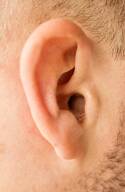
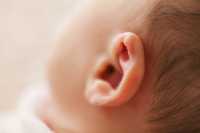
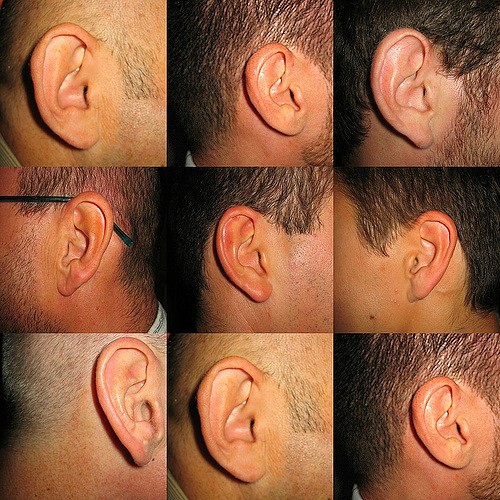
Hearing is often described as a simple act of receiving sound, but in reality it’s a deeply interactive process. Every noise, voice, or melody you encounter sets off an intricate exchange between your ears and your brain. Your brain sorts through the chaos, interprets patterns, and gives meaning to what you hear. When hearing weakens, this seamless coordination becomes strained, and the brain must work harder to keep up.
When sound input becomes faint or distorted, the brain starts compensating by trying to reconstruct what was missed. That extra mental effort drains cognitive resources that would normally support attention, memory, and comprehension. People may not notice the load they’re carrying until they begin feeling mentally tired, overwhelmed in conversation, or unable to follow speech in groups.
Hearing loss also affects the brain’s auditory centers—the areas responsible for interpreting sound and supporting higher-level thinking skills. When these pathways receive less stimulation, they can weaken, which may influence broader cognitive functions over time. This connection helps explain why untreated hearing difficulties often coincide with challenges in focus, processing, or recall.
Social behavior plays a role as well. When hearing becomes a struggle, many individuals gradually step back from group interactions or noisy environments. With fewer conversations and less meaningful auditory engagement, the brain loses important practice. This creates a circular pattern: difficulty hearing leads to less participation, which then reduces the brain’s exposure to the very stimulation that keeps it sharp.
[caption id="attachment_67762" align="aligncenter" width="500"] Source[/caption]
If you have tinnitus, it can range from aggravating to a daily agony. If you have a relatively mild case, you can often live with it fairly easily. If you have a much worse case, though, it’s distinctly difficult to get through your daily life.
Getting rid of tinnitus isn’t usually possible, though there are ways to treat it that have been proven effective. Let’s take a moment to discuss where medical science is with tinnitus research. If this condition affects you, then you will certainly want to be paying attention to this information.
Source[/caption]
If you have tinnitus, it can range from aggravating to a daily agony. If you have a relatively mild case, you can often live with it fairly easily. If you have a much worse case, though, it’s distinctly difficult to get through your daily life.
Getting rid of tinnitus isn’t usually possible, though there are ways to treat it that have been proven effective. Let’s take a moment to discuss where medical science is with tinnitus research. If this condition affects you, then you will certainly want to be paying attention to this information.
 Source[/caption]
If you have tinnitus, it can range from aggravating to a daily agony. If you have a relatively mild case, you can often live with it fairly easily. If you have a much worse case, though, it’s distinctly difficult to get through your daily life.
Getting rid of tinnitus isn’t usually possible, though there are ways to treat it that have been proven effective. Let’s take a moment to discuss where medical science is with tinnitus research. If this condition affects you, then you will certainly want to be paying attention to this information.
Source[/caption]
If you have tinnitus, it can range from aggravating to a daily agony. If you have a relatively mild case, you can often live with it fairly easily. If you have a much worse case, though, it’s distinctly difficult to get through your daily life.
Getting rid of tinnitus isn’t usually possible, though there are ways to treat it that have been proven effective. Let’s take a moment to discuss where medical science is with tinnitus research. If this condition affects you, then you will certainly want to be paying attention to this information.
Hearing Loss / 04.02.2025
The Future of Tinnitus Treatment: Breakthroughs That Could Silence the Noise
 Living with tinnitus often feels like a constant battle against sounds that refuse to fade. Whether it’s a high-pitched ringing, a steady hum, or an unpredictable buzzing, the condition can disrupt nearly every part of daily life. Sleep becomes difficult, focus weakens, and the emotional toll can be overwhelming. For years, available treatments have focused more on managing symptoms than providing lasting relief.
Now, that’s beginning to change. Advances in neuroscience, medical research, and technology are uncovering the underlying causes of tinnitus, bringing a wave of new treatments that go beyond simply masking the noise. The potential for lasting relief—or even complete elimination—feels closer than ever.
Living with tinnitus often feels like a constant battle against sounds that refuse to fade. Whether it’s a high-pitched ringing, a steady hum, or an unpredictable buzzing, the condition can disrupt nearly every part of daily life. Sleep becomes difficult, focus weakens, and the emotional toll can be overwhelming. For years, available treatments have focused more on managing symptoms than providing lasting relief.
Now, that’s beginning to change. Advances in neuroscience, medical research, and technology are uncovering the underlying causes of tinnitus, bringing a wave of new treatments that go beyond simply masking the noise. The potential for lasting relief—or even complete elimination—feels closer than ever.
Advancements in Neuromodulation Therapy
Neuromodulation is emerging as a leading approach to tinnitus treatment. Unlike conventional methods that focus on distraction or symptom management, this therapy targets the neural circuits responsible for generating phantom sounds. Techniques such as transcranial magnetic stimulation (TMS) and transcranial direct current stimulation (tDCS) aim to modify brain activity, potentially reducing tinnitus intensity. One particularly exciting development is paired stimulation, which integrates sound therapy with electrical or magnetic pulses. This approach to tinnitus patients is designed to retrain the brain’s response to tinnitus by strengthening normal auditory pathways while weakening abnormal ones. Early studies suggest that regular sessions may lead to long-term improvements, even after treatment ends. Clinics like Regain Hearing are closely monitoring these advancements, ensuring that individuals with tinnitus have access to the latest diagnostic tools and therapies as they become available.
While neuromodulation remains in the experimental stage, ongoing clinical trials continue to refine these techniques. Personalized therapies tailored to an individual’s specific tinnitus profile may soon become widely accessible, offering new options for those who have struggled to find effective solutions.
One particularly exciting development is paired stimulation, which integrates sound therapy with electrical or magnetic pulses. This approach to tinnitus patients is designed to retrain the brain’s response to tinnitus by strengthening normal auditory pathways while weakening abnormal ones. Early studies suggest that regular sessions may lead to long-term improvements, even after treatment ends. Clinics like Regain Hearing are closely monitoring these advancements, ensuring that individuals with tinnitus have access to the latest diagnostic tools and therapies as they become available.
While neuromodulation remains in the experimental stage, ongoing clinical trials continue to refine these techniques. Personalized therapies tailored to an individual’s specific tinnitus profile may soon become widely accessible, offering new options for those who have struggled to find effective solutions.
ENT / 24.12.2024
Essential Tools for Ear Care: A Closer Look at the Cerumen Hook and Jobson Horne Probe
When it comes to ear care, having the right tools can make all the difference. Whether you’re an audiologist, ENT specialist, or someone who’s simply curious about ear health, understanding the value of specialized instruments is key. Two of the most indispensable tools for earwax removal are the cerumen hook and the Jobson Horne probe. Each tool offers unique advantages and plays a vital role in ensuring safe and effective ear care.
[caption id="attachment_65669" align="aligncenter" width="333"] Photo by Gustavo Fring[/caption]
Why Tools Matter in Ear Care
Cerumen, or earwax, is a natural part of our body’s defense system. It protects the ear canal by trapping dirt and debris and preventing infections. However, when it builds up excessively, it can cause discomfort, hearing issues, or even infections. That’s where professional tools like the cerumen hook and Jobson Horne probe come in, providing a safe and efficient way to manage earwax buildup.
What Is a Cerumen Hook?
The cerumen hook is a precision tool designed specifically for the removal of hardened or deep-seated earwax. Its distinct hook-shaped tip allows practitioners to carefully extract wax without pushing it further into the canal.
Photo by Gustavo Fring[/caption]
Why Tools Matter in Ear Care
Cerumen, or earwax, is a natural part of our body’s defense system. It protects the ear canal by trapping dirt and debris and preventing infections. However, when it builds up excessively, it can cause discomfort, hearing issues, or even infections. That’s where professional tools like the cerumen hook and Jobson Horne probe come in, providing a safe and efficient way to manage earwax buildup.
What Is a Cerumen Hook?
The cerumen hook is a precision tool designed specifically for the removal of hardened or deep-seated earwax. Its distinct hook-shaped tip allows practitioners to carefully extract wax without pushing it further into the canal.
 Photo by Gustavo Fring[/caption]
Why Tools Matter in Ear Care
Cerumen, or earwax, is a natural part of our body’s defense system. It protects the ear canal by trapping dirt and debris and preventing infections. However, when it builds up excessively, it can cause discomfort, hearing issues, or even infections. That’s where professional tools like the cerumen hook and Jobson Horne probe come in, providing a safe and efficient way to manage earwax buildup.
What Is a Cerumen Hook?
The cerumen hook is a precision tool designed specifically for the removal of hardened or deep-seated earwax. Its distinct hook-shaped tip allows practitioners to carefully extract wax without pushing it further into the canal.
Photo by Gustavo Fring[/caption]
Why Tools Matter in Ear Care
Cerumen, or earwax, is a natural part of our body’s defense system. It protects the ear canal by trapping dirt and debris and preventing infections. However, when it builds up excessively, it can cause discomfort, hearing issues, or even infections. That’s where professional tools like the cerumen hook and Jobson Horne probe come in, providing a safe and efficient way to manage earwax buildup.
What Is a Cerumen Hook?
The cerumen hook is a precision tool designed specifically for the removal of hardened or deep-seated earwax. Its distinct hook-shaped tip allows practitioners to carefully extract wax without pushing it further into the canal.
Key Features:
- Precision Design: The hook’s shape makes it ideal for targeting stubborn earwax that’s difficult to reach with other tools.
- Patient Safety: It minimizes the risk of damage to the ear canal when used correctly.
- Efficiency: Perfect for removing larger chunks of wax in a controlled manner.
Author Interviews, ENT, Pediatrics, University of Pittsburgh / 13.05.2021
Ear Infections in Children: Tubes vs Medical Management Compared
MedicalResearch.com Interview with:
[caption id="attachment_57406" align="alignleft" width="200"] Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
 Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
Dr. Hoberman[/caption]
Alejandro Hoberman, M.D.
Vice Chair of Clinical Research, Division Director, General Academic Pediatrics, and Professor of Pediatrics and Clinical and Translational Science
Jack L. Paradise, MD Endowed Professor of Pediatric Research, UPMC Children's Hospital of PittsburghPresident, UPMC Children's Community Pediatrics
MedicalResearch.com: What is the background for this study?
Response: Acute otitis media (AOM) is the most frequently diagnosed illness in children in the United States for which antibiotics are prescribed. Recurrent AOM is the principal indication for tympanostomy-tube placement, the most frequently performed operation in children after the newborn period. Supporting the performance of tympanostomy-tube placement for recurrent acute otitis media has been the commonplace observation, after surgery, of acute otitis media–free periods of varying duration. Counterbalancing this view have been the cost of tympanostomy-tube placement; risks and possible late sequelae of anesthesia in young children; the possible occurrence of refractory tube otorrhea, tube blockage, premature extrusion, or dislocation of the tube into the middle-ear cavity; various structural tympanic membrane sequelae; and the possible development of mild conductive hearing loss. Tempering support for surgery is the progressive reduction in the incidence of acute otitis media that usually accompanies a child’s increasing age.
Previous trials of tympanostomy-tube placement for recurrent acute otitis media, all conducted before the introduction of pneumococcal conjugate vaccine, have given mixed results and were limited, variously, by small sample size, uncertain validity of diagnoses of acute otitis media determining trial eligibility, short periods of follow-up, and substantial attrition of participants. Official recommendations regarding tympanostomy-tube placement for children with recurrent acute otitis media differ — an otolaryngologic guideline recommends the procedure for children with recurrent acute otitis media, provided that middle-ear effusion is present in at least one ear; a contemporaneous pediatric guideline discusses tympanostomy-tube placement as an “option [that] clinicians may offer.”
Given these uncertainties, we undertook the present trial involving children 6 to 35 months of age who had a history of recurrent acute otitis media to determine whether tympanostomy-tube placement, as compared with medical management (comprising episodic antimicrobial treatment, with the option of tympanostomy-tube placement in the event of treatment failure), would result in a greater reduction in the children’s rate of recurrence of acute otitis media during the ensuing 2-year period.
Accidents & Violence, Author Interviews, ENT, JAMA / 09.12.2019
Dramatic Rise in Head and Neck Injuries Associated with Cell Phone Use
MedicalResearch.com Interview with:
Roman Povolotskiy
MD Candidate '20
Rutgers University
New Jersey Medical School
MedicalResearch.com: What is the background for this study?
Response: The idea for the study came from seeing a few patients with stories of their injuries related to cellphones. Aside from the now ubiquitous texting while driving, we also had patients who were dropping cellphones on their faces while texting in bed. We wanted to see how many head and neck injuries are related to these devices that we can’t seem to take out hands or eyes off of.
The main findings were that the incidence of cell phone related injuries has seen a dramatic rise in the recent decade, starting around the time that smart phones really started to take off. We also found that this problem is most prevalent in the adolescent and young adult age groups.
Author Interviews, Brigham & Women's - Harvard, Cost of Health Care, ENT, Surgical Research / 25.07.2019
Arcane CMS Formulas Can Over and Under Pay For ENT Surgical Services
MedicalResearch.com Interview with:
[caption id="attachment_50402" align="alignleft" width="133"] Dr. Rathi[/caption]
Vinay K. Rathi, MD
Otolaryngology Resident | Massachusetts Eye and Ear
Project Manager | Partners Ambulatory Care
MBA Candidate | Harvard Business School
MedicalResearch.com: What is the background for this study?
Response: This study is a secondary subgroup analysis that follows on the heels of a recently published study in The New England Journal of Medicine (NEJM) examining physician reimbursement for surgical procedures in the Medicare Physician Fee Schedule (PFS), which both public and private insurers use to determine payment rates for clinician services.
Although it is widely understood that physician time (i.e., the amount of physician time required to perform a procedure) is perhaps the most important factor used to determine payment rates, the Centers for Medicare and Medicaid Services (CMS) has historically relied upon limited and potentially biased survey data to estimate physician time.
Leveraging time data from American College of Surgeons National Quality Improvement Program, the authors of the recent NEJM study demonstrated that CMS does not appear to systematically misestimate intraoperative times, but there are substantial discrepancies that may result in over- or undercompensation for certain procedures and specialties.
Dr. Rathi[/caption]
Vinay K. Rathi, MD
Otolaryngology Resident | Massachusetts Eye and Ear
Project Manager | Partners Ambulatory Care
MBA Candidate | Harvard Business School
MedicalResearch.com: What is the background for this study?
Response: This study is a secondary subgroup analysis that follows on the heels of a recently published study in The New England Journal of Medicine (NEJM) examining physician reimbursement for surgical procedures in the Medicare Physician Fee Schedule (PFS), which both public and private insurers use to determine payment rates for clinician services.
Although it is widely understood that physician time (i.e., the amount of physician time required to perform a procedure) is perhaps the most important factor used to determine payment rates, the Centers for Medicare and Medicaid Services (CMS) has historically relied upon limited and potentially biased survey data to estimate physician time.
Leveraging time data from American College of Surgeons National Quality Improvement Program, the authors of the recent NEJM study demonstrated that CMS does not appear to systematically misestimate intraoperative times, but there are substantial discrepancies that may result in over- or undercompensation for certain procedures and specialties.
 Dr. Rathi[/caption]
Vinay K. Rathi, MD
Otolaryngology Resident | Massachusetts Eye and Ear
Project Manager | Partners Ambulatory Care
MBA Candidate | Harvard Business School
MedicalResearch.com: What is the background for this study?
Response: This study is a secondary subgroup analysis that follows on the heels of a recently published study in The New England Journal of Medicine (NEJM) examining physician reimbursement for surgical procedures in the Medicare Physician Fee Schedule (PFS), which both public and private insurers use to determine payment rates for clinician services.
Although it is widely understood that physician time (i.e., the amount of physician time required to perform a procedure) is perhaps the most important factor used to determine payment rates, the Centers for Medicare and Medicaid Services (CMS) has historically relied upon limited and potentially biased survey data to estimate physician time.
Leveraging time data from American College of Surgeons National Quality Improvement Program, the authors of the recent NEJM study demonstrated that CMS does not appear to systematically misestimate intraoperative times, but there are substantial discrepancies that may result in over- or undercompensation for certain procedures and specialties.
Dr. Rathi[/caption]
Vinay K. Rathi, MD
Otolaryngology Resident | Massachusetts Eye and Ear
Project Manager | Partners Ambulatory Care
MBA Candidate | Harvard Business School
MedicalResearch.com: What is the background for this study?
Response: This study is a secondary subgroup analysis that follows on the heels of a recently published study in The New England Journal of Medicine (NEJM) examining physician reimbursement for surgical procedures in the Medicare Physician Fee Schedule (PFS), which both public and private insurers use to determine payment rates for clinician services.
Although it is widely understood that physician time (i.e., the amount of physician time required to perform a procedure) is perhaps the most important factor used to determine payment rates, the Centers for Medicare and Medicaid Services (CMS) has historically relied upon limited and potentially biased survey data to estimate physician time.
Leveraging time data from American College of Surgeons National Quality Improvement Program, the authors of the recent NEJM study demonstrated that CMS does not appear to systematically misestimate intraoperative times, but there are substantial discrepancies that may result in over- or undercompensation for certain procedures and specialties.
Accidents & Violence, Author Interviews, ENT, Pediatrics / 06.06.2019
Are Some Dog Breeds More Likely to Bite?
MedicalResearch.com Interview with:
[caption id="attachment_49636" align="alignleft" width="200"] Dr. Essig[/caption]
Dr. Garth Essig, MD
Otolaryngologist
The Ohio State University Wexner Medical Center.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Dog bites are a significant yet modifiable public health concern, but the true magnitude is difficult to estimate with such wide ranges in reporting, severity of injury and varieties of breeds that bite. We reviewed bites from reports in the literature and from two regionally distinct medical centers.
We concluded that bite frequency and severity could be attributed to certain breeds in this sample, if the breed is known. Our study also acknowledged the significant risk of biting with the mixed breed population, which creates a dilemma with identification.
Dr. Essig[/caption]
Dr. Garth Essig, MD
Otolaryngologist
The Ohio State University Wexner Medical Center.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Dog bites are a significant yet modifiable public health concern, but the true magnitude is difficult to estimate with such wide ranges in reporting, severity of injury and varieties of breeds that bite. We reviewed bites from reports in the literature and from two regionally distinct medical centers.
We concluded that bite frequency and severity could be attributed to certain breeds in this sample, if the breed is known. Our study also acknowledged the significant risk of biting with the mixed breed population, which creates a dilemma with identification.
 Dr. Essig[/caption]
Dr. Garth Essig, MD
Otolaryngologist
The Ohio State University Wexner Medical Center.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Dog bites are a significant yet modifiable public health concern, but the true magnitude is difficult to estimate with such wide ranges in reporting, severity of injury and varieties of breeds that bite. We reviewed bites from reports in the literature and from two regionally distinct medical centers.
We concluded that bite frequency and severity could be attributed to certain breeds in this sample, if the breed is known. Our study also acknowledged the significant risk of biting with the mixed breed population, which creates a dilemma with identification.
Dr. Essig[/caption]
Dr. Garth Essig, MD
Otolaryngologist
The Ohio State University Wexner Medical Center.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Dog bites are a significant yet modifiable public health concern, but the true magnitude is difficult to estimate with such wide ranges in reporting, severity of injury and varieties of breeds that bite. We reviewed bites from reports in the literature and from two regionally distinct medical centers.
We concluded that bite frequency and severity could be attributed to certain breeds in this sample, if the breed is known. Our study also acknowledged the significant risk of biting with the mixed breed population, which creates a dilemma with identification.
Author Interviews, ENT / 03.06.2019
Congestion Might Mean Something Different To You and Your Doctor
MedicalResearch.com Interview with:
[caption id="attachment_49517" align="alignleft" width="138"] Dr. McCoul[/caption]
Edward McCoul, MD, MPH, FACS
Associate Professor
Director, Rhinology and Sinus Surgery
Department of Otorhinolaryngology
Ochsner Clinic
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although the potential for doctors and patients to misunderstand each other has been noted in other areas of medicine, the meaning of the word "congestion" had not previously been the subject of study. This paper calls attention to the relevance of potential communication gap in otolaryngology. This is particularly important since congestion is a major diagnostic criteria of sinusitis, which ranks nationwide in the top 5 reasons for clinical encounters year after year. If a communication gap is evident around this particular term, which is integral to establishing a diagnosis of sinusitis, then the likelihood increases that patients who present with "sinusitis" will be incorrectly diagnosed.
The process of congestion refers to the microscopic accumulation of blood and/or fluid within cells or the spaces between cells in a particular tissue or body part. When this occurs in the nose, the result is swelling inside the nose, which narrows the space for air to flow. A patient would perceive this as blockage or obstruction of airflow. This can be treated with anti-inflammatory medication that reduces swelling. Medications that clear up mucus generally are not great at reducing swelling. Many over-the-counter products are available that combine both types of medications, but using those products runs the risk of overmedication, which can have adverse consequences.
Dr. McCoul[/caption]
Edward McCoul, MD, MPH, FACS
Associate Professor
Director, Rhinology and Sinus Surgery
Department of Otorhinolaryngology
Ochsner Clinic
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although the potential for doctors and patients to misunderstand each other has been noted in other areas of medicine, the meaning of the word "congestion" had not previously been the subject of study. This paper calls attention to the relevance of potential communication gap in otolaryngology. This is particularly important since congestion is a major diagnostic criteria of sinusitis, which ranks nationwide in the top 5 reasons for clinical encounters year after year. If a communication gap is evident around this particular term, which is integral to establishing a diagnosis of sinusitis, then the likelihood increases that patients who present with "sinusitis" will be incorrectly diagnosed.
The process of congestion refers to the microscopic accumulation of blood and/or fluid within cells or the spaces between cells in a particular tissue or body part. When this occurs in the nose, the result is swelling inside the nose, which narrows the space for air to flow. A patient would perceive this as blockage or obstruction of airflow. This can be treated with anti-inflammatory medication that reduces swelling. Medications that clear up mucus generally are not great at reducing swelling. Many over-the-counter products are available that combine both types of medications, but using those products runs the risk of overmedication, which can have adverse consequences.
 Dr. McCoul[/caption]
Edward McCoul, MD, MPH, FACS
Associate Professor
Director, Rhinology and Sinus Surgery
Department of Otorhinolaryngology
Ochsner Clinic
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although the potential for doctors and patients to misunderstand each other has been noted in other areas of medicine, the meaning of the word "congestion" had not previously been the subject of study. This paper calls attention to the relevance of potential communication gap in otolaryngology. This is particularly important since congestion is a major diagnostic criteria of sinusitis, which ranks nationwide in the top 5 reasons for clinical encounters year after year. If a communication gap is evident around this particular term, which is integral to establishing a diagnosis of sinusitis, then the likelihood increases that patients who present with "sinusitis" will be incorrectly diagnosed.
The process of congestion refers to the microscopic accumulation of blood and/or fluid within cells or the spaces between cells in a particular tissue or body part. When this occurs in the nose, the result is swelling inside the nose, which narrows the space for air to flow. A patient would perceive this as blockage or obstruction of airflow. This can be treated with anti-inflammatory medication that reduces swelling. Medications that clear up mucus generally are not great at reducing swelling. Many over-the-counter products are available that combine both types of medications, but using those products runs the risk of overmedication, which can have adverse consequences.
Dr. McCoul[/caption]
Edward McCoul, MD, MPH, FACS
Associate Professor
Director, Rhinology and Sinus Surgery
Department of Otorhinolaryngology
Ochsner Clinic
New Orleans, Louisiana
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Although the potential for doctors and patients to misunderstand each other has been noted in other areas of medicine, the meaning of the word "congestion" had not previously been the subject of study. This paper calls attention to the relevance of potential communication gap in otolaryngology. This is particularly important since congestion is a major diagnostic criteria of sinusitis, which ranks nationwide in the top 5 reasons for clinical encounters year after year. If a communication gap is evident around this particular term, which is integral to establishing a diagnosis of sinusitis, then the likelihood increases that patients who present with "sinusitis" will be incorrectly diagnosed.
The process of congestion refers to the microscopic accumulation of blood and/or fluid within cells or the spaces between cells in a particular tissue or body part. When this occurs in the nose, the result is swelling inside the nose, which narrows the space for air to flow. A patient would perceive this as blockage or obstruction of airflow. This can be treated with anti-inflammatory medication that reduces swelling. Medications that clear up mucus generally are not great at reducing swelling. Many over-the-counter products are available that combine both types of medications, but using those products runs the risk of overmedication, which can have adverse consequences.
Author Interviews, Cancer Research, ENT, JAMA, Surgical Research / 06.11.2018
Treatment Delays Linked To High Mortality for Head and Neck Cancer
MedicalResearch.com Interview with:
[caption id="attachment_45744" align="alignleft" width="200"] Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
 Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
Author Interviews, End of Life Care, Hearing Loss, JAMA / 28.09.2018
Hyperbaric Oxygen Therapy Can Salvage Hearing In Some Sensorineural Loss Cases
MedicalResearch.com Interview with:
Tae-Min Rhee, M.D.
Chief of Undersea and Diving Medicine,
Underwater Medical Institute,
National Maritime Medical Center,
Republic of Korea Navy, Changwon
Republic of Korea
MedicalResearch.com: What is the background for this study?
Response: The sudden sensorineural hearing loss (SSNHL) has an incidence of 5 to 20 per 100,000 person-years in the general population and sometimes results in permanent deafness followed by considerable socio-economic costs. The causes of SSNHL are often unclear, and in these cases there are no treatment of choice that is proven to be effective. In addition, spontaneous recovery is not uncommon in SSNHL, making it difficult to predict the natural course of the disease, and thus a well-controlled clinical trial is rare in spite of its clinical significance.
Many treatment options (systemic or intratympanic steroids, antiviral agents, vasodilators, and hyperbaric oxygen therapy) have been suggested and tried to date, but only systemic steroid therapy has been the most effective among them. However, for the cases with contraindications to steroids, or steroid-refractory SSNHL, there is paucity of information on the second line treatment option.
Hyperbaric oxygen therapy (HBOT), i.e., high-pressurized oxygen therapy, is a method of treating patients within a chamber saturated with 100% oxygen maintained at a high pressure of 2.0 to 2.5 atm. Cochlea is an organ that relies more on the diffusion of oxygen than the direct vascular supply, and thus it is known to be vulnerable to ischemia. Since this is suggested as one of the main pathophysiology of SSNHL, we wanted to prove the hypothesis that, by providing high-pressure oxygen, the partial pressure of oxygen delivered to the inner ear is maximized, and the additional or complementary therapeutic effects can be observed. A number of reports have been published for 20 years, but there is no systematically organized evidence except a Cochrane Review in 2012. Therefore, our research team tried to integrate the evidence through a comprehensive meta-analysis and to provide important clues for further research.
Author Interviews, Cancer Research, Cost of Health Care, ENT, HPV, JAMA, Surgical Research / 18.09.2018
Access to Treatment for Head/Neck Cancer Patients Improved with Medicaid Expansion
MedicalResearch.com Interview with:
[caption id="attachment_44611" align="alignleft" width="133"] Dr. Cannon[/caption]
Richard B. Cannon, MD
Division of Otolaryngology–Head and Neck Surgery
School of Medicine
University of Utah, Salt Lake City
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Patient Protection and Affordable Care Act (ACA) is a nationwide effort to reduce the number of uninsured individuals in the United States and increase access to health care. This legislation is commonly debated and objective data is needed to evaluate its impact. As a head and neck cancer surgeon, I sought to evaluate how the ACA had specifically influenced my patients. Main findings below:
MedicalResearch.com: What should readers take away from your report?
Response: This population-based study found an increase in the percentage of patients enrolled in Medicaid and private insurance and a large decrease in the rates of uninsured patients after implementation of the Patient Protection and Affordable Care Act (ACA). This change was only seen in states that adopted the Medicaid expansion in 2014. The decrease in the rate of uninsured patients was significant, 6.2% before versus 3.0% after. Patients who were uninsured prior to the Patient Protection and Affordable Care Act had poorer survival outcomes.
Dr. Cannon[/caption]
Richard B. Cannon, MD
Division of Otolaryngology–Head and Neck Surgery
School of Medicine
University of Utah, Salt Lake City
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Patient Protection and Affordable Care Act (ACA) is a nationwide effort to reduce the number of uninsured individuals in the United States and increase access to health care. This legislation is commonly debated and objective data is needed to evaluate its impact. As a head and neck cancer surgeon, I sought to evaluate how the ACA had specifically influenced my patients. Main findings below:
MedicalResearch.com: What should readers take away from your report?
Response: This population-based study found an increase in the percentage of patients enrolled in Medicaid and private insurance and a large decrease in the rates of uninsured patients after implementation of the Patient Protection and Affordable Care Act (ACA). This change was only seen in states that adopted the Medicaid expansion in 2014. The decrease in the rate of uninsured patients was significant, 6.2% before versus 3.0% after. Patients who were uninsured prior to the Patient Protection and Affordable Care Act had poorer survival outcomes.
 Dr. Cannon[/caption]
Richard B. Cannon, MD
Division of Otolaryngology–Head and Neck Surgery
School of Medicine
University of Utah, Salt Lake City
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Patient Protection and Affordable Care Act (ACA) is a nationwide effort to reduce the number of uninsured individuals in the United States and increase access to health care. This legislation is commonly debated and objective data is needed to evaluate its impact. As a head and neck cancer surgeon, I sought to evaluate how the ACA had specifically influenced my patients. Main findings below:
MedicalResearch.com: What should readers take away from your report?
Response: This population-based study found an increase in the percentage of patients enrolled in Medicaid and private insurance and a large decrease in the rates of uninsured patients after implementation of the Patient Protection and Affordable Care Act (ACA). This change was only seen in states that adopted the Medicaid expansion in 2014. The decrease in the rate of uninsured patients was significant, 6.2% before versus 3.0% after. Patients who were uninsured prior to the Patient Protection and Affordable Care Act had poorer survival outcomes.
Dr. Cannon[/caption]
Richard B. Cannon, MD
Division of Otolaryngology–Head and Neck Surgery
School of Medicine
University of Utah, Salt Lake City
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Patient Protection and Affordable Care Act (ACA) is a nationwide effort to reduce the number of uninsured individuals in the United States and increase access to health care. This legislation is commonly debated and objective data is needed to evaluate its impact. As a head and neck cancer surgeon, I sought to evaluate how the ACA had specifically influenced my patients. Main findings below:
MedicalResearch.com: What should readers take away from your report?
Response: This population-based study found an increase in the percentage of patients enrolled in Medicaid and private insurance and a large decrease in the rates of uninsured patients after implementation of the Patient Protection and Affordable Care Act (ACA). This change was only seen in states that adopted the Medicaid expansion in 2014. The decrease in the rate of uninsured patients was significant, 6.2% before versus 3.0% after. Patients who were uninsured prior to the Patient Protection and Affordable Care Act had poorer survival outcomes.
Author Interviews, ENT, Environmental Risks, Occupational Health / 06.09.2018
Microwave Radiation Targeting Diplomats in Cuba and China Resembles Traumatic Brain Injury
MedicalResearch.com Interview with:
[caption id="attachment_44250" align="alignleft" width="173"] Dr. Golomb[/caption]
Beatrice Golomb, MD, PhD
Director of the Golomb Research Group
Professor of Medicine
University of California, San DiegoResponse:
MedicalResearch.com: What is the background for this study? How was the radiation emitted?
Response: Possibilities include surveillance devices (or things to jam them), electronic weapons, or, less likely, “innocent” communications devices.
MedicalResearch.com: What are the main findings?
Response: That all key features of diplomats’ experiences comport with pulsed radiofrequency/ microwave (RF/MW) radiation.
Dr. Golomb[/caption]
Beatrice Golomb, MD, PhD
Director of the Golomb Research Group
Professor of Medicine
University of California, San DiegoResponse:
MedicalResearch.com: What is the background for this study? How was the radiation emitted?
Response: Possibilities include surveillance devices (or things to jam them), electronic weapons, or, less likely, “innocent” communications devices.
MedicalResearch.com: What are the main findings?
Response: That all key features of diplomats’ experiences comport with pulsed radiofrequency/ microwave (RF/MW) radiation.
 Dr. Golomb[/caption]
Beatrice Golomb, MD, PhD
Director of the Golomb Research Group
Professor of Medicine
University of California, San DiegoResponse:
MedicalResearch.com: What is the background for this study? How was the radiation emitted?
Response: Possibilities include surveillance devices (or things to jam them), electronic weapons, or, less likely, “innocent” communications devices.
MedicalResearch.com: What are the main findings?
Response: That all key features of diplomats’ experiences comport with pulsed radiofrequency/ microwave (RF/MW) radiation.
Dr. Golomb[/caption]
Beatrice Golomb, MD, PhD
Director of the Golomb Research Group
Professor of Medicine
University of California, San DiegoResponse:
MedicalResearch.com: What is the background for this study? How was the radiation emitted?
Response: Possibilities include surveillance devices (or things to jam them), electronic weapons, or, less likely, “innocent” communications devices.
MedicalResearch.com: What are the main findings?
Response: That all key features of diplomats’ experiences comport with pulsed radiofrequency/ microwave (RF/MW) radiation.
- The nature of the “sounds” heard – chirping, clicking, ringing, grinding/buzzing – are known “sounds” produced via the “microwave auditory effect” aka Frey effect. Different sounds are heard by different people, because the character of the sound heard depends on head dimensions (as well as pulse characteristics). Sounds were primarily heard at night: consistent with the microwave auditory effect, which requires low ambient noise. Some diplomats reported that sounds were spatially localized with “laserlike” specificity – said to defy known physics. This defies the physics of sound, but not radiation. The “sound” was reported to follow a diplomat as he walked, within the territory in which it was heard. Sound from a fixed source does not seem to follow people – but the microwave auditory affect does, often perceived as being located just behind (or in some cases just above, or inside) the head of the person, irrespective of the person’s orientation relative to the radiation source.
- The symptoms reported following these experiences also fit. Rates of reported symptoms in diplomats – headache, cognitive and sleep problems dominating, then dizziness, tinnitus, anxiety, nausea at lesser but still high rates – match closely with rates of the same symptoms reported in a 2012 Japanese study of people who report health effects from radiation, typically including pulsed RF/MW. Hearing loss is a relatively distinctive and prominent symptom in both diplomats, and RF/MW affected civilians. In both groups, some reportedly experience speech problems, balance problems, nosebleed, and strange sensations of vibration and pressure.
- Hundreds (if not thousands) of studies have illuminated mechanisms by which these effects may arise, centered on oxidative stress (the kind of injury that antioxidants help to defend against) – and many downstream effects of oxidative stress (membrane damage, blood brain barrier impairment with potential for brain swelling, inflammation, voltage gated calcium (and other) channel effects (which can also lead to oxidative stress), mitochondrial impairment, autoimmune activation, etc.)
- There is precedent for use of microwaves in the diplomat setting. It is known that the US embassy in Moscow was microwaved for several decades beginning in the early 1950s (with some embassy staff citing – disputed - health problems). A 1976 NY Times story (“Moscow rays linked to U.S. bugging”) referenced speculation these were for surveillance; the Soviets claimed their purpose was to thwart U.S. listening devices on the roof of the embassy.
Author Interviews, ENT, JAMA, NIH / 17.08.2018
Who Suffers From Phantom Smells?
MedicalResearch.com Interview with:
 Kathleen Bainbridge, PhD
Epidemiology and Biostatistics Program
NIDCD
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The causes of phantom odor perception are not understood. This study looked for the prevalence and risk factors for this disorder. We found that that 1 in 15 Americans (or 6.5 percent) over the age of 40 experiences phantom odors.
This study, is the first in the U.S. to use nationally representative data to examine the prevalence of and risk factors for phantom odor perception. The study included about 7,400 adults who participated in the National Health and Nutrition Examination Survey, a continuous survey conducted by the National Center for Health Statistics which is part of the Centers for Disease Control and Prevention. The study could inform future research aiming to unlock the mysteries of phantom odors.
We identified risk factors that may be related to the perception of phantom odors. People are more likely to experience this condition if they are female, and are relatively young—we found a higher prevalence in 40-60 year-olds compared to 60+ year-olds. Other risk factors include head injury, dry mouth, poor overall health, and low socio-economic status. People with lower socio-economic status may have health conditions that contribute to phantom odors, either directly or because of medications needed to treat their health conditions.
Kathleen Bainbridge, PhD
Epidemiology and Biostatistics Program
NIDCD
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The causes of phantom odor perception are not understood. This study looked for the prevalence and risk factors for this disorder. We found that that 1 in 15 Americans (or 6.5 percent) over the age of 40 experiences phantom odors.
This study, is the first in the U.S. to use nationally representative data to examine the prevalence of and risk factors for phantom odor perception. The study included about 7,400 adults who participated in the National Health and Nutrition Examination Survey, a continuous survey conducted by the National Center for Health Statistics which is part of the Centers for Disease Control and Prevention. The study could inform future research aiming to unlock the mysteries of phantom odors.
We identified risk factors that may be related to the perception of phantom odors. People are more likely to experience this condition if they are female, and are relatively young—we found a higher prevalence in 40-60 year-olds compared to 60+ year-olds. Other risk factors include head injury, dry mouth, poor overall health, and low socio-economic status. People with lower socio-economic status may have health conditions that contribute to phantom odors, either directly or because of medications needed to treat their health conditions.
 Kathleen Bainbridge, PhD
Epidemiology and Biostatistics Program
NIDCD
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The causes of phantom odor perception are not understood. This study looked for the prevalence and risk factors for this disorder. We found that that 1 in 15 Americans (or 6.5 percent) over the age of 40 experiences phantom odors.
This study, is the first in the U.S. to use nationally representative data to examine the prevalence of and risk factors for phantom odor perception. The study included about 7,400 adults who participated in the National Health and Nutrition Examination Survey, a continuous survey conducted by the National Center for Health Statistics which is part of the Centers for Disease Control and Prevention. The study could inform future research aiming to unlock the mysteries of phantom odors.
We identified risk factors that may be related to the perception of phantom odors. People are more likely to experience this condition if they are female, and are relatively young—we found a higher prevalence in 40-60 year-olds compared to 60+ year-olds. Other risk factors include head injury, dry mouth, poor overall health, and low socio-economic status. People with lower socio-economic status may have health conditions that contribute to phantom odors, either directly or because of medications needed to treat their health conditions.
Kathleen Bainbridge, PhD
Epidemiology and Biostatistics Program
NIDCD
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The causes of phantom odor perception are not understood. This study looked for the prevalence and risk factors for this disorder. We found that that 1 in 15 Americans (or 6.5 percent) over the age of 40 experiences phantom odors.
This study, is the first in the U.S. to use nationally representative data to examine the prevalence of and risk factors for phantom odor perception. The study included about 7,400 adults who participated in the National Health and Nutrition Examination Survey, a continuous survey conducted by the National Center for Health Statistics which is part of the Centers for Disease Control and Prevention. The study could inform future research aiming to unlock the mysteries of phantom odors.
We identified risk factors that may be related to the perception of phantom odors. People are more likely to experience this condition if they are female, and are relatively young—we found a higher prevalence in 40-60 year-olds compared to 60+ year-olds. Other risk factors include head injury, dry mouth, poor overall health, and low socio-economic status. People with lower socio-economic status may have health conditions that contribute to phantom odors, either directly or because of medications needed to treat their health conditions.
Author Interviews, Cancer Research, ENT, HPV / 25.07.2018
Head and Neck Cancer Survivors at Risk of Secondary Cancers, esp if They Smoke
MedicalResearch.com Interview with:
[caption id="attachment_43416" align="alignleft" width="200"] Dr. Boakye[/caption]
Eric Adjei PhD, MA
Saint Louis University Center for Health Outcomes Research (SLUCOR)
St. Louis, Missouri
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Survivors of head and neck cancer (HNC) develop second primary cancers (SPCs) at a higher rate than most common cancers. This is concerning because the number of HNC survivors are increasing due to advancements in treatment and technology. Patients whose head and neck cancer was caused by smoking and alcohol are different than those whose HNC were caused by human papillomavirus (HPV). We therefore used data from 2000-2014 National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) 18 database to examine if the incidence and the type of SPC that patients with smoking-related HNC develop were different from those from HPV-related head and neck cancer.
First, independent of group of HNC (HPV-related or not), we found that SPCs among survivors of head and neck cancer were high, with about 1-in-8 patients developing an SPC. Additionally, irrespective of whether the index . head and neck cancer was from smoking-related or HPV-related, the majority of SPCs were second malignancies in head and neck region (e.g. tongue, gum, mouth floor etc), lung and esophagus. However, we observed different incidence rates between the two groups. Patients with smoking-related head and neck cancer developed SPCs at a higher rate (14%) than those with HPV-related HNC (10%).
Dr. Boakye[/caption]
Eric Adjei PhD, MA
Saint Louis University Center for Health Outcomes Research (SLUCOR)
St. Louis, Missouri
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Survivors of head and neck cancer (HNC) develop second primary cancers (SPCs) at a higher rate than most common cancers. This is concerning because the number of HNC survivors are increasing due to advancements in treatment and technology. Patients whose head and neck cancer was caused by smoking and alcohol are different than those whose HNC were caused by human papillomavirus (HPV). We therefore used data from 2000-2014 National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) 18 database to examine if the incidence and the type of SPC that patients with smoking-related HNC develop were different from those from HPV-related head and neck cancer.
First, independent of group of HNC (HPV-related or not), we found that SPCs among survivors of head and neck cancer were high, with about 1-in-8 patients developing an SPC. Additionally, irrespective of whether the index . head and neck cancer was from smoking-related or HPV-related, the majority of SPCs were second malignancies in head and neck region (e.g. tongue, gum, mouth floor etc), lung and esophagus. However, we observed different incidence rates between the two groups. Patients with smoking-related head and neck cancer developed SPCs at a higher rate (14%) than those with HPV-related HNC (10%).
 Dr. Boakye[/caption]
Eric Adjei PhD, MA
Saint Louis University Center for Health Outcomes Research (SLUCOR)
St. Louis, Missouri
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Survivors of head and neck cancer (HNC) develop second primary cancers (SPCs) at a higher rate than most common cancers. This is concerning because the number of HNC survivors are increasing due to advancements in treatment and technology. Patients whose head and neck cancer was caused by smoking and alcohol are different than those whose HNC were caused by human papillomavirus (HPV). We therefore used data from 2000-2014 National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) 18 database to examine if the incidence and the type of SPC that patients with smoking-related HNC develop were different from those from HPV-related head and neck cancer.
First, independent of group of HNC (HPV-related or not), we found that SPCs among survivors of head and neck cancer were high, with about 1-in-8 patients developing an SPC. Additionally, irrespective of whether the index . head and neck cancer was from smoking-related or HPV-related, the majority of SPCs were second malignancies in head and neck region (e.g. tongue, gum, mouth floor etc), lung and esophagus. However, we observed different incidence rates between the two groups. Patients with smoking-related head and neck cancer developed SPCs at a higher rate (14%) than those with HPV-related HNC (10%).
Dr. Boakye[/caption]
Eric Adjei PhD, MA
Saint Louis University Center for Health Outcomes Research (SLUCOR)
St. Louis, Missouri
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Survivors of head and neck cancer (HNC) develop second primary cancers (SPCs) at a higher rate than most common cancers. This is concerning because the number of HNC survivors are increasing due to advancements in treatment and technology. Patients whose head and neck cancer was caused by smoking and alcohol are different than those whose HNC were caused by human papillomavirus (HPV). We therefore used data from 2000-2014 National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) 18 database to examine if the incidence and the type of SPC that patients with smoking-related HNC develop were different from those from HPV-related head and neck cancer.
First, independent of group of HNC (HPV-related or not), we found that SPCs among survivors of head and neck cancer were high, with about 1-in-8 patients developing an SPC. Additionally, irrespective of whether the index . head and neck cancer was from smoking-related or HPV-related, the majority of SPCs were second malignancies in head and neck region (e.g. tongue, gum, mouth floor etc), lung and esophagus. However, we observed different incidence rates between the two groups. Patients with smoking-related head and neck cancer developed SPCs at a higher rate (14%) than those with HPV-related HNC (10%).
Author Interviews, ENT, JAMA, Neurology, Pain Research / 17.07.2018
Migraine Management Crucial For Treatment of Tinnitus
MedicalResearch.com Interview with: Jen-Tsung Lai, MD Department of Otolaryngology Kuang-Tien General Hospital Shalu, Taichung, Taiwan MedicalResearch.com: What is the background for this study? What are the main...
Annals Internal Medicine, Author Interviews, ENT, Environmental Risks, Hearing Loss / 19.04.2018
LOUD Outdoor Concerts Lead To Temporary Hearing Loss, esp in Men
 MedicalResearch.com Interview with:
Dr. Véronique J. C. Kraaijenga MD
Department of Otorhinolaryngology–Head and Neck Surgery
Brain Center Rudolf Magnus, University Medical Center Utrecht, Utrecht, the Netherlands
MedicalResearch.com: What is the background for this study?
Response: During the past two decades, the frequency of hearing loss among young people has increased and going to music concerts, clubs and festivals may part of the reason. Noise-induced hearing loss because of recreational noise exposure is reduced by using earplugs.
Our study evaluated 51 adults who attended an outdoor music festival in Amsterdam, the Netherlands, in September 2015. The study measured music festival visit for 4.5 hours (intervention); temporary hearing loss (outcome).
MedicalResearch.com Interview with:
Dr. Véronique J. C. Kraaijenga MD
Department of Otorhinolaryngology–Head and Neck Surgery
Brain Center Rudolf Magnus, University Medical Center Utrecht, Utrecht, the Netherlands
MedicalResearch.com: What is the background for this study?
Response: During the past two decades, the frequency of hearing loss among young people has increased and going to music concerts, clubs and festivals may part of the reason. Noise-induced hearing loss because of recreational noise exposure is reduced by using earplugs.
Our study evaluated 51 adults who attended an outdoor music festival in Amsterdam, the Netherlands, in September 2015. The study measured music festival visit for 4.5 hours (intervention); temporary hearing loss (outcome).
Author Interviews, ENT, JAMA, Surgical Research / 02.03.2018
Selfies Distort Your Face and Make Your Nose Look Bigger
MedicalResearch.com Interview with:
[caption id="attachment_40303" align="alignleft" width="142"] Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
 Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
Dr. Paskhover[/caption]
Boris Paskhover, MD
Rutgers New Jersey Medical School
Adjunct Instructor,Department of Otolaryngology-Head and Neck Surgery
NYU Langone Medical Center
MedicalResearch.com: What is the background for this study?
Response: Patient's and the general public routinely mention that their nose appears large, especially when they look at photos taken with their phone. I realized that patients in general are taking selfies more often nowadays. In my training, we routinely would tell patient’s not to use selfies as a marker of how they look, and we instead would take a 5ft distance photograph since we knew that is more realistic. I looked through the medical literature, and it appeared to me that no one had thoroughly discussed why selfies are a bad when evaluating the nose. I contacted a colleague at Stanford who has a PhD with interest in computer graphics and we developed a model for the face/nose.
Accidents & Violence, Author Interviews, Emergency Care, ENT, JAMA / 21.12.2017
Cotton Tip Applicators Single Biggest Cause of Eardrum Ruptures
 MedicalResearch.com Interview with:
Eric T. Carniol, MD, MBA
Division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology–Head and Neck Surgery, University of Toronto
Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Tympanic membrane perforations (aka "popped" or "burst" ear drum) is a common complaint of patients presenting to the emergency room, primary care offices, and otolaryngologist (ENT doctors) offices. These may be caused by trauma, infections, or other causes. As well, many patients will use qtips (cotton-tipped applicators) to clean ears and remove ear wax and are unaware of the potential harms of doing so.
This study was designed to examine the cause of ear drum perforations as diagnosed in emergency departments in the United States.
Foreign body instrumentation of the ear (qtips, hair combs, hair pins, needles, etc) were the cause of 61.2% of perforations. Cotton tip applicators are the single leading cause of traumatic tympanic membrane perforation in all age groups except young adults (13-18) and 19-36 year olds, in which it is the second largest cause (behind water trauma).
Children less than 18 years old constitute nearly 2/3 of all ear drum perforations in the emergency department.
MedicalResearch.com Interview with:
Eric T. Carniol, MD, MBA
Division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology–Head and Neck Surgery, University of Toronto
Toronto, Ontario, Canada
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Tympanic membrane perforations (aka "popped" or "burst" ear drum) is a common complaint of patients presenting to the emergency room, primary care offices, and otolaryngologist (ENT doctors) offices. These may be caused by trauma, infections, or other causes. As well, many patients will use qtips (cotton-tipped applicators) to clean ears and remove ear wax and are unaware of the potential harms of doing so.
This study was designed to examine the cause of ear drum perforations as diagnosed in emergency departments in the United States.
Foreign body instrumentation of the ear (qtips, hair combs, hair pins, needles, etc) were the cause of 61.2% of perforations. Cotton tip applicators are the single leading cause of traumatic tympanic membrane perforation in all age groups except young adults (13-18) and 19-36 year olds, in which it is the second largest cause (behind water trauma).
Children less than 18 years old constitute nearly 2/3 of all ear drum perforations in the emergency department.
Author Interviews, ENT, Surgical Research / 22.09.2017
Mild Hypothermia During Prolonged Surgery May Reduce Complications
MedicalResearch.com Interview with:
[caption id="attachment_36885" align="alignleft" width="114"] Dr. Miles[/caption]
Brett A. Miles, DDS MD FACS
Associate Professor of Otolaryngology Head and Neck Surgery
Co-Chief Division Head and Neck Oncology
Fellowship Director
Head and Neck Oncologic and Microvascular Reconstructive Surgery
Department of Otolaryngology Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, NY 10029
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ideal core temperature for patients undergoing prolonged major head and neck surgery remains unknown. Previous data indicates the low temperatures may increase the risk of developing postoperative complications such as tissue loss, hematomas, or surgical infections.(1) Other studies have indicated that high temperatures may also influence outcomes and lead to increased complications such as bleeding.(2)
This study was a study of 519 patients who underwent major head and neck surgery at the Mount Sinai Hospital, New York, New York. The study looked at the core temperature of the patients during prolonged surgery for head and neck cancer in order to identify the optimal temperature range for these patients to prevent complications.
The study found that higher intraoperative temperatures were associated with worse outcomes in terms of tissue loss, wound complications, and infection. Our study suggests an optimal temperature range of 35.3C-37.6C. If patients were above or below that range for a significant period of time, their complications increased. Therefore maintaining this temperature range (mild hypothermia) may improve flap outcomes in this population.
Dr. Miles[/caption]
Brett A. Miles, DDS MD FACS
Associate Professor of Otolaryngology Head and Neck Surgery
Co-Chief Division Head and Neck Oncology
Fellowship Director
Head and Neck Oncologic and Microvascular Reconstructive Surgery
Department of Otolaryngology Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, NY 10029
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ideal core temperature for patients undergoing prolonged major head and neck surgery remains unknown. Previous data indicates the low temperatures may increase the risk of developing postoperative complications such as tissue loss, hematomas, or surgical infections.(1) Other studies have indicated that high temperatures may also influence outcomes and lead to increased complications such as bleeding.(2)
This study was a study of 519 patients who underwent major head and neck surgery at the Mount Sinai Hospital, New York, New York. The study looked at the core temperature of the patients during prolonged surgery for head and neck cancer in order to identify the optimal temperature range for these patients to prevent complications.
The study found that higher intraoperative temperatures were associated with worse outcomes in terms of tissue loss, wound complications, and infection. Our study suggests an optimal temperature range of 35.3C-37.6C. If patients were above or below that range for a significant period of time, their complications increased. Therefore maintaining this temperature range (mild hypothermia) may improve flap outcomes in this population.
 Dr. Miles[/caption]
Brett A. Miles, DDS MD FACS
Associate Professor of Otolaryngology Head and Neck Surgery
Co-Chief Division Head and Neck Oncology
Fellowship Director
Head and Neck Oncologic and Microvascular Reconstructive Surgery
Department of Otolaryngology Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, NY 10029
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ideal core temperature for patients undergoing prolonged major head and neck surgery remains unknown. Previous data indicates the low temperatures may increase the risk of developing postoperative complications such as tissue loss, hematomas, or surgical infections.(1) Other studies have indicated that high temperatures may also influence outcomes and lead to increased complications such as bleeding.(2)
This study was a study of 519 patients who underwent major head and neck surgery at the Mount Sinai Hospital, New York, New York. The study looked at the core temperature of the patients during prolonged surgery for head and neck cancer in order to identify the optimal temperature range for these patients to prevent complications.
The study found that higher intraoperative temperatures were associated with worse outcomes in terms of tissue loss, wound complications, and infection. Our study suggests an optimal temperature range of 35.3C-37.6C. If patients were above or below that range for a significant period of time, their complications increased. Therefore maintaining this temperature range (mild hypothermia) may improve flap outcomes in this population.
Dr. Miles[/caption]
Brett A. Miles, DDS MD FACS
Associate Professor of Otolaryngology Head and Neck Surgery
Co-Chief Division Head and Neck Oncology
Fellowship Director
Head and Neck Oncologic and Microvascular Reconstructive Surgery
Department of Otolaryngology Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, NY 10029
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The ideal core temperature for patients undergoing prolonged major head and neck surgery remains unknown. Previous data indicates the low temperatures may increase the risk of developing postoperative complications such as tissue loss, hematomas, or surgical infections.(1) Other studies have indicated that high temperatures may also influence outcomes and lead to increased complications such as bleeding.(2)
This study was a study of 519 patients who underwent major head and neck surgery at the Mount Sinai Hospital, New York, New York. The study looked at the core temperature of the patients during prolonged surgery for head and neck cancer in order to identify the optimal temperature range for these patients to prevent complications.
The study found that higher intraoperative temperatures were associated with worse outcomes in terms of tissue loss, wound complications, and infection. Our study suggests an optimal temperature range of 35.3C-37.6C. If patients were above or below that range for a significant period of time, their complications increased. Therefore maintaining this temperature range (mild hypothermia) may improve flap outcomes in this population.
Author Interviews, Endocrinology, ENT, Surgical Research / 11.09.2017
Risk Factors For Reoperation and Readmission After Parathyroidectomy Identified
MedicalResearch.com Interview with:
[caption id="attachment_36879" align="alignleft" width="114"] Dr. Rai[/caption]
Raymond L. Chai, MD
Assistant Professor of Otolaryngology
Icahn School of Medicine at Mount Sinai.
MedicalResearch.com: What is the background for this study?
Response: Primary hyperparathyroidism is a common endocrine disorder affecting up to 1% of the general population. Surgical intervention is the only known durable cure for the disease. Untreated primary hyperparathyroidism can lead to number of health problems, including progressive osteoporosis and kidney stones. Although parathyroidectomy is a commonly performed surgical procedure by otolaryngologists, limited data exists regarding risk factors and rates of reoperation and readmission following surgery.
Dr. Rai[/caption]
Raymond L. Chai, MD
Assistant Professor of Otolaryngology
Icahn School of Medicine at Mount Sinai.
MedicalResearch.com: What is the background for this study?
Response: Primary hyperparathyroidism is a common endocrine disorder affecting up to 1% of the general population. Surgical intervention is the only known durable cure for the disease. Untreated primary hyperparathyroidism can lead to number of health problems, including progressive osteoporosis and kidney stones. Although parathyroidectomy is a commonly performed surgical procedure by otolaryngologists, limited data exists regarding risk factors and rates of reoperation and readmission following surgery.
 Dr. Rai[/caption]
Raymond L. Chai, MD
Assistant Professor of Otolaryngology
Icahn School of Medicine at Mount Sinai.
MedicalResearch.com: What is the background for this study?
Response: Primary hyperparathyroidism is a common endocrine disorder affecting up to 1% of the general population. Surgical intervention is the only known durable cure for the disease. Untreated primary hyperparathyroidism can lead to number of health problems, including progressive osteoporosis and kidney stones. Although parathyroidectomy is a commonly performed surgical procedure by otolaryngologists, limited data exists regarding risk factors and rates of reoperation and readmission following surgery.
Dr. Rai[/caption]
Raymond L. Chai, MD
Assistant Professor of Otolaryngology
Icahn School of Medicine at Mount Sinai.
MedicalResearch.com: What is the background for this study?
Response: Primary hyperparathyroidism is a common endocrine disorder affecting up to 1% of the general population. Surgical intervention is the only known durable cure for the disease. Untreated primary hyperparathyroidism can lead to number of health problems, including progressive osteoporosis and kidney stones. Although parathyroidectomy is a commonly performed surgical procedure by otolaryngologists, limited data exists regarding risk factors and rates of reoperation and readmission following surgery.
Author Interviews, ENT, JAMA, Obstructive Sleep Apnea, Sleep Disorders, UT Southwestern / 02.03.2017
Obstructive Sleep Apnea More Common In Obese Adolescents With Enlarged Tonsils
MedicalResearch.com Interview with:
[caption id="attachment_32582" align="alignleft" width="132"] Dr. Ron Mitchell[/caption]
Ron B. Mitchell, MD
Professor and Vice Chairman,
Department of Otolaryngology, Head and Neck Surgery
William Beckner Distinguished Chair in Otolaryngology
Chief of Pediatric Otolaryngology
UT Southwestern and Children's Medical Center Dallas
Dallas, TX 75207
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Obstructive Sleep Apnea (OSA) has not been widely studies in adolescents. This is one of a few studies that was targeted at 12-17 year olds who were referred for a sleep study for possible OSA. The study included 224 adolescents (53% male). aged 12 to 17 years. The mean BMI was 33.4 and most were either Hispanic or African American (85.3%). A total of 148 (66.1%) were obese. Most adolescents referred for a sleep study (68%), had Obstructive Sleep Apnea. Normal-weight adolescents were least likely to have OSA at 48%, while obese children were most likely at 77%. Severe OSA was most likely in obese males with tonsillar hypertrophy.
Dr. Ron Mitchell[/caption]
Ron B. Mitchell, MD
Professor and Vice Chairman,
Department of Otolaryngology, Head and Neck Surgery
William Beckner Distinguished Chair in Otolaryngology
Chief of Pediatric Otolaryngology
UT Southwestern and Children's Medical Center Dallas
Dallas, TX 75207
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Obstructive Sleep Apnea (OSA) has not been widely studies in adolescents. This is one of a few studies that was targeted at 12-17 year olds who were referred for a sleep study for possible OSA. The study included 224 adolescents (53% male). aged 12 to 17 years. The mean BMI was 33.4 and most were either Hispanic or African American (85.3%). A total of 148 (66.1%) were obese. Most adolescents referred for a sleep study (68%), had Obstructive Sleep Apnea. Normal-weight adolescents were least likely to have OSA at 48%, while obese children were most likely at 77%. Severe OSA was most likely in obese males with tonsillar hypertrophy.
 Dr. Ron Mitchell[/caption]
Ron B. Mitchell, MD
Professor and Vice Chairman,
Department of Otolaryngology, Head and Neck Surgery
William Beckner Distinguished Chair in Otolaryngology
Chief of Pediatric Otolaryngology
UT Southwestern and Children's Medical Center Dallas
Dallas, TX 75207
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Obstructive Sleep Apnea (OSA) has not been widely studies in adolescents. This is one of a few studies that was targeted at 12-17 year olds who were referred for a sleep study for possible OSA. The study included 224 adolescents (53% male). aged 12 to 17 years. The mean BMI was 33.4 and most were either Hispanic or African American (85.3%). A total of 148 (66.1%) were obese. Most adolescents referred for a sleep study (68%), had Obstructive Sleep Apnea. Normal-weight adolescents were least likely to have OSA at 48%, while obese children were most likely at 77%. Severe OSA was most likely in obese males with tonsillar hypertrophy.
Dr. Ron Mitchell[/caption]
Ron B. Mitchell, MD
Professor and Vice Chairman,
Department of Otolaryngology, Head and Neck Surgery
William Beckner Distinguished Chair in Otolaryngology
Chief of Pediatric Otolaryngology
UT Southwestern and Children's Medical Center Dallas
Dallas, TX 75207
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Obstructive Sleep Apnea (OSA) has not been widely studies in adolescents. This is one of a few studies that was targeted at 12-17 year olds who were referred for a sleep study for possible OSA. The study included 224 adolescents (53% male). aged 12 to 17 years. The mean BMI was 33.4 and most were either Hispanic or African American (85.3%). A total of 148 (66.1%) were obese. Most adolescents referred for a sleep study (68%), had Obstructive Sleep Apnea. Normal-weight adolescents were least likely to have OSA at 48%, while obese children were most likely at 77%. Severe OSA was most likely in obese males with tonsillar hypertrophy.
Author Interviews, Brigham & Women's - Harvard, ENT, Neurological Disorders / 30.11.2016
Vestibular or Inner Ear System Weakens After Age 40
MedicalResearch.com Interview with:
[caption id="attachment_30046" align="alignleft" width="150"] Dr. Daniel M. Merfeld[/caption]
Daniel M. Merfeld, Ph.D.
Professor of Otolaryngology
Harvard Medical School
Massachusetts Eye and Ear
Director, Jenks Vestibular Physiology Laboratory
Senior Scientist
MedicalResearch.com: What is the background for this study?
Response: Nearly half of the population will see a clinician at some point in their lives with symptoms related to the vestibular system (e.g., dizziness, vertigo, imbalance and blurred vision). The vestibular system, made up of tiny fluid-filled membranes in the inner ear, is responsible for receiving information about motion, balance and spatial orientation. With the goal of determining whether age affected the function of the vestibular system, our research team administered balance and motion tests to 105 healthy people ranging from 18 to 80 years old and measured their vestibular thresholds (“threshold” refers to the smallest possible motion administered that the subject is able to perceive correctly).
Dr. Daniel M. Merfeld[/caption]
Daniel M. Merfeld, Ph.D.
Professor of Otolaryngology
Harvard Medical School
Massachusetts Eye and Ear
Director, Jenks Vestibular Physiology Laboratory
Senior Scientist
MedicalResearch.com: What is the background for this study?
Response: Nearly half of the population will see a clinician at some point in their lives with symptoms related to the vestibular system (e.g., dizziness, vertigo, imbalance and blurred vision). The vestibular system, made up of tiny fluid-filled membranes in the inner ear, is responsible for receiving information about motion, balance and spatial orientation. With the goal of determining whether age affected the function of the vestibular system, our research team administered balance and motion tests to 105 healthy people ranging from 18 to 80 years old and measured their vestibular thresholds (“threshold” refers to the smallest possible motion administered that the subject is able to perceive correctly).
 Dr. Daniel M. Merfeld[/caption]
Daniel M. Merfeld, Ph.D.
Professor of Otolaryngology
Harvard Medical School
Massachusetts Eye and Ear
Director, Jenks Vestibular Physiology Laboratory
Senior Scientist
MedicalResearch.com: What is the background for this study?
Response: Nearly half of the population will see a clinician at some point in their lives with symptoms related to the vestibular system (e.g., dizziness, vertigo, imbalance and blurred vision). The vestibular system, made up of tiny fluid-filled membranes in the inner ear, is responsible for receiving information about motion, balance and spatial orientation. With the goal of determining whether age affected the function of the vestibular system, our research team administered balance and motion tests to 105 healthy people ranging from 18 to 80 years old and measured their vestibular thresholds (“threshold” refers to the smallest possible motion administered that the subject is able to perceive correctly).
Dr. Daniel M. Merfeld[/caption]
Daniel M. Merfeld, Ph.D.
Professor of Otolaryngology
Harvard Medical School
Massachusetts Eye and Ear
Director, Jenks Vestibular Physiology Laboratory
Senior Scientist
MedicalResearch.com: What is the background for this study?
Response: Nearly half of the population will see a clinician at some point in their lives with symptoms related to the vestibular system (e.g., dizziness, vertigo, imbalance and blurred vision). The vestibular system, made up of tiny fluid-filled membranes in the inner ear, is responsible for receiving information about motion, balance and spatial orientation. With the goal of determining whether age affected the function of the vestibular system, our research team administered balance and motion tests to 105 healthy people ranging from 18 to 80 years old and measured their vestibular thresholds (“threshold” refers to the smallest possible motion administered that the subject is able to perceive correctly).
Author Interviews, Cancer Research, ENT, JAMA, Radiation Therapy, Stanford / 15.11.2016
Post-Op Radiotherapy Improved Survival In Oral Cavity and Oropharyngeal Squamous Cell Carcinoma
MedicalResearch.com Interview with:
[caption id="attachment_29579" align="alignleft" width="188"] Dr. Michelle Chen[/caption]
Michelle M. Chen, MD/MHS
Department of Otolaryngology- Head and Neck Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The benefit of post-operative radiotherapy (PORT) for patients with T1-T2 N1 oral cavity and oropharyngeal cancer without adverse pathologic features is unclear. Starting in 2014, the national guidelines no longer recommended consideration of post-operative radiotherapy for N1 oropharyngeal cancer patients, but left it as a consideration for N1 oral cavity cancer patients. We found that post-operative radiotherapy was associated with improved survival in both oral cavity and oropharyngeal cancers, particularly in patients younger than 70 years of age and those with T2 disease.
Dr. Michelle Chen[/caption]
Michelle M. Chen, MD/MHS
Department of Otolaryngology- Head and Neck Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The benefit of post-operative radiotherapy (PORT) for patients with T1-T2 N1 oral cavity and oropharyngeal cancer without adverse pathologic features is unclear. Starting in 2014, the national guidelines no longer recommended consideration of post-operative radiotherapy for N1 oropharyngeal cancer patients, but left it as a consideration for N1 oral cavity cancer patients. We found that post-operative radiotherapy was associated with improved survival in both oral cavity and oropharyngeal cancers, particularly in patients younger than 70 years of age and those with T2 disease.
 Dr. Michelle Chen[/caption]
Michelle M. Chen, MD/MHS
Department of Otolaryngology- Head and Neck Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The benefit of post-operative radiotherapy (PORT) for patients with T1-T2 N1 oral cavity and oropharyngeal cancer without adverse pathologic features is unclear. Starting in 2014, the national guidelines no longer recommended consideration of post-operative radiotherapy for N1 oropharyngeal cancer patients, but left it as a consideration for N1 oral cavity cancer patients. We found that post-operative radiotherapy was associated with improved survival in both oral cavity and oropharyngeal cancers, particularly in patients younger than 70 years of age and those with T2 disease.
Dr. Michelle Chen[/caption]
Michelle M. Chen, MD/MHS
Department of Otolaryngology- Head and Neck Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The benefit of post-operative radiotherapy (PORT) for patients with T1-T2 N1 oral cavity and oropharyngeal cancer without adverse pathologic features is unclear. Starting in 2014, the national guidelines no longer recommended consideration of post-operative radiotherapy for N1 oropharyngeal cancer patients, but left it as a consideration for N1 oral cavity cancer patients. We found that post-operative radiotherapy was associated with improved survival in both oral cavity and oropharyngeal cancers, particularly in patients younger than 70 years of age and those with T2 disease.
Author Interviews, Cancer Research, ENT, HPV / 04.10.2016
Epidemic of HPV Associated Throat Cancer in Men
MedicalResearch.com Interview with:
[caption id="attachment_28537" align="alignleft" width="133"] Dr. Eric Genden[/caption]
Eric M Genden, MD, FACS
Isidore Friesner Professor and Chairman
Department of Otolaryngology-Head and Neck Surgery
The Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this report? How has the clinical picture of HPV infections of oral and throat cancers changed over the past two decades?
Response: There has been no change however there has been a epidemic of viral induced throat cancer in men. The HPV virus has been established a the causative agent in cervical cancer in women. It has now been identified as a major causative agent in tonsillar and base of tongue cancer.
Dr. Eric Genden[/caption]
Eric M Genden, MD, FACS
Isidore Friesner Professor and Chairman
Department of Otolaryngology-Head and Neck Surgery
The Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this report? How has the clinical picture of HPV infections of oral and throat cancers changed over the past two decades?
Response: There has been no change however there has been a epidemic of viral induced throat cancer in men. The HPV virus has been established a the causative agent in cervical cancer in women. It has now been identified as a major causative agent in tonsillar and base of tongue cancer.
 Dr. Eric Genden[/caption]
Eric M Genden, MD, FACS
Isidore Friesner Professor and Chairman
Department of Otolaryngology-Head and Neck Surgery
The Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this report? How has the clinical picture of HPV infections of oral and throat cancers changed over the past two decades?
Response: There has been no change however there has been a epidemic of viral induced throat cancer in men. The HPV virus has been established a the causative agent in cervical cancer in women. It has now been identified as a major causative agent in tonsillar and base of tongue cancer.
Dr. Eric Genden[/caption]
Eric M Genden, MD, FACS
Isidore Friesner Professor and Chairman
Department of Otolaryngology-Head and Neck Surgery
The Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this report? How has the clinical picture of HPV infections of oral and throat cancers changed over the past two decades?
Response: There has been no change however there has been a epidemic of viral induced throat cancer in men. The HPV virus has been established a the causative agent in cervical cancer in women. It has now been identified as a major causative agent in tonsillar and base of tongue cancer.
Author Interviews, Biomarkers, Cancer Research, ENT, HPV / 03.10.2016
Cell Biomarkers To Distinguish Deadly From Less Aggressive HPV Oral Cancers
MedicalResearch.com Interview with:
[caption id="attachment_28510" align="alignleft" width="200"] Dr. Elizabeth Franzmann[/caption]
Elizabeth Franzmann, M.D.
Scientific Founder and Chief Scientific Officer
Vigilant Biosciences
MedicalResearch.com: What is the background for this study?
Response: Head and neck cancer involves cancers of the oral cavity, oropharynx and larynx. It is difficult to treat. Part of the challenge is that it is distinguishing the patients with tumors that are going to behave aggressively from those with less aggressive disease. As a result, many patients undergo treatment that may be more intensive and morbid than they need while others need more aggressive treatment. Tissue markers associated with prognosis may be able to help clinicians differentiate patients who need more aggressive treatment from those whose treatment can be less intensive. CD44 is a cell surface glycoprotein and tumor-initiating marker. CD44 and another surface protein, EGFR, are involved in tumor extension and are associated with poor prognosis. Certain forms of Human Papillomavirus (HPV) are known to cause oropharyngeal cancer and are associated with a good prognosis. P16 is a surrogate marker for the kind of HPV that causes cancer. Understanding the relationships between how these markers are expressed in cancer tissue may direct patient treatment in the future.
Dr. Elizabeth Franzmann[/caption]
Elizabeth Franzmann, M.D.
Scientific Founder and Chief Scientific Officer
Vigilant Biosciences
MedicalResearch.com: What is the background for this study?
Response: Head and neck cancer involves cancers of the oral cavity, oropharynx and larynx. It is difficult to treat. Part of the challenge is that it is distinguishing the patients with tumors that are going to behave aggressively from those with less aggressive disease. As a result, many patients undergo treatment that may be more intensive and morbid than they need while others need more aggressive treatment. Tissue markers associated with prognosis may be able to help clinicians differentiate patients who need more aggressive treatment from those whose treatment can be less intensive. CD44 is a cell surface glycoprotein and tumor-initiating marker. CD44 and another surface protein, EGFR, are involved in tumor extension and are associated with poor prognosis. Certain forms of Human Papillomavirus (HPV) are known to cause oropharyngeal cancer and are associated with a good prognosis. P16 is a surrogate marker for the kind of HPV that causes cancer. Understanding the relationships between how these markers are expressed in cancer tissue may direct patient treatment in the future.
 Dr. Elizabeth Franzmann[/caption]
Elizabeth Franzmann, M.D.
Scientific Founder and Chief Scientific Officer
Vigilant Biosciences
MedicalResearch.com: What is the background for this study?
Response: Head and neck cancer involves cancers of the oral cavity, oropharynx and larynx. It is difficult to treat. Part of the challenge is that it is distinguishing the patients with tumors that are going to behave aggressively from those with less aggressive disease. As a result, many patients undergo treatment that may be more intensive and morbid than they need while others need more aggressive treatment. Tissue markers associated with prognosis may be able to help clinicians differentiate patients who need more aggressive treatment from those whose treatment can be less intensive. CD44 is a cell surface glycoprotein and tumor-initiating marker. CD44 and another surface protein, EGFR, are involved in tumor extension and are associated with poor prognosis. Certain forms of Human Papillomavirus (HPV) are known to cause oropharyngeal cancer and are associated with a good prognosis. P16 is a surrogate marker for the kind of HPV that causes cancer. Understanding the relationships between how these markers are expressed in cancer tissue may direct patient treatment in the future.
Dr. Elizabeth Franzmann[/caption]
Elizabeth Franzmann, M.D.
Scientific Founder and Chief Scientific Officer
Vigilant Biosciences
MedicalResearch.com: What is the background for this study?
Response: Head and neck cancer involves cancers of the oral cavity, oropharynx and larynx. It is difficult to treat. Part of the challenge is that it is distinguishing the patients with tumors that are going to behave aggressively from those with less aggressive disease. As a result, many patients undergo treatment that may be more intensive and morbid than they need while others need more aggressive treatment. Tissue markers associated with prognosis may be able to help clinicians differentiate patients who need more aggressive treatment from those whose treatment can be less intensive. CD44 is a cell surface glycoprotein and tumor-initiating marker. CD44 and another surface protein, EGFR, are involved in tumor extension and are associated with poor prognosis. Certain forms of Human Papillomavirus (HPV) are known to cause oropharyngeal cancer and are associated with a good prognosis. P16 is a surrogate marker for the kind of HPV that causes cancer. Understanding the relationships between how these markers are expressed in cancer tissue may direct patient treatment in the future.
Author Interviews, ENT, Surgical Research / 22.09.2016
Decision-Making in Laryngology: Both Sides of the Story
MedicalResearch.com Interview with:
[caption id="attachment_28269" align="alignleft" width="133"] Dr. Mark Courey[/caption]
Dr. Mark Courey, MD
Senior Faculty,Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in voice disorders?
Response: I became interested in voice disorders because during my residency in the late 1980’s there was little known about how to help patients with disorders of voice. The main instrument we use to evaluate vocal folds (the stroboscope) was just becoming clinically available. Only a handful of physicians had one available. We could not see vocal fold function and could only see the lesions on the vocal folds. We did not know how the lesions affected function. So many surgeons only treated patients with laryngeal cancer and told the others to be happy that they did not have cancer.
Dr. Mark Courey[/caption]
Dr. Mark Courey, MD
Senior Faculty,Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in voice disorders?
Response: I became interested in voice disorders because during my residency in the late 1980’s there was little known about how to help patients with disorders of voice. The main instrument we use to evaluate vocal folds (the stroboscope) was just becoming clinically available. Only a handful of physicians had one available. We could not see vocal fold function and could only see the lesions on the vocal folds. We did not know how the lesions affected function. So many surgeons only treated patients with laryngeal cancer and told the others to be happy that they did not have cancer.
 Dr. Mark Courey[/caption]
Dr. Mark Courey, MD
Senior Faculty,Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in voice disorders?
Response: I became interested in voice disorders because during my residency in the late 1980’s there was little known about how to help patients with disorders of voice. The main instrument we use to evaluate vocal folds (the stroboscope) was just becoming clinically available. Only a handful of physicians had one available. We could not see vocal fold function and could only see the lesions on the vocal folds. We did not know how the lesions affected function. So many surgeons only treated patients with laryngeal cancer and told the others to be happy that they did not have cancer.
Dr. Mark Courey[/caption]
Dr. Mark Courey, MD
Senior Faculty,Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in voice disorders?
Response: I became interested in voice disorders because during my residency in the late 1980’s there was little known about how to help patients with disorders of voice. The main instrument we use to evaluate vocal folds (the stroboscope) was just becoming clinically available. Only a handful of physicians had one available. We could not see vocal fold function and could only see the lesions on the vocal folds. We did not know how the lesions affected function. So many surgeons only treated patients with laryngeal cancer and told the others to be happy that they did not have cancer.
Author Interviews, ENT, Surgical Research / 22.09.2016
ENT Surgeon Manages Middle Ear Cholesteatoma Removal In One Surgical Procedure
MedicalResearch.com Interview with:
[caption id="attachment_28267" align="alignleft" width="160"] Dr. Eric E Smouha[/caption]
Eric E Smouha, MD
Professor, Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and specifically middle ear problems?
Response: I am a neurotologist, i.e. , ENT physician specialized in disorders of the ear and skull base. Neurotologists treat problems of the middle ear and inner ear. Middle ear problems are interesting because they are prevalent, and surgery frequently results in restoration of function.
Dr. Eric E Smouha[/caption]
Eric E Smouha, MD
Professor, Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and specifically middle ear problems?
Response: I am a neurotologist, i.e. , ENT physician specialized in disorders of the ear and skull base. Neurotologists treat problems of the middle ear and inner ear. Middle ear problems are interesting because they are prevalent, and surgery frequently results in restoration of function.
 Dr. Eric E Smouha[/caption]
Eric E Smouha, MD
Professor, Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and specifically middle ear problems?
Response: I am a neurotologist, i.e. , ENT physician specialized in disorders of the ear and skull base. Neurotologists treat problems of the middle ear and inner ear. Middle ear problems are interesting because they are prevalent, and surgery frequently results in restoration of function.
Dr. Eric E Smouha[/caption]
Eric E Smouha, MD
Professor, Otolaryngology
The Mount Sinai Hospital
New York Eye and Ear Infirmary of Mount Sinai
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and specifically middle ear problems?
Response: I am a neurotologist, i.e. , ENT physician specialized in disorders of the ear and skull base. Neurotologists treat problems of the middle ear and inner ear. Middle ear problems are interesting because they are prevalent, and surgery frequently results in restoration of function.
Author Interviews, ENT, Surgical Research, Technology / 22.09.2016
3D Models and Immersive Virtual Reality Simulation for Complex Skull Base Surgery
MedicalResearch.com Interview with:
[caption id="attachment_28265" align="alignleft" width="160"] Dr. Alfred Marc Calo Iloreta[/caption]
Alfred Marc Calo Iloreta, MD
Assistant Professor
Skull Base Surgery and Rhinology
Department of Otolaryngology -
Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, New York
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and your subspecialty in particular?
Response: I am a ENT/Head and Neck Surgeon practicing in Manhattan at the Mount Sinai Hospital. I trained here in New York City for residency and also completed a fellowship in Rhinology and Skull Base Surgery.
I chose this field and sub-specialty because of the intricate and complex anatomy of the head and neck. In addition rhinology and skull base surgery utilizes multiple advanced technologies from high definition optics, to neuronavigation to allow us to work with this complex anatomy.
Dr. Alfred Marc Calo Iloreta[/caption]
Alfred Marc Calo Iloreta, MD
Assistant Professor
Skull Base Surgery and Rhinology
Department of Otolaryngology -
Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, New York
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and your subspecialty in particular?
Response: I am a ENT/Head and Neck Surgeon practicing in Manhattan at the Mount Sinai Hospital. I trained here in New York City for residency and also completed a fellowship in Rhinology and Skull Base Surgery.
I chose this field and sub-specialty because of the intricate and complex anatomy of the head and neck. In addition rhinology and skull base surgery utilizes multiple advanced technologies from high definition optics, to neuronavigation to allow us to work with this complex anatomy.
 Dr. Alfred Marc Calo Iloreta[/caption]
Alfred Marc Calo Iloreta, MD
Assistant Professor
Skull Base Surgery and Rhinology
Department of Otolaryngology -
Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, New York
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and your subspecialty in particular?
Response: I am a ENT/Head and Neck Surgeon practicing in Manhattan at the Mount Sinai Hospital. I trained here in New York City for residency and also completed a fellowship in Rhinology and Skull Base Surgery.
I chose this field and sub-specialty because of the intricate and complex anatomy of the head and neck. In addition rhinology and skull base surgery utilizes multiple advanced technologies from high definition optics, to neuronavigation to allow us to work with this complex anatomy.
Dr. Alfred Marc Calo Iloreta[/caption]
Alfred Marc Calo Iloreta, MD
Assistant Professor
Skull Base Surgery and Rhinology
Department of Otolaryngology -
Head and Neck Surgery
Icahn School of Medicine at Mount Sinai
New York, New York
MedicalResearch.com: Would you tell us a little about yourself? How did you become interested in ENT and your subspecialty in particular?
Response: I am a ENT/Head and Neck Surgeon practicing in Manhattan at the Mount Sinai Hospital. I trained here in New York City for residency and also completed a fellowship in Rhinology and Skull Base Surgery.
I chose this field and sub-specialty because of the intricate and complex anatomy of the head and neck. In addition rhinology and skull base surgery utilizes multiple advanced technologies from high definition optics, to neuronavigation to allow us to work with this complex anatomy.
Author Interviews, ENT, Surgical Research / 21.09.2016
An answer for eschar buildup: anti-stick solution for electrosurgery
MedicalResearch.com Interview with
 Tim Reese, president of Eagle Surgical Products, LLC,
Sales and distribution company for Electro Lube®
MedicalResearch.com: What is the background of Electro Lube®?
Response: Developed in 2004, Electro Lube® is an anti-stick solution for electrosurgery designed to keep instruments clean. The product is a mixture of natural, non-synthetic, non-flammable, non-allergenic biocompatible phospholipids without any known side effects associated with patient use.
Tim Reese, president of Eagle Surgical Products, LLC,
Sales and distribution company for Electro Lube®
MedicalResearch.com: What is the background of Electro Lube®?
Response: Developed in 2004, Electro Lube® is an anti-stick solution for electrosurgery designed to keep instruments clean. The product is a mixture of natural, non-synthetic, non-flammable, non-allergenic biocompatible phospholipids without any known side effects associated with patient use.
 Tim Reese, president of Eagle Surgical Products, LLC,
Sales and distribution company for Electro Lube®
MedicalResearch.com: What is the background of Electro Lube®?
Response: Developed in 2004, Electro Lube® is an anti-stick solution for electrosurgery designed to keep instruments clean. The product is a mixture of natural, non-synthetic, non-flammable, non-allergenic biocompatible phospholipids without any known side effects associated with patient use.
Tim Reese, president of Eagle Surgical Products, LLC,
Sales and distribution company for Electro Lube®
MedicalResearch.com: What is the background of Electro Lube®?
Response: Developed in 2004, Electro Lube® is an anti-stick solution for electrosurgery designed to keep instruments clean. The product is a mixture of natural, non-synthetic, non-flammable, non-allergenic biocompatible phospholipids without any known side effects associated with patient use.
- 1
- 2