MedicalResearch.com Interview with:
[caption id="attachment_37066" align="alignleft" width="300"]
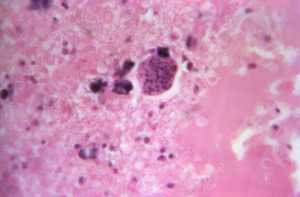
Under a magnification of 900X, this hematoxylin and eosin-stained (H&E) photomicrograph of a brain tissue specimen revealed a case of neurotoxoplasmosis in a patient who had also been diagnosed with multiple myeloma. Note the Toxoplasma gondii tissue cyst, within which bradyzoites could be seen developing. CDC Image[/caption]
Rima McLeod, M.D., F.A.C.P, F.I.D.S.A
Professor of Ophthalmology and Visual Sciences,Pediatrics (Infectious Diseases), and The College,
Director, Toxoplasmosis Center,
Senior Fellow,Institute of Genomics, Genetics and Systems Biology, Member, Commitees on Immunology, and Molecular Medicine and Pathogenesis,
Member Global Health Center, Affiliate CHeSS;
Attending Physician, Chicago Medicine,
The University of Chicago
MedicalResearch.com: What is the background for this study?
* One third of humans are infected lifelong with the brain-dwelling, protozoan parasite, Toxoplasma gondii.
* Approximately fifteen million of these have congenital toxoplasmosis.
* The parasite interconverts between slow-growing, encysted bradyzoites and rapid-growing tachyzoites.
* In mice, T. gondii creates a chronic intra-neuronal infection and an inflammatory process.
* Mice with acute and chronic infection have alterations in neurotransmitters, memory, seizures, and neurobehavior.
* Some epidemiologic-serologic studies show associations between seropositivity for T. gondii and human neurologic diseases, for example, Parkinson’s and Alzheimer’s diseases.
* Although neurobehavioral disease is associated with seropositivity, causality is unproven.
* Serologic studies of humans with diverse genetics are not optimal to detect strong associations or directionality.
* Epidemiologic associations also do not reveal parasite-modulated gene networks in human brain that could provide insights into how to cure and prevent resultant diseases.
* We need integrative approaches to examine relationships between brain parasitism and other brain diseases, to provide a foundation to identify key pathways and molecules for drug and vaccine design
* To address these problems, we considered two central questions: (i) If chronic brain parasitism associates with other neurologic diseases, what are they? And (ii) Which macromolecular networks are modulated by the parasite in human brain that lead to neuropathology which could underpin and facilitate design of treatments?
* We hypothesized that a systems approach integrating multiple levels of host parasite interactions might resolve these questions.
* To better understand what this parasite does to human brains, we performed a comprehensive systems analysis of the infected brain.
 David G. Loughrey, BA(Hons)
NEIL (Neuro Enhancement for Independent Lives) Programme
Trinity College Institute of Neuroscience, School of Medicine
Trinity College Dublin, Dublin, Ireland
MedicalResearch.com: What is the background for this study?
Response: Age-related hearing loss, a common chronic condition among older adults, has emerged in the literature as a potential modifiable risk factor for dementia. This is of interest as current pharmacological therapies for dementias such as Alzheimer’s disease only offer symptom-modifying effects. Treatment of risk factors such as hearing loss may help delay the onset of dementia and may provide an alternate therapeutic strategy. However, there is variance in the research on hearing loss and cognition with some studies reporting a small or non-significant association. In this meta-analysis, we investigated this association and we only included observational studies that used standard assessments of cognitive function and pure-tone audiometry (the clinical standard).
David G. Loughrey, BA(Hons)
NEIL (Neuro Enhancement for Independent Lives) Programme
Trinity College Institute of Neuroscience, School of Medicine
Trinity College Dublin, Dublin, Ireland
MedicalResearch.com: What is the background for this study?
Response: Age-related hearing loss, a common chronic condition among older adults, has emerged in the literature as a potential modifiable risk factor for dementia. This is of interest as current pharmacological therapies for dementias such as Alzheimer’s disease only offer symptom-modifying effects. Treatment of risk factors such as hearing loss may help delay the onset of dementia and may provide an alternate therapeutic strategy. However, there is variance in the research on hearing loss and cognition with some studies reporting a small or non-significant association. In this meta-analysis, we investigated this association and we only included observational studies that used standard assessments of cognitive function and pure-tone audiometry (the clinical standard).

























