Author Interviews, Dermatology, Global Health, NEJM, Zika / 15.03.2018
Zika Birth Defects More Severe When Mothers Infected During First Trimester
MedicalResearch.com Interview with:
[caption id="attachment_40591" align="alignleft" width="233"]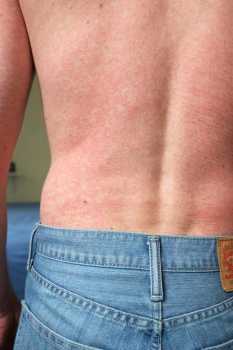 This image depicts a posterior view of a patient’s back, captured in a clinical setting, upon presenting with this blotchy rash. After a diagnostic work-up, it was determined that the rash had been caused by the Zika virus.
This image depicts a posterior view of a patient’s back, captured in a clinical setting, upon presenting with this blotchy rash. After a diagnostic work-up, it was determined that the rash had been caused by the Zika virus.
Note: Not all patients with Zika get a rash
CDC image[/caption] Professor Bruno Hoen, M.D., Ph.D Dept of Infectious Diseases, Dermatology, and Internal Medicine University Medical Center of Guadeloupe MedicalResearch.com: What is the background for this study? Response: Zika virus (ZIKV) infection during pregnancy has been identified only recently to cause severe birth defects, including microcephaly, other brain defects, and the congenital Zika syndrome. However, the magnitude of this risk was not clearly defined, with discrepancies between observational data from Brazil and the U.S. Zika Pregnancy Registry. We implemented a cohort study of pregnant women who have been exposed to ZIKV throughout the outbreak that hit the Caribbean in 2016.
 This image depicts a posterior view of a patient’s back, captured in a clinical setting, upon presenting with this blotchy rash. After a diagnostic work-up, it was determined that the rash had been caused by the Zika virus.
This image depicts a posterior view of a patient’s back, captured in a clinical setting, upon presenting with this blotchy rash. After a diagnostic work-up, it was determined that the rash had been caused by the Zika virus.Note: Not all patients with Zika get a rash
CDC image[/caption] Professor Bruno Hoen, M.D., Ph.D Dept of Infectious Diseases, Dermatology, and Internal Medicine University Medical Center of Guadeloupe MedicalResearch.com: What is the background for this study? Response: Zika virus (ZIKV) infection during pregnancy has been identified only recently to cause severe birth defects, including microcephaly, other brain defects, and the congenital Zika syndrome. However, the magnitude of this risk was not clearly defined, with discrepancies between observational data from Brazil and the U.S. Zika Pregnancy Registry. We implemented a cohort study of pregnant women who have been exposed to ZIKV throughout the outbreak that hit the Caribbean in 2016.