Author Interviews, BMJ, Surgical Research / 15.10.2020
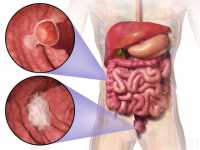
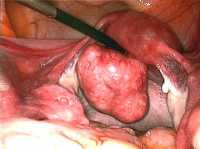
Surgical Procedures That Generate Aerosols Requiring Enhanced PPE
MedicalResearch.com Interview with:
Sebastian Straube, BM BCh, MA (Oxon), DPhil
Professor and Director, Division of Preventive Medicine, Department of Medicine
University of Alberta
Zone Section Chief, Occupational Medicine Edmonton Zone, Alberta Health Services
Director, Foundation Course in Occupational Medicine
 MedicalResearch.com: What is the background for this study?
Response: In view of the COVID-19 pandemic, medical procedures that generate aerosols require a higher grade of personal protective equipment, typically including filtering facepiece respirators (e.g. N95 masks). We wanted to know which procedures were aerosol-generating and would require such enhanced precautions.
MedicalResearch.com: How did you approach that question?
Response: We conducted a systematic review of the literature and aimed to find those procedures for which there is widespread agreement that they are aerosol-generating. We assembled a team of researchers with expertise in the subject matter as well as in systematic review methodology, and we searched widely for relevant guidelines, policy documents, and academic papers.
MedicalResearch.com: What is the background for this study?
Response: In view of the COVID-19 pandemic, medical procedures that generate aerosols require a higher grade of personal protective equipment, typically including filtering facepiece respirators (e.g. N95 masks). We wanted to know which procedures were aerosol-generating and would require such enhanced precautions.
MedicalResearch.com: How did you approach that question?
Response: We conducted a systematic review of the literature and aimed to find those procedures for which there is widespread agreement that they are aerosol-generating. We assembled a team of researchers with expertise in the subject matter as well as in systematic review methodology, and we searched widely for relevant guidelines, policy documents, and academic papers.
 MedicalResearch.com: What is the background for this study?
Response: In view of the COVID-19 pandemic, medical procedures that generate aerosols require a higher grade of personal protective equipment, typically including filtering facepiece respirators (e.g. N95 masks). We wanted to know which procedures were aerosol-generating and would require such enhanced precautions.
MedicalResearch.com: How did you approach that question?
Response: We conducted a systematic review of the literature and aimed to find those procedures for which there is widespread agreement that they are aerosol-generating. We assembled a team of researchers with expertise in the subject matter as well as in systematic review methodology, and we searched widely for relevant guidelines, policy documents, and academic papers.
MedicalResearch.com: What is the background for this study?
Response: In view of the COVID-19 pandemic, medical procedures that generate aerosols require a higher grade of personal protective equipment, typically including filtering facepiece respirators (e.g. N95 masks). We wanted to know which procedures were aerosol-generating and would require such enhanced precautions.
MedicalResearch.com: How did you approach that question?
Response: We conducted a systematic review of the literature and aimed to find those procedures for which there is widespread agreement that they are aerosol-generating. We assembled a team of researchers with expertise in the subject matter as well as in systematic review methodology, and we searched widely for relevant guidelines, policy documents, and academic papers.






 Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
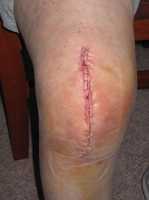
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.
Dr. Cavanaugh[/caption]
Alyson Cavanaugh, PT, PhD
Joint Doctoral Program in Epidemiology
University of California, San Diego/ San Diego State University
MedicalResearch.com: What is the background for this study?
Response: More than 700,000 total knee replacements are performed annually in the United States, but there is a racial disparity in outcomes after the surgery. If the knee replacement procedure is considered a highly effective treatment, why don't black women present with the same outcomes as whites?
Physical function when going into surgery has a large impact on the potential functional outcomes after surgery. Our hypothesis was that black women were presenting to surgery with poorer physical function, which was contributing to poorer functional outcomes after surgery.