MedicalResearch.com Interview with:
Dr Dilip Kachhawa, MD
Department of Skin & Venereal Disease
Dr Sampurnanand Medical College
Jodhpur, Rajasthan, India
MedicalResearch.com: What are the main findings?
[caption id="attachment_59328" align="alignleft" width="150"]
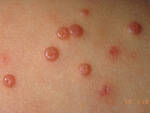
Molluscum DermNet image[/caption]
Response: Molluscum Contagiosum (MC) is an infection caused by molluscipoxvirus. It is difficult to study since the virus only survives in human skin, and therefore there isn’t an animal or cell model to study potential treatments. Molluscum lesions appear as raised, domed shaped skin-colored lesions and can occur anywhere on the body but are most common on the face, neck, arms, legs, and abdomen. Sometimes there are few lesions, but clusters of several lesions can appear. Children are the most likely to get molluscum, and the virus is highly contagious, transmitted by direct contact with infected skin or contaminated objects, like towels, linens and toys. Scratching can cause autoinoculation which is when a person reinfects themself.
MC is very common, impacting an estimated 6 million adults and mostly children in the US each year. In 2010, there was an estimated 122 million cases worldwide. It occurs primarily in humid and warm climates, and transmission via swimming pools and bathtubs may be possible. Therefore, molluscum is often called “water warts.”
Many physicians may take a “watch and wait” approach since the virus may clear on its own. However, it can take months to up to 5 years for some to experience complete clearance, In the meantime, the person is still highly contagious and may spread the virus to others, particularly children. Lesions can be bothersome, causing itching and sometimes a secondary infection. There is also a psychosocial component. In a recent study, 1 in 10 children with molluscum experienced a major quality of life issue.
Berdazimer Gel, 10.3% is a potential first-in-class topical controlled-nitric oxide releasing medication containing Berdazimer (sodium), a new chemical entity, and the active ingredient in berdazimer gel 10.3%. The mechanism of action of berdazimer in the treatment of molluscum is unknown, but in vitro lab studies show that the nitric oxide, released when berdazimer is combined with a hydrogel, may impede viral replication and perhaps help body’s natural immune response against molluscum.
 Laura Gould[/caption]
Laura Gould, MSc, MA, PT
Research Scientist
SUDC Registry and Research Collaborative
Comprehensive Epilepsy Center
Department of Neurology
NYU Langone Grossman School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Sudden Unexplained death in childhood (SUDC) is the unexplained death of a child on or after their 1st birthday that remains unexplained after a comprehensive death investigation. About 400 SUDC occur annually between the ages of 1-18, but more than half occur in toddlers, aged 1-4 years. Since most deaths are sleep related and unwitnessed with unremarkable autopsies, mechanisms of deaths have eluded our understanding.
Febrile seizures are common in young children; ~ 3% of US children 6 months to 5 years will experience one. SUDC however has been associated with a 10-fold increase in febrile seizures; our study is the first to implicate them at time of death. The SUDC Registry and Research Collaborative (www.sudcrrc.org) at NYU Langone Health has enrolled over 300 cases of unexplained child death; seven with audiovisual recordings from the child’s bedroom during their last sleep period. More than 80% of the cases enrolled in the registry were children 1-4 years at the time of death. The seven cases with videos were aged 13-27 months with normal development and no pathogenic disease-causing variants by whole exome sequencing.
Laura Gould[/caption]
Laura Gould, MSc, MA, PT
Research Scientist
SUDC Registry and Research Collaborative
Comprehensive Epilepsy Center
Department of Neurology
NYU Langone Grossman School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Sudden Unexplained death in childhood (SUDC) is the unexplained death of a child on or after their 1st birthday that remains unexplained after a comprehensive death investigation. About 400 SUDC occur annually between the ages of 1-18, but more than half occur in toddlers, aged 1-4 years. Since most deaths are sleep related and unwitnessed with unremarkable autopsies, mechanisms of deaths have eluded our understanding.
Febrile seizures are common in young children; ~ 3% of US children 6 months to 5 years will experience one. SUDC however has been associated with a 10-fold increase in febrile seizures; our study is the first to implicate them at time of death. The SUDC Registry and Research Collaborative (www.sudcrrc.org) at NYU Langone Health has enrolled over 300 cases of unexplained child death; seven with audiovisual recordings from the child’s bedroom during their last sleep period. More than 80% of the cases enrolled in the registry were children 1-4 years at the time of death. The seven cases with videos were aged 13-27 months with normal development and no pathogenic disease-causing variants by whole exome sequencing.


 Dr. Brousseau[/caption]
David Brousseau, MD, MS
Chair of Pediatrics
Nemours Children’s Health, Delaware and the
Sidney Kimmel Medical College at Thomas Jefferson University
Dr. Brousseau[/caption]
David Brousseau, MD, MS
Chair of Pediatrics
Nemours Children’s Health, Delaware and the
Sidney Kimmel Medical College at Thomas Jefferson University

 Dr. Sood[/caption]
Neeraj Sood, PhD
Verna and Peter Dauterive Hall
University Park Campus
University of Southern California
Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We conducted this study to inform school COVID-19 policies.
The main findings are that the median duration of infectivity after a positive COVID-19 test in children is 3 days. The median duration of infectivity does not vary with vaccination.
Dr. Sood[/caption]
Neeraj Sood, PhD
Verna and Peter Dauterive Hall
University Park Campus
University of Southern California
Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We conducted this study to inform school COVID-19 policies.
The main findings are that the median duration of infectivity after a positive COVID-19 test in children is 3 days. The median duration of infectivity does not vary with vaccination. 

 Dr. Payne-Sturges[/caption]
Dr. Payne-Sturges[/caption]


 Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD
Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD


 Dr. Li Li[/caption]
Li Li, M.D., Ph.D., M.P.H
Walter M. Seward Professor
Chair of Family Medicine
Director of population health
University of Virginia School of Medicine
Editor-in-chief of The BMJ Family Medicine
Dr. Li joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force reviewed the latest available evidence to evaluate whether screening all children and adolescents who are 20 years old or younger for high cholesterol improves their heart health into adulthood.
At this time, there is not enough evidence to determine whether or not screening all kids is beneficial, so we are calling for additional research on the effectiveness of screening and treatment of high cholesterol in kids and teens.
Dr. Li Li[/caption]
Li Li, M.D., Ph.D., M.P.H
Walter M. Seward Professor
Chair of Family Medicine
Director of population health
University of Virginia School of Medicine
Editor-in-chief of The BMJ Family Medicine
Dr. Li joined the U.S. Preventive Services Task Force in January 2021
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force reviewed the latest available evidence to evaluate whether screening all children and adolescents who are 20 years old or younger for high cholesterol improves their heart health into adulthood.
At this time, there is not enough evidence to determine whether or not screening all kids is beneficial, so we are calling for additional research on the effectiveness of screening and treatment of high cholesterol in kids and teens.
 Dr. Davis[/caption]
Prof. Jonathan Davis, MD,
Chief of Newborn Medicine
Tufts Medical Center and
[caption id="attachment_60599" align="alignleft" width="125"]
Dr. Davis[/caption]
Prof. Jonathan Davis, MD,
Chief of Newborn Medicine
Tufts Medical Center and
[caption id="attachment_60599" align="alignleft" width="125"]
 Dr. Miller[/caption]
Alex P. Miller, PhD
TranSTAR T32 Postdoctoral Fellow
Department of Psychiatry
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study?
Response: Adolescent cannabis use is increasing in the United States. Prior research suggests that people who start using cannabis earlier are more likely to engage in problematic use and also experience greater mental health challenges and socioeconomic disadvantages overall. For example, children who begin using cannabis early are more likely to have behavioral problems and disorders and are more less likely to complete school.
In our study, we used data from the Adolescent Brain Cognitive Development (ABCD) Study, which is following nearly 12,000 kids across the nation to track behavior and brain development as well as health from middle childhood to young adulthood. We looked at what factors are associated with the initiation of cannabis use by age 12-14.
Dr. Miller[/caption]
Alex P. Miller, PhD
TranSTAR T32 Postdoctoral Fellow
Department of Psychiatry
Washington University School of Medicine
St. Louis, MO
MedicalResearch.com: What is the background for this study?
Response: Adolescent cannabis use is increasing in the United States. Prior research suggests that people who start using cannabis earlier are more likely to engage in problematic use and also experience greater mental health challenges and socioeconomic disadvantages overall. For example, children who begin using cannabis early are more likely to have behavioral problems and disorders and are more less likely to complete school.
In our study, we used data from the Adolescent Brain Cognitive Development (ABCD) Study, which is following nearly 12,000 kids across the nation to track behavior and brain development as well as health from middle childhood to young adulthood. We looked at what factors are associated with the initiation of cannabis use by age 12-14.

 Yuxia Wei[/caption]
Yuxia Wei | PhD Student
Unit of Epidemiology
Institute of Environmental Medicine
Karolinska Institutet
Stockholm | Sweden
MedicalResearch.com: What is the background for this study?
Response: Diabetes is traditionally known for having two types (type 1 diabetes and type 2 diabetes). However, it is becoming increasingly clear that diabetes is much more complex than this traditional classification. Several attempts have been made to address this heterogeneity and in 2018, a Swedish ground-breaking study proposed that there are five distinct subtypes of diabetes in adults. They have been replicated in different populations and it has been shown that there are differences between the subtypes in terms of genetics and risks of complications. Another way of elucidating the relevance of these subtypes is to investigate whether the influence of known risk factors for diabetes is different on different subtypes. Our study is one of the first attempts to address this. We used a study design known as Mendelian randomization, to investigate the influence of childhood obesity on these diabetes subtypes that typically occur after age 35. This work was a collaboration between Karolinska institutet in Stockholm, University of Bristol in the UK and Sun Yat-Sen University in China.
Yuxia Wei[/caption]
Yuxia Wei | PhD Student
Unit of Epidemiology
Institute of Environmental Medicine
Karolinska Institutet
Stockholm | Sweden
MedicalResearch.com: What is the background for this study?
Response: Diabetes is traditionally known for having two types (type 1 diabetes and type 2 diabetes). However, it is becoming increasingly clear that diabetes is much more complex than this traditional classification. Several attempts have been made to address this heterogeneity and in 2018, a Swedish ground-breaking study proposed that there are five distinct subtypes of diabetes in adults. They have been replicated in different populations and it has been shown that there are differences between the subtypes in terms of genetics and risks of complications. Another way of elucidating the relevance of these subtypes is to investigate whether the influence of known risk factors for diabetes is different on different subtypes. Our study is one of the first attempts to address this. We used a study design known as Mendelian randomization, to investigate the influence of childhood obesity on these diabetes subtypes that typically occur after age 35. This work was a collaboration between Karolinska institutet in Stockholm, University of Bristol in the UK and Sun Yat-Sen University in China.



 Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.
Dr. Pierce[/caption]
Karen Pierce, Ph.D.
Professor, Department of Neurosciences, UCSD
Co-Director, Autism Center of Excellence, UCSD
MedicalResearch.com: What is the background for this study?
Response: The mean age of ASD diagnosis and eventual treatment remains at ~52 months in the United States1 - years beyond the disorder’s prenatal origins2, and beyond the age when it can be reliably diagnosed in many cases3.
Currently the only way to determine if a child has autism spectrum disorder (ASD) is to receive a developmental evaluation from an experienced clinician (usually a licensed clinical psychologist). There are often long waiting lists, and only a small number of clinicians have the experience required to make early-age (i.e., between 12-36 months) diagnoses of ASD. Thus, there are many places in the country as well as world wide wherein children wait months or years to receive a formal diagnosis due to a lack of available expertise. Moreover, diagnostic evaluations are expensive and usually cost the parent and/or insurance approximately ~$2,000 or more per evaluation. Finally, clinical evaluations usually take between 2-3 hours to complete and result in fatigue for both the parent and toddler.
Eye-tracking, which generates biologically-relevant, objective, and quantifiable metrics of both visual and auditory preference profiles in babies and toddlers in just minutes, is a technology that can dramatically change how ASD is diagnosed.




 Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.

 Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).

 Dr. Stingone[/caption]
Jeanette Stingone PhD
Assistant Professor, Epidemiology
Mailman School of Public Health
Columbia University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lead is a well-established neurotoxin, particularly when exposure occurs early in life and in childhood. Associations between elevated blood lead levels and lower scores on tests of neurodevelopment and cognition are seen consistently across studies, even when examining lower levels of exposure.
While reducing exposure to lead is the primary intervention to prevent these adverse outcomes, there aren’t many interventions designed to support the neurodevelopment of children who have been exposed to lead. Some municipalities consider elevated blood lead levels as a criteria for inclusion in Early Intervention programs. Early Intervention programs are mandated under the Individuals with Disabilities Education Act and provide services for children younger than 3 years old with disabilities or developmental delays.
The objective of this study was to compare 3rd grade standardized test scores among children who had elevated blood lead levels early in life to see if children who had received Early Intervention services performed better on these tests than those who did not receive services. Using matching methods and an existing administrative data linkage of children who were born and attended public school in New York City, we observed that children exposed to lead who received Early Intervention services scored higher on standardized tests in both math and English Language arts than children exposed to lead who did not receive services.
Dr. Stingone[/caption]
Jeanette Stingone PhD
Assistant Professor, Epidemiology
Mailman School of Public Health
Columbia University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lead is a well-established neurotoxin, particularly when exposure occurs early in life and in childhood. Associations between elevated blood lead levels and lower scores on tests of neurodevelopment and cognition are seen consistently across studies, even when examining lower levels of exposure.
While reducing exposure to lead is the primary intervention to prevent these adverse outcomes, there aren’t many interventions designed to support the neurodevelopment of children who have been exposed to lead. Some municipalities consider elevated blood lead levels as a criteria for inclusion in Early Intervention programs. Early Intervention programs are mandated under the Individuals with Disabilities Education Act and provide services for children younger than 3 years old with disabilities or developmental delays.
The objective of this study was to compare 3rd grade standardized test scores among children who had elevated blood lead levels early in life to see if children who had received Early Intervention services performed better on these tests than those who did not receive services. Using matching methods and an existing administrative data linkage of children who were born and attended public school in New York City, we observed that children exposed to lead who received Early Intervention services scored higher on standardized tests in both math and English Language arts than children exposed to lead who did not receive services. 
 Dr. Fernandez-Mendoza[/caption]
Julio Fernandez-Mendoza, PhD, CBSM, DBSM
Associate Professor of Psychiatry & Behavioral Health
Sleep Research & Treatment Center
Director, Behavioral Sleep Medicine Program
Penn State Health Milton S. Hershey Medical Center
MedicalResearch.com: What is the background for this study? Is insomnia familial?
Response: Consistent research has shown that about 25% of school-age children have insomnia symptoms consisting of difficulties initiating or maintaining sleep. However, what has remained unknown is to what extent those insomnia symptoms persist all the way into adulthood, or whether they developmentally remit (go away with age) as the child grows into adolescence or young adulthood. This is the question that our study focused on.
Dr. Fernandez-Mendoza[/caption]
Julio Fernandez-Mendoza, PhD, CBSM, DBSM
Associate Professor of Psychiatry & Behavioral Health
Sleep Research & Treatment Center
Director, Behavioral Sleep Medicine Program
Penn State Health Milton S. Hershey Medical Center
MedicalResearch.com: What is the background for this study? Is insomnia familial?
Response: Consistent research has shown that about 25% of school-age children have insomnia symptoms consisting of difficulties initiating or maintaining sleep. However, what has remained unknown is to what extent those insomnia symptoms persist all the way into adulthood, or whether they developmentally remit (go away with age) as the child grows into adolescence or young adulthood. This is the question that our study focused on.


 Dr. Aris[/caption]
Izzuddin M Aris, PhD
Assistant Professor
Department of Population Medicine, Harvard Medical School
Division of Chronic Disease Research Across the Lifecourse
Harvard Pilgrim Health Care Institute
Boston, MA
MedicalResearch.com: What is the background for this study?
Response: Puberty is a key stage during child development. Previous research indicates that children in the United States are entering puberty at younger ages. These children may be in danger of developing certain diseases, such as type 2 diabetes, later in life. A better understanding of how early life factors affect puberty development is important for combating earlier puberty onset. .
Dr. Aris[/caption]
Izzuddin M Aris, PhD
Assistant Professor
Department of Population Medicine, Harvard Medical School
Division of Chronic Disease Research Across the Lifecourse
Harvard Pilgrim Health Care Institute
Boston, MA
MedicalResearch.com: What is the background for this study?
Response: Puberty is a key stage during child development. Previous research indicates that children in the United States are entering puberty at younger ages. These children may be in danger of developing certain diseases, such as type 2 diabetes, later in life. A better understanding of how early life factors affect puberty development is important for combating earlier puberty onset. .

 Dr. Myran[/caption]
Daniel Myran, MD, MPH, CCFP, FRCPC
Family and Public Health and Preventive Medicine Physician
CIHR Fellow, Ottawa Hospital Research Institute
Department of Family Medicine Innovation Fellow
University of Ottawa
MedicalResearch.com: What is the background for this study?
Response: Canada legalized recreational, or non-medical, cannabis in October 2018. Canada took phased approach to legalization initially only allowing flower-based cannabis products and oils and after one year permitting the sale of commercial cannabis edibles (e.g. THC containing candies, baked goods, and drinks). In this study we took advantage of this phased roll out of legal cannabis to understand the impact of legalization on cannabis exposures or poisonings in children aged 0-9 years and the contribution of different types of cannabis products to these events.
Dr. Myran[/caption]
Daniel Myran, MD, MPH, CCFP, FRCPC
Family and Public Health and Preventive Medicine Physician
CIHR Fellow, Ottawa Hospital Research Institute
Department of Family Medicine Innovation Fellow
University of Ottawa
MedicalResearch.com: What is the background for this study?
Response: Canada legalized recreational, or non-medical, cannabis in October 2018. Canada took phased approach to legalization initially only allowing flower-based cannabis products and oils and after one year permitting the sale of commercial cannabis edibles (e.g. THC containing candies, baked goods, and drinks). In this study we took advantage of this phased roll out of legal cannabis to understand the impact of legalization on cannabis exposures or poisonings in children aged 0-9 years and the contribution of different types of cannabis products to these events.

