Author Interviews, Cost of Health Care, Kidney Disease / 03.07.2019
Social Risk Factors May Influence Dialysis Quality Measures and Financial Penalties
MedicalResearch.com Interview with:
 Andrew C. Qi, Medical student
Karen E. Joynt Maddox MD MPH
Assistant professor of medicine
Washington University School of Medicine
Saint Louis, Missouri.
MedicalResearch.com: What is the background for this study?
Response: The End-Stage Renal Disease Quality Incentive Program (ESRD QIP) is a Medicare program that evaluates dialysis facilities in the U.S. based on a set of quality measures, and penalizes low-performing facilities. We’ve seen a growing understanding of how social risk factors like poverty and race/ethnicity impact patient outcomes in other settings, making it difficult for providers caring for disadvantaged populations to perform as well in these kinds of pay-for-performance programs. We were interested in seeing if this was the case for dialysis facilities as well, especially since patients receiving dialysis are already a vulnerable population.
Andrew C. Qi, Medical student
Karen E. Joynt Maddox MD MPH
Assistant professor of medicine
Washington University School of Medicine
Saint Louis, Missouri.
MedicalResearch.com: What is the background for this study?
Response: The End-Stage Renal Disease Quality Incentive Program (ESRD QIP) is a Medicare program that evaluates dialysis facilities in the U.S. based on a set of quality measures, and penalizes low-performing facilities. We’ve seen a growing understanding of how social risk factors like poverty and race/ethnicity impact patient outcomes in other settings, making it difficult for providers caring for disadvantaged populations to perform as well in these kinds of pay-for-performance programs. We were interested in seeing if this was the case for dialysis facilities as well, especially since patients receiving dialysis are already a vulnerable population.
 Andrew C. Qi, Medical student
Karen E. Joynt Maddox MD MPH
Assistant professor of medicine
Washington University School of Medicine
Saint Louis, Missouri.
MedicalResearch.com: What is the background for this study?
Response: The End-Stage Renal Disease Quality Incentive Program (ESRD QIP) is a Medicare program that evaluates dialysis facilities in the U.S. based on a set of quality measures, and penalizes low-performing facilities. We’ve seen a growing understanding of how social risk factors like poverty and race/ethnicity impact patient outcomes in other settings, making it difficult for providers caring for disadvantaged populations to perform as well in these kinds of pay-for-performance programs. We were interested in seeing if this was the case for dialysis facilities as well, especially since patients receiving dialysis are already a vulnerable population.
Andrew C. Qi, Medical student
Karen E. Joynt Maddox MD MPH
Assistant professor of medicine
Washington University School of Medicine
Saint Louis, Missouri.
MedicalResearch.com: What is the background for this study?
Response: The End-Stage Renal Disease Quality Incentive Program (ESRD QIP) is a Medicare program that evaluates dialysis facilities in the U.S. based on a set of quality measures, and penalizes low-performing facilities. We’ve seen a growing understanding of how social risk factors like poverty and race/ethnicity impact patient outcomes in other settings, making it difficult for providers caring for disadvantaged populations to perform as well in these kinds of pay-for-performance programs. We were interested in seeing if this was the case for dialysis facilities as well, especially since patients receiving dialysis are already a vulnerable population.






 Dr. Childers[/caption]
Chris Childers, MD, PhD
Division of General Surgery
David Geffen School of Medicine at UCLA
Los Angeles, CA 90095
MedicalResearch.com: What is the background for this study?
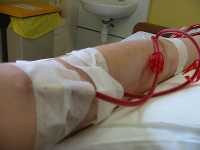
Response: Patients with end-stage renal disease – poorly functioning kidneys – often have to receive dialysis. This typically requires a patient to visit an outpatient clinic several times a week to have their blood filtered by a machine. Over the past few years, two for-profit companies have increased their control over the outpatient dialysis market – DaVita and Fresenius. Combined they control approximately ¾ of the market. A number of concerns have been raised against these for-profit companies suggesting that the quality of care they deliver may be worse than the care delivered at not-for-profit companies. But, because they control so much of the market and because patients have to receive dialysis so frequently, patients may not have much choice in the clinic they visit.
Medicare covers patients who are 65 years or older and also patients on dialysis regardless of age. Medicare pays a fixed rate for dialysis which they believe is adequate to cover the clinics' costs. However, if a patient also has private insurance, the insurer is required to pay for dialysis instead of Medicare. Whereas Medicare rates are fixed by the federal government, private insurers have to negotiate the price they pay, and may pay much more as a result.
Dr. Childers[/caption]
Chris Childers, MD, PhD
Division of General Surgery
David Geffen School of Medicine at UCLA
Los Angeles, CA 90095
MedicalResearch.com: What is the background for this study?
Response: Patients with end-stage renal disease – poorly functioning kidneys – often have to receive dialysis. This typically requires a patient to visit an outpatient clinic several times a week to have their blood filtered by a machine. Over the past few years, two for-profit companies have increased their control over the outpatient dialysis market – DaVita and Fresenius. Combined they control approximately ¾ of the market. A number of concerns have been raised against these for-profit companies suggesting that the quality of care they deliver may be worse than the care delivered at not-for-profit companies. But, because they control so much of the market and because patients have to receive dialysis so frequently, patients may not have much choice in the clinic they visit.
Medicare covers patients who are 65 years or older and also patients on dialysis regardless of age. Medicare pays a fixed rate for dialysis which they believe is adequate to cover the clinics' costs. However, if a patient also has private insurance, the insurer is required to pay for dialysis instead of Medicare. Whereas Medicare rates are fixed by the federal government, private insurers have to negotiate the price they pay, and may pay much more as a result.











 Dr. Rebholz[/caption]
Casey M. Rebholz, PhD, MS, MNSP, MPH, FAHA
Assistant Professor, Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Core Faculty, Welch Center for Prevention, Epidemiology, and Clinical Research
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Individual beverages have been previously shown to influence risk of a wide range of cardiometabolic diseases. Less is known about beverage consumption and kidney disease risk.
In this study population, we found that one such beverage pattern consisted of soda, sugar-sweetened beverages, and water, and that higher adherence to the sugar-sweetened beverage pattern was associated with greater odds of developing incident kidney disease, even after accounting for demographic characteristics and established risk factors.
Dr. Rebholz[/caption]
Casey M. Rebholz, PhD, MS, MNSP, MPH, FAHA
Assistant Professor, Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Core Faculty, Welch Center for Prevention, Epidemiology, and Clinical Research
Baltimore, MD 21287
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Individual beverages have been previously shown to influence risk of a wide range of cardiometabolic diseases. Less is known about beverage consumption and kidney disease risk.
In this study population, we found that one such beverage pattern consisted of soda, sugar-sweetened beverages, and water, and that higher adherence to the sugar-sweetened beverage pattern was associated with greater odds of developing incident kidney disease, even after accounting for demographic characteristics and established risk factors.  Dr. Nguyen[/caption]
Oanh Kieu Nguyen, MD, MA
Assistant Professor
Division of Hospital Medicine
Zuckerberg San Francisco General Hospital
UCSF
MedicalResearch.com: What is the background for this study?
Response: In U.S. citizens and permanent residents with kidney failure or end-stage renal disease (ESRD), having health insurance, Medicare, or Medicaid guarantees access to regularly scheduled hemodialysis 2-3 times per week, the evidence-based standard of care for ESRD. This treatment helps people live relatively normal lives. In 40 of 50 U.S. states, undocumented immigrants with ESRD have limited access to hemodialysis because they are not eligible for any form of federal assistance including Medicare or Medicaid, and must wait until they are life-threateningly ill to receive dialysis through a hospital emergency department, a situation called “emergency-only hemodialysis.” There are an estimated 6,500 undocumented individuals in the U.S. suffering from ESRD.
A unique opportunity made it feasible for uninsured undocumented immigrants with ESRD receiving emergency-only dialysis in Dallas, Texas, to enroll in private, commercial health insurance plans in 2015 and made it possible for researchers to compare scheduled vs. emergency-only dialysis among undocumented immigrants with ESRD. This natural experiment included 181
Dr. Nguyen[/caption]
Oanh Kieu Nguyen, MD, MA
Assistant Professor
Division of Hospital Medicine
Zuckerberg San Francisco General Hospital
UCSF
MedicalResearch.com: What is the background for this study?
Response: In U.S. citizens and permanent residents with kidney failure or end-stage renal disease (ESRD), having health insurance, Medicare, or Medicaid guarantees access to regularly scheduled hemodialysis 2-3 times per week, the evidence-based standard of care for ESRD. This treatment helps people live relatively normal lives. In 40 of 50 U.S. states, undocumented immigrants with ESRD have limited access to hemodialysis because they are not eligible for any form of federal assistance including Medicare or Medicaid, and must wait until they are life-threateningly ill to receive dialysis through a hospital emergency department, a situation called “emergency-only hemodialysis.” There are an estimated 6,500 undocumented individuals in the U.S. suffering from ESRD.
A unique opportunity made it feasible for uninsured undocumented immigrants with ESRD receiving emergency-only dialysis in Dallas, Texas, to enroll in private, commercial health insurance plans in 2015 and made it possible for researchers to compare scheduled vs. emergency-only dialysis among undocumented immigrants with ESRD. This natural experiment included 181 



 Dr. Verge[/caption]
Danilo Verge MD MBA
Vice President, CVRM Global Medical Affairs
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Dapagliflozin, an SGLT2 inhibitor (sodium-glucose co-transporter 2), has been shown to improve glycemic control by decreasing glucose reabsorption in the kidneys and inducing urinary glucose clearance. SGLT2 inhibitors have also been shown to be effective in lowering albuminuria and stabilizing eGFR (estimated glomerular filtration rate). The effect of dapagliflozin on UACR (urine albumin-to-creatinine ratio) has been shown to vary among patients.
The objective of this post-hoc analysis, based on the pooled data from 11 randomized, placebo-controlled clinical trials, was to assess baseline characteristics and concurrent changes in cardiovascular (CV) risk markers associated with UACR response to dapagliflozin.
Dr. Verge[/caption]
Danilo Verge MD MBA
Vice President, CVRM Global Medical Affairs
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Dapagliflozin, an SGLT2 inhibitor (sodium-glucose co-transporter 2), has been shown to improve glycemic control by decreasing glucose reabsorption in the kidneys and inducing urinary glucose clearance. SGLT2 inhibitors have also been shown to be effective in lowering albuminuria and stabilizing eGFR (estimated glomerular filtration rate). The effect of dapagliflozin on UACR (urine albumin-to-creatinine ratio) has been shown to vary among patients.
The objective of this post-hoc analysis, based on the pooled data from 11 randomized, placebo-controlled clinical trials, was to assess baseline characteristics and concurrent changes in cardiovascular (CV) risk markers associated with UACR response to dapagliflozin.

 Lei Qin[/caption]
Lei Qin MS
Director, Health Economics and Payer Analytics
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Renin-angiotensin-aldosterone system inhibitors (RAASi) are guideline-recommended therapies for patients with chronic kidney disease (CKD), but are commonly prescribed at suboptimal doses, which has been associated with worsening clinical outcomes. The objective of our study was to estimate the real-world associations between RAASi dose and adverse clinical outcomes in patients prescribed RAASi therapies with new-onset CKD in the UK.
Lei Qin[/caption]
Lei Qin MS
Director, Health Economics and Payer Analytics
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Renin-angiotensin-aldosterone system inhibitors (RAASi) are guideline-recommended therapies for patients with chronic kidney disease (CKD), but are commonly prescribed at suboptimal doses, which has been associated with worsening clinical outcomes. The objective of our study was to estimate the real-world associations between RAASi dose and adverse clinical outcomes in patients prescribed RAASi therapies with new-onset CKD in the UK.

 Dr. Agrawal[/caption]
Rahul Agrawal MD PhD
VP, Global Medicines Leader
AstraZeneca
MedicalResearch.com: What is the background for this study?
About the study: HARMONIZE Global is a Phase III, randomized, multicenter, double-blind, placebo-controlled trial involving 267 patients with hyperkalemia (mean potassium levels greater than 5.0 mEq/L) in 47 study locations across the Asia Pacific region, which will support registration in Japan, Taiwan, Korea and Russia.
Study design: The trial design of HARMONIZE Global is similar to HARMONIZE (NCT02088073) but evaluated two doses of LOKELMATM (sodium zirconium cyclosilicate) instead of three, as well as patients in different geographical regions.
Dr. Agrawal[/caption]
Rahul Agrawal MD PhD
VP, Global Medicines Leader
AstraZeneca
MedicalResearch.com: What is the background for this study?
About the study: HARMONIZE Global is a Phase III, randomized, multicenter, double-blind, placebo-controlled trial involving 267 patients with hyperkalemia (mean potassium levels greater than 5.0 mEq/L) in 47 study locations across the Asia Pacific region, which will support registration in Japan, Taiwan, Korea and Russia.
Study design: The trial design of HARMONIZE Global is similar to HARMONIZE (NCT02088073) but evaluated two doses of LOKELMATM (sodium zirconium cyclosilicate) instead of three, as well as patients in different geographical regions.


 Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (
Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (