Alzheimer's - Dementia, Author Interviews, Diabetes, JAMA, Weight Research / 09.04.2025
Study Suggests GLP-1 Obesity Drugs Associated with Lower Risk of Dementia
MedicalResearch.com Interview with:
[caption id="attachment_67848" align="alignleft" width="150"] Dr. Reddin[/caption]
Dr. Catriona Reddin MD
Fourth year Specialist Registrar in Geriatric Medicine and
an Irish Clinical Academic Training (ICAT) fellow
University Hospital Galway, Galway, Ireland
MedicalResearch.com: What is the background for this study?
Response: Dementia is a leading cause of disability globally, which is projected to affect approximately 75 million people by 2030. Diabetes mellitus is a risk factor for dementia, it was unclear if glucose lower therapies reduce the risk of dementia. The research, a systematic review and meta-analysis of 26 clinical trials involving over 160,000 participants, found that while most glucose-lowering therapies were not significantly associated with a reduction in dementia risk, one class of drugs—GLP-1Ras—was linked to a significant reduction.
Dr. Reddin[/caption]
Dr. Catriona Reddin MD
Fourth year Specialist Registrar in Geriatric Medicine and
an Irish Clinical Academic Training (ICAT) fellow
University Hospital Galway, Galway, Ireland
MedicalResearch.com: What is the background for this study?
Response: Dementia is a leading cause of disability globally, which is projected to affect approximately 75 million people by 2030. Diabetes mellitus is a risk factor for dementia, it was unclear if glucose lower therapies reduce the risk of dementia. The research, a systematic review and meta-analysis of 26 clinical trials involving over 160,000 participants, found that while most glucose-lowering therapies were not significantly associated with a reduction in dementia risk, one class of drugs—GLP-1Ras—was linked to a significant reduction.
 Dr. Reddin[/caption]
Dr. Catriona Reddin MD
Fourth year Specialist Registrar in Geriatric Medicine and
an Irish Clinical Academic Training (ICAT) fellow
University Hospital Galway, Galway, Ireland
MedicalResearch.com: What is the background for this study?
Response: Dementia is a leading cause of disability globally, which is projected to affect approximately 75 million people by 2030. Diabetes mellitus is a risk factor for dementia, it was unclear if glucose lower therapies reduce the risk of dementia. The research, a systematic review and meta-analysis of 26 clinical trials involving over 160,000 participants, found that while most glucose-lowering therapies were not significantly associated with a reduction in dementia risk, one class of drugs—GLP-1Ras—was linked to a significant reduction.
Dr. Reddin[/caption]
Dr. Catriona Reddin MD
Fourth year Specialist Registrar in Geriatric Medicine and
an Irish Clinical Academic Training (ICAT) fellow
University Hospital Galway, Galway, Ireland
MedicalResearch.com: What is the background for this study?
Response: Dementia is a leading cause of disability globally, which is projected to affect approximately 75 million people by 2030. Diabetes mellitus is a risk factor for dementia, it was unclear if glucose lower therapies reduce the risk of dementia. The research, a systematic review and meta-analysis of 26 clinical trials involving over 160,000 participants, found that while most glucose-lowering therapies were not significantly associated with a reduction in dementia risk, one class of drugs—GLP-1Ras—was linked to a significant reduction.







 Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH, MACP
Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH, MACP




 Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
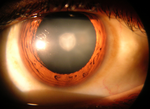
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia.
Dr. Lee[/caption]
Cecilia S. Lee, MD, MS
Associate Professor,Director, Clinical Research
Department of Ophthalmology
Harborview Medical Center
University of Washington Seattle, WA
MedicalResearch.com: What is the background for this study?
Response: Cataract is a natural aging process of the eye and affects the majority of older adults who are at risk for dementia. Sensory loss, including vision and hearing, is of interest to the research community as a possible risk factor for dementia, and also as a potential point of intervention. Because cataract surgery improves visual function, we hypothesized that older people who undergo cataract surgery may have a decreased risk of developing Alzheimer disease and dementia.
We used the longitudinal data from an ongoing, prospective, community based cohort, Adult Changes in Thought (ACT) study. The ACT study includes over 5000 participants to date who are dementia free at recruitment and followed until they develop Alzheimer disease or dementia. We had access to their extensive medical history including comprehensive ophthalmology visit data. We investigated whether cataract surgery was associated with a decreased risk of developing Alzheimer disease and dementia. 


 Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
Dr. Dunietz[/caption]
Galit Levi Dunietz MPH, PhD
Assistant Professor
 Dr. Braley[/caption]
Dr. Braley[/caption]



 Dr. Jensen[/caption]
Majken K. Jensen, Ph.D.
Adjunct Professor of Nutrition
Harvard T.H. Chan School of Public Health &
Professor in the Department of Public Health
University of Copenhagen, Copenhagen, Denmark
MedicalResearch.com: What is the background for this study?
Response: Alzheimer’s disease and other dementias are highly prevalent conditions. According to the Alzheimer’s Association, 50 million people are currently living with Alzheimer’s disease or other dementias worldwide. Lower apolipoprotein E in plasma is a risk factor for dementia, but the underlying biological mechanisms are not fully understood. Thus, we investigated the role of apolipoprotein E overall and in lipoproteins with distinct metabolic functions in relation to cognitive function and dementia risk..
Dr. Jensen[/caption]
Majken K. Jensen, Ph.D.
Adjunct Professor of Nutrition
Harvard T.H. Chan School of Public Health &
Professor in the Department of Public Health
University of Copenhagen, Copenhagen, Denmark
MedicalResearch.com: What is the background for this study?
Response: Alzheimer’s disease and other dementias are highly prevalent conditions. According to the Alzheimer’s Association, 50 million people are currently living with Alzheimer’s disease or other dementias worldwide. Lower apolipoprotein E in plasma is a risk factor for dementia, but the underlying biological mechanisms are not fully understood. Thus, we investigated the role of apolipoprotein E overall and in lipoproteins with distinct metabolic functions in relation to cognitive function and dementia risk..

 Dr. Zhang[/caption]
Ruiyuan Zhang, MD, MS
Department of Epidemiology and Biostatistics
University of Georgia College of Public Health
Athens, Georgia
MedicalResearch.com: What is the background for this study?
Response: Although there are several studies that focused on the effect of alcohol drinking on cognitive function, their findings were still mixed. So we want to use some new analysis techniques on this topic to see if we can have new findings.
MedicalResearch.com: What are the main findings?
Response: The main finding of our study is that low-to-moderate alcohol drinking is associated with better cognitive function outcomes.
Dr. Zhang[/caption]
Ruiyuan Zhang, MD, MS
Department of Epidemiology and Biostatistics
University of Georgia College of Public Health
Athens, Georgia
MedicalResearch.com: What is the background for this study?
Response: Although there are several studies that focused on the effect of alcohol drinking on cognitive function, their findings were still mixed. So we want to use some new analysis techniques on this topic to see if we can have new findings.
MedicalResearch.com: What are the main findings?
Response: The main finding of our study is that low-to-moderate alcohol drinking is associated with better cognitive function outcomes.













