Legal-Malpractice, Surgical Research / 03.02.2026
Warning Signs or Surgical Errors and Medical Malpractice
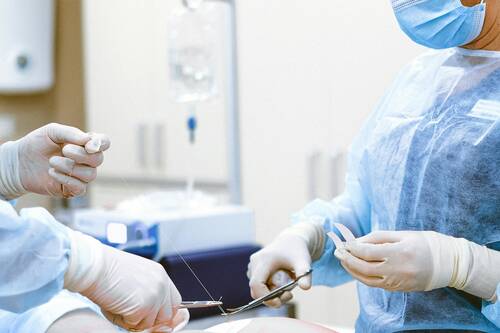
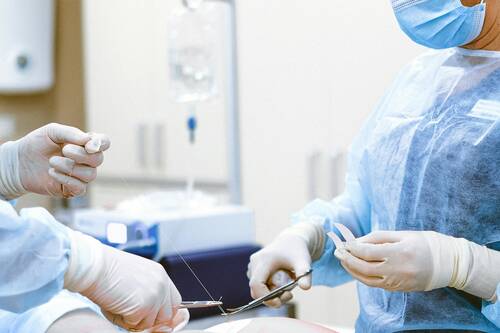
[caption id="attachment_72239" align="aligncenter" width="500"] Photo by Cedric Fauntleroy[/caption]
During the onset of surgeries, a surgeon starts to heal the patient as the team professionally handles the operation. When trust between the surgeon and the team breaks down, the likelihood of errors or mistakes increases significantly. The patients should learn to notice the warning signals and understand critical interventions.
According to a 2024 Forbes article, nearly 20,000 medical malpractice cases are filed annually in the United States. This article also said that in the course of their careers, 31.2% of physicians reported they had already been sued at least once.
A patient who notices sudden complications or feels neglected during surgery should take action right away.
What should you do when you first discover medical malpractice? Let’s find out below.
Photo by Cedric Fauntleroy[/caption]
During the onset of surgeries, a surgeon starts to heal the patient as the team professionally handles the operation. When trust between the surgeon and the team breaks down, the likelihood of errors or mistakes increases significantly. The patients should learn to notice the warning signals and understand critical interventions.
According to a 2024 Forbes article, nearly 20,000 medical malpractice cases are filed annually in the United States. This article also said that in the course of their careers, 31.2% of physicians reported they had already been sued at least once.
A patient who notices sudden complications or feels neglected during surgery should take action right away.
What should you do when you first discover medical malpractice? Let’s find out below.
 Photo by Cedric Fauntleroy[/caption]
During the onset of surgeries, a surgeon starts to heal the patient as the team professionally handles the operation. When trust between the surgeon and the team breaks down, the likelihood of errors or mistakes increases significantly. The patients should learn to notice the warning signals and understand critical interventions.
According to a 2024 Forbes article, nearly 20,000 medical malpractice cases are filed annually in the United States. This article also said that in the course of their careers, 31.2% of physicians reported they had already been sued at least once.
A patient who notices sudden complications or feels neglected during surgery should take action right away.
What should you do when you first discover medical malpractice? Let’s find out below.
Photo by Cedric Fauntleroy[/caption]
During the onset of surgeries, a surgeon starts to heal the patient as the team professionally handles the operation. When trust between the surgeon and the team breaks down, the likelihood of errors or mistakes increases significantly. The patients should learn to notice the warning signals and understand critical interventions.
According to a 2024 Forbes article, nearly 20,000 medical malpractice cases are filed annually in the United States. This article also said that in the course of their careers, 31.2% of physicians reported they had already been sued at least once.
A patient who notices sudden complications or feels neglected during surgery should take action right away.
What should you do when you first discover medical malpractice? Let’s find out below.








 Dr. Magruder[/caption]
Matthew Magruder, MD PGY3
Orthopaedic Residency Program
Department of Orthopaedic Surgery and Rehabilitation
Maimonides Medical Center
MedicalResearch.com: What is the background for this study?
Response: The prevalence of obesity and diabetes mellitus has reached epidemic proportions. Approximately 37.3 million people in the United States, accounting for 11.3% of the total population, have diabetes, and 100.1 million, or 41.9%, of all US citizens are obese. Furthermore, these numbers are only projected to increase in the coming decades. This is an issue for orthopaedic surgeons because diabetes and obesity have consistently been demonstrated to be risk factors for complications following total joint replacements, especially total hip replacements. Therefore, we are in desperate need of new and more effective tools in mitigating the risk of poor outcomes in our joint replacement patients.
Semaglutide, and other GLP-1 agonists, are potentially a new tool that can be used to help decrease the risks following joint replacement surgery. Initially a medication to treat diabetes, semaglutide has recently been approved by the FDA to treat obesity as well, as randomized controlled trials have consistently demonstrated significant weight loss with minimal side effects. The purpose of our study was to see what effect the use of semaglutide had on total hip arthroplasty patient outcomes.
Dr. Magruder[/caption]
Matthew Magruder, MD PGY3
Orthopaedic Residency Program
Department of Orthopaedic Surgery and Rehabilitation
Maimonides Medical Center
MedicalResearch.com: What is the background for this study?
Response: The prevalence of obesity and diabetes mellitus has reached epidemic proportions. Approximately 37.3 million people in the United States, accounting for 11.3% of the total population, have diabetes, and 100.1 million, or 41.9%, of all US citizens are obese. Furthermore, these numbers are only projected to increase in the coming decades. This is an issue for orthopaedic surgeons because diabetes and obesity have consistently been demonstrated to be risk factors for complications following total joint replacements, especially total hip replacements. Therefore, we are in desperate need of new and more effective tools in mitigating the risk of poor outcomes in our joint replacement patients.
Semaglutide, and other GLP-1 agonists, are potentially a new tool that can be used to help decrease the risks following joint replacement surgery. Initially a medication to treat diabetes, semaglutide has recently been approved by the FDA to treat obesity as well, as randomized controlled trials have consistently demonstrated significant weight loss with minimal side effects. The purpose of our study was to see what effect the use of semaglutide had on total hip arthroplasty patient outcomes.

 Dr. Wallis[/caption]
Christopher Wallis, MD, PhD
Assistant Professor of Urology
Department of Surgery
University of Toronto and Urologic Oncologist
Mount Sinai Hospital
MedicalResearch.com: Could you give a little context - what was the question you were looking at?
Dr. Wallis[/caption]
Christopher Wallis, MD, PhD
Assistant Professor of Urology
Department of Surgery
University of Toronto and Urologic Oncologist
Mount Sinai Hospital
MedicalResearch.com: Could you give a little context - what was the question you were looking at?

 Dr. Potnuru[/caption]
Paul Potnuru, MD
Assistant Professor
Anesthesiology, Critical Care and Pain Medicine
The John P. and Kathrine G. McGovern Medical School
The University of Texas Health Science Center at Houston
Dr. Potnuru[/caption]
Paul Potnuru, MD
Assistant Professor
Anesthesiology, Critical Care and Pain Medicine
The John P. and Kathrine G. McGovern Medical School
The University of Texas Health Science Center at Houston

 Dr. Bailey[/caption]
Michael Bailey Ph.D.
Senior Principal Engineer, Applied Physics Laboratory
Associate Professor. Mechanical Engineering
Adjunct Associate Professor Urology
MedicalResearch.com: What is the background for this study?
Response: Small (< 6 mm) kidney stones are common and often are asymptomatic. Do you do surgery or wait for them to cause a problem? Or specifically here if you are getting surgery already for other stones that are causing a problem do you take the time and possibly extra risk of cleaning out the small stone in the kidney or in the other kidney?
Dr. Bailey[/caption]
Michael Bailey Ph.D.
Senior Principal Engineer, Applied Physics Laboratory
Associate Professor. Mechanical Engineering
Adjunct Associate Professor Urology
MedicalResearch.com: What is the background for this study?
Response: Small (< 6 mm) kidney stones are common and often are asymptomatic. Do you do surgery or wait for them to cause a problem? Or specifically here if you are getting surgery already for other stones that are causing a problem do you take the time and possibly extra risk of cleaning out the small stone in the kidney or in the other kidney?


 Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.
Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.