Author Interviews, Heart Disease, JAMA / 04.05.2022
USPSTF Narrows Recommendations for Daily Aspirin Use
[caption id="attachment_56129" align="alignleft" width="133"] Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
 Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.


 Mr. Londoner[/caption]
Ken Londoner, MBA
Founder, Chief Executive Officer, Chairman, and Director
Mr. Londoner[/caption]
Ken Londoner, MBA
Founder, Chief Executive Officer, Chairman, and Director



 Dr. Torkamani[/caption]
Ali Torkamani, Ph.D.
Director of Genomics and Genome Informatics
Scripps Research Translational Institute
Professor, Integrative Structural and Computational Biology
Scripps Research
La Jolla, CA 92037
MedicalResearch.com: What is the background for this study?
Response: Prior research has shown that people with higher polygenic risk for coronary artery disease achieve greater risk reduction with statin or other lipid lowering therapy. In general, adherence to standard guidelines for lipid lowering therapy is low - about 30% of people who should be on lipid lowering therapy are, with no correlation to their genetic risk. We set out to see whether communicating personalized risk, including polygenic risk, for coronary artery disease would drive the adoption of lipid lowering therapy.
Dr. Torkamani[/caption]
Ali Torkamani, Ph.D.
Director of Genomics and Genome Informatics
Scripps Research Translational Institute
Professor, Integrative Structural and Computational Biology
Scripps Research
La Jolla, CA 92037
MedicalResearch.com: What is the background for this study?
Response: Prior research has shown that people with higher polygenic risk for coronary artery disease achieve greater risk reduction with statin or other lipid lowering therapy. In general, adherence to standard guidelines for lipid lowering therapy is low - about 30% of people who should be on lipid lowering therapy are, with no correlation to their genetic risk. We set out to see whether communicating personalized risk, including polygenic risk, for coronary artery disease would drive the adoption of lipid lowering therapy.

 Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.
Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.





 Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.
Dr. Ashwin Nathan[/caption]
Ashwin Nathan, MD, MSHP
Assistant Professor, Medicine, Perelman School of Medicine
Interventional Cardiologist
Hospital of the University of Pennsylvania and at the
Corporal Michael C. Crescenz VA Medical Center in Philadelphia
Penn Cardiovascular Outcomes, Quality & Evaluative Research Center
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We found that the rates of TAVR were lower in areas with higher proportions of Black, Hispanic and socioeconomically disadvantaged patients. Inequities in access in areas with higher proportions of Black and Hispanic patients existed despite adjusting for socioeconomic status.



 Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
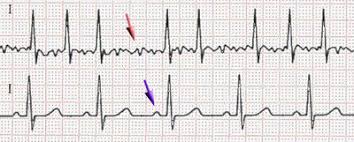
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.
Dr. Singer[/caption]
Daniel E. Singer, MD
Professor of Medicine, Harvard Medical School
Professor in the Department of Epidemiology
Harvard T.H. Chan School of Public Health
Division of General Internal Medicine
Massachusetts General Hospital
Boston, MA, 02114
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) raises the risk of ischemic stroke 4-5-fold and this risk is largely reversible by oral anticoagulants (OAC). These facts are part of the core knowledge of internal medicine and the basis of multiple guidelines. They are based on studies of patients with persistent or predominantly “heavy burden” paroxysmal AF completed in the 1990s.
More recent studies using cardiac implantable devices (CIEDs: implantable defibrillators, pacemakers, etc) which have the capacity to monitor heart rhythm continuously have found that many older patients have brief, often undiagnosed, episodes of AF. Several of these studies have found that strokes occur during periods of sinus rhythm temporally distant from a preceding episode of AF. This has led to a widespread suspicion that AF is not a direct causal risk factor but a risk “marker” indicating the presence of other truly causal features like a diseased left atrium (atrial myopathy). If the risk marker hypothesis is correct, then long-term anticoagulation is needed even for brief and rare episodes of AF (assuming the patient’ s CHA2DS2-VASc score is high enough). The key problem with prior prospective studies using CIEDs was that only a small number of strokes were observed leading to inadequate statistical power.
Our study addressed this power problem by linking the very large Optum electronic health record database which could identify ischemic strokes with the Medtronic CareLink database of long-term, continuous heart rhythm records of patients with CIEDs. We ended up studying 891 individuals who had an ischemic stroke and had 120 days of continuous heart monitoring prior to the stroke.
 Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.
Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.

 Dr. Tian[/caption]
MedicalResearch.com Interview with:
Maoyi TIAN PhD
Program Head, Digital Health and Head, Injury & Trauma
Senior Research Fellow
The George Institute
MedicalResearch.com: What is the background for this study?
Response: There is clear evidence from the literature that sodium reduction or potassium supplementation can reduce blood pressure. Reduced blood pressure can also lead to a risk reduction for cardiovascular diseases.
Salt substitute is a reduced sodium added potassium product combined those effects. Previous research of salt substitute focus on the blood pressure outcome. There is no evidence if salt substitute can reduce the risk of cardiovascular diseases or pre-mature death. This study provided a definitive evidence for this unaddressed question.
MedicalResearch.com: What are the main findings?
The main findings of the research were:
Dr. Tian[/caption]
MedicalResearch.com Interview with:
Maoyi TIAN PhD
Program Head, Digital Health and Head, Injury & Trauma
Senior Research Fellow
The George Institute
MedicalResearch.com: What is the background for this study?
Response: There is clear evidence from the literature that sodium reduction or potassium supplementation can reduce blood pressure. Reduced blood pressure can also lead to a risk reduction for cardiovascular diseases.
Salt substitute is a reduced sodium added potassium product combined those effects. Previous research of salt substitute focus on the blood pressure outcome. There is no evidence if salt substitute can reduce the risk of cardiovascular diseases or pre-mature death. This study provided a definitive evidence for this unaddressed question.
MedicalResearch.com: What are the main findings?
The main findings of the research were:

 Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).
Dr. Ribeiro[/caption]
Fernando Ribeiro PhD
School of Health Sciences
Institute of Biomedicine - iBiMED
University of Aveiro
Aveiro, Portugal
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Resistant hypertension is a puzzling problem without a clear solution. The available treatment options to lower blood pressure, namely medication and renal denervation, have had limited success, making nonpharmacological strategies good candidates to optimize the treatment of this condition.
Exercise training is consistently recommended as adjuvant therapy for patients with hypertension, yet, it is with a great delay that the efficacy of exercise training is being tested in patients with resistant hypertension.
Having that in mind, the EnRicH trial was designed to address whether the benefits of an exercise intervention with proven results in hypertensive individuals are extended to patients with resistant hypertension, a clinical population with low responsiveness to drug therapy. Exercise training was safe and associated with a significant and clinically relevant reduction in 24-hour, daytime ambulatory, and office blood pressure compared with control (usual care).



 Prof. Hypponen[/caption]
Professor Elina Hypponen
Professor in Nutritional and Genetic Epidemiology
Director: Australian Centre for Precision Health
University of South Australia
MedicalResearch.com: What is the background for this study?
Response: Diet is an important determinant of cardiovascular disease, and several studies have shown an association between high dairy and milk consumption with cardio-metabolic risk factors.
Especially high fat dairy products can increase the risk of high cholesterol and cardiovascular disease by increasing the intakes of saturated fat and dietary cholesterol.
However, milk is also a rich source of calcium and other nutrients, and evidence from randomized controlled trials has been inconsistent with respect to the role milk may have in cardiovascular health
Prof. Hypponen[/caption]
Professor Elina Hypponen
Professor in Nutritional and Genetic Epidemiology
Director: Australian Centre for Precision Health
University of South Australia
MedicalResearch.com: What is the background for this study?
Response: Diet is an important determinant of cardiovascular disease, and several studies have shown an association between high dairy and milk consumption with cardio-metabolic risk factors.
Especially high fat dairy products can increase the risk of high cholesterol and cardiovascular disease by increasing the intakes of saturated fat and dietary cholesterol.
However, milk is also a rich source of calcium and other nutrients, and evidence from randomized controlled trials has been inconsistent with respect to the role milk may have in cardiovascular health 


 Dr. Clarke[/caption]
Katherine Clark, MD MBA
Division of Cardiovascular Medicine
Department of Internal Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Racial and ethnic disparities affect cardiac transplantation outcomes. In cohort analyses of racial and ethnic groups from the previous three decades, Black patients were constantly at a higher risk of mortality after cardiac transplantation. In 2018, the United Network for Organ Sharing (UNOS) revised the allocation system to expand access to organs for the most medically urgent patients and reduce disparities and regional differences. We sought to evaluate contemporary trends and impact of the new 2018 allocation system.
Dr. Clarke[/caption]
Katherine Clark, MD MBA
Division of Cardiovascular Medicine
Department of Internal Medicine
Yale School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Racial and ethnic disparities affect cardiac transplantation outcomes. In cohort analyses of racial and ethnic groups from the previous three decades, Black patients were constantly at a higher risk of mortality after cardiac transplantation. In 2018, the United Network for Organ Sharing (UNOS) revised the allocation system to expand access to organs for the most medically urgent patients and reduce disparities and regional differences. We sought to evaluate contemporary trends and impact of the new 2018 allocation system.


