Author Interviews, Cancer Research, JAMA, Lung Cancer, Surgical Research / 23.12.2015
Malignant Chest Fluid Drainage: Optimal Tube Size and Pain Control Studied
[caption id="attachment_20177" align="alignleft" width="129"] Dr. Najib Rahman[/caption]
MedicalResearch.com Interview with:
Dr Najib Rahman D Phil MSc MRCP
Consultant and Senior Lecturer
Lead for Pleural Diseases
Oxford Centre for Respiratory Medicine
Clinical Director, Oxford Respiratory Trials Unit
Tutor in Clinical Medicine
University College, Oxford
Medical Research: What is the background for this study?
Dr. Rahman : Up to TIME1, the evidence base behind optimal pleurodesis for malignant pleural effusion in terms of tube size and analgesia was poor. Optimal pleurodesis in this context is one which is successful (i.e. the patient needs no further pleural interventions for that malignant effusion), but occurs with the minimum discomfort. This is particularly important as the treatment intent in malignant effusion pleurodesis is palliative.
This is the first adequately powered randomized trial to address two important issues in pleurodesis for malignant pleural effusion - that of whether NSAIDs reduce pleurodesis efficacy, and if smaller chest tubes (12F) are "as good as" larger chest tubes (24F) for pleurodesis success and in terms of pain.
Medical Research: What are the main findings?
Dr. Rahman : The main and somewhat surprising findings are that:
Dr. Najib Rahman[/caption]
MedicalResearch.com Interview with:
Dr Najib Rahman D Phil MSc MRCP
Consultant and Senior Lecturer
Lead for Pleural Diseases
Oxford Centre for Respiratory Medicine
Clinical Director, Oxford Respiratory Trials Unit
Tutor in Clinical Medicine
University College, Oxford
Medical Research: What is the background for this study?
Dr. Rahman : Up to TIME1, the evidence base behind optimal pleurodesis for malignant pleural effusion in terms of tube size and analgesia was poor. Optimal pleurodesis in this context is one which is successful (i.e. the patient needs no further pleural interventions for that malignant effusion), but occurs with the minimum discomfort. This is particularly important as the treatment intent in malignant effusion pleurodesis is palliative.
This is the first adequately powered randomized trial to address two important issues in pleurodesis for malignant pleural effusion - that of whether NSAIDs reduce pleurodesis efficacy, and if smaller chest tubes (12F) are "as good as" larger chest tubes (24F) for pleurodesis success and in terms of pain.
Medical Research: What are the main findings?
Dr. Rahman : The main and somewhat surprising findings are that:
 Dr. Najib Rahman[/caption]
MedicalResearch.com Interview with:
Dr Najib Rahman D Phil MSc MRCP
Consultant and Senior Lecturer
Lead for Pleural Diseases
Oxford Centre for Respiratory Medicine
Clinical Director, Oxford Respiratory Trials Unit
Tutor in Clinical Medicine
University College, Oxford
Medical Research: What is the background for this study?
Dr. Rahman : Up to TIME1, the evidence base behind optimal pleurodesis for malignant pleural effusion in terms of tube size and analgesia was poor. Optimal pleurodesis in this context is one which is successful (i.e. the patient needs no further pleural interventions for that malignant effusion), but occurs with the minimum discomfort. This is particularly important as the treatment intent in malignant effusion pleurodesis is palliative.
This is the first adequately powered randomized trial to address two important issues in pleurodesis for malignant pleural effusion - that of whether NSAIDs reduce pleurodesis efficacy, and if smaller chest tubes (12F) are "as good as" larger chest tubes (24F) for pleurodesis success and in terms of pain.
Medical Research: What are the main findings?
Dr. Rahman : The main and somewhat surprising findings are that:
Dr. Najib Rahman[/caption]
MedicalResearch.com Interview with:
Dr Najib Rahman D Phil MSc MRCP
Consultant and Senior Lecturer
Lead for Pleural Diseases
Oxford Centre for Respiratory Medicine
Clinical Director, Oxford Respiratory Trials Unit
Tutor in Clinical Medicine
University College, Oxford
Medical Research: What is the background for this study?
Dr. Rahman : Up to TIME1, the evidence base behind optimal pleurodesis for malignant pleural effusion in terms of tube size and analgesia was poor. Optimal pleurodesis in this context is one which is successful (i.e. the patient needs no further pleural interventions for that malignant effusion), but occurs with the minimum discomfort. This is particularly important as the treatment intent in malignant effusion pleurodesis is palliative.
This is the first adequately powered randomized trial to address two important issues in pleurodesis for malignant pleural effusion - that of whether NSAIDs reduce pleurodesis efficacy, and if smaller chest tubes (12F) are "as good as" larger chest tubes (24F) for pleurodesis success and in terms of pain.
Medical Research: What are the main findings?
Dr. Rahman : The main and somewhat surprising findings are that:
- NSAIDs given short term but at high dose do not impair pleurodesis - they are no better than morphine for pain control (in fact, they needed modestly more rescue medication), but can be freely used during malignant effusion pleurodesis with no fear of reducing pleurodesis success.
- Smaller tubes were marginally less painful than larger tubes - but this difference was not clinically very relevant
- Smaller tubes cannot now be said to be "as good as" larger tubes for malignant effusion pleurodesis. Our data shows that they failed in non-inferiority to larger tubes for pleurodesis success at 3 months.
- Smaller tubes resulted in higher fall our rates, a higher incidence of not being able to administer talc and were associated with more complications during insertion .

 Dr. Jochen Reinöhl[/caption]
MedicalResearch.com Interview with:
Dr. Jochen Reinöhl
Consultant and Head of the ISAH team (intervention for structural and congenital cardiovascular diseases)
Department of Cardiology and Angiology I (Medical Director: Prof. Dr. Christoph Bode)
University Heart Center Freiburg ∙ Bad Krozingen
Medical Research: What is the background for this study? What are the main findings?
Dr. Reinöhl: Aortic valve stenosis is a medical condition with very high short-term mortality. Previously its only treatment – therefore the gold standard – consisted of surgical valve replacement. Since 2007 transcatheter aortic-valve replacement (TAVR) can be considered alternative. Its impact on clinical practice, however, is largely unknown.
TAVR numbers rose from 144 in 2007 to 9,147 in 2013, whereas surgical aortic-valve replacement procedures only marginally decreased from 8,622 to 7,048. For both groups in-hospital mortality, as well as, the incidence of stroke, bleeding and pacemaker implantation (but not acute kidney injury) decreased.
Dr. Jochen Reinöhl[/caption]
MedicalResearch.com Interview with:
Dr. Jochen Reinöhl
Consultant and Head of the ISAH team (intervention for structural and congenital cardiovascular diseases)
Department of Cardiology and Angiology I (Medical Director: Prof. Dr. Christoph Bode)
University Heart Center Freiburg ∙ Bad Krozingen
Medical Research: What is the background for this study? What are the main findings?
Dr. Reinöhl: Aortic valve stenosis is a medical condition with very high short-term mortality. Previously its only treatment – therefore the gold standard – consisted of surgical valve replacement. Since 2007 transcatheter aortic-valve replacement (TAVR) can be considered alternative. Its impact on clinical practice, however, is largely unknown.
TAVR numbers rose from 144 in 2007 to 9,147 in 2013, whereas surgical aortic-valve replacement procedures only marginally decreased from 8,622 to 7,048. For both groups in-hospital mortality, as well as, the incidence of stroke, bleeding and pacemaker implantation (but not acute kidney injury) decreased.
 Dr. Minneci[/caption]
MedicalResearch.com Interview with:
Dr. Peter C. Minneci, M.D., MHSc
Center for Innovation in Pediatric Practice
Assistant Professor, Pediatric Surgery
The Ohio State's Wexner Medical Center
Medical Research: What is the background for this study? What are the main findings?
Dr. Minneci: Non-operative management of uncomplicated appendicitis has been shown to safe and effective studied in several international adult trials. To be a reasonable treatment alternative to urgent appendectomy, non-operative management of appendicitis in children must have a clinically acceptable success rate with minimal harm in patients that fail and subsequently undergo appendectomy. We performed a prospective single-institution patient choice trial allowing the families of children with acute uncomplicated appendicitis to choose between urgent appendectomy or non-operative management with antibiotics alone. We enrolled 102 patients, with 65 choosing surgery and 37 choosing non-operative management with antibiotics alone. Non-operative management had an in-hospital success rate of 94%, a 30-day success rate of 89%, and a 1-year success rate of 76%. Compared to the surgery group, patients managed non-operatively reported higher quality of life scores at 30 days and had significantly fewer disability days and lower costs, with no differences in the rates of complicated appendicitis or treatment-related complications at 1 year of follow-up. With this being said, there are some cases that I have read about where doctors have failed to diagnose patients for Appendicitis even after they have complained about having a number of the symptoms associated with it. Following this, some patients have even contacted companies like
Dr. Minneci[/caption]
MedicalResearch.com Interview with:
Dr. Peter C. Minneci, M.D., MHSc
Center for Innovation in Pediatric Practice
Assistant Professor, Pediatric Surgery
The Ohio State's Wexner Medical Center
Medical Research: What is the background for this study? What are the main findings?
Dr. Minneci: Non-operative management of uncomplicated appendicitis has been shown to safe and effective studied in several international adult trials. To be a reasonable treatment alternative to urgent appendectomy, non-operative management of appendicitis in children must have a clinically acceptable success rate with minimal harm in patients that fail and subsequently undergo appendectomy. We performed a prospective single-institution patient choice trial allowing the families of children with acute uncomplicated appendicitis to choose between urgent appendectomy or non-operative management with antibiotics alone. We enrolled 102 patients, with 65 choosing surgery and 37 choosing non-operative management with antibiotics alone. Non-operative management had an in-hospital success rate of 94%, a 30-day success rate of 89%, and a 1-year success rate of 76%. Compared to the surgery group, patients managed non-operatively reported higher quality of life scores at 30 days and had significantly fewer disability days and lower costs, with no differences in the rates of complicated appendicitis or treatment-related complications at 1 year of follow-up. With this being said, there are some cases that I have read about where doctors have failed to diagnose patients for Appendicitis even after they have complained about having a number of the symptoms associated with it. Following this, some patients have even contacted companies like  Dr. Chagpar[/caption]
MedicalResearch.com Interview with:
Anees B. Chagpar, MD, MSc, MPH, MA, MBA, FRCS(C), FACS
Associate Professor, Department of Surgery
Director, The Breast Center
Smilow Cancer Hospital at Yale-New Haven
Assistant Director -- Global Oncology
Yale Comprehensive Cancer Center
Yale University School of Medicine
Medical Research: What is the background for this study?
Dr. Chagpar: Up to 40% of women undergoing breast conserving surgery for breast cancer will have to return to the operating room due to positive margins (or cancer cells being found at the edge of what was removed at the initial surgery). We recently reported the results of a randomized controlled trial, published in the
Dr. Chagpar[/caption]
MedicalResearch.com Interview with:
Anees B. Chagpar, MD, MSc, MPH, MA, MBA, FRCS(C), FACS
Associate Professor, Department of Surgery
Director, The Breast Center
Smilow Cancer Hospital at Yale-New Haven
Assistant Director -- Global Oncology
Yale Comprehensive Cancer Center
Yale University School of Medicine
Medical Research: What is the background for this study?
Dr. Chagpar: Up to 40% of women undergoing breast conserving surgery for breast cancer will have to return to the operating room due to positive margins (or cancer cells being found at the edge of what was removed at the initial surgery). We recently reported the results of a randomized controlled trial, published in the  Dr. Grovaert[/caption]
MedicalResearch.com Interview with:
Johannes Govaert MD
Department of Surgery
Leiden University Medical Center
Leiden, The Netherlands
Medical Research: What is the background for this study?
Dr. Govaert: The Value Based Health Care agenda ofPprof. Porter (Harvard Business School) suggests that focus in healthcare should shift from reducing costs to improving quality: where quality of healthcare improves, cost reduction will follow. One of the cornerstones of potential cost reduction, as mentioned by Porter, could be availability of key clinical data on processes and outcomes of care. Despite the important societal and economical role the healthcare system fulfils, it still lags behind when it comes to standardised reporting processes. With the introduction of the Dutch Surgical Colorectal Audit (DSCA) in 2009, robust quality information became available enabling monitoring, evaluation and improvement of surgical colorectal cancer care in the Netherlands. Since the introduction of the DSCA postoperative morbidity and mortality declined.
Primary aim of this study was to investigate whether improving quality of surgical colorectal cancer care, by using a national quality improvement initiative, leads to a reduction of hospital costs. Detailed clinical data was obtained from the 2010-2012 population-based Dutch Surgical Colorectal Audit. Costs at patient-level were measured uniformly in all 29 participating hospitals and based on Time-Driven Activity-Based Costing.
Medical Research: What are the main findings?
Dr. Govaert: Over three consecutive years (2010-2012) severe complications and mortality after colorectal cancer surgery respectively declined with 20% and 29%. Simultaneously, costs during primary admission decreased with 9% without increase in costs within the first 90 days after discharge. Moreover, an inverse relationship (at hospital level) between severe complication rate and hospital costs was identified among the 29 participating hospitals. Hospitals with increasing severe complication rates (between 2010 and 2012) were associated with increasing costs whereas hospitals with declining severe complication rates were associated with cost reduction.
Dr. Grovaert[/caption]
MedicalResearch.com Interview with:
Johannes Govaert MD
Department of Surgery
Leiden University Medical Center
Leiden, The Netherlands
Medical Research: What is the background for this study?
Dr. Govaert: The Value Based Health Care agenda ofPprof. Porter (Harvard Business School) suggests that focus in healthcare should shift from reducing costs to improving quality: where quality of healthcare improves, cost reduction will follow. One of the cornerstones of potential cost reduction, as mentioned by Porter, could be availability of key clinical data on processes and outcomes of care. Despite the important societal and economical role the healthcare system fulfils, it still lags behind when it comes to standardised reporting processes. With the introduction of the Dutch Surgical Colorectal Audit (DSCA) in 2009, robust quality information became available enabling monitoring, evaluation and improvement of surgical colorectal cancer care in the Netherlands. Since the introduction of the DSCA postoperative morbidity and mortality declined.
Primary aim of this study was to investigate whether improving quality of surgical colorectal cancer care, by using a national quality improvement initiative, leads to a reduction of hospital costs. Detailed clinical data was obtained from the 2010-2012 population-based Dutch Surgical Colorectal Audit. Costs at patient-level were measured uniformly in all 29 participating hospitals and based on Time-Driven Activity-Based Costing.
Medical Research: What are the main findings?
Dr. Govaert: Over three consecutive years (2010-2012) severe complications and mortality after colorectal cancer surgery respectively declined with 20% and 29%. Simultaneously, costs during primary admission decreased with 9% without increase in costs within the first 90 days after discharge. Moreover, an inverse relationship (at hospital level) between severe complication rate and hospital costs was identified among the 29 participating hospitals. Hospitals with increasing severe complication rates (between 2010 and 2012) were associated with increasing costs whereas hospitals with declining severe complication rates were associated with cost reduction.
 Dr. Soroush Zaghi[/caption]
MedicalResearch.com Interview with:
Soroush Zaghi, MD
Department of Head and Neck Surgery
David Geffen School of Medicine at UCLA
University of California, Los Angeles
MedicalResearch: What is the central message for clinicians and surgeons from your results?
Dr. Zaghi: Multiple studies from different practitioners and institutions agree that Maxillomandibular Advancement (MMA) is a highly effective surgical option for patients with obstructive sleep apnea who cannot tolerate positive pressure therapy and have not found success with other surgical procedures.
Dr. Soroush Zaghi[/caption]
MedicalResearch.com Interview with:
Soroush Zaghi, MD
Department of Head and Neck Surgery
David Geffen School of Medicine at UCLA
University of California, Los Angeles
MedicalResearch: What is the central message for clinicians and surgeons from your results?
Dr. Zaghi: Multiple studies from different practitioners and institutions agree that Maxillomandibular Advancement (MMA) is a highly effective surgical option for patients with obstructive sleep apnea who cannot tolerate positive pressure therapy and have not found success with other surgical procedures.
 Dr. Yao[/caption]
MedicalResearch.com Interview with:
Katharine Yao, MD
Director, Breast Surgical Program
NorthShore University HealthSystem
Illinois
Medical Research: What is the background for this study? What are the main findings?
Dr. Yao: A survey of breast surgeons was conducted to determine their knowledge level with contralateral breast cancer and how contralateral prophylactic mastectomy (CPM) affects survival. Of five knowledge questions, only 60% scored with high knowledge (4 or 5 questions correct) scores. Surgeons mostly scored low on contralateral cancer risks. Most surgeons correctly stated that
Dr. Yao[/caption]
MedicalResearch.com Interview with:
Katharine Yao, MD
Director, Breast Surgical Program
NorthShore University HealthSystem
Illinois
Medical Research: What is the background for this study? What are the main findings?
Dr. Yao: A survey of breast surgeons was conducted to determine their knowledge level with contralateral breast cancer and how contralateral prophylactic mastectomy (CPM) affects survival. Of five knowledge questions, only 60% scored with high knowledge (4 or 5 questions correct) scores. Surgeons mostly scored low on contralateral cancer risks. Most surgeons correctly stated that  Dr. Chunsheng Wang[/caption]
MedicalResearch.com Interview with:
Chunsheng Wang, MD
Department of Cardiovascular Surgery, Shanghai Cardiovascular Institution
and Zhongshan Hospital
Fudan University, Shanghai, China
Medical Research: What is the background for this study? What are the main findings?
Dr. Wang: Transcatheter aortic valve replacement (TAVR) has been widely used in high-risk patients for surgical aortic valve replacement. However, the majority of the TAVR devices were designed for aortic valve stenosis with significant valve calcification. For most of these devices, predominant aortic regurgitation remained to be a technological challenge because of questionable anchoring, which can result in a high incidence of valve migration and paravalvular leak. Consequently, the guidelines from the United States and the Europe suggest that candidates with predominant aortic regurgitation (>grade 3+) or noncalcified valve should not undergo
Dr. Chunsheng Wang[/caption]
MedicalResearch.com Interview with:
Chunsheng Wang, MD
Department of Cardiovascular Surgery, Shanghai Cardiovascular Institution
and Zhongshan Hospital
Fudan University, Shanghai, China
Medical Research: What is the background for this study? What are the main findings?
Dr. Wang: Transcatheter aortic valve replacement (TAVR) has been widely used in high-risk patients for surgical aortic valve replacement. However, the majority of the TAVR devices were designed for aortic valve stenosis with significant valve calcification. For most of these devices, predominant aortic regurgitation remained to be a technological challenge because of questionable anchoring, which can result in a high incidence of valve migration and paravalvular leak. Consequently, the guidelines from the United States and the Europe suggest that candidates with predominant aortic regurgitation (>grade 3+) or noncalcified valve should not undergo  Dr. Jason Gold[/caption]
MedicalResearch.com Interview with:
Jason S. Gold MD FACS
Chief of Surgical Oncology, VA Boston Healthcare System
Assistant Professor of Surgery, Harvard Medical School
Brigham and Women’s Hospital
Medical Research: What is the background for this study?
Dr. Gold: Pancreas cancer is a lethal disease. While advances in the best available care for pancreas cancer are desperately needed, improvements can be made in addressing disparities in care. This study aimed to evaluate associations of social and demographic variables with the utilization of surgical resection as well as with survival after surgical resection for early-stage pancreas cancer.
Medical Research: What are the main findings?
Dr. Gold: The main findings are the following:
1: We found that less than half of patients with early-stage pancreas cancer undergo resection in the United States. Interestingly, the rate of resection has not changed with time during the eight-year study period.
2. We also found significant disparities associated with the utilization of surgical resection for early-stage pancreas cancer in the United States. African American patients, Hispanic patients, single patients, and uninsured patients were significantly less likely to have their tumors removed. There were regional variations in the utilization of surgical resection as well. Patients in the Southeast were significantly less likely to have a pancreas resection for cancer compared to patients in the Northeast.
3. Among the patients who underwent surgical resection for early-stage pancreas cancer, we did not see significant independent associations with survival for most of the social and demographic variables analyzed. Surprisingly, however, patients from the Southeast had worse long-term survival after pancreas cancer resection compared to those in other regions of the United States even after adjusting for other variables.
Dr. Jason Gold[/caption]
MedicalResearch.com Interview with:
Jason S. Gold MD FACS
Chief of Surgical Oncology, VA Boston Healthcare System
Assistant Professor of Surgery, Harvard Medical School
Brigham and Women’s Hospital
Medical Research: What is the background for this study?
Dr. Gold: Pancreas cancer is a lethal disease. While advances in the best available care for pancreas cancer are desperately needed, improvements can be made in addressing disparities in care. This study aimed to evaluate associations of social and demographic variables with the utilization of surgical resection as well as with survival after surgical resection for early-stage pancreas cancer.
Medical Research: What are the main findings?
Dr. Gold: The main findings are the following:
1: We found that less than half of patients with early-stage pancreas cancer undergo resection in the United States. Interestingly, the rate of resection has not changed with time during the eight-year study period.
2. We also found significant disparities associated with the utilization of surgical resection for early-stage pancreas cancer in the United States. African American patients, Hispanic patients, single patients, and uninsured patients were significantly less likely to have their tumors removed. There were regional variations in the utilization of surgical resection as well. Patients in the Southeast were significantly less likely to have a pancreas resection for cancer compared to patients in the Northeast.
3. Among the patients who underwent surgical resection for early-stage pancreas cancer, we did not see significant independent associations with survival for most of the social and demographic variables analyzed. Surprisingly, however, patients from the Southeast had worse long-term survival after pancreas cancer resection compared to those in other regions of the United States even after adjusting for other variables.
 Dr. Schlansky[/caption]
MedicalResearch.com Interview with:
Barry Schlansky, M.D., M.P.H
Assistant Professor of Medicine
Oregon Health & Science University
Medical Research: What are the main findings and significance of this study?
Dr. Schlansky: This study examines how obese patients fare before and after liver transplantation. Similar to other researchers, we found that obese patients do just as well as normal weight patients after liver transplantation. We were surprised, however, to find that very obese patients died more often while on the wait list before liver transplant.
Dr. Schlansky[/caption]
MedicalResearch.com Interview with:
Barry Schlansky, M.D., M.P.H
Assistant Professor of Medicine
Oregon Health & Science University
Medical Research: What are the main findings and significance of this study?
Dr. Schlansky: This study examines how obese patients fare before and after liver transplantation. Similar to other researchers, we found that obese patients do just as well as normal weight patients after liver transplantation. We were surprised, however, to find that very obese patients died more often while on the wait list before liver transplant.
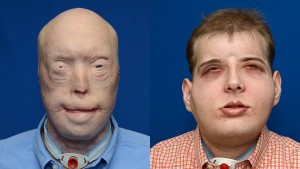 Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to
Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to  MedicalResearch.com Interview with:
Dr. Giuseppe Andò
University of Messina, Messina, Italy
Medical Research: What is the background for this study?
Dr. Andò: Patients’ preference for radial access for coronary angiography and percutaneous intervention is paralleled by an almost complete abolition of access-site bleeding. Given the deleterious impact of any clinically relevant bleeding event on short- and long-term outcomes, the use of radial access should translate into a reduction in net adverse events, especially in patients with high risk of bleeding such as those with an acute coronary syndrome. Nonetheless, studies conducted over the past decade by pioneers of
MedicalResearch.com Interview with:
Dr. Giuseppe Andò
University of Messina, Messina, Italy
Medical Research: What is the background for this study?
Dr. Andò: Patients’ preference for radial access for coronary angiography and percutaneous intervention is paralleled by an almost complete abolition of access-site bleeding. Given the deleterious impact of any clinically relevant bleeding event on short- and long-term outcomes, the use of radial access should translate into a reduction in net adverse events, especially in patients with high risk of bleeding such as those with an acute coronary syndrome. Nonetheless, studies conducted over the past decade by pioneers of 









