Author Interviews, Heart Disease, JAMA, Race/Ethnic Diversity, Stanford / 26.12.2018
No Evidence to Support the “Hispanic Paradox” of Cardiovascular Disease
MedicalResearch.com Interview with:
[caption id="attachment_46704" align="alignleft" width="200"] Dr. Rodriguez[/caption]
Fatima Rodriguez, MD, MPH, FACC
Assistant Professor
Cardiovascular Medicine
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The “Hispanic Paradox” is an idea based on some epidemiological observations that Hispanics have lower disease prevalence and mortality (across a wide spectrum of disease states), despite adverse risk profiles and lower socioeconomic status than their non-Hispanic white counterparts.
Our study is unique in that it includes a Hispanic population with overall high educational attainment followed longitudinally. In contrast to prior work in this area, we found no evidence in support of the Hispanic paradox for estimated atherosclerotic cardiovascular disease risk, atherosclerotic disease (as measured by CAC), or overall mortality.
Dr. Rodriguez[/caption]
Fatima Rodriguez, MD, MPH, FACC
Assistant Professor
Cardiovascular Medicine
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The “Hispanic Paradox” is an idea based on some epidemiological observations that Hispanics have lower disease prevalence and mortality (across a wide spectrum of disease states), despite adverse risk profiles and lower socioeconomic status than their non-Hispanic white counterparts.
Our study is unique in that it includes a Hispanic population with overall high educational attainment followed longitudinally. In contrast to prior work in this area, we found no evidence in support of the Hispanic paradox for estimated atherosclerotic cardiovascular disease risk, atherosclerotic disease (as measured by CAC), or overall mortality.
 Dr. Rodriguez[/caption]
Fatima Rodriguez, MD, MPH, FACC
Assistant Professor
Cardiovascular Medicine
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The “Hispanic Paradox” is an idea based on some epidemiological observations that Hispanics have lower disease prevalence and mortality (across a wide spectrum of disease states), despite adverse risk profiles and lower socioeconomic status than their non-Hispanic white counterparts.
Our study is unique in that it includes a Hispanic population with overall high educational attainment followed longitudinally. In contrast to prior work in this area, we found no evidence in support of the Hispanic paradox for estimated atherosclerotic cardiovascular disease risk, atherosclerotic disease (as measured by CAC), or overall mortality.
Dr. Rodriguez[/caption]
Fatima Rodriguez, MD, MPH, FACC
Assistant Professor
Cardiovascular Medicine
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The “Hispanic Paradox” is an idea based on some epidemiological observations that Hispanics have lower disease prevalence and mortality (across a wide spectrum of disease states), despite adverse risk profiles and lower socioeconomic status than their non-Hispanic white counterparts.
Our study is unique in that it includes a Hispanic population with overall high educational attainment followed longitudinally. In contrast to prior work in this area, we found no evidence in support of the Hispanic paradox for estimated atherosclerotic cardiovascular disease risk, atherosclerotic disease (as measured by CAC), or overall mortality.




 Dr. Steen[/caption]
Dr. Lowell H. Steen, Jr., M.D.
Interventional Cardiologist
Loyola University Medical Center
Dr. Steen discusses how holiday treats & stress can increase the risk of heart attack.
MedicalResearch.com: What are the main factors that are linked to an increase in heart related adverse events during the Christmas holiday season? Who is most at risk?
Response: The increase in holiday season heart-related hospitalizations and deaths are due to a variety of behaviors such as putting off seeking medical help until after the holidays, overeating rich foods, strenuous travel, excessive alcohol consumption and stressful family interactions. These factors can all trigger heart issues.
Factors such as age, diabetes, high cholesterol and smoking all increase heart risk. Additionally, those with high blood pressure, which is a leading risk factor for heart disease and stroke, are exceptionally at risk and should celebrate the hectic holiday season with caution.
Dr. Steen[/caption]
Dr. Lowell H. Steen, Jr., M.D.
Interventional Cardiologist
Loyola University Medical Center
Dr. Steen discusses how holiday treats & stress can increase the risk of heart attack.
MedicalResearch.com: What are the main factors that are linked to an increase in heart related adverse events during the Christmas holiday season? Who is most at risk?
Response: The increase in holiday season heart-related hospitalizations and deaths are due to a variety of behaviors such as putting off seeking medical help until after the holidays, overeating rich foods, strenuous travel, excessive alcohol consumption and stressful family interactions. These factors can all trigger heart issues.
Factors such as age, diabetes, high cholesterol and smoking all increase heart risk. Additionally, those with high blood pressure, which is a leading risk factor for heart disease and stroke, are exceptionally at risk and should celebrate the hectic holiday season with caution. 









 Dr. Yandrapalli[/caption]
Dr. Srikanth Yandrapalli
New York Medical College
NYMC · Cardiology
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Selection of coronary artery bypass grafting over percutaneous coronary intervention during an acute myocardial infarction is influenced by the extent of coronary artery disease and patient comorbidities. Prior studies have shown sex and racial differences in coronary artery diseaseburden.
We sought to identify if there are any sex and racial differences in the utilization of coronary artery bypass grafting over percutaneous coronary intervention during a revascularized first acute myocardial infarction in the US.
We found that males had a higher coronary artery bypass grafting rate than women, and compared to Whites, Blacks had lower coronary artery bypass grafting rate and Asians had higher coronary artery bypass grafting at the time of a first myocardial infarction.
Dr. Yandrapalli[/caption]
Dr. Srikanth Yandrapalli
New York Medical College
NYMC · Cardiology
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Selection of coronary artery bypass grafting over percutaneous coronary intervention during an acute myocardial infarction is influenced by the extent of coronary artery disease and patient comorbidities. Prior studies have shown sex and racial differences in coronary artery diseaseburden.
We sought to identify if there are any sex and racial differences in the utilization of coronary artery bypass grafting over percutaneous coronary intervention during a revascularized first acute myocardial infarction in the US.
We found that males had a higher coronary artery bypass grafting rate than women, and compared to Whites, Blacks had lower coronary artery bypass grafting rate and Asians had higher coronary artery bypass grafting at the time of a first myocardial infarction.



 Dr. Papoutsidakis[/caption]
Nikolaos Papoutsidakis, M.D., Ph.D.
Associate Research Scientist,
Yale University School of Medicine
New Haven, CT
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lifestyle education is a significant part of Hypertrophic Cardiomyopathy management. HCM patients, who frequently have to abstain from intense athletics, often ask if such restrictions extend to thrill-seeking activities they previously enjoyed, such as rollercoaster rides. Werealized there is very little data on this topic, which prompted us to set up this study.
We found that for Hypertrophic Cardiomyopathy patients who elected to participate in thrill-seeking activities, adverse events (defined as losing consciousness or experiencing a shock from an implantable cardioverter-defibrillator) were rare. We also asked patients (participating and non participating) about advice received from their physician on this topic. We found that, probably due to the lack of data, physicians often avoid providing advice or provide conflicting advice regarding participation in thrill seeking activities.
Dr. Papoutsidakis[/caption]
Nikolaos Papoutsidakis, M.D., Ph.D.
Associate Research Scientist,
Yale University School of Medicine
New Haven, CT
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Lifestyle education is a significant part of Hypertrophic Cardiomyopathy management. HCM patients, who frequently have to abstain from intense athletics, often ask if such restrictions extend to thrill-seeking activities they previously enjoyed, such as rollercoaster rides. Werealized there is very little data on this topic, which prompted us to set up this study.
We found that for Hypertrophic Cardiomyopathy patients who elected to participate in thrill-seeking activities, adverse events (defined as losing consciousness or experiencing a shock from an implantable cardioverter-defibrillator) were rare. We also asked patients (participating and non participating) about advice received from their physician on this topic. We found that, probably due to the lack of data, physicians often avoid providing advice or provide conflicting advice regarding participation in thrill seeking activities. 

 Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.
Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.
 Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.
Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.


 Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population. 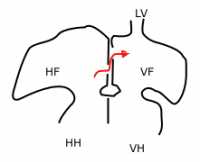
 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.