MedicalResearch.com Interview with:
[caption id="attachment_44092" align="alignleft" width="200"]
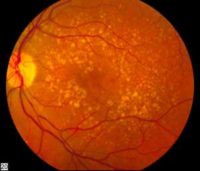
Picture of the back of the eye showing intermediate age-related macular degeneration: Wikipedia image[/caption]
Jason Hsu, MD
Retina Service, Wills Eye Hospital
Associate Professor of Ophthalmology
Thomas Jefferson University
Mid Atlantic Retina
Anthony Obeid MD MPH
School of Public Health
The University of Sydney ·
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Neovascular age-related macular degeneration (nAMD) is a vision-threatening disease that often afflicts elderly patients. The introduction of intravitreal anti-vascular endothelial growth factor treatment drastically improved the prognosis of eyes with nAMD. Despite its efficacy, patients require consistent follow-up (sometimes as often as monthly), with ongoing injections to maintain the visual benefits of the drug. Unfortunately, few studies have reported the number of patients that do not follow-up with recommended guidelines. Moreover, there remains limited evidence on the risk factors associated with loss to follow-up.
Our study, consisting of 9007 patients with a history of nAMD receiving treatment between 2012 and 2016, evaluated both these parameters. We defined loss to follow-up as having at least one injection without a subsequent follow-up visit within 12 months post-treatment.
Using this definition, we found that over 20% of patients are lost to follow-up over the entire study period. We further identified key risk factors associated with loss to follow-up, which included patients of older age, race, patients residing in a region of a lower average adjusted gross income, patients living at greater distances from clinic, patients with active nAMD in only one eye, and patients with worse visual acuity.
 Dr. Gerlach[/caption]
Lauren B. Gerlach, D.O.
Clinical Lecturer
Department of Psychiatry
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In this study we used data from the Supporting Seniors Receiving Treatment and Intervention or SUSTAIN program. The program provides a supplement to a Pennsylvania medication coverage program for low-income older adults. It provides behavioral health and case management services by phone across the state. This included detailed interviews to screen for mental health issues including anxiety, depression, sleep issues, and pain, as well as analysis of prescription records and other clinical data.
Among older adults prescribed a new benzodiazepine prescription by a non-psychiatric provider, we determined how many then went on to long-term use of the medication and what patient and clinical characteristics predicted long-term use over the following year.
Dr. Gerlach[/caption]
Lauren B. Gerlach, D.O.
Clinical Lecturer
Department of Psychiatry
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In this study we used data from the Supporting Seniors Receiving Treatment and Intervention or SUSTAIN program. The program provides a supplement to a Pennsylvania medication coverage program for low-income older adults. It provides behavioral health and case management services by phone across the state. This included detailed interviews to screen for mental health issues including anxiety, depression, sleep issues, and pain, as well as analysis of prescription records and other clinical data.
Among older adults prescribed a new benzodiazepine prescription by a non-psychiatric provider, we determined how many then went on to long-term use of the medication and what patient and clinical characteristics predicted long-term use over the following year.





















![MedicalResearch.com Interview with: Cole Wayant Oklahoma State University Center for Health Sciences ‐ Analytical and Institutional Research Tulsa, OK MedicalResearch.com: What is the background for this study? What are the main findings? Response: New FDA-approved oncology drugs are essential to oncology practice. These drugs may immediately change clinical care by offering better treatments for common, lethal forms of cancer. But, new FDA-approved oncology drugs are expensive and have been shown to have variable efficacy. Given the importance of new FDA-approved oncology drugs to patients and physicians, the trials that underpin the FDA-approval of these drugs must be free from bias and transparent. Therefore, we investigated the financial relationships between oncologist-authors of clinical trials that underpin FDA-approvals. MedicalResearch.com: What should readers take away from your report? Response: The key takeaway from our study is that oncologist-authors often do not fully disclose their financial relationships with pharmaceutical companies. Financial disclosures are important for the reasons of transparency and trust between physicians and other stakeholders, such as patients. Disclosing conflicts of interest helps readers interpret the findings of a research study, especially given the fact that drug companies finance their own drug trials. MedicalResearch.com: What recommendations do you have for future research as a result of this work? Response: In the future, beyond recommending that authors fully disclose all financial relationships with the sponsor of the trial, I recommend that journals use the Open Payments Database to verify the accuracy and completeness of author disclosure statements. Doing so is a small first step toward mitigating the potential for financial bias in the oncology literature.” Disclosures: I do not have anything else to add. None of the authors have conflicts of interest - financial or otherwise. Citation: Financial Conflicts of Interest Among Oncologist Authors of Reports of Clinical Drug Trials [wysija_form id="3"] [last-modified] The information on MedicalResearch.com is provided for educational purposes only, and is in no way intended to diagnose, cure, or treat any medical or other condition. Always seek the advice of your physician or other qualified health and ask your doctor any questions you may have regarding a medical condition. In addition to all other limitations and disclaimers in this agreement, service provider and its third party providers disclaim any liability or loss in connection with the content provided on this website.](https://medicalresearch.com/wp-content/uploads/Cole-Wayant.jpg)