Author Interviews, Cancer Research, JAMA, Race/Ethnic Diversity / 10.06.2022
Rural Cancer Survival Trails Urban Patients, Especially for Minorities
MedicalResearch.com Interview with:
[caption id="attachment_59246" align="alignleft" width="150"] Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
 Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.



 Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace.
Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace. 
 Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?

 Dr. Vashi[/caption]
Dr. Neelam Vashi MD
Director of the Boston University Center for Ethnic Skin
Dermatologist at Boston Medical Center, and
[caption id="attachment_59079" align="alignleft" width="100"]
Dr. Vashi[/caption]
Dr. Neelam Vashi MD
Director of the Boston University Center for Ethnic Skin
Dermatologist at Boston Medical Center, and
[caption id="attachment_59079" align="alignleft" width="100"] Dr. De La Garza[/caption]
Dr. Henriette De La Garza MD
Research fellow
Boston University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: The COVID-19 pandemic abruptly shifted many of our daily activities to an online world, dramatically increasing the use of electronic devices. Although visible light exposure from screens is small compared with the amount of exposure from the sun, there is concern about the long-term effects of excessive screen time. Recent studies have demonstrated that exposure to light emitted from electronic devices, even for as little as 1 hour, may cause reactive oxygen species generation, apoptosis, collagen degradation, and necrosis of skin cells. Visible light increases tyrosinase activity and induces immediate erythema in light-skinned individuals and long-lasting pigmentation in dark-skinned individuals. In recent years, tinted sunscreens have been rising in popularity because they are an effective and convenient way to protect against high-energy visible light while providing cosmetic benefits. The purpose of this analysis was to study current available options and product factors that may influence consumer preference when choosing a tinted sunscreen so dermatologists can improve their familiarity with available products and tailor their recommendations to patients with all skin tones.
Dr. De La Garza[/caption]
Dr. Henriette De La Garza MD
Research fellow
Boston University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: The COVID-19 pandemic abruptly shifted many of our daily activities to an online world, dramatically increasing the use of electronic devices. Although visible light exposure from screens is small compared with the amount of exposure from the sun, there is concern about the long-term effects of excessive screen time. Recent studies have demonstrated that exposure to light emitted from electronic devices, even for as little as 1 hour, may cause reactive oxygen species generation, apoptosis, collagen degradation, and necrosis of skin cells. Visible light increases tyrosinase activity and induces immediate erythema in light-skinned individuals and long-lasting pigmentation in dark-skinned individuals. In recent years, tinted sunscreens have been rising in popularity because they are an effective and convenient way to protect against high-energy visible light while providing cosmetic benefits. The purpose of this analysis was to study current available options and product factors that may influence consumer preference when choosing a tinted sunscreen so dermatologists can improve their familiarity with available products and tailor their recommendations to patients with all skin tones.




 Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota




 Dr. Eberly[/caption]
Lauren A. Eberly, MD, MPH
Clinical Fellow, Cardiovascular Medicine
Perelman School of Medicine
Cardiovascular Division, Perelman School of Medicine
Center for Cardiovascular Outcomes, Quality, and Evaluative Research,
Cardiovascular Center for Health Equity and Social Justice,
Leonard Davis Institute of Health Economics
University of Pennsylvania, Philadelphia
MedicalResearch.com: What is the background for this study?
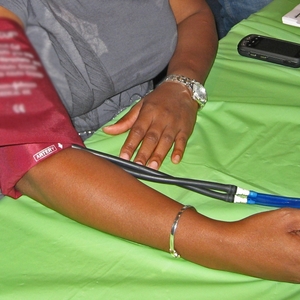
Response: Racial inequities are pervasive in our country, and cardiovascular therapeutics with proven benefit have been shown to be underutilized among Black and Latinx patients.
Glucagon-like peptide-1 receptor agonists (GLP-1 RAs), a recommended treatment option for glycemic control in patients with diabetes, have recently emerged as a cardioprotective therapy as multiple large randomized clinical trials have shown they prevent cardiovascular events among patients with Type 2 Diabetes (T2D), particularly patients with established atherosclerotic cardiovascular disease (ASCVD). Given this, they are now recommended therapy for patients with diabetes and established or high risk of ASCVD.
Given the known inequitable utilization of other therapies, along with the known higher burden of diabetes and cardiovascular disease among Black patients, the aim of this study was to evaluate the uptake of GLP-1 RA as well as for inequities in utilization.
Dr. Eberly[/caption]
Lauren A. Eberly, MD, MPH
Clinical Fellow, Cardiovascular Medicine
Perelman School of Medicine
Cardiovascular Division, Perelman School of Medicine
Center for Cardiovascular Outcomes, Quality, and Evaluative Research,
Cardiovascular Center for Health Equity and Social Justice,
Leonard Davis Institute of Health Economics
University of Pennsylvania, Philadelphia
MedicalResearch.com: What is the background for this study?
Response: Racial inequities are pervasive in our country, and cardiovascular therapeutics with proven benefit have been shown to be underutilized among Black and Latinx patients.
Glucagon-like peptide-1 receptor agonists (GLP-1 RAs), a recommended treatment option for glycemic control in patients with diabetes, have recently emerged as a cardioprotective therapy as multiple large randomized clinical trials have shown they prevent cardiovascular events among patients with Type 2 Diabetes (T2D), particularly patients with established atherosclerotic cardiovascular disease (ASCVD). Given this, they are now recommended therapy for patients with diabetes and established or high risk of ASCVD.
Given the known inequitable utilization of other therapies, along with the known higher burden of diabetes and cardiovascular disease among Black patients, the aim of this study was to evaluate the uptake of GLP-1 RA as well as for inequities in utilization.
 Jiawen Liu[/caption]
Jiawen Liu, PhD student
Department of Civil & Environmental Engineering
University of Washington
MedicalResearch.com: What is the background for this study?
Response: As previous literature has documented, racial/ethnic minority populations and lower-income populations in the US often experience higher-than-average burdens of air pollution and its associated health impacts.
The disparities vary by pollutant, location, and time. In 2014, Clark et al. found higher average NO2 exposure for nonwhites than for whites and for below-poverty-level than for above-poverty-level. Clark et al. (2017) expanded research for NO2 exposure by race-ethnicity and socioeconomic status to 2000 and 2010 and found that absolute racial-ethnic disparities decreased over time while relative racial-ethnic disparities persisted.
Jiawen Liu[/caption]
Jiawen Liu, PhD student
Department of Civil & Environmental Engineering
University of Washington
MedicalResearch.com: What is the background for this study?
Response: As previous literature has documented, racial/ethnic minority populations and lower-income populations in the US often experience higher-than-average burdens of air pollution and its associated health impacts.
The disparities vary by pollutant, location, and time. In 2014, Clark et al. found higher average NO2 exposure for nonwhites than for whites and for below-poverty-level than for above-poverty-level. Clark et al. (2017) expanded research for NO2 exposure by race-ethnicity and socioeconomic status to 2000 and 2010 and found that absolute racial-ethnic disparities decreased over time while relative racial-ethnic disparities persisted. 

 Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.


 Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
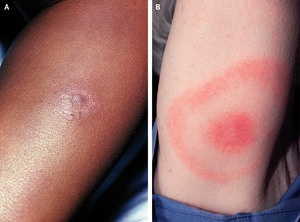
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications.
Dr. Dan P. Ly[/caption]
Division of General Internal Medicine and Health Services Research
David Geffen School of Medicine at UCLA
Los Angeles, CA
MedicalResearch.com: What is the background for this study?
Response: Lyme disease presents first on the skin with the classic “bull’s-eye” rash. But such rashes in Black patients aren’t well-represented in medical textbooks. This may lead to physicians not recognizing such rashes in Black patients.
As a result, Black patients are more likely to present with later complications of Lyme disease when first diagnosed such as neurologic complications. 


 Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.

 Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
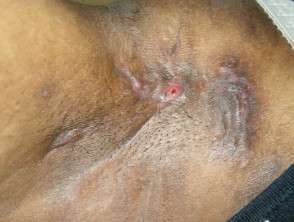
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend
Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend


 Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"]
Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"] Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
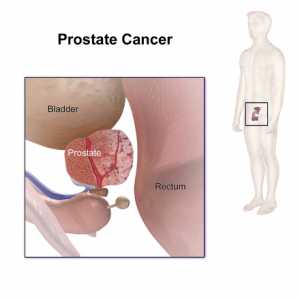
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.