[caption id="attachment_72926" align="aligncenter" width="500"]
 Freepix
Freepix[/caption]
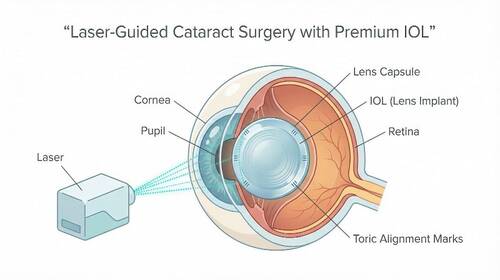
Innovation is at the heart of the life sciences industry. Whether developing new medicines, producing advanced medical devices, or driving progress in biotechnology and digital health, organisations in this space play a critical role in improving and extending lives.
However, the impact of these products also means the risks are significant. If a product fails—due to a defect, contamination, incorrect instructions or a systems error—the consequences can be severe. Businesses may face claims involving patient injury, financial losses, regulatory intervention and lasting reputational harm.
For this reason, product liability life science insurance is a key consideration for companies operating across the life sciences sector. Below, we explore what it covers, who should consider it, and the wider risk landscape.
Understanding Product Liability in Life Sciences
Product liability insurance is designed to protect businesses when a product they manufacture, supply or distribute causes harm or damage.
Within life sciences, the nature of these risks is often more complex than in other sectors. Potential causes of claims include:
- Flaws in product design
- Errors during manufacturing
- Insufficient instructions or safety warnings
- Software or system failures in medical technologies
- Contamination during production or storage
- Weaknesses in quality assurance processes
Given the strict regulatory environment in the UK and beyond, any failure can quickly escalate. Claims may involve substantial compensation payments, legal costs and scrutiny from regulatory authorities.
 Photo by beyzahzah[/caption]
Choosing a career in nutrition usually stems from a genuine desire to help people live healthier lives through the science of food. However, the academic road to becoming a Registered Dietitian (RD) or Registered Dietitian Nutritionist (RDN) is rigorous and highly regulated. If you are balancing a job or family life, you’ve likely wondered if you can complete this path virtually. The answer is a resounding yes—provided you choose a program with the right accreditation. To jumpstart your career in this field, finding a high-quality nutrition degree online is the essential first step toward meeting the national standards for clinical practice.
Photo by beyzahzah[/caption]
Choosing a career in nutrition usually stems from a genuine desire to help people live healthier lives through the science of food. However, the academic road to becoming a Registered Dietitian (RD) or Registered Dietitian Nutritionist (RDN) is rigorous and highly regulated. If you are balancing a job or family life, you’ve likely wondered if you can complete this path virtually. The answer is a resounding yes—provided you choose a program with the right accreditation. To jumpstart your career in this field, finding a high-quality nutrition degree online is the essential first step toward meeting the national standards for clinical practice.












 Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.
Hearing loss often creeps in slowly. A person may start asking others to repeat themselves, miss parts of conversations in noisy rooms, or turn the television up a little more than before. That is one reason newer devices that blend hearing support into familiar objects are getting attention.
Hearing glasses are one of those devices. They are designed to combine eyewear with built-in hearing assistance, which can make them feel less medical and more natural to use in daily life. Still, the real question is not whether they sound innovative. It is whether they are actually effective for older adults.
In many cases, they can be helpful, especially for older adults with mild to moderate hearing loss who want something discreet and easier to work into everyday routines. But they are not a universal replacement for traditional hearing aids, and how well they work depends a lot on the user’s hearing needs, lifestyle, and expectations.