Alzheimer's - Dementia, Author Interviews, Genetic Research, Race/Ethnic Diversity, Stanford / 21.02.2023
Stanford Study Identifies Genetic Variant Linked to Alzheimer’s in African Americans
MedicalResearch.com Interview with:
[caption id="attachment_60059" align="alignleft" width="125"] Dr. Yann Le Guen[/caption]
Yann Le Guen, Ph.D.
Assistant Director, Computational Biology
Quantitative Sciences Unit
Stanford Medicine
MedicalResearch.com: What is the background for this study?
Response: Apart from aging, the strongest contributing factor for late-onset Alzheimer’s disease is a specific allele of the APOE gene, which has three common alleles E2, E3, and E4. While E3 is the most common and considered as the reference, E2 is associated with decreased Alzheimer’s disease risk and E4 is associated with increased Alzheimer’s disease risk. Notably the prevalence of E4 among Alzheimer’s patient is high with about 60% of these carrying at least one E4 allele, while solely about 30% Americans carry one E4 allele. It’s worth emphasizing that individuals with an E4/E4 genotype have an exponential increased in their risk to develop AD (10 times as likely than the reference E3/E3 genotype), and individuals with an E3/E4 genotype have an intermediate risk.
Though, most studies of Alzheimer’s disease genetic have been focused on European ancestry, this is beginning to change thanks to NIH’s efforts to fund more studies in non-European ancestry individuals. Our study built on these recent efforts to assess the Alzheimer disease risk associated with an APOE variant (R145C) present in about ~4% African Americans, but extremely rare in Europeans.
Dr. Yann Le Guen[/caption]
Yann Le Guen, Ph.D.
Assistant Director, Computational Biology
Quantitative Sciences Unit
Stanford Medicine
MedicalResearch.com: What is the background for this study?
Response: Apart from aging, the strongest contributing factor for late-onset Alzheimer’s disease is a specific allele of the APOE gene, which has three common alleles E2, E3, and E4. While E3 is the most common and considered as the reference, E2 is associated with decreased Alzheimer’s disease risk and E4 is associated with increased Alzheimer’s disease risk. Notably the prevalence of E4 among Alzheimer’s patient is high with about 60% of these carrying at least one E4 allele, while solely about 30% Americans carry one E4 allele. It’s worth emphasizing that individuals with an E4/E4 genotype have an exponential increased in their risk to develop AD (10 times as likely than the reference E3/E3 genotype), and individuals with an E3/E4 genotype have an intermediate risk.
Though, most studies of Alzheimer’s disease genetic have been focused on European ancestry, this is beginning to change thanks to NIH’s efforts to fund more studies in non-European ancestry individuals. Our study built on these recent efforts to assess the Alzheimer disease risk associated with an APOE variant (R145C) present in about ~4% African Americans, but extremely rare in Europeans.
 Dr. Yann Le Guen[/caption]
Yann Le Guen, Ph.D.
Assistant Director, Computational Biology
Quantitative Sciences Unit
Stanford Medicine
MedicalResearch.com: What is the background for this study?
Response: Apart from aging, the strongest contributing factor for late-onset Alzheimer’s disease is a specific allele of the APOE gene, which has three common alleles E2, E3, and E4. While E3 is the most common and considered as the reference, E2 is associated with decreased Alzheimer’s disease risk and E4 is associated with increased Alzheimer’s disease risk. Notably the prevalence of E4 among Alzheimer’s patient is high with about 60% of these carrying at least one E4 allele, while solely about 30% Americans carry one E4 allele. It’s worth emphasizing that individuals with an E4/E4 genotype have an exponential increased in their risk to develop AD (10 times as likely than the reference E3/E3 genotype), and individuals with an E3/E4 genotype have an intermediate risk.
Though, most studies of Alzheimer’s disease genetic have been focused on European ancestry, this is beginning to change thanks to NIH’s efforts to fund more studies in non-European ancestry individuals. Our study built on these recent efforts to assess the Alzheimer disease risk associated with an APOE variant (R145C) present in about ~4% African Americans, but extremely rare in Europeans.
Dr. Yann Le Guen[/caption]
Yann Le Guen, Ph.D.
Assistant Director, Computational Biology
Quantitative Sciences Unit
Stanford Medicine
MedicalResearch.com: What is the background for this study?
Response: Apart from aging, the strongest contributing factor for late-onset Alzheimer’s disease is a specific allele of the APOE gene, which has three common alleles E2, E3, and E4. While E3 is the most common and considered as the reference, E2 is associated with decreased Alzheimer’s disease risk and E4 is associated with increased Alzheimer’s disease risk. Notably the prevalence of E4 among Alzheimer’s patient is high with about 60% of these carrying at least one E4 allele, while solely about 30% Americans carry one E4 allele. It’s worth emphasizing that individuals with an E4/E4 genotype have an exponential increased in their risk to develop AD (10 times as likely than the reference E3/E3 genotype), and individuals with an E3/E4 genotype have an intermediate risk.
Though, most studies of Alzheimer’s disease genetic have been focused on European ancestry, this is beginning to change thanks to NIH’s efforts to fund more studies in non-European ancestry individuals. Our study built on these recent efforts to assess the Alzheimer disease risk associated with an APOE variant (R145C) present in about ~4% African Americans, but extremely rare in Europeans.



 Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences
Dr. Holland[/caption]
Thomas M Holland, MD, MS
Assistant Professor
Rush Institute for Health Aging
Rush College of Medicine & Rush College of Health Sciences

 Response: We started many years ago by studying some natural and synthetic molecules that were able to counteract the early stages of this disease. With a view to early prevention, we wondered if these molecules could be routinely taken with the diet or dietary supplements. So our studies focused on the search for bioactive molecules present in food and edible plants.
Hops are very rich in polyphenolic compounds, and for this reason it is historically used for the production of beer, but also for the preparation of herbal teas and infusions, and its uses in traditional medicine are known. In recent years we have also collected interesting results on Coffee, Sage, Radix Imperatoriae, Cocoa and Cinnamon extracts.
Response: We started many years ago by studying some natural and synthetic molecules that were able to counteract the early stages of this disease. With a view to early prevention, we wondered if these molecules could be routinely taken with the diet or dietary supplements. So our studies focused on the search for bioactive molecules present in food and edible plants.
Hops are very rich in polyphenolic compounds, and for this reason it is historically used for the production of beer, but also for the preparation of herbal teas and infusions, and its uses in traditional medicine are known. In recent years we have also collected interesting results on Coffee, Sage, Radix Imperatoriae, Cocoa and Cinnamon extracts.






 Dr. van Dalen[/caption]
Jan Willem van Dalen, PhD
Department of Neurology
Donders Institute for Brain, Behaviour and Cognition
Radboud University Medical Centre Nijmegen
Department of Neurology
The Netherlands3Department of Public and Occupational Health
Amsterdam UMC, University of Amsterdam, Amsterdam
MedicalResearch.com: What is the background for this study?
Response: Although high systolic blood pressure in midlife has consistently been reported as a condition that increases the risk of developing dementia in old age, reports regarding this relationship in older people have been inconsistent. One potential reason for this, is that the relationship between systolic blood pressure and dementia in later life may be U-shaped, meaning that both individuals with low and with high systolic blood pressure are at increased incident dementia risk.
This study combined data from several longitudinal cohort studies specifically designed to study incident dementia in older people, to investigate whether these U-shaped relationships exist, and in which age ranges they appear. We included more than 16,500 people aged 60 and older, with over 2,700 incident dementia cases.
Also, we aimed to investigate whether these observational associations might be caused by confounding, differences in mortality, or result from opposite relationships between certain subgroups of individuals.
Dr. van Dalen[/caption]
Jan Willem van Dalen, PhD
Department of Neurology
Donders Institute for Brain, Behaviour and Cognition
Radboud University Medical Centre Nijmegen
Department of Neurology
The Netherlands3Department of Public and Occupational Health
Amsterdam UMC, University of Amsterdam, Amsterdam
MedicalResearch.com: What is the background for this study?
Response: Although high systolic blood pressure in midlife has consistently been reported as a condition that increases the risk of developing dementia in old age, reports regarding this relationship in older people have been inconsistent. One potential reason for this, is that the relationship between systolic blood pressure and dementia in later life may be U-shaped, meaning that both individuals with low and with high systolic blood pressure are at increased incident dementia risk.
This study combined data from several longitudinal cohort studies specifically designed to study incident dementia in older people, to investigate whether these U-shaped relationships exist, and in which age ranges they appear. We included more than 16,500 people aged 60 and older, with over 2,700 incident dementia cases.
Also, we aimed to investigate whether these observational associations might be caused by confounding, differences in mortality, or result from opposite relationships between certain subgroups of individuals.
 Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
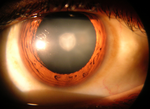
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia.
Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia. 



 Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
 Dr. Braley[/caption]
Dr. Braley[/caption]




 Dr. Willette[/caption]
Auriel Willette, PhD
Assistant Professor
Food Science and Human Nutrition
Iowa State University
MedicalResearch.com: What is the background for this study?
Response: To date, pharmacology therapies done to slow down or halt Alzheimer's disease have been inconclusive. Lifestyle interventions like changes in diet and activity are also mixed but do show some promise. Dietary clinical trials or self-reported diet have tended to focus on groups of foods such as the Mediterranean or MIND diet. To build from this excellent work, we were curious if we could pinpoint specific foods that were correlated with changes in fluid intelligence over time. Fluid intelligence represents our ability to creatively use existing knowledge, working memory, and other components of "thinking flexibly."
Further, we tested if these patterns of association differed based on genetic risk. In this case, genetic risk was defined as having a family history of Alzheimer's disease or having 1-2 "bad" copies of the Apolipoprotein E (APOE) gene, which is the strongest genetic risk factor for Alzheimer's disease.
Dr. Willette[/caption]
Auriel Willette, PhD
Assistant Professor
Food Science and Human Nutrition
Iowa State University
MedicalResearch.com: What is the background for this study?
Response: To date, pharmacology therapies done to slow down or halt Alzheimer's disease have been inconclusive. Lifestyle interventions like changes in diet and activity are also mixed but do show some promise. Dietary clinical trials or self-reported diet have tended to focus on groups of foods such as the Mediterranean or MIND diet. To build from this excellent work, we were curious if we could pinpoint specific foods that were correlated with changes in fluid intelligence over time. Fluid intelligence represents our ability to creatively use existing knowledge, working memory, and other components of "thinking flexibly."
Further, we tested if these patterns of association differed based on genetic risk. In this case, genetic risk was defined as having a family history of Alzheimer's disease or having 1-2 "bad" copies of the Apolipoprotein E (APOE) gene, which is the strongest genetic risk factor for Alzheimer's disease.
 Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
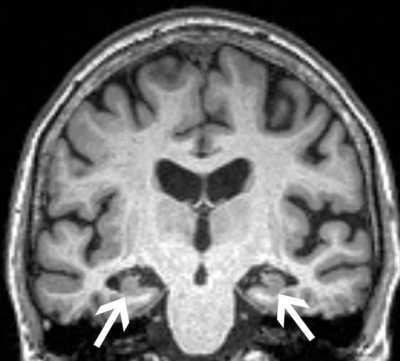
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population.
Dr. Spampinato[/caption]
Maria Vittoria Spampinato, MD
Neuroradiology Division Director
Department of Radiology and Radiological Science
Medical University of South Carolina
Charleston, SC 29425-3230
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Alzheimer’s disease (AD) represents a major public health crisis worldwide. More than 5 million people currently have AD in the United States. AD is a slowly progressing neurodegenerative brain disorder with a long preclinical phase. Many people with AD first suffer from mild cognitive impairment (MCI), a decline in cognitive abilities like memory and thinking skills that is greater than that associated with normal aging. A person with MCI is at an increased risk of developing AD or another dementia, although some individuals with MCI remain cognitively stable or improve.
Anxiety is frequently observed in individuals with MCI. The reported prevalence of anxiety in MCI patients varies between 10 and 50%. In this study we evaluated a cohort of 339 individuals with MCI participating in the Alzheimer’s Disease Neuroimaging Initiative study (ADNI2). During the five years of study participation, 72 patients experienced cognitive decline and were diagnosed with AD. We did not find difference in age, gender and education among patients with and without AD conversion. Patients who progressed had greater atrophy of the hippocampi and entorhinal cortex on their MRI scan, as expected (hippocampal atrophy is often used as a marker of neurodegeneration in AD), as well as greater prevalence of APOE4 is the strongest known genetic risk factor for AD. Patients who progressed to Alzheimer’s disease also had greater severity of anxiety during the study, as measured using the Neuropsychiatric Inventory-Questionnaire. Next we determined the effect of the MRI findings (hippocampal and entorhinal cortex atrophy), of the genetic risk factor (APOE4) and of the severity of anxiety on the time to progression to AD. We found that higher levels of anxiety were associated with faster progression from MCI to AD, independently of whether they had a genetic risk factor for Alzheimer’s disease or brain volume loss. We still need to understand better the association between anxiety disorders and cognitive decline. We do not know whether increased levels of anxiety are a consequence of cognitive decline or if anxiety exacerbates to cognitive decline. If we were able to find in the future that anxiety is actually contributing to cognitive decline, then we should more aggressively screen for anxiety disorders in the elderly population. 




 Dr. Jensen[/caption]
Majken K. Jensen, Ph.D.
Adjunct Professor of Nutrition
Harvard T.H. Chan School of Public Health &
Professor in the Department of Public Health
University of Copenhagen, Copenhagen, Denmark
MedicalResearch.com: What is the background for this study?
Response: Alzheimer’s disease and other dementias are highly prevalent conditions. According to the Alzheimer’s Association, 50 million people are currently living with Alzheimer’s disease or other dementias worldwide. Lower apolipoprotein E in plasma is a risk factor for dementia, but the underlying biological mechanisms are not fully understood. Thus, we investigated the role of apolipoprotein E overall and in lipoproteins with distinct metabolic functions in relation to cognitive function and dementia risk..
Dr. Jensen[/caption]
Majken K. Jensen, Ph.D.
Adjunct Professor of Nutrition
Harvard T.H. Chan School of Public Health &
Professor in the Department of Public Health
University of Copenhagen, Copenhagen, Denmark
MedicalResearch.com: What is the background for this study?
Response: Alzheimer’s disease and other dementias are highly prevalent conditions. According to the Alzheimer’s Association, 50 million people are currently living with Alzheimer’s disease or other dementias worldwide. Lower apolipoprotein E in plasma is a risk factor for dementia, but the underlying biological mechanisms are not fully understood. Thus, we investigated the role of apolipoprotein E overall and in lipoproteins with distinct metabolic functions in relation to cognitive function and dementia risk..






