MedicalResearch.com Interview with:
[caption id="attachment_36295" align="alignleft" width="160"]

Dr. El Khoudary[/caption]
Samar R. El Khoudary, Ph.D., M.P.H. BPharm, FAHA
Associate Professor
Department of Epidemiology
University of Pittsburgh Graduate School of Public Health
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study is based on the current measurements used to determine cardiovascular disease risk in postmenopausal women. Higher levels of HDL “good cholesterol” as measured by the widely available clinical test, HDL-Cholesterol, may not always be indicative of a lower risk of cardiovascular disease in postmenopausal women.
HDL is a family of particles found in the blood that vary in sizes, cholesterol contents and function. HDL particles can become dysfunctional under certain conditions such as chronic inflammation. HDL has traditionally been measured as the total cholesterol carried by the HDL particles, known as HDL cholesterol. HDL cholesterol, however, does not necessarily reflect the overall concentration, the uneven distribution, or the content and function of HDL particles.
We looked at 1,138 women aged 45 through 84 enrolled across the U.S. in the Multi-Ethnic Study of Atherosclerosis (MESA), a medical research study sponsored by the National Heart, Lung and Blood Institute of the National Institutes of Health (NIH). MESA began in 1999 and is still following participants today. We assessed two specific measurements of HDL: the number and size of the HDL particles and total cholesterol carried by HDL particles. Our study also looked at how age when women transitioned into post menopause, and the amount of time since transitioning, may impact the expected cardio-protective associations of HDL measures.
Our study points out that the traditional measure of the good cholesterol, HDL cholesterol, fails to portray an accurate depiction of heart disease risk for postmenopausal women. We reported a harmful association between higher HDL cholesterol and atherosclerosis risk that was most evident in women with older age at menopause and who were greater than, or equal to, 10 years into post menopause. In contrast to HDL cholesterol, a higher concentration of total HDL particles was associated with lower risk of atherosclerosis. Additionally, having a high number of small HDL particles was found beneficial for postmenopausal women. These findings persist irrespective of age and how long it has been since women became postmenopausal.
On the other hand, large HDL particles are linked to an increased risk of cardiovascular disease close to menopause. Women are subject to a variety of physiological changes in their sex hormones, lipids, body fat deposition and vascular health as they transition through menopause. We are hypothesizing that the decrease of estrogen, a cardio-protective sex hormone, along with other metabolic changes, can trigger chronic inflammation over time, which may alter the quality of HDL particles. Future studies should test this hypothesis.
The study findings indicate that measuring size and number of HDL particles can better reflect the well-known cardio-protective features of the good cholesterol in postmenopausal women.







 Dr. Zhong[/caption]
Victor Wenze Zhong, Ph.D.
Postdoctoral fellow
Department of Preventive Medicine
Feinberg School of Medicine
Northwestern University
Chicago, IL 60611
MedicalResearch.com: What is the background for this study?
Response: Dietary cholesterol is a common nutrient in human diet. Eggs, specially egg yolks, are the single richest source of dietary cholesterol among all commonly consumed foods. The associations between dietary cholesterol consumption and cardiovascular disease and mortality remain controversial despite decades of research. Eating less than 300 mg of dietary cholesterol per day was the guideline recommendation before 2015. However, the most recent 2015-2020 Dietary Guidelines for Americans no longer include a daily consumption limit for dietary cholesterol and recommend weekly egg consumption as part of the healthy US-style eating pattern. Whether these recommendations are appropriate have been intensely debated.
Dr. Zhong[/caption]
Victor Wenze Zhong, Ph.D.
Postdoctoral fellow
Department of Preventive Medicine
Feinberg School of Medicine
Northwestern University
Chicago, IL 60611
MedicalResearch.com: What is the background for this study?
Response: Dietary cholesterol is a common nutrient in human diet. Eggs, specially egg yolks, are the single richest source of dietary cholesterol among all commonly consumed foods. The associations between dietary cholesterol consumption and cardiovascular disease and mortality remain controversial despite decades of research. Eating less than 300 mg of dietary cholesterol per day was the guideline recommendation before 2015. However, the most recent 2015-2020 Dietary Guidelines for Americans no longer include a daily consumption limit for dietary cholesterol and recommend weekly egg consumption as part of the healthy US-style eating pattern. Whether these recommendations are appropriate have been intensely debated.





 Dr. Bollag[/caption]
Wendy Bollag, PhD, FAHA
Professor of Physiology
VA Research Career Scientist
Augusta University, Georgia
MedicalResearch.com: What is the background for this study?
Response: We have previously shown that the lipid (fat) phosphatidylglycerol (PG) is able to inhibit rapidly growing keratinocytes (skin cells) and promote their maturation. We also found that PG can suppress skin inflammation.
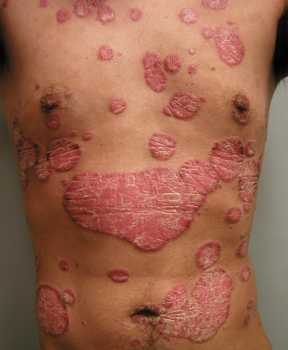
Since the common skin disease psoriasis is characterized by inflammation and excessive growth and abnormal maturation of skin cells, we believed that PG might be useful as a treatment. However, the mechanism of its anti-inflammatory effect was unknown. PG in the lung has been found to inhibit inflammation induced by microbes or their components, which work by activating the innate immune system via binding to proteins called toll-like receptors (TLRs); however, psoriasis is not considered to be an infectious disease.
We hypothesized that PG would also inhibit inflammation induced by anti-microbial peptides that activate TLRs. Anti-microbial peptides, produced normally by the skin to protect against infection, are known to be excessively up-regulated in psoriatic skin.
Dr. Bollag[/caption]
Wendy Bollag, PhD, FAHA
Professor of Physiology
VA Research Career Scientist
Augusta University, Georgia
MedicalResearch.com: What is the background for this study?
Response: We have previously shown that the lipid (fat) phosphatidylglycerol (PG) is able to inhibit rapidly growing keratinocytes (skin cells) and promote their maturation. We also found that PG can suppress skin inflammation.
Since the common skin disease psoriasis is characterized by inflammation and excessive growth and abnormal maturation of skin cells, we believed that PG might be useful as a treatment. However, the mechanism of its anti-inflammatory effect was unknown. PG in the lung has been found to inhibit inflammation induced by microbes or their components, which work by activating the innate immune system via binding to proteins called toll-like receptors (TLRs); however, psoriasis is not considered to be an infectious disease.
We hypothesized that PG would also inhibit inflammation induced by anti-microbial peptides that activate TLRs. Anti-microbial peptides, produced normally by the skin to protect against infection, are known to be excessively up-regulated in psoriatic skin.