Author Interviews, JAMA, Opiods, Surgical Research, University of Michigan / 07.11.2018
Most Surgical Patients Only Use About 25% Of Their Prescribed Opioids
MedicalResearch.com Interview with:
Joceline Vu, MD
Resident, PGY-5
Department of Surgery
University of Michigan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study examined how much opioid patients use after surgery, and looked at factors that might predispose some patients to use more or less.
Patient opioid use after surgery is an interesting question that’s gained a lot of attention recently, because it’s different from other uses for opioids. If you have chronic pain, you’re probably going to use all of your prescription. But if you have surgery, you may not take all of your pills, and this leaves people with leftover pills that can be dangerous later.
From this study, we found that patients only use, on average, about quarter of their prescription, meaning that a lot of them are left with leftover pills. Moreover, we found that the biggest determinant of how much they used wasn’t how much pain they reported, or any other factor—it was how big their original prescription was.
What this means is that opioid use after surgery isn’t just determined by pain, but also by what surgeons prescribe. It’s important to keep this in mind as we try to reduce unnecessary opioid prescribing after surgical procedures.



 Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.
Dr. Yano[/caption]
Yuichiro Yano MD PhD
Assistant Professor in Community and Family Medicine
Duke University
MedicalResearch.com: What is the background for this study?
Response: New blood pressure guidelines, issued in 2017 in the US, lowered the blood pressure thresholds for hypertension from systolic blood pressure/diastolic ≥140/90 mm Hg to systolic/diastolic ≥130/80 mm Hg. This change increased the prevalence of hypertension two- to three-fold among young adults. The guidelines also newly defined elevated blood pressure as, 120-129 mmHg systolic blood pressure over 80 mmHg diastolic or less. However, no study investigated that high blood pressure, as defined by the new criteria, is something that younger people should be concerned about as a potential precursor to serious problems.
Our study is among the first to report that people younger than age 40 who have elevated blood pressure or hypertension are at increased risk of heart failure, strokes and blood vessel blockages as they age.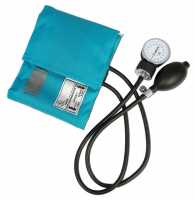













 Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.
Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.

 Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.
Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.

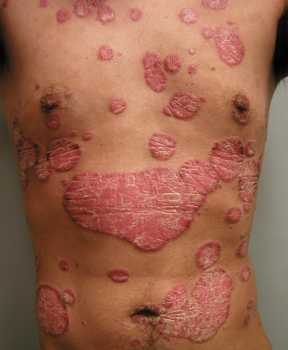
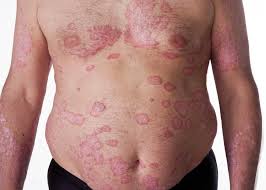 Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease.
Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease. 







