Author Interviews, Heart Disease, JACC, Pediatrics, Surgical Research, UCSD / 04.01.2018
Children with Heart Failure from Dilated Cardiomyopathy are Surviving Longer in the Most Recent Era
[caption id="attachment_39174" align="alignleft" width="300"]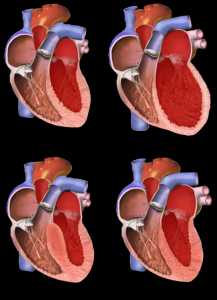 Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
 Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.
Structural categories of cardiomyopathy Wikipedia image[/caption]
MedicalResearch.com Interview with:
Rakesh K. Singh MD, MS
Department of Pediatrics, University of California–San Diego and
Rady Children’s Hospital
San Diego, California
Steven E. Lipshultz MD
Department of Pediatrics
Wayne State University School of Medicine and
Children’s Hospital of Michigan
Detroit, Michigan
MedicalResearch.com: What is the background for this study?
Response: Dilated cardiomyopathy (DCM) is a disease characterized by dilation and dysfunction of the left ventricle of the heart. While DCM is a relatively rare disease in children, nearly 40% of children with DCM require a heart transplant or die within 2 years of diagnosis. Heart transplantation has improved the outcomes of children with DCM over the last 3 decades, but is limited by donor heart availability. Newer therapies, including advanced ICU care and artificial heart machines, are now being used to treat children with DCM.
This study published in the November 28, 2017 issue of the Journal of American College of Cardiology (JACC) sought to determine whether more children with DCM were surviving longer in the more recent era. Specifically, it investigated whether children with DCM were surviving longer without the need for heart transplantation. Rakesh Singh, MD is the first author and an Associate Professor of Pediatrics at UC San Diego/Rady Children’s Hospital, while the senior author is Steven Lipshultz, MD, Professor at Wayne State University School of Medicine/Detroit Medical Center’s Children’s Hospital of Michigan and Director of Children’s Research Center of Michigan.
The Pediatric Cardiomyopathy Registry (PCMR) is a National Heart, Lung, and Blood Institute (NHLBI) sponsored registry from 98 pediatric centers in United States and Canada created to study the outcomes of children with various heart muscle disorders known as cardiomyopathies. For this study, outcomes of 1,199 children diagnosed with DCM from 1990-1999 were compared with 754 children diagnosed with DCM from 2000-2009.






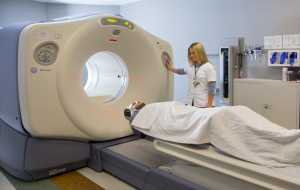









 Dr. Jacobs[/caption]
Dr. Lisa K. Jacobs MD
Johns Hopkins School of Medicine
Baltimore, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Breast preservation is the preferred treatment for many women diagnosed with breast cancer. The most common question that a patient will ask after the surgery is, “Did you get it all?” In the ideal case, this is accomplished in a single outpatient surgery with very good cosmetic results. In our study, Beyond the Margins-Economic Costs and Complications Associated with Repeated Breast-Conserving Surgeries we evaluated the detrimental effects of an unsuccessful initial surgery due to positive surgical margins. Using private insurance claims data, we found that 16% of patients planning breast preservation required a second breast-conserving surgery and an additional 7% converted to mastectomy. Of those patients that required additional surgery there was a 56% ($16,072) increase in cost and a 48% increase in complications. Those complications include infection, hematoma, seroma, and fat necrosis. This study demonstrates that repeated surgery has not only cosmetic consequences, but also has financial implications and increased risk.
Dr. Jacobs[/caption]
Dr. Lisa K. Jacobs MD
Johns Hopkins School of Medicine
Baltimore, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Breast preservation is the preferred treatment for many women diagnosed with breast cancer. The most common question that a patient will ask after the surgery is, “Did you get it all?” In the ideal case, this is accomplished in a single outpatient surgery with very good cosmetic results. In our study, Beyond the Margins-Economic Costs and Complications Associated with Repeated Breast-Conserving Surgeries we evaluated the detrimental effects of an unsuccessful initial surgery due to positive surgical margins. Using private insurance claims data, we found that 16% of patients planning breast preservation required a second breast-conserving surgery and an additional 7% converted to mastectomy. Of those patients that required additional surgery there was a 56% ($16,072) increase in cost and a 48% increase in complications. Those complications include infection, hematoma, seroma, and fat necrosis. This study demonstrates that repeated surgery has not only cosmetic consequences, but also has financial implications and increased risk.


