology
School of Public Health & INFANT Centre
University College Cork
Cork, Ireland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There is some evidence to suggest an increased likelihood of neurodevelopmental disorders in relation to hypertensive disorders in pregnancy, however consensus is lacking. Considering hypertensive disorders in pregnancy are among the most common prenatal complication, we decided to synthesise the published literature on this topic by conducting a comprehensive systematic review and meta-analysis.
Our main findings suggest that hypertensive disorders in pregnancy are associated with about 30% increase in the likelihood of autism spectrum disorders (ASD) and ADHD in the offspring, compared to offspring not exposed to hypertensive disorders in pregnancy.