Author Interviews, Leukemia, NEJM, Transplantation / 08.09.2016
Cord Blood Transplant in Leukemia With Minimal Residual Disease
MedicalResearch.com Interview with:
[caption id="attachment_27654" align="alignleft" width="133"] Dr. Filippo Milano[/caption]
Dr. Filippo Milano, MD, PhD
Assistant Member, Clinical Research Division
Associate Director Cord Blood Transplantation
Cord Blood Program
Assistant Professor, University of Washington
Fred Hutchinson Cancer Research Center
MedicalResearch.com: What is the background for this study?
Response: When first introduced, cord blood (CB) graft was used only as a last resort when no suitable conventional donor could be identified, largely due to the limiting cell doses available in a cord blood graft. A CB graft, however, is attractive due to the increased level of HLA disparity that can be tolerated, without increased risk of graft versus host disease, allowing nearly all patients to find such a donor.
The main intent of the study was to evaluate whether or not, at our Institution, cord blood SHOULD STILL BE considered only AS an alternative DONOR or IF instead outcomes were comparable to those obtained with more “conventional” types of transplants from matched and mismatched unrelated donors.
Dr. Filippo Milano[/caption]
Dr. Filippo Milano, MD, PhD
Assistant Member, Clinical Research Division
Associate Director Cord Blood Transplantation
Cord Blood Program
Assistant Professor, University of Washington
Fred Hutchinson Cancer Research Center
MedicalResearch.com: What is the background for this study?
Response: When first introduced, cord blood (CB) graft was used only as a last resort when no suitable conventional donor could be identified, largely due to the limiting cell doses available in a cord blood graft. A CB graft, however, is attractive due to the increased level of HLA disparity that can be tolerated, without increased risk of graft versus host disease, allowing nearly all patients to find such a donor.
The main intent of the study was to evaluate whether or not, at our Institution, cord blood SHOULD STILL BE considered only AS an alternative DONOR or IF instead outcomes were comparable to those obtained with more “conventional” types of transplants from matched and mismatched unrelated donors.
 Dr. Filippo Milano[/caption]
Dr. Filippo Milano, MD, PhD
Assistant Member, Clinical Research Division
Associate Director Cord Blood Transplantation
Cord Blood Program
Assistant Professor, University of Washington
Fred Hutchinson Cancer Research Center
MedicalResearch.com: What is the background for this study?
Response: When first introduced, cord blood (CB) graft was used only as a last resort when no suitable conventional donor could be identified, largely due to the limiting cell doses available in a cord blood graft. A CB graft, however, is attractive due to the increased level of HLA disparity that can be tolerated, without increased risk of graft versus host disease, allowing nearly all patients to find such a donor.
The main intent of the study was to evaluate whether or not, at our Institution, cord blood SHOULD STILL BE considered only AS an alternative DONOR or IF instead outcomes were comparable to those obtained with more “conventional” types of transplants from matched and mismatched unrelated donors.
Dr. Filippo Milano[/caption]
Dr. Filippo Milano, MD, PhD
Assistant Member, Clinical Research Division
Associate Director Cord Blood Transplantation
Cord Blood Program
Assistant Professor, University of Washington
Fred Hutchinson Cancer Research Center
MedicalResearch.com: What is the background for this study?
Response: When first introduced, cord blood (CB) graft was used only as a last resort when no suitable conventional donor could be identified, largely due to the limiting cell doses available in a cord blood graft. A CB graft, however, is attractive due to the increased level of HLA disparity that can be tolerated, without increased risk of graft versus host disease, allowing nearly all patients to find such a donor.
The main intent of the study was to evaluate whether or not, at our Institution, cord blood SHOULD STILL BE considered only AS an alternative DONOR or IF instead outcomes were comparable to those obtained with more “conventional” types of transplants from matched and mismatched unrelated donors.




 Dr. Maria Luisa Alegre[/caption]
Maria-Luisa Alegre, MD, PhD
Professor of medicine
University of Chicago
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Most of the research that investigates why/how transplanted organs are rejected has focused on the genetic disparities between the donor and the recipient. Foreign proteins in the donor organ are recognized by the immune system of the host, which becomes activated to reject the transplanted organ. This is why transplant recipients need to take immunosuppressive medications for the rest of their lives.
Whether environmental factors, in addition to genetic factors, can also affect how the immune system is activated by the transplanted organ is much less understood. In particular, the microbiota, the communities of microbes that live on and in our body, is distinct in each individual and is known to affect the function of the immune system in diseases ranging from autoimmunity to cancer.
Using mouse models of skin and heart transplantation, we investigated if the microbiota was an environmental factor that could affect the speed at which the immune system rejects a transplanted organ.
We found that the microbial communities that colonize the donor and the host fine-tune the function of the immune system and control the strength with which the immune system reacts to a transplanted organ.
Dr. Maria Luisa Alegre[/caption]
Maria-Luisa Alegre, MD, PhD
Professor of medicine
University of Chicago
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Most of the research that investigates why/how transplanted organs are rejected has focused on the genetic disparities between the donor and the recipient. Foreign proteins in the donor organ are recognized by the immune system of the host, which becomes activated to reject the transplanted organ. This is why transplant recipients need to take immunosuppressive medications for the rest of their lives.
Whether environmental factors, in addition to genetic factors, can also affect how the immune system is activated by the transplanted organ is much less understood. In particular, the microbiota, the communities of microbes that live on and in our body, is distinct in each individual and is known to affect the function of the immune system in diseases ranging from autoimmunity to cancer.
Using mouse models of skin and heart transplantation, we investigated if the microbiota was an environmental factor that could affect the speed at which the immune system rejects a transplanted organ.
We found that the microbial communities that colonize the donor and the host fine-tune the function of the immune system and control the strength with which the immune system reacts to a transplanted organ.
 Dr. Joseph Alvarnas[/caption]
Joseph Alvarnas, MD
Associate clinical professor
Department of hematology and Director of value-based analytics
City of Hope National Medical Center
Duarte, CA
MedicalResearch.com: What is the background for this study?
Dr. Alvarnas: Patients with HIV infection have a significantly increased risk of non-Hodgkin lymphoma and Hodgkin lymphoma. Prior to the availability of effective anti-retroviral therapy, HIV-infected patients with lymphoma had very poor treatment outcomes. Following the availability of effective anti-HIV therapy, patient outcomes for HIV-infected patients now parallel those of non-infected patients. Historically, however, HIV infection has been used as a criterion for not offering patients autologous blood stem cell transplantation outside of centers with unique expertise. The purpose of this trial was to evaluate outcomes, complication rates, and immunological reconstitution of HIV-infected patients following autologous blood stem cell transplantation.
Dr. Joseph Alvarnas[/caption]
Joseph Alvarnas, MD
Associate clinical professor
Department of hematology and Director of value-based analytics
City of Hope National Medical Center
Duarte, CA
MedicalResearch.com: What is the background for this study?
Dr. Alvarnas: Patients with HIV infection have a significantly increased risk of non-Hodgkin lymphoma and Hodgkin lymphoma. Prior to the availability of effective anti-retroviral therapy, HIV-infected patients with lymphoma had very poor treatment outcomes. Following the availability of effective anti-HIV therapy, patient outcomes for HIV-infected patients now parallel those of non-infected patients. Historically, however, HIV infection has been used as a criterion for not offering patients autologous blood stem cell transplantation outside of centers with unique expertise. The purpose of this trial was to evaluate outcomes, complication rates, and immunological reconstitution of HIV-infected patients following autologous blood stem cell transplantation.
 Dr. Jaimin Trivedi[/caption]
Jaimin Trivedi, MD, MPH
Instructor
Department of Cardiovascular and Thoracic Surgery
University of Louisville
Louisville, KY 40202
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Trivedi: There is a donor heart shortage in United States and certain donor hearts are likely to be turned down because the donors required cardiopulmonary resuscitation (CPR) prior to procurement. The rationale behind conducting the study was to identify impact of donor CPR and its duration on recipient survival after transplantation.
Our findings show that presence of CPR and duration of CPR does not adversely impact the post heart transplant survival. The study also shows that ejection fraction and peak cardiac troponins between the CPR and non-CPR donors were comparable at time of transplant suggesting recovery of cardiac function.
Dr. Jaimin Trivedi[/caption]
Jaimin Trivedi, MD, MPH
Instructor
Department of Cardiovascular and Thoracic Surgery
University of Louisville
Louisville, KY 40202
MedicalResearch.com: What is the background for this study? What are the main findings?
Dr. Trivedi: There is a donor heart shortage in United States and certain donor hearts are likely to be turned down because the donors required cardiopulmonary resuscitation (CPR) prior to procurement. The rationale behind conducting the study was to identify impact of donor CPR and its duration on recipient survival after transplantation.
Our findings show that presence of CPR and duration of CPR does not adversely impact the post heart transplant survival. The study also shows that ejection fraction and peak cardiac troponins between the CPR and non-CPR donors were comparable at time of transplant suggesting recovery of cardiac function.






 Pritesh Karia[/caption]
MedicalResearch.com Interview with:
Pritesh Karia[/caption]
MedicalResearch.com Interview with: Dr. Sergio Acuna[/caption]
MedicalResearch.com Interview with:
Sergio A. Acuna, MD
Graduate Student at St. Michael's Hospital and IHPME
University of Toronto
Medical Research: What is the background for this study?
Dr. Acuna: Solid organ transplant recipients are known to be at greater risk of developing cancers compared to the general population; however, because they are also at high increased risk of mortality from non-cancer causes, the risk of cancer morality in this population is unclear. As previous studies on this topic have reported disparate findings, the cancer mortality risk in this population remained uncertain.
Medical Research: What are the main findings?
Dr. Acuna: Our study provides conclusive evidence that solid organ transplant recipients are at increased risk of cancer mortality. Our findings demonstrate that solid organ transplant recipients are at increased risk of cancer death compared to the general population regardless of age, transplanted organ, and year of transplantation, and indicate cancer is a substantial cause of death in this population.
Dr. Sergio Acuna[/caption]
MedicalResearch.com Interview with:
Sergio A. Acuna, MD
Graduate Student at St. Michael's Hospital and IHPME
University of Toronto
Medical Research: What is the background for this study?
Dr. Acuna: Solid organ transplant recipients are known to be at greater risk of developing cancers compared to the general population; however, because they are also at high increased risk of mortality from non-cancer causes, the risk of cancer morality in this population is unclear. As previous studies on this topic have reported disparate findings, the cancer mortality risk in this population remained uncertain.
Medical Research: What are the main findings?
Dr. Acuna: Our study provides conclusive evidence that solid organ transplant recipients are at increased risk of cancer mortality. Our findings demonstrate that solid organ transplant recipients are at increased risk of cancer death compared to the general population regardless of age, transplanted organ, and year of transplantation, and indicate cancer is a substantial cause of death in this population.
 Dr. Cassie Kennedy[/caption]
MedicalResearch.com Interview with:
Cassie Kennedy, M.D.
Pulmonology and Critical Care Medicine
Mayo Clinic
Medical Research: What is the background for this study?
Dr. Kennedy: Lung transplant is a surgical procedure that can offer extended life expectancy and improved quality of life to selected patients with end-stage lung disease. However there are about 1700 patients awaiting lung transplant at any given time in the United States because transplant recipients far exceed potential donors. In addition, even with carefully chosen candidates, lung transplant recipients live on average about 5.5 years. It is therefore very important for transplant physicians to choose patients who will receive the most benefit from their lung transplant.
Frailty (defined as an increased vulnerability to adverse health outcomes) has typically been a subjective consideration by transplant physicians when choosing lung transplant candidates. The emergence of more objective and reproducible frailty measures from the geriatric literature present an opportunity to study the prevalence of frailty in lung transplant (despite that subjective screening) and to determine whether the presence of frailty has any impact on patient outcomes.
Medical Research: What are the main findings?
Dr. Kennedy: Frailty is quite common --46 percent of our patient cohort was frail by the Frailty Deficit Index. We also saw a significant association between frailty and worsened survival following lung transplantation: one-year survival rate for frail patients was 71.7 percent, compared to 92.9 percent for patients who were not frail. At three years this difference in survival persisted--the survival rate for frail patients was 41.3 percent, compared to 66.1 percent for patients who were not frail.
Dr. Cassie Kennedy[/caption]
MedicalResearch.com Interview with:
Cassie Kennedy, M.D.
Pulmonology and Critical Care Medicine
Mayo Clinic
Medical Research: What is the background for this study?
Dr. Kennedy: Lung transplant is a surgical procedure that can offer extended life expectancy and improved quality of life to selected patients with end-stage lung disease. However there are about 1700 patients awaiting lung transplant at any given time in the United States because transplant recipients far exceed potential donors. In addition, even with carefully chosen candidates, lung transplant recipients live on average about 5.5 years. It is therefore very important for transplant physicians to choose patients who will receive the most benefit from their lung transplant.
Frailty (defined as an increased vulnerability to adverse health outcomes) has typically been a subjective consideration by transplant physicians when choosing lung transplant candidates. The emergence of more objective and reproducible frailty measures from the geriatric literature present an opportunity to study the prevalence of frailty in lung transplant (despite that subjective screening) and to determine whether the presence of frailty has any impact on patient outcomes.
Medical Research: What are the main findings?
Dr. Kennedy: Frailty is quite common --46 percent of our patient cohort was frail by the Frailty Deficit Index. We also saw a significant association between frailty and worsened survival following lung transplantation: one-year survival rate for frail patients was 71.7 percent, compared to 92.9 percent for patients who were not frail. At three years this difference in survival persisted--the survival rate for frail patients was 41.3 percent, compared to 66.1 percent for patients who were not frail.
 Dr. Vitiello[/caption]
MedicalResearch.com Interview with:
Gerardo Vitiello, MD
Emory University School of Medicine
Emory Transplant Center
NYU Langone Medical Center
Department of Surgery
Medical Research: What is the background for this study? What are the main findings?
Dr. Vitiello: Screening for prostate cancer with prostate specific antigen (PSA) levels is highly controversial, as it is a non-specific marker for prostate cancer. A PSA level may be elevated in a variety of disease processes (not only prostate cancer), and even in the general population, the benefit of early intervention for prostate cancer is unclear. In contrast, end stage renal disease (ESRD), where patients no longer have renal function and require dialysis, is a major health problem with a huge impact on a patient’s quality of life. The only cure for ESRD is kidney transplantation, which has been shown to have an enormous health and quality of life benefit for transplant recipients. Transplant centers have rigorously screened candidates for potential malignancy prior to transplantation to ensure that there are no contraindications to receiving a transplant. For the first time, we demonstrate that screening for prostate cancer in kidney transplant candidates is not beneficial, and may actually be harmful, since it delays time to transplant and reduces a patient’s chance of receiving a transplant without an apparent benefit on patient survival.
Dr. Vitiello[/caption]
MedicalResearch.com Interview with:
Gerardo Vitiello, MD
Emory University School of Medicine
Emory Transplant Center
NYU Langone Medical Center
Department of Surgery
Medical Research: What is the background for this study? What are the main findings?
Dr. Vitiello: Screening for prostate cancer with prostate specific antigen (PSA) levels is highly controversial, as it is a non-specific marker for prostate cancer. A PSA level may be elevated in a variety of disease processes (not only prostate cancer), and even in the general population, the benefit of early intervention for prostate cancer is unclear. In contrast, end stage renal disease (ESRD), where patients no longer have renal function and require dialysis, is a major health problem with a huge impact on a patient’s quality of life. The only cure for ESRD is kidney transplantation, which has been shown to have an enormous health and quality of life benefit for transplant recipients. Transplant centers have rigorously screened candidates for potential malignancy prior to transplantation to ensure that there are no contraindications to receiving a transplant. For the first time, we demonstrate that screening for prostate cancer in kidney transplant candidates is not beneficial, and may actually be harmful, since it delays time to transplant and reduces a patient’s chance of receiving a transplant without an apparent benefit on patient survival.
 Dr. Schlansky[/caption]
MedicalResearch.com Interview with:
Barry Schlansky, M.D., M.P.H
Assistant Professor of Medicine
Oregon Health & Science University
Medical Research: What are the main findings and significance of this study?
Dr. Schlansky: This study examines how obese patients fare before and after liver transplantation. Similar to other researchers, we found that obese patients do just as well as normal weight patients after liver transplantation. We were surprised, however, to find that very obese patients died more often while on the wait list before liver transplant.
Dr. Schlansky[/caption]
MedicalResearch.com Interview with:
Barry Schlansky, M.D., M.P.H
Assistant Professor of Medicine
Oregon Health & Science University
Medical Research: What are the main findings and significance of this study?
Dr. Schlansky: This study examines how obese patients fare before and after liver transplantation. Similar to other researchers, we found that obese patients do just as well as normal weight patients after liver transplantation. We were surprised, however, to find that very obese patients died more often while on the wait list before liver transplant.
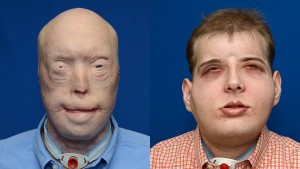 Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to
Patrick Hardison before surgery (left) and in November 2015, nearly three months after the surgery.[/caption]
Mr. Hardison was referred to  Dr. Givens
Dr. Givens




