Author Interviews, Heart Disease, Lipids / 01.04.2020
Monoclonal Antibody Evinacumab is a Major Benefit to Patients with Homozygous Familial Hypercholesterolemia
MedicalResearch.com Interview with:
[caption id="attachment_53714" align="alignleft" width="172"] Professor F. J. Raal[/caption]
Professor F. J. Raal, FRCP, FCP(SA), Cert Endo, MMED, PhD
Director, Carbohydrate & Lipid Metabolism Research Unit
Professor & Head, Division of Endocrinology & Metabolism,
Faculty of Health Sciences, University of the Witwatersrand
MedicalResearch.com: What is the background for this study? How does Evinacumab differ from the three drugs used in triple therapy for this severe form of hypercholesterolemia?
Response: Despite available lipid lowering therapies, the vast majority of patients with homozygous familial hypercholesterolemia are unable to achieve desirable LDL-cholesterol levels and remain at high risk for premature atherosclerotic cardiovascular disease.
Unlike statins and PCSK9-inhibitors which act mainly by upregulating LDL receptor activity on the cell surface, evinacumab, a monoclonal antibody inhibitor of ANGPTL3, acts independent of the LDL receptor.
Professor F. J. Raal[/caption]
Professor F. J. Raal, FRCP, FCP(SA), Cert Endo, MMED, PhD
Director, Carbohydrate & Lipid Metabolism Research Unit
Professor & Head, Division of Endocrinology & Metabolism,
Faculty of Health Sciences, University of the Witwatersrand
MedicalResearch.com: What is the background for this study? How does Evinacumab differ from the three drugs used in triple therapy for this severe form of hypercholesterolemia?
Response: Despite available lipid lowering therapies, the vast majority of patients with homozygous familial hypercholesterolemia are unable to achieve desirable LDL-cholesterol levels and remain at high risk for premature atherosclerotic cardiovascular disease.
Unlike statins and PCSK9-inhibitors which act mainly by upregulating LDL receptor activity on the cell surface, evinacumab, a monoclonal antibody inhibitor of ANGPTL3, acts independent of the LDL receptor.
 Professor F. J. Raal[/caption]
Professor F. J. Raal, FRCP, FCP(SA), Cert Endo, MMED, PhD
Director, Carbohydrate & Lipid Metabolism Research Unit
Professor & Head, Division of Endocrinology & Metabolism,
Faculty of Health Sciences, University of the Witwatersrand
MedicalResearch.com: What is the background for this study? How does Evinacumab differ from the three drugs used in triple therapy for this severe form of hypercholesterolemia?
Response: Despite available lipid lowering therapies, the vast majority of patients with homozygous familial hypercholesterolemia are unable to achieve desirable LDL-cholesterol levels and remain at high risk for premature atherosclerotic cardiovascular disease.
Unlike statins and PCSK9-inhibitors which act mainly by upregulating LDL receptor activity on the cell surface, evinacumab, a monoclonal antibody inhibitor of ANGPTL3, acts independent of the LDL receptor.
Professor F. J. Raal[/caption]
Professor F. J. Raal, FRCP, FCP(SA), Cert Endo, MMED, PhD
Director, Carbohydrate & Lipid Metabolism Research Unit
Professor & Head, Division of Endocrinology & Metabolism,
Faculty of Health Sciences, University of the Witwatersrand
MedicalResearch.com: What is the background for this study? How does Evinacumab differ from the three drugs used in triple therapy for this severe form of hypercholesterolemia?
Response: Despite available lipid lowering therapies, the vast majority of patients with homozygous familial hypercholesterolemia are unable to achieve desirable LDL-cholesterol levels and remain at high risk for premature atherosclerotic cardiovascular disease.
Unlike statins and PCSK9-inhibitors which act mainly by upregulating LDL receptor activity on the cell surface, evinacumab, a monoclonal antibody inhibitor of ANGPTL3, acts independent of the LDL receptor.



















 Deborah M Eaton
Doctorate Student / Research Assistant
Temple University
MedicalResearch.com: What is the background for this study?
Response: Heart failure (HF) with preserved ejection fraction (HFpEF) accounts for approximately 50% of cases of HF and to date clinical trials with HFpEF patients have failed to produce positive outcomes. Part of this is likely due to the lack of HFpEF animal models for preclinical testing. Our lab addressed this gap in knowledge by developing an animal model that mimics critical features of the human HFpEF phenotype. We performed an in-depth cardiopulmonary characterization highlighting that the model has characteristics of human disease. We then tested the effects of a pan-HDAC inhibitor, vorinostat/SAHA, in collaboration with Dr. Timothy McKinsey, who is an expert in HDAC inhibitors and recently published work1 that laid the foundation for this study.
Deborah M Eaton
Doctorate Student / Research Assistant
Temple University
MedicalResearch.com: What is the background for this study?
Response: Heart failure (HF) with preserved ejection fraction (HFpEF) accounts for approximately 50% of cases of HF and to date clinical trials with HFpEF patients have failed to produce positive outcomes. Part of this is likely due to the lack of HFpEF animal models for preclinical testing. Our lab addressed this gap in knowledge by developing an animal model that mimics critical features of the human HFpEF phenotype. We performed an in-depth cardiopulmonary characterization highlighting that the model has characteristics of human disease. We then tested the effects of a pan-HDAC inhibitor, vorinostat/SAHA, in collaboration with Dr. Timothy McKinsey, who is an expert in HDAC inhibitors and recently published work1 that laid the foundation for this study. 






 Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
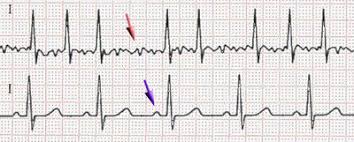
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.
Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.





