Author Interviews, Cognitive Issues, Environmental Risks, NIH, Pediatrics / 27.08.2024
NIEHS Examines Link Between Flouride in Water and IQ in Children
MedicalResearch.com Interview with:
Rick Woychik, Ph.D.
Director of the National Toxicology Program
Director of the National Institute of Environmental Health Sciences
Principal Investigator
Mammalian Genome Research Group
Division for Intramural Research at NIEHS
MedicalResearch.com: What is the background for this study?
[caption id="attachment_62975" align="alignleft" width="200"] Source[/caption]
Response: Since 1945, the use of fluoride has been a successful public health initiative for reducing dental cavities and improving general oral health of adults and children. There is a concern, however, that some pregnant women and children may be getting more fluoride than they need because they now get fluoride from many sources including treated public water, water-added foods and beverages, teas, toothpaste, floss, and mouthwash, and the combined total intake of fluoride may exceed safe amounts.
Therefore, the National Toxicology Program (NTP) conducted a systematic review of the published scientific literature on the association between fluoride exposure and neurodevelopment and cognition. The NTP released their findings in a State of the Science Monograph on August 21, 2024, and posted to the NTP website. A corresponding meta-analysis on children’s IQ has been accepted by a scientific journal for publication later in 2024.
The NTP started this work in 2016. As with all research documents intended for publication, the NTP fluoride monograph and meta-analysis underwent rigorous scientific evaluation. The evaluation process has involved many steps. The draft fluoride monograph received significant critical feedback during peer-review by the National Academies of Science, Engineering and Medicine (NASEM), from other external experts, and from experts in several federal health agencies. After modifications were made, additional evaluation following a rigorous scientific framework was conducted by subject matter experts organized by the NTP Board of Scientific Counselors. I am very pleased that this document is now complete and available for reference.
Since fluoride is such an important topic to the public and to public health officials, it was imperative that we made every effort to get the science right. I commend the report authors, the NTP Board of Scientific Counselors, and countless subject matter experts who participated in this evaluation. The monograph represents a thorough review of the data, and the various interpretations of the data, to accurately reflect what we know and where additional research is needed.
Source[/caption]
Response: Since 1945, the use of fluoride has been a successful public health initiative for reducing dental cavities and improving general oral health of adults and children. There is a concern, however, that some pregnant women and children may be getting more fluoride than they need because they now get fluoride from many sources including treated public water, water-added foods and beverages, teas, toothpaste, floss, and mouthwash, and the combined total intake of fluoride may exceed safe amounts.
Therefore, the National Toxicology Program (NTP) conducted a systematic review of the published scientific literature on the association between fluoride exposure and neurodevelopment and cognition. The NTP released their findings in a State of the Science Monograph on August 21, 2024, and posted to the NTP website. A corresponding meta-analysis on children’s IQ has been accepted by a scientific journal for publication later in 2024.
The NTP started this work in 2016. As with all research documents intended for publication, the NTP fluoride monograph and meta-analysis underwent rigorous scientific evaluation. The evaluation process has involved many steps. The draft fluoride monograph received significant critical feedback during peer-review by the National Academies of Science, Engineering and Medicine (NASEM), from other external experts, and from experts in several federal health agencies. After modifications were made, additional evaluation following a rigorous scientific framework was conducted by subject matter experts organized by the NTP Board of Scientific Counselors. I am very pleased that this document is now complete and available for reference.
Since fluoride is such an important topic to the public and to public health officials, it was imperative that we made every effort to get the science right. I commend the report authors, the NTP Board of Scientific Counselors, and countless subject matter experts who participated in this evaluation. The monograph represents a thorough review of the data, and the various interpretations of the data, to accurately reflect what we know and where additional research is needed.
 Source[/caption]
Response: Since 1945, the use of fluoride has been a successful public health initiative for reducing dental cavities and improving general oral health of adults and children. There is a concern, however, that some pregnant women and children may be getting more fluoride than they need because they now get fluoride from many sources including treated public water, water-added foods and beverages, teas, toothpaste, floss, and mouthwash, and the combined total intake of fluoride may exceed safe amounts.
Therefore, the National Toxicology Program (NTP) conducted a systematic review of the published scientific literature on the association between fluoride exposure and neurodevelopment and cognition. The NTP released their findings in a State of the Science Monograph on August 21, 2024, and posted to the NTP website. A corresponding meta-analysis on children’s IQ has been accepted by a scientific journal for publication later in 2024.
The NTP started this work in 2016. As with all research documents intended for publication, the NTP fluoride monograph and meta-analysis underwent rigorous scientific evaluation. The evaluation process has involved many steps. The draft fluoride monograph received significant critical feedback during peer-review by the National Academies of Science, Engineering and Medicine (NASEM), from other external experts, and from experts in several federal health agencies. After modifications were made, additional evaluation following a rigorous scientific framework was conducted by subject matter experts organized by the NTP Board of Scientific Counselors. I am very pleased that this document is now complete and available for reference.
Since fluoride is such an important topic to the public and to public health officials, it was imperative that we made every effort to get the science right. I commend the report authors, the NTP Board of Scientific Counselors, and countless subject matter experts who participated in this evaluation. The monograph represents a thorough review of the data, and the various interpretations of the data, to accurately reflect what we know and where additional research is needed.
Source[/caption]
Response: Since 1945, the use of fluoride has been a successful public health initiative for reducing dental cavities and improving general oral health of adults and children. There is a concern, however, that some pregnant women and children may be getting more fluoride than they need because they now get fluoride from many sources including treated public water, water-added foods and beverages, teas, toothpaste, floss, and mouthwash, and the combined total intake of fluoride may exceed safe amounts.
Therefore, the National Toxicology Program (NTP) conducted a systematic review of the published scientific literature on the association between fluoride exposure and neurodevelopment and cognition. The NTP released their findings in a State of the Science Monograph on August 21, 2024, and posted to the NTP website. A corresponding meta-analysis on children’s IQ has been accepted by a scientific journal for publication later in 2024.
The NTP started this work in 2016. As with all research documents intended for publication, the NTP fluoride monograph and meta-analysis underwent rigorous scientific evaluation. The evaluation process has involved many steps. The draft fluoride monograph received significant critical feedback during peer-review by the National Academies of Science, Engineering and Medicine (NASEM), from other external experts, and from experts in several federal health agencies. After modifications were made, additional evaluation following a rigorous scientific framework was conducted by subject matter experts organized by the NTP Board of Scientific Counselors. I am very pleased that this document is now complete and available for reference.
Since fluoride is such an important topic to the public and to public health officials, it was imperative that we made every effort to get the science right. I commend the report authors, the NTP Board of Scientific Counselors, and countless subject matter experts who participated in this evaluation. The monograph represents a thorough review of the data, and the various interpretations of the data, to accurately reflect what we know and where additional research is needed.


 Dr. Walsh[/caption]
Christopher Walsh, M.D., Ph.D.
Chief, Division of Genetics and Genomics
Bullard Professor of Pediatrics and Neurology at Harvard Medical School
and researcher who has used material donated to the brain bank
MedicalResearch.com: What is the background for this study?
Response: Many different types of genetic variants contribute to neurodevelopmental disorders such as autism. Copy number variants are large pieces of genetic material that are duplicated or deleted. We have known for many years that many copy number variants at certain genetic locations are linked to autism. Because these copy number variants may include lots of different genes, it has been difficult to understand how these copy number variants alter human brain function. Furthermore, although animal models are important, autism is in many ways defined by differences in uniquely human cognitive and social functioning. Better understanding of how these copy number variants change human brain function will shed light on universal mechanisms that regulate neurodevelopment. We studied a copy number variant called dup15q, that is associated with almost 40-fold higher rates of autism vs. the general population. We studied post-mortem human brain tissue from individuals with dup15q, individuals with autism not related to dup15q, and neurotypical controls, to better understand how the human brain is impacted by dup15q. We focused on frontal cortex, an important brain region in executive function and social perspective taking. We applied cutting edge techniques that allow us to assess individual cells in the brain.
Dr. Walsh[/caption]
Christopher Walsh, M.D., Ph.D.
Chief, Division of Genetics and Genomics
Bullard Professor of Pediatrics and Neurology at Harvard Medical School
and researcher who has used material donated to the brain bank
MedicalResearch.com: What is the background for this study?
Response: Many different types of genetic variants contribute to neurodevelopmental disorders such as autism. Copy number variants are large pieces of genetic material that are duplicated or deleted. We have known for many years that many copy number variants at certain genetic locations are linked to autism. Because these copy number variants may include lots of different genes, it has been difficult to understand how these copy number variants alter human brain function. Furthermore, although animal models are important, autism is in many ways defined by differences in uniquely human cognitive and social functioning. Better understanding of how these copy number variants change human brain function will shed light on universal mechanisms that regulate neurodevelopment. We studied a copy number variant called dup15q, that is associated with almost 40-fold higher rates of autism vs. the general population. We studied post-mortem human brain tissue from individuals with dup15q, individuals with autism not related to dup15q, and neurotypical controls, to better understand how the human brain is impacted by dup15q. We focused on frontal cortex, an important brain region in executive function and social perspective taking. We applied cutting edge techniques that allow us to assess individual cells in the brain. 






 The pregnancy brain is often referred to as momnesia or baby brain.
The pregnancy brain is often referred to as momnesia or baby brain.





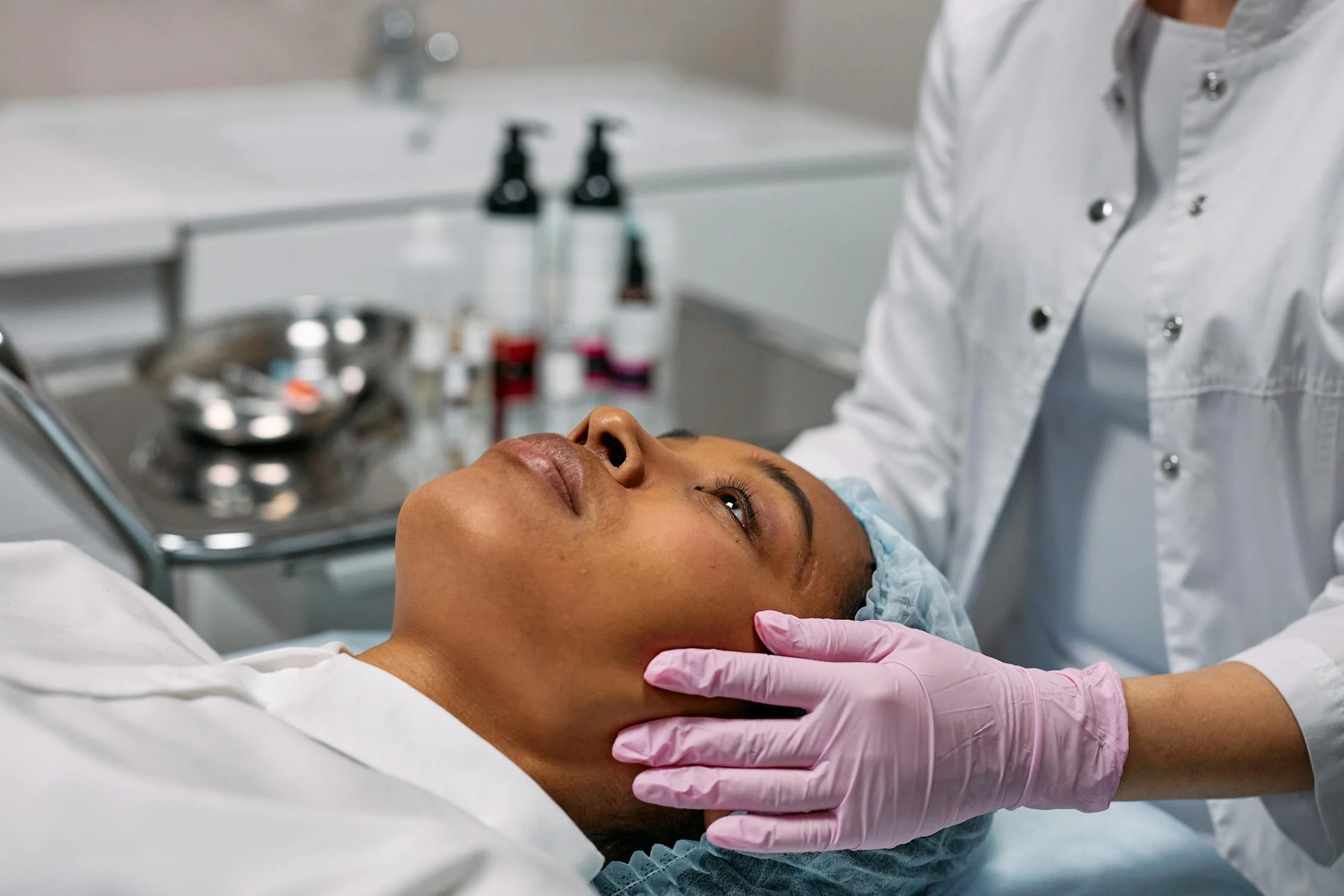
 Photo by cottonbro studio[/caption]
One of the most significant psychological benefits of cosmetic surgery is the enhancement of self-esteem and body image. We've all got our own physical quirks that can make us feel, well, less than confident. Whether you're looking to revitalize your facial features or refine your neck and jawline, surgical solutions like rhinoplasty, neck lifts, and facelifts can reshape your confidence from the inside out. Exploring various surgical solutions can bring profound changes, such as enhanced facial symmetry or
Photo by cottonbro studio[/caption]
One of the most significant psychological benefits of cosmetic surgery is the enhancement of self-esteem and body image. We've all got our own physical quirks that can make us feel, well, less than confident. Whether you're looking to revitalize your facial features or refine your neck and jawline, surgical solutions like rhinoplasty, neck lifts, and facelifts can reshape your confidence from the inside out. Exploring various surgical solutions can bring profound changes, such as enhanced facial symmetry or 


 Meditation, as explained by
Meditation, as explained by 







 Stress in the workplace is the body's response to the demands and pressures encountered in professional situations. It can manifest as acute stress, which is short-term and often related to specific events, or chronic stress, which persists over a long period due to ongoing challenges.
Stress in the workplace is the body's response to the demands and pressures encountered in professional situations. It can manifest as acute stress, which is short-term and often related to specific events, or chronic stress, which persists over a long period due to ongoing challenges. 
 The High-Stress Environment of Nursing
The High-Stress Environment of Nursing

 As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing
As technology continues to evolve within the healthcare sector, creating new opportunities for enhancing patient care, it's crucial that empathy doesn't get lost in the shuffle. Innovative tools and systems should be seen as avenues to deepen our understanding and connection with patients, rather than as barriers to the human touch. Embracing technology with empathetic intention can lead to an even greater level of personalized care.
One specific area where empathy can play a transformative role is in addressing 