MedicalResearch.com Interview with:
[caption id="attachment_60763" align="alignleft" width="200"]

Dr. Worthley[/caption]
Daniel L. Worthley
MBBS (Hons), PhD, MPH, FRACP, AGAF
Gastroenterologist
Associate Professor
University of Adelaide
MedicalResearch.com: What is the background for this study?
Response: Cells are revolutionising healthcare, from modern faecal microbial transplantation in the gut to CAR-T cells fighting cancers, life healing life. Some aspects of cellular care are so entrenched in medicine that they are almost overlooked for the miraculous cellular therapies that they are, such as stem cell transplantation to treat haematological malignancies and, of course, in vitro fertilization, life creating life. Modern medicine is slowly, but surely, pivoting from pills to cells. Professor Siddhartha Mukherjeee, oncologist, scientist, and author, provides a beautiful thesis of this in his book Song of the Cell and in his TED talk on the cellular revolution in medicine (
https://youtu.be/qG_YmIPFO68?feature=shared). I was lucky enough to have trained with Sid as a post-doc at Columbia and this concept was really drummed into me. But, as a gastroenterologist, perhaps it was the bacterial cells, rather than the blood cells, that had most to offer in the management of bowel disorders? Around the same time, Professors Jeff Hasty, Tal Danino and Omar Din from UC San Diego had been inventing and publishing, in my opinion, the best bacterial engineering work that has ever been produced to specifically target cancer. I remember when we first reviewed their 2016 Nature paper in our lab meeting (
https://www.nature.com/articles/nature18930#citeas), it was like – “We gotta meet these guys!”. Through Tal, who was by then, working at Columbia, I was introduced to Jeff and I attended his lab meeting back in 2019. That was where our project began after a lab meeting in La Jolla. Rob Cooper had presented his work on horizontal gene transfer. Everything that comes out of Jeff’s lab is both practical and reproducible but also beautiful. Beautiful in a scientific self-evident way that instantly communicates the purpose, approach and outcomes of an experiment.
Rob’s presentation that day was a case-in-point. Rob was studying genes and gene transfer in bacteria (see part of Rob’s fascinating presentation here,
https://youtu.be/5nBsRF-BsA8?feature=shared). Genes are the fundamental unit of heredity and gene transfer (or inheritance) the process by which genes are passed from one cell to another. Genes may be inherited vertically when one cell replicates its DNA and divides into two, now separate, cells (reproduction). Genes are the stuff, and vertical gene transfer is the process, by which you receive your mother’s laugh and your father’s eyebrows. Genes may also, however, be inherited horizontally when DNA is passed between unrelated cells, outside of parent to offspring inheritance. Horizontal gene transfer is quite common in the microbial world. Certain bacteria can salvage genes from cell-free DNA found within its environment. This sweeping up of cell-free DNA, into a cell, is called natural competence. So, competent bacteria can sample their nearby environment and, in doing so, acquire genes that may provide a selective advantage to that cell. Like cellular panning for flecks of gold in a stream. After Rob’s presentation, Jeff, Rob and I started to discuss the possibilities. If bacteria can take up DNA, and cancer is defined genetically by a change in its DNA then, theoretically, bacteria could be engineered to detect cancer. Colorectal cancer seemed a logical proof of concept as the colorectal lumen is full of microbes and, in the setting of cancer, full of tumour DNA. When a biophysicist, a scientist and a gastroenterologist walk into a bar, after a lab meeting, this is what can happen! Professor Susi Woods and Dr Josephine Wright, superb cancer scientists from Adelaide, Australia, were quickly recruited in as essential founding members of the group. We all got to work. Australian and US grants, lots of experiments, early morning Zoom calls across the Pacific, inventing new animal models and approaches, i.e. a many year, iterative process of design-build-test-learn, that got us all to where we are now.
 Source[/caption]
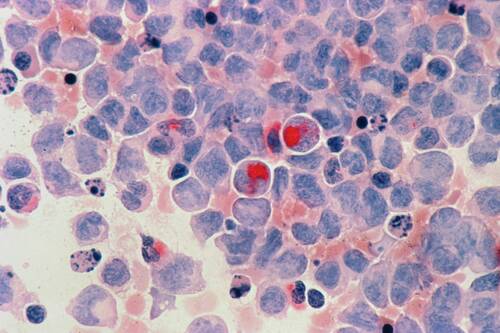
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
 Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.
Source[/caption]
Cancer research is entering a new phase. For years, scientists focused on how cancer cells grow and divide. That model still matters, but it is no longer enough. New research shows something deeper: cancer cells are not fixed. They can change their identity and shift how they behave based on internal signals.
One of the strongest of those signals is metabolism. Emerging research shows that metabolism does more than provide energy — it also controls how genes are turned on and off, which means it can shape what a cancer cell becomes. This is a major shift in thinking, and it changes how researchers approach treatment and discovery.






 Dr. Lopes[/caption]
Gilberto Lopes, M.D.
Professor, Chief, Division of Medical Oncology
Associate Director for the Cancer Center and
Medical Director for International Affairs
Sylvester Comprehensive Cancer Center
MedicalResearch.com: What is the background for this study?
Response: There is growing evidence linking alcohol consumption to increased cancer risk and mortality. This association was recently emphasized by the former U.S. Surgeon General, prompting renewed public health interest. In response to these concerns, under the mentorship of Dr. Lopes, we evaluated national trends in alcohol-associated cancer mortality using data from the Global Burden of Disease database.
Dr. Lopes[/caption]
Gilberto Lopes, M.D.
Professor, Chief, Division of Medical Oncology
Associate Director for the Cancer Center and
Medical Director for International Affairs
Sylvester Comprehensive Cancer Center
MedicalResearch.com: What is the background for this study?
Response: There is growing evidence linking alcohol consumption to increased cancer risk and mortality. This association was recently emphasized by the former U.S. Surgeon General, prompting renewed public health interest. In response to these concerns, under the mentorship of Dr. Lopes, we evaluated national trends in alcohol-associated cancer mortality using data from the Global Burden of Disease database.

 Dr. Zeynep Gümüş[/caption]
Zeynep H. Gümüş, PhD
Associate Professor
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: The germline genome of each individual person has a unique combination of millions of genetic variants that influence virtually all biological processes throughout life, including cancer evolution. In this study, we have investigated the impact of germline variants – genetic defects one is born with – on gene expression and protein abundance in tumors across cancer types.
MedicalResearch.com: Would you describe the technique of precision peptidomics?
Response: We have leveraged a cohort of 1,064 patients with multiple cancer types to explore the impact of germline variations on cancer-relevant genes through multiple-omics layers: from DNA to RNA, protein abundance and post-translational modifications. To assess the effects of coding variants and their association with cognate proteins, we used precision peptidomics, which is the quantification of peptides carrying genetic variants from individual patients. Through this approach, we mapped 337,469 protein coding germline variants onto patient peptides, revealing their potential impact on protein modifications, protein stability, allele-specific expression, and protein structure by leveraging the relevant protein databases.
Dr. Zeynep Gümüş[/caption]
Zeynep H. Gümüş, PhD
Associate Professor
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: The germline genome of each individual person has a unique combination of millions of genetic variants that influence virtually all biological processes throughout life, including cancer evolution. In this study, we have investigated the impact of germline variants – genetic defects one is born with – on gene expression and protein abundance in tumors across cancer types.
MedicalResearch.com: Would you describe the technique of precision peptidomics?
Response: We have leveraged a cohort of 1,064 patients with multiple cancer types to explore the impact of germline variations on cancer-relevant genes through multiple-omics layers: from DNA to RNA, protein abundance and post-translational modifications. To assess the effects of coding variants and their association with cognate proteins, we used precision peptidomics, which is the quantification of peptides carrying genetic variants from individual patients. Through this approach, we mapped 337,469 protein coding germline variants onto patient peptides, revealing their potential impact on protein modifications, protein stability, allele-specific expression, and protein structure by leveraging the relevant protein databases.

 Dr. Mzoughi[/caption]
Slim Mzoughi, PhD
Dr. Mzoughi[/caption]
Slim Mzoughi, PhD











 Dr. Tesi[/caption]
MedicalResearch.com Interview with:
RJ Tesi M.D.
CEO and Founder of
Dr. Tesi[/caption]
MedicalResearch.com Interview with:
RJ Tesi M.D.
CEO and Founder of 







 Dr. Kamath[/caption]
Dr. Suneel Kamath MD
Gastrointestinal Oncologist
Cleveland Clinic
Senior Author on this research
MedicalResearch.com: What is the background for this study?
Response: Colorectal cancer rates in young people under age 50 are skyrocketing and have been for the last 3-4 decades. We really don’t understand why because most cases (probably around 70%) are not genetic or hereditary, just random, unfortunate events. We suspect that it is some exposure(s) like excess consumption of red meat, processed foods, sugar-sweetened beverages, excess antibiotic use altering the microbiome, rising incidence of obesity or some other factors. We really don’t know why yet.
Our study used a technology called metabolomics, the study of breakdown products and production building blocks for our bodies, to look for differences in colorectal cancer in young people versus people that are older that developed colorectal cancer. Because metabolomics measures how each individual interacts with the exposures in our environment like diet, air quality, etc., it is a way to bridge the gap between our nature (determined by genetics) and nurture (determined by our exposures).
Dr. Kamath[/caption]
Dr. Suneel Kamath MD
Gastrointestinal Oncologist
Cleveland Clinic
Senior Author on this research
MedicalResearch.com: What is the background for this study?
Response: Colorectal cancer rates in young people under age 50 are skyrocketing and have been for the last 3-4 decades. We really don’t understand why because most cases (probably around 70%) are not genetic or hereditary, just random, unfortunate events. We suspect that it is some exposure(s) like excess consumption of red meat, processed foods, sugar-sweetened beverages, excess antibiotic use altering the microbiome, rising incidence of obesity or some other factors. We really don’t know why yet.
Our study used a technology called metabolomics, the study of breakdown products and production building blocks for our bodies, to look for differences in colorectal cancer in young people versus people that are older that developed colorectal cancer. Because metabolomics measures how each individual interacts with the exposures in our environment like diet, air quality, etc., it is a way to bridge the gap between our nature (determined by genetics) and nurture (determined by our exposures).


