MedicalResearch.com Interview with:|
[caption id="attachment_59757" align="alignleft" width="133"]

Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
 Dr. Sapp[/caption]
John Sapp MD FRCPC FHRSHeart Rhythm, Division of Cardiology
QEII Health Sciences Centre
Dalhousie University
MedicalResearch.com: What is the background for this study?
Response: Cardiac resynchronization is a robust therapy for heart failure in patients with ventricular dysfunction, left bundle branch block and left bundle branch block. It has been shown to improve heart failure status, symptoms, survival and reduce new onset ventricular arrhythmias for appropriate candidates. The RAFT study (NEJM 2010) enrolled patients with functional class II and III heart failure, wide QRS duration on ECG and reduced left ventricular ejection fraction, and demonstrated a reduction in heart failure hospitalization and mortality during a mean follow-up of 44 months. The long-term outcomes are not known.
Dr. Sapp[/caption]
John Sapp MD FRCPC FHRSHeart Rhythm, Division of Cardiology
QEII Health Sciences Centre
Dalhousie University
MedicalResearch.com: What is the background for this study?
Response: Cardiac resynchronization is a robust therapy for heart failure in patients with ventricular dysfunction, left bundle branch block and left bundle branch block. It has been shown to improve heart failure status, symptoms, survival and reduce new onset ventricular arrhythmias for appropriate candidates. The RAFT study (NEJM 2010) enrolled patients with functional class II and III heart failure, wide QRS duration on ECG and reduced left ventricular ejection fraction, and demonstrated a reduction in heart failure hospitalization and mortality during a mean follow-up of 44 months. The long-term outcomes are not known.




 Dr. Gaba[/caption]
Prakriti Gaba, MD
Cardiovascular Medicine Fellow
Brigham and Women's Hospital
[caption id="attachment_31114" align="alignleft" width="120"]
Dr. Gaba[/caption]
Prakriti Gaba, MD
Cardiovascular Medicine Fellow
Brigham and Women's Hospital
[caption id="attachment_31114" align="alignleft" width="120"] Dr. Deepak Bhatt[/caption]
Deepak L. Bhatt MD MPH
Director of Mount Sinai Fuster Heart Hospital
Dr. Valentin Fuster Professor of Cardiovascular Medicine
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: Accurate classification of acute myocardial infarction is instrumental for the appropriate diagnosis and effective management of patients suffering from this widely prevalent cardiovascular condition.
In the past, there have been a variety of clinical scores published to advise clinicians on the best classifications schemes for patients with acute MI. These have included the Thrombolysis in Myocardial Infarction (TIMI) risk score, the HEART score, and the Killip classification. The strength of these traditional scores includes their practicality, as they can be implemented at the bedside to rapidly assist with prognostication. Nonetheless, as technologic advancements have made imaging and tissue identification more accessible, national and international committees are looking to revise traditional classification schemes of acute MI with novel ones leveraging multimodal approaches.
Dr. Deepak Bhatt[/caption]
Deepak L. Bhatt MD MPH
Director of Mount Sinai Fuster Heart Hospital
Dr. Valentin Fuster Professor of Cardiovascular Medicine
Icahn School of Medicine at Mount Sinai
MedicalResearch.com: What is the background for this study?
Response: Accurate classification of acute myocardial infarction is instrumental for the appropriate diagnosis and effective management of patients suffering from this widely prevalent cardiovascular condition.
In the past, there have been a variety of clinical scores published to advise clinicians on the best classifications schemes for patients with acute MI. These have included the Thrombolysis in Myocardial Infarction (TIMI) risk score, the HEART score, and the Killip classification. The strength of these traditional scores includes their practicality, as they can be implemented at the bedside to rapidly assist with prognostication. Nonetheless, as technologic advancements have made imaging and tissue identification more accessible, national and international committees are looking to revise traditional classification schemes of acute MI with novel ones leveraging multimodal approaches.





 Dr. Finn[/caption]
Aloke V. Finn MD
Medical Director/Chief Scientific Officer
CVPath Institute Inc.
Gaithersburg, MD 20878
MedicalResearch.com: What is the background for this study?
Response:Transcatheter left atrial appendageal closure (LAAC) has become an established therapeutic approach for prevention of stroke in subjects with non-valvular atrial fibrillation who are ineligible for long-term oral anticoagulation. Device-related thrombus (DRT), developing after LAAO procedures occurs in a small proportion but patients receiving these devices but is associated with critical embolic events such as ischemic stroke. Thrombogenicity and delayed endothelialization of fabric play a role in the development of DRT. Fluorinated polymers are known to have thromboresistant properties which may favorably modify blood biomaterial interactions of a LAAO device.
In this study we compared the thrombogenicity and endothelial coverage (EC) after left atrial appendage occlusion (LAAO) between a novel fluoropolymer-coated Watchman (FP-WM (Watchman FLX PRO) and the conventional uncoated Watchman FLX (WM).
Dr. Finn[/caption]
Aloke V. Finn MD
Medical Director/Chief Scientific Officer
CVPath Institute Inc.
Gaithersburg, MD 20878
MedicalResearch.com: What is the background for this study?
Response:Transcatheter left atrial appendageal closure (LAAC) has become an established therapeutic approach for prevention of stroke in subjects with non-valvular atrial fibrillation who are ineligible for long-term oral anticoagulation. Device-related thrombus (DRT), developing after LAAO procedures occurs in a small proportion but patients receiving these devices but is associated with critical embolic events such as ischemic stroke. Thrombogenicity and delayed endothelialization of fabric play a role in the development of DRT. Fluorinated polymers are known to have thromboresistant properties which may favorably modify blood biomaterial interactions of a LAAO device.
In this study we compared the thrombogenicity and endothelial coverage (EC) after left atrial appendage occlusion (LAAO) between a novel fluoropolymer-coated Watchman (FP-WM (Watchman FLX PRO) and the conventional uncoated Watchman FLX (WM).








 Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
Dr. Simin Liu[/caption]
Simin Liu MD MPH ScD
Professor of Epidemiology at the School of Public Health,
Professor of Medicine (Endocrinology) and
Professor of Surgery at the Alpert School of Medicine
Brown University
MedicalResearch.com: What is the background for this study?
Response: Our research team has been researching the roles of environmental and genetic determinants of chronic diseases for nearly three decades, with special emphasis on evaluating micronutrients, minerals, and trace elements in relation to cardiometabolic outcomes, and findings of which have contributed to the design of several large, randomized trials of dietary supplements in the US (Liu JAMA 1999; 2011; Diabetes Care 2005a,b; Diabetes 2006). Several large intervention trials have consistently shown beneficial effects on clinical cardiometabolic outcomes of a diet pattern rich in micronutrients, although research on micronutrient supplementation has mainly focused on the health effects of a single or a few vitamins and minerals.
We decided to take a comprehensive and systematic approach to evaluate all the publicly available/accessible studies reporting all micronutrients including phytochemicals and antioxidant supplements and their effects on cardiovascular risk factors as well as multiple CVDs.
 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
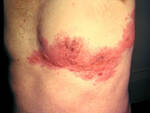
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.









 Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.
Dr. Barry[/caption]
Michael J. Barry, M.D
Director of the Informed Medical Decisions Program
Health Decision Sciences Center
Massachusetts General Hospital.
Professor of medicine at Harvard Medical School
Dr. Barry was appointed as Vice Chair of USPSTF in March 2021.
He previously served as a member from January 2017 through December 2020.
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The Task Force looked at the use of vitamin and mineral supplementation specifically for the prevention of heart disease, stroke, and cancer. We found that there is not enough evidence to recommend for or against taking multivitamin supplements, nor the use of single or paired nutrient supplements, to prevent these conditions.
However, we do know that you should not take vitamin E or beta-carotene for this purpose.

