Alcohol, Author Interviews, Heart Disease, JACC / 09.05.2021
Moderate Alcohol Intake May Reduce Cardiovascular Events Through Stress Reduction
MedicalResearch.com Interview with:
[caption id="attachment_57388" align="alignleft" width="150"] Dr. Mezue[/caption]
Kenechukwu Ndubisi Mezue, M.D
Fellow in Nuclear Cardiology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Observational studies have shown that moderate alcohol intake may have beneficial effects on cardiovascular disease. However, the mechanisms through which this benefit occurs is mostly unknown. Chronic stress is also known to associate with increased risk of cardiovascular disease and our group has shown in previous work that increased activity in the stress-associated regions of the brain (such as the amygdala) is significantly associated with increased bone marrow activity, arterial inflammation, and cardiovascular events.
Our current study hypothesizes that moderate alcohol intake reduces cardiovascular events by reducing chronic stress-associated brain activity.
Dr. Mezue[/caption]
Kenechukwu Ndubisi Mezue, M.D
Fellow in Nuclear Cardiology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Observational studies have shown that moderate alcohol intake may have beneficial effects on cardiovascular disease. However, the mechanisms through which this benefit occurs is mostly unknown. Chronic stress is also known to associate with increased risk of cardiovascular disease and our group has shown in previous work that increased activity in the stress-associated regions of the brain (such as the amygdala) is significantly associated with increased bone marrow activity, arterial inflammation, and cardiovascular events.
Our current study hypothesizes that moderate alcohol intake reduces cardiovascular events by reducing chronic stress-associated brain activity.
 Dr. Mezue[/caption]
Kenechukwu Ndubisi Mezue, M.D
Fellow in Nuclear Cardiology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Observational studies have shown that moderate alcohol intake may have beneficial effects on cardiovascular disease. However, the mechanisms through which this benefit occurs is mostly unknown. Chronic stress is also known to associate with increased risk of cardiovascular disease and our group has shown in previous work that increased activity in the stress-associated regions of the brain (such as the amygdala) is significantly associated with increased bone marrow activity, arterial inflammation, and cardiovascular events.
Our current study hypothesizes that moderate alcohol intake reduces cardiovascular events by reducing chronic stress-associated brain activity.
Dr. Mezue[/caption]
Kenechukwu Ndubisi Mezue, M.D
Fellow in Nuclear Cardiology
Massachusetts General Hospital
MedicalResearch.com: What is the background for this study?
Response: Observational studies have shown that moderate alcohol intake may have beneficial effects on cardiovascular disease. However, the mechanisms through which this benefit occurs is mostly unknown. Chronic stress is also known to associate with increased risk of cardiovascular disease and our group has shown in previous work that increased activity in the stress-associated regions of the brain (such as the amygdala) is significantly associated with increased bone marrow activity, arterial inflammation, and cardiovascular events.
Our current study hypothesizes that moderate alcohol intake reduces cardiovascular events by reducing chronic stress-associated brain activity. 


 Dr. Gamboa Madeira[/caption]
Sara Gamboa Madeira
Medical Doctor - General & Family Physician
PhD Student - EnviHealth&Co - Faculty of Medicine
Lisbon University
MedicalResearch.com: What is the background for this study?
Response: One in every five employees work in shifts across Europe1. Shift work have been associated with an increased risk for several cardiovascular diseases2 and three main mechanism have been proposed: unhealthy behaviours, disturbed sleep, and circadian misalignment.
This study focused on the role of circadian misalignment, which we assessed via social jetlag. Social jetlag is calculated using the Munich Chronotype Questionnaire3 by the difference between sleep behaviour on free-days (mainly driven by the individual “biological clock”, also called chronotype) and sleep behaviour on workdays (mainly drive by the “social clock”, namely work schedules). Chronotype is an individual feature which ranges from early/morning people to late/evening people (from proverbial lark to owls), with the majority of the population falling in between as a Gaussian distribution. Therefore higher levels of social jetlag mean a greater mismatch between what your biological clock need (e.g. go to sleep at 9pm) and what your social obligations impose on you (e.g. work until midnight).
Dr. Gamboa Madeira[/caption]
Sara Gamboa Madeira
Medical Doctor - General & Family Physician
PhD Student - EnviHealth&Co - Faculty of Medicine
Lisbon University
MedicalResearch.com: What is the background for this study?
Response: One in every five employees work in shifts across Europe1. Shift work have been associated with an increased risk for several cardiovascular diseases2 and three main mechanism have been proposed: unhealthy behaviours, disturbed sleep, and circadian misalignment.
This study focused on the role of circadian misalignment, which we assessed via social jetlag. Social jetlag is calculated using the Munich Chronotype Questionnaire3 by the difference between sleep behaviour on free-days (mainly driven by the individual “biological clock”, also called chronotype) and sleep behaviour on workdays (mainly drive by the “social clock”, namely work schedules). Chronotype is an individual feature which ranges from early/morning people to late/evening people (from proverbial lark to owls), with the majority of the population falling in between as a Gaussian distribution. Therefore higher levels of social jetlag mean a greater mismatch between what your biological clock need (e.g. go to sleep at 9pm) and what your social obligations impose on you (e.g. work until midnight).

 Dr. Virani[/caption]
Senior & Corresponding Author
Salim S. Virani, MD, PhD, FACC, FAHA, FASPC
Professor, Section of Cardiovascular Research
Director, Cardiology Fellowship Training Program
Baylor College of Medicine
Staff Cardiologist, Michael E. DeBakey Veterans Affairs Medical Center
Co-Director, VA Advanced Fellowship in Health Services Research & Development Michael E. DeBakey VA Medical Center, Houston, TX
Investigator, Health Policy, Quality and Informatics Program
Michael E. DeBakey Veterans Affairs Medical Center HSR&D Center of Innovation
Houston, TX
MedicalResearch.com: What is the background for this study?
Response: Atherosclerotic cardiovascular disease (ASCVD), defined as ischemic heart disease (IHD), ischemic cerebrovascular disease (ICVD), or peripheral arterial disease (PAD), is the leading cause of death globally. Particularly in young ASCVD patients, secondary prevention with antiplatelet therapy and statins are extremely important in reducing disease burden.
Dr. Virani[/caption]
Senior & Corresponding Author
Salim S. Virani, MD, PhD, FACC, FAHA, FASPC
Professor, Section of Cardiovascular Research
Director, Cardiology Fellowship Training Program
Baylor College of Medicine
Staff Cardiologist, Michael E. DeBakey Veterans Affairs Medical Center
Co-Director, VA Advanced Fellowship in Health Services Research & Development Michael E. DeBakey VA Medical Center, Houston, TX
Investigator, Health Policy, Quality and Informatics Program
Michael E. DeBakey Veterans Affairs Medical Center HSR&D Center of Innovation
Houston, TX
MedicalResearch.com: What is the background for this study?
Response: Atherosclerotic cardiovascular disease (ASCVD), defined as ischemic heart disease (IHD), ischemic cerebrovascular disease (ICVD), or peripheral arterial disease (PAD), is the leading cause of death globally. Particularly in young ASCVD patients, secondary prevention with antiplatelet therapy and statins are extremely important in reducing disease burden.

 Dr. Raisi-Estabra[/caption]
Dr Zahra Raisi-Estabragh, PhD fellow
Cardiologist Trainee at Queen Mary University of London and
Barts Health NHS Trust
MedicalResearch.com: What is the background for this study?
Response: Previous studies have linked greater consumption of red and processed meat to poorer clinical cardiovascular outcomes, for example, higher risk of having a heart attack or of dying from heart disease. However, the biological mechanisms underlying these relationships are not well understood. Furthermore, the impact of meat intake on more direct measures of heart health, such as, structure and function of the heart and blood vessels, has not been previously studied in large cohorts. Examining how meat intake may influence different aspects of cardiovascular health can help us better understand its health effects.
Dr. Raisi-Estabra[/caption]
Dr Zahra Raisi-Estabragh, PhD fellow
Cardiologist Trainee at Queen Mary University of London and
Barts Health NHS Trust
MedicalResearch.com: What is the background for this study?
Response: Previous studies have linked greater consumption of red and processed meat to poorer clinical cardiovascular outcomes, for example, higher risk of having a heart attack or of dying from heart disease. However, the biological mechanisms underlying these relationships are not well understood. Furthermore, the impact of meat intake on more direct measures of heart health, such as, structure and function of the heart and blood vessels, has not been previously studied in large cohorts. Examining how meat intake may influence different aspects of cardiovascular health can help us better understand its health effects. 

 Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
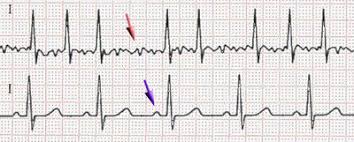
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
Dr. Fornwalt[/caption]
Brandon K Fornwalt, MD, PhD
Associate Professor, Director Department of Imaging Science and Innovation
Geisinger
MedicalResearch.com: What is the background for this study?
Response: Atrial fibrillation (AF) is an abnormal heart rhythm that is associated with outcomes such as stroke, heart failure and death. If we know a patient has atrial fibrillation, we can treat them to reduce the risk of stroke by nearly two-thirds. Unfortunately, patients often don’t know they have AF. They present initially with a stroke, and we have no chance to treat them before this happens. If we could predict who is at high risk of either currently having AF or developing it in the near future, we could intervene earlier and hopefully reduce bad outcomes like stroke. Artificial intelligence approaches may be able to help with this task.
 Anne Yuk-Lam Ho, MPH
Million Veteran Program (MVP) Data Core
MVP Coordinating Center
VA Boston Healthcare System
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) has been the leading cause of morbidity and mortality globally. Prevalence of CVD among US population is approximately 7% which places huge burden on our healthcare systems. And prevalence of CVD is as high as 28% among veterans at the VA healthcare system as veteran users are primarily older male with more histories of comorbidities. Most CVD risk factors including lipids and blood pressure can be controlled by lifestyle modifications, such as diet.
Chocolate is among dietary factors that play a role in modulating CVD risk factors is widely consumed in the US (~2.8 billion pounds annually. Although previous studies have reported beneficial effects of chocolate and/or cacao products (rich in flavonoids) on lipids, glucose metabolism and risk of diabetes, and lipids, little is known about the association of chocolate intake with coronary artery disease (CAD) among US veterans. Thus, sought to test the hypothesis that chocolate consumption is associated with a lower risk of CAD among xxx US veterans enrolled in the Million Veteran Program.
Anne Yuk-Lam Ho, MPH
Million Veteran Program (MVP) Data Core
MVP Coordinating Center
VA Boston Healthcare System
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) has been the leading cause of morbidity and mortality globally. Prevalence of CVD among US population is approximately 7% which places huge burden on our healthcare systems. And prevalence of CVD is as high as 28% among veterans at the VA healthcare system as veteran users are primarily older male with more histories of comorbidities. Most CVD risk factors including lipids and blood pressure can be controlled by lifestyle modifications, such as diet.
Chocolate is among dietary factors that play a role in modulating CVD risk factors is widely consumed in the US (~2.8 billion pounds annually. Although previous studies have reported beneficial effects of chocolate and/or cacao products (rich in flavonoids) on lipids, glucose metabolism and risk of diabetes, and lipids, little is known about the association of chocolate intake with coronary artery disease (CAD) among US veterans. Thus, sought to test the hypothesis that chocolate consumption is associated with a lower risk of CAD among xxx US veterans enrolled in the Million Veteran Program.




 Dr. El Khoudary[/caption]
Samar El Khoudary, PhD, MPH, BPharm, FAHA
Associate Professor of Epidemiology
University of Pittsburgh Graduate School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Research increasingly shows that it isn’t so important how much fat a woman is carrying, which doctors typically measure using weight and BMI, as it is where she is carrying that fat. To investigate this, we looked at 25 years of data on 362 women from Pittsburgh and Chicago who participated in the
Dr. El Khoudary[/caption]
Samar El Khoudary, PhD, MPH, BPharm, FAHA
Associate Professor of Epidemiology
University of Pittsburgh Graduate School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Research increasingly shows that it isn’t so important how much fat a woman is carrying, which doctors typically measure using weight and BMI, as it is where she is carrying that fat. To investigate this, we looked at 25 years of data on 362 women from Pittsburgh and Chicago who participated in the 













 Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
Dr. Flaherty[/caption]
Michael R. Flaherty, DO
Attending, Pediatric Critical Care Medicine
Co-Director, Trauma and Injury Prevention Outreach Program, MGH
Instructor in Pediatrics,
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study was a joint collaboration between Massachusetts General Hospital and Boston Children’s Hospital. The Consumer Product Safety Commission (CPSC) found an increasing incidence of rare earth magnet ingestions by children causing serious injury; Injuries are particularly serious when a child ingests two of these small magnets, or a magnet with another metal object – this can lead to bowel walls becoming attached and kinked, leading to catastrophic bowel injury and/or death.
The Consumer Product Safety Commission initiated campaigns to limit sales in 2012 with voluntary recalls and safety standards, as well as public awareness campaigns, legislative advocacy, and lawsuits. In October 2014, the CPSC published their final rule, “Safety Standard for Magnet Sets,” which prohibited the sale of magnets based on a pre-specified size and power scale, essentially eliminating the ability to sell SREMs. This rule was appealed by largest manufacturer of these magnets, Zen Magnets, LLC., and in November 2016 this rule was legally reversed by the U.S. Court of Appeals Tenth Circuit resulting in a resurgence of these magnets on the market.
 Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms.
Dr. Kubik[/caption]
Martha Kubik, Ph.D., R.N.
Professor and director of the School of Nursing
College of Health and Human Services at George Mason University
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study? What are the main findings? Has the recommendation changed over the last decade?
Response: High blood pressure is becoming more common among children and teens in the United States and can have serious negative health effects in childhood and adulthood, such as kidney and heart disease. However, there is not enough research to know whether treating high blood pressure in young people improves cardiovascular health in adulthood.
The Task Force continued to find that there is not enough evidence to recommend for or against screening for high blood pressure in children and teens who do not have signs or symptoms.