Author Interviews, COVID -19 Coronavirus, Nature, Pediatrics / 19.02.2021
COVID-19: Immune Cells Act Quicker in Children Than Adults
MedicalResearch.com Interview with:
[caption id="attachment_56723" align="alignleft" width="200"] Dr. Neeland[/caption]
Dr Melanie Neeland PhD
Research Fellow
Murdoch Children's Research Institute
Royal Children's Hospital
Flemington Road, Parkville
Victoria Australia
MedicalResearch.com: What is the background for this study?
Response: Children generally have mild COVID-19 disease compared to adults, however the immune mechanisms underpinning this response are unclear. Understanding the underlying age-related differences in the severity of COVID-19 will provide important insights and opportunities for prevention and treatment of COVID-19.
Dr. Neeland[/caption]
Dr Melanie Neeland PhD
Research Fellow
Murdoch Children's Research Institute
Royal Children's Hospital
Flemington Road, Parkville
Victoria Australia
MedicalResearch.com: What is the background for this study?
Response: Children generally have mild COVID-19 disease compared to adults, however the immune mechanisms underpinning this response are unclear. Understanding the underlying age-related differences in the severity of COVID-19 will provide important insights and opportunities for prevention and treatment of COVID-19.
 Dr. Neeland[/caption]
Dr Melanie Neeland PhD
Research Fellow
Murdoch Children's Research Institute
Royal Children's Hospital
Flemington Road, Parkville
Victoria Australia
MedicalResearch.com: What is the background for this study?
Response: Children generally have mild COVID-19 disease compared to adults, however the immune mechanisms underpinning this response are unclear. Understanding the underlying age-related differences in the severity of COVID-19 will provide important insights and opportunities for prevention and treatment of COVID-19.
Dr. Neeland[/caption]
Dr Melanie Neeland PhD
Research Fellow
Murdoch Children's Research Institute
Royal Children's Hospital
Flemington Road, Parkville
Victoria Australia
MedicalResearch.com: What is the background for this study?
Response: Children generally have mild COVID-19 disease compared to adults, however the immune mechanisms underpinning this response are unclear. Understanding the underlying age-related differences in the severity of COVID-19 will provide important insights and opportunities for prevention and treatment of COVID-19.


 Jill Sommerville[/caption]
Jill Sommerville M.Sc
Director of Medical at WaterWipes
MedicalResearch.com: What is the background for this study? How prevalent is diaper dermatitis? Is it more severe in some babies?
Response: The Utah study is an independent clinical study conducted by the University of Utah Hospital NICU, Salt Lake City and recently published in Advances in Neonatal Care journal. It was a year-long study conducted between January 2018 – March 2019. The NICU staff were interested in exploring a new Perineal Skin Care Guideline in their unit, encompassing use of WaterWipes, to decrease the incidence of diaper dermatitis. Their stated aim was to reduce diaper dermatitis by 20% within a 1-year period. The study involved 1,070 premature babies, 11% of which were born at less than 30 weeks of gestational age. The inclusion criteria for the study were all babies who stayed for more than 1 day in the NICU.
Diaper dermatitis is known to cause discomfort and emotional distress in all babies and can be a possible source of infection among NICU babies. Diaper dermatitis remains prevalent, especially in preterm babies. The reported incidence varies from 21% to 25% among newborn intensive care babies. 1
Diaper dermatitis in pre term babies can be multifactorial especially as babies born early have a less well developed stratum corneum, the outer most layer of skin. NICU babies are often exposed to antibiotics and fortified milk to help them catch up growth. Other medical complications in addition can lead to altered gut flora and altered stool composition resulting in more frequency of stool.
The presence of urine and frequent stools necessitates regular cleaning which can result in excessive rubbing of the skin or the use of wipes containing harsh ingredients that can damage the skin.
Jill Sommerville[/caption]
Jill Sommerville M.Sc
Director of Medical at WaterWipes
MedicalResearch.com: What is the background for this study? How prevalent is diaper dermatitis? Is it more severe in some babies?
Response: The Utah study is an independent clinical study conducted by the University of Utah Hospital NICU, Salt Lake City and recently published in Advances in Neonatal Care journal. It was a year-long study conducted between January 2018 – March 2019. The NICU staff were interested in exploring a new Perineal Skin Care Guideline in their unit, encompassing use of WaterWipes, to decrease the incidence of diaper dermatitis. Their stated aim was to reduce diaper dermatitis by 20% within a 1-year period. The study involved 1,070 premature babies, 11% of which were born at less than 30 weeks of gestational age. The inclusion criteria for the study were all babies who stayed for more than 1 day in the NICU.
Diaper dermatitis is known to cause discomfort and emotional distress in all babies and can be a possible source of infection among NICU babies. Diaper dermatitis remains prevalent, especially in preterm babies. The reported incidence varies from 21% to 25% among newborn intensive care babies. 1
Diaper dermatitis in pre term babies can be multifactorial especially as babies born early have a less well developed stratum corneum, the outer most layer of skin. NICU babies are often exposed to antibiotics and fortified milk to help them catch up growth. Other medical complications in addition can lead to altered gut flora and altered stool composition resulting in more frequency of stool.
The presence of urine and frequent stools necessitates regular cleaning which can result in excessive rubbing of the skin or the use of wipes containing harsh ingredients that can damage the skin.

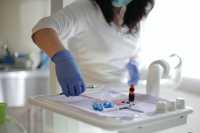

 Dr. Master[/caption]
Christina L. Master, MD, FAAP, CAQSM, FACSM
Professor of Clinical Pediatrics
Perelman School of Medicine at the University of Pennsylvania
Co-Director, Minds Matter Concussion Program
Pediatric and Adolescent Sports Medicine, Division of Pediatric Orthopedics
Attending Physician, Care Network - Karabots Center
The Children's Hospital of Philadelphia
Philadelphia, PA 19104
MedicalResearch.com: What is the background for this study?
Response: There have been multiple studies investigating potential sex differences in outcomes from concussion which have sometimes had conflicting results with some studies indicating that females take longer to recover than males and some studies reporting no difference in recovery between females and males, with most of these studies being conducted either retrospectively or prospectively in smaller cohorts. This large-scale multi-center prospective study in collegiate athletes provided an opportunity to compare females and males across comparable sports to examine both potential intrinsic or biologic factors (sex differences) or extrinsic (environmental or gender differences) that contribute to outcomes.
Dr. Master[/caption]
Christina L. Master, MD, FAAP, CAQSM, FACSM
Professor of Clinical Pediatrics
Perelman School of Medicine at the University of Pennsylvania
Co-Director, Minds Matter Concussion Program
Pediatric and Adolescent Sports Medicine, Division of Pediatric Orthopedics
Attending Physician, Care Network - Karabots Center
The Children's Hospital of Philadelphia
Philadelphia, PA 19104
MedicalResearch.com: What is the background for this study?
Response: There have been multiple studies investigating potential sex differences in outcomes from concussion which have sometimes had conflicting results with some studies indicating that females take longer to recover than males and some studies reporting no difference in recovery between females and males, with most of these studies being conducted either retrospectively or prospectively in smaller cohorts. This large-scale multi-center prospective study in collegiate athletes provided an opportunity to compare females and males across comparable sports to examine both potential intrinsic or biologic factors (sex differences) or extrinsic (environmental or gender differences) that contribute to outcomes.

 Dongmei Li, Ph.D.[/caption]
Dongmei Li, Ph.D., Associate Professor
Clinical and Translational Science Institute
University of Rochester Medical Center
MedicalResearch.com: What is the background for this study?
Response: Previous animal and human studies have found that nicotine exposure could harm adolescents’ brain development and impact their cognitive functions. Electronic cigarettes, which have become very popular among youth in the US in recent years, usually contain nicotine at equivalent or possibly higher levels than traditional tobacco cigarettes. Thus, it is reasonable to assume that vaping might be associated with self-reported cognitive complaints.
MedicalResearch.com: What are the main findings?
Response: Main findings from our study are:
Dongmei Li, Ph.D.[/caption]
Dongmei Li, Ph.D., Associate Professor
Clinical and Translational Science Institute
University of Rochester Medical Center
MedicalResearch.com: What is the background for this study?
Response: Previous animal and human studies have found that nicotine exposure could harm adolescents’ brain development and impact their cognitive functions. Electronic cigarettes, which have become very popular among youth in the US in recent years, usually contain nicotine at equivalent or possibly higher levels than traditional tobacco cigarettes. Thus, it is reasonable to assume that vaping might be associated with self-reported cognitive complaints.
MedicalResearch.com: What are the main findings?
Response: Main findings from our study are:



 Rebecca McNally[/caption]
Rebecca McAdams, MA, MPH
Senior research associate
Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: Sledding is a popular winter activity in communities across the country, but it may not be as risk-free as many people think.
MedicalResearch.com: What are the main findings?
Response: We found that 220,488 patients were treated in U.S. emergency departments for injuries related to sledding from 2008 through 2017. Nearly 70% of these patients were children age 19 years and younger. Compared to adults, children were almost seven times as likely to be treated in an emergency department for a sledding-related injury.
The majority of patients were injured as the result of a collision (63%). Collision injuries occurred when the patient made contact with an object in the environment (47%), when they hit the ground (16%), or when they ran into another person (10%) or sled (7%).
Head injuries are a serious concern during sledding. The head was the most frequently injured body part for children. In fact, nearly 82% of those who sustained an injury to the head were children. The type of sled can also impact the risk of head injury. Children injured while riding snow tubes and disks had a greater risk of sustaining a concussion or CHI than children who were riding sleds or toboggans. Researchers recommend wearing a helmet while sledding to reduce the risk and severity of head injuries.
While less frequent (3% of all cases), injuries occurring as a result of the sled being pulled by a motorized vehicle such as a car, ATV or snowmobile resulted in more serious injuries that required hospitalization (14%). This practice should be avoided.
Rebecca McNally[/caption]
Rebecca McAdams, MA, MPH
Senior research associate
Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: Sledding is a popular winter activity in communities across the country, but it may not be as risk-free as many people think.
MedicalResearch.com: What are the main findings?
Response: We found that 220,488 patients were treated in U.S. emergency departments for injuries related to sledding from 2008 through 2017. Nearly 70% of these patients were children age 19 years and younger. Compared to adults, children were almost seven times as likely to be treated in an emergency department for a sledding-related injury.
The majority of patients were injured as the result of a collision (63%). Collision injuries occurred when the patient made contact with an object in the environment (47%), when they hit the ground (16%), or when they ran into another person (10%) or sled (7%).
Head injuries are a serious concern during sledding. The head was the most frequently injured body part for children. In fact, nearly 82% of those who sustained an injury to the head were children. The type of sled can also impact the risk of head injury. Children injured while riding snow tubes and disks had a greater risk of sustaining a concussion or CHI than children who were riding sleds or toboggans. Researchers recommend wearing a helmet while sledding to reduce the risk and severity of head injuries.
While less frequent (3% of all cases), injuries occurring as a result of the sled being pulled by a motorized vehicle such as a car, ATV or snowmobile resulted in more serious injuries that required hospitalization (14%). This practice should be avoided. 
 Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.
Dr. Soller[/caption]
Lianne Soller, PhD
Allergy Research Manager
BC Children’s Hospital Allergy Clinic
Vancouver, BC, Canada
MedicalResearch.com: What is the background for this study?
Response: Peanut oral immunotherapy (also known as OIT) has been studied for many years in clinical trials and has been found to be safe and effective in preschoolers. However, we know that clinical trials do not always reflect what happens in the real world.
We wanted to see study whether peanut OIT would work as well in the real world. This is a follow up of our preschool peanut OIT safety study published in April 2019 which noted only 0.4% severe reactions and 4% epinephrine use during build-up.

 Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:
Dr. Halpern-Felsher[/caption]
Bonnie Halpern-Felsher, PhD, FSAHM (pronouns: she/her)
Professor of Pediatrics
Taube Endowed Research Faculty Scholar
Professor (by courtesy), Epidemiology and Population Health
Professor (by courtesy), Psychiatry and Behavioral Sciences
Director of Fellows’ Scholarship, Department of Pediatrics
Director of Research, Division of Adolescent Medicine
Co-leader, Scholarly Concentrations, Pediatrics Residency Program
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: To examine adolescent and young adult e-cigarette use during the COVID-19 pandemic.
There were 4 main findings:



 Dr. Goyal[/caption]
Dr. Monika K. Goyal, MD
Associate Division Chief, Emergency Medicine
Children’s National Hospital
Department of Pediatrics, School of Medicine and Health Sciences
The George Washington University
Washington, District of Columbia
MedicalResearch.com: What is the background for this study?
Response: There has been growing attention to the disproportionate use of police force in communities of color. Therefore, we sought to investigate whether Black and Hispanic teenagers have higher rates of death due to police shootings when compared to white youth.
Dr. Goyal[/caption]
Dr. Monika K. Goyal, MD
Associate Division Chief, Emergency Medicine
Children’s National Hospital
Department of Pediatrics, School of Medicine and Health Sciences
The George Washington University
Washington, District of Columbia
MedicalResearch.com: What is the background for this study?
Response: There has been growing attention to the disproportionate use of police force in communities of color. Therefore, we sought to investigate whether Black and Hispanic teenagers have higher rates of death due to police shootings when compared to white youth.


 Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms.
 Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR.
Prof. Pottel[/caption]
Prof. Dr. Hans Pottel PhD
Professeur Invité (titre honorifique)
Faculté de Médecine
Université de Liège
KULeuven-KULAK, Kortrijk, Belgium
MedicalResearch.com: What is the background for this study? Why do we need a new GFR?
Response: The currently recommended equations have flaws, mainly because there is one equation (CKiD) recommended for children, and one recommended (CKD-EPI) for adults (by KDIGO). When transitioning from pediatric nephrology care to adult nephrology care, the switch from CKiD to CKD-EPI causes implausible jumps (of more than 50%), mainly because CKD-EPI largely overestimates GFR in young adults (18-30 years). The new equation overcomes this problem as it applies for all ages (for children and adults) and overcomes the known flaws of the currently most used equations. The new equation is less biased and more precise across the full age spectrum and for the full range of serum creatinine concentrations.
The equation was developed in 11 251 participants from 7 cohorts (development and internal validation datasets) and validated in 8 378 participants from 6 cohorts (external validation dataset). Data were coming from European and American nephrology centers. No patients of African-American ancestry were included. Actually, the previously published FAS-equation served as the basic mathematical form for the equation, but we adjusted the power coefficients for serum creatinine (very much like it was done in the CKD-EPI equation). You could say that we used properties of both the FAS and CKD-EPI equation to come to an improved equation to estimate GFR. Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"]
Dr. Ganson[/caption]
Kyle T. Ganson, PhD, MSW
Assistant Professor, Factor-Inwentash Faculty of Social Work
University of Toronto
Toronto, Canada
[caption id="attachment_55902" align="alignleft" width="132"] Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.
Dr. Nagata[/caption]
Jason Nagata, MD, MSc
Assistant Professor of Pediatrics
University of California, San Francisco
San Francisco, California, USA
MedicalResearch.com: What is the background for this study?
Response: A quarter of young adults in the US have reported being unemployed during the COVID-19 pandemic. Young adults may be especially affected by employment loss as they often work in industries most adversely affected by social distancing.
MedicalResearch.com: What are the main findings?
Response: Among a sample of nearly 5,000 young adults age 18 to 26 in the US, we found that since March 2020, young adults who lost their job or were part of a household that experienced employment loss were more likely than those with secure employment to experience four common symptoms of anxiety and depression. This was also true of young adults who expected an employment loss in the next four weeks. The study also found that symptoms of anxiety and depression were common among the sample of young adults. In the seven days prior to the survey, 75% reported being nervous, anxious or on edge, 68% reported not being able to stop or control worrying, 67% reported having little interest or pleasure in doing things, and 64% reported feeling down, depressed, or hopeless.

 Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment.
Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment. 

 Response: The background for this study involves the associations of household rules and parental awareness with youth tobacco use using data from the Population Assessment Tobacco and Health Study. Health concerns regarding non-cigarette tobacco products, specifically e-cigarettes, have been on the rise. We wanted to explore whether parents are up to date with the trends of popular tobacco products today and what role they may play in youth tobacco cessation and prevention.
The main findings of the study revealed that parents less often suspected their children’s tobacco use if their children reported using only e-cigarettes, and other non-cigarette tobacco products, when compared with cigarettes. Additionally, we found that youth who agreed with their parents that their home has strict rules for tobacco use were less likely to initiate of tobacco use compared to youth who had different understanding of the rules from their parents or youth from households with more permissive household rules.
Response: The background for this study involves the associations of household rules and parental awareness with youth tobacco use using data from the Population Assessment Tobacco and Health Study. Health concerns regarding non-cigarette tobacco products, specifically e-cigarettes, have been on the rise. We wanted to explore whether parents are up to date with the trends of popular tobacco products today and what role they may play in youth tobacco cessation and prevention.
The main findings of the study revealed that parents less often suspected their children’s tobacco use if their children reported using only e-cigarettes, and other non-cigarette tobacco products, when compared with cigarettes. Additionally, we found that youth who agreed with their parents that their home has strict rules for tobacco use were less likely to initiate of tobacco use compared to youth who had different understanding of the rules from their parents or youth from households with more permissive household rules. 


 Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).
Melanie Leung[/caption]
Melanie Leung, M.D.,C.M. candidate 2021
4th-year medical student at McGill University
Division of Allergy and Clinical Immunology
Department of Pediatrics, Montreal Children’s Hospital
McGill University Health Centre, Montreal, QC, Canada
Dr. Moshe Ben-Shoshan, MD, MSc
Pediatric allergist and immunologist at the MCH (Montreal Children’s Hospital) and
Scientist at the Research Institute of the MUHC (McGill University Health Center)
MedicalResearch.com: What is the background for this study?
Response: In Canada, up to 9% of children have at least 1 food allergy. Anaphylaxis is the most severe and potential life-threatening manifestation of food allergy. Peanuts and tree nuts are the main culprits in food-induced anaphylaxis and account for most fatal cases in North America.
Public awareness about peanut and nut anaphylaxis can help to prevent and to act promptly, in the case of anaphylactic reaction. However, the best timing for public awareness campaigns remained unknown, as no previous study looked at the potential association between specific times of the year, such as public holidays, and the incidence of peanut and tree nut anaphylaxis. Our aim was to evaluate the risk of peanut and tree nut-induced anaphylaxis on Halloween, Christmas, Easter, Diwali, Chinese New Year, and Eid al-Adha.
Data was collected from 1390 pediatric cases of peanut or nut-induced anaphylaxis across Canada (Newfoundland & Labrador, Quebec, Ontario, and British Columbia), from 2011 to 2020. 62% of children were boys and the median age was 5.4 years. We compared the average daily number of cases during each holiday and compared it to the rest of the year (i.e.: non-holiday period).
 Dr. Lara-Corrales[/caption]
Irene Lara-Corrales, MD
Associate Professor of Pediatrics at the University of Toronto
Staff physician in Pediatric Dermatology at the
Hospital for Sick Children in Toronto, Canada
She is a member of the
Dr. Lara-Corrales[/caption]
Irene Lara-Corrales, MD
Associate Professor of Pediatrics at the University of Toronto
Staff physician in Pediatric Dermatology at the
Hospital for Sick Children in Toronto, Canada
She is a member of the