Author Interviews, Blood Pressure - Hypertension, Duke, Heart Disease, JAMA, Race/Ethnic Diversity / 14.08.2019
Not Just in the Clinic: Day and Night Blood Pressures Linked to Heart Disease Risk in African Americans
MedicalResearch.com Interview with:
[caption id="attachment_50729" align="alignleft" width="200"] Dr. Yano[/caption]
Yuichiro Yano MD
Assistant Professor in Family Medicine and Community Health
Duke University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: African Americans are disproportionally affected by hypertension-related cardiovascular disease compared with other racial/ethnic groups in the United States and have higher blood pressure levels inside and outside the clinic than whites and Asians. However, little is known, among African Americans, regarding whether higher mean blood pressure measured outside of the clinic setting on 24-hour ambulatory blood pressure monitoring is associated with an increased risk for cardiovascular disease events, independent of blood pressure measured in the clinic setting.
Dr. Yano[/caption]
Yuichiro Yano MD
Assistant Professor in Family Medicine and Community Health
Duke University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: African Americans are disproportionally affected by hypertension-related cardiovascular disease compared with other racial/ethnic groups in the United States and have higher blood pressure levels inside and outside the clinic than whites and Asians. However, little is known, among African Americans, regarding whether higher mean blood pressure measured outside of the clinic setting on 24-hour ambulatory blood pressure monitoring is associated with an increased risk for cardiovascular disease events, independent of blood pressure measured in the clinic setting.
 Dr. Yano[/caption]
Yuichiro Yano MD
Assistant Professor in Family Medicine and Community Health
Duke University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: African Americans are disproportionally affected by hypertension-related cardiovascular disease compared with other racial/ethnic groups in the United States and have higher blood pressure levels inside and outside the clinic than whites and Asians. However, little is known, among African Americans, regarding whether higher mean blood pressure measured outside of the clinic setting on 24-hour ambulatory blood pressure monitoring is associated with an increased risk for cardiovascular disease events, independent of blood pressure measured in the clinic setting.
Dr. Yano[/caption]
Yuichiro Yano MD
Assistant Professor in Family Medicine and Community Health
Duke University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: African Americans are disproportionally affected by hypertension-related cardiovascular disease compared with other racial/ethnic groups in the United States and have higher blood pressure levels inside and outside the clinic than whites and Asians. However, little is known, among African Americans, regarding whether higher mean blood pressure measured outside of the clinic setting on 24-hour ambulatory blood pressure monitoring is associated with an increased risk for cardiovascular disease events, independent of blood pressure measured in the clinic setting.













 Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
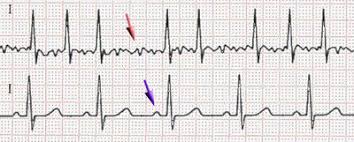
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.
Dr. Phelan[/caption]
Dermot Phelan, MD, PhD
Director of the Sports Cardiology Center
Cleveland Clinic in Cleveland, Ohio
MedicalResearch.com: What is the background for this study?
Response: It is well recognized that long-term elite endurance athletes are at higher risk of atrial fibrillation. We wished to evaluate whether this held true for primarily strength-type athletes. We had the opportunity to screen almost 500 former NFL athletes. It became clear that we were seeing more atrial fibrillation than one would expect during the screenings.

 Dr. Wee[/caption]
Christina C. Wee, MD, MPH
Associate Professor of Medicine
Harvard Medical School
Director , Obesity Research Program Division of General Medicine
Beth Israel Deaconess Medical Center (BIDMC)
Associate Program Director, Internal Medicine Program, BIDMC
Deputy Editor of the Annals of Internal Medicine
MedicalResearch.com: What is the background for this study?
Response: New research is showing that for many people without diagnosed heart disease, the risk of bleeding may outweigh the benefits of taking a daily aspirin particularly in adults over 70 years of age. The American Heart Association and the American College of Cardiology recently updated their guidelines and now explicitly recommend against aspirin use among those over the age of 70 who do not have existing heart disease or stroke.
Our study found that in 2017, a quarter of adults aged 40 years or older without cardiovascular disease – approximately 29 million people – reported taking daily aspirin for prevention of heart disease. Of these, some 6.6. million people did so without a physician's recommendation.
Dr. Wee[/caption]
Christina C. Wee, MD, MPH
Associate Professor of Medicine
Harvard Medical School
Director , Obesity Research Program Division of General Medicine
Beth Israel Deaconess Medical Center (BIDMC)
Associate Program Director, Internal Medicine Program, BIDMC
Deputy Editor of the Annals of Internal Medicine
MedicalResearch.com: What is the background for this study?
Response: New research is showing that for many people without diagnosed heart disease, the risk of bleeding may outweigh the benefits of taking a daily aspirin particularly in adults over 70 years of age. The American Heart Association and the American College of Cardiology recently updated their guidelines and now explicitly recommend against aspirin use among those over the age of 70 who do not have existing heart disease or stroke.
Our study found that in 2017, a quarter of adults aged 40 years or older without cardiovascular disease – approximately 29 million people – reported taking daily aspirin for prevention of heart disease. Of these, some 6.6. million people did so without a physician's recommendation.


















