Author Interviews, COVID -19 Coronavirus, Dermatology / 04.04.2020
Coronavirus Outbreak: Prevention of Device-Related Pressure Ulcers and Injuries
MedicalResearch.com Interview with:
[caption id="attachment_53780" align="alignleft" width="164"] Dr. Gefen[/caption]
Amit Gefen PhD
Professor of Biomedical Engineering
The Herbert J. Berman Chair in Vascular Bioengineering
Department of Biomedical Engineering, Faculty of Engineering
Tel Aviv University, Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: Although we are witnessing continuous progress in medical technologies, the design of many of the most commonly used medical devices e.g. oxygen masks or cervical collars has changed very little over a period of decades. Not surprisingly, these devices are also the ones which are frequently associated with device-related pressure ulcers (DRPUs). These DRPUs are frequently a hospital-acquired injury which involves risk of infections (including e.g. sepsis and antibiotic-resistant bacteria), scarring with serious psychological consequences, additional and significant healthcare costs and a basis for liability suits and litigation. The problem is massive in Europe and the US and is most frequently encountered in clinical environments where devices are used intensively, such as in operation theatres, intensive care units and emergency care settings (in both adult and pediatric medicine), but also, in elderly care facilities where patients often have fragile skin. With the current pandemic spread of the coronavirus, facilities worldwide are experiencing a considerable rise in usage of emergency and intensive care equipment, which will very likely considerably escalate the incidence of DRPUs.
Early in 2019, a committee of global experts which I have chaired, has met for two days of intensive deliberation in London UK, to start developing the first-ever international consensus document on device-related pressure ulcers . After a rigorous review process by an international review committee of other experts, this consensus report has been published as a Special Edition of the Journal of Wound Care in February 2019 (https://doi.org/10.12968/jowc.2020.29.Sup2a.S1), under the name "Device-related pressure ulcers: SECURE prevention". The publisher has kindly made this publication freely downloadable and thereby accessible and available to anyone, including all professionals who may need guidance in this regard, including clinicians, industry, regulators and academic researches.
Dr. Gefen[/caption]
Amit Gefen PhD
Professor of Biomedical Engineering
The Herbert J. Berman Chair in Vascular Bioengineering
Department of Biomedical Engineering, Faculty of Engineering
Tel Aviv University, Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: Although we are witnessing continuous progress in medical technologies, the design of many of the most commonly used medical devices e.g. oxygen masks or cervical collars has changed very little over a period of decades. Not surprisingly, these devices are also the ones which are frequently associated with device-related pressure ulcers (DRPUs). These DRPUs are frequently a hospital-acquired injury which involves risk of infections (including e.g. sepsis and antibiotic-resistant bacteria), scarring with serious psychological consequences, additional and significant healthcare costs and a basis for liability suits and litigation. The problem is massive in Europe and the US and is most frequently encountered in clinical environments where devices are used intensively, such as in operation theatres, intensive care units and emergency care settings (in both adult and pediatric medicine), but also, in elderly care facilities where patients often have fragile skin. With the current pandemic spread of the coronavirus, facilities worldwide are experiencing a considerable rise in usage of emergency and intensive care equipment, which will very likely considerably escalate the incidence of DRPUs.
Early in 2019, a committee of global experts which I have chaired, has met for two days of intensive deliberation in London UK, to start developing the first-ever international consensus document on device-related pressure ulcers . After a rigorous review process by an international review committee of other experts, this consensus report has been published as a Special Edition of the Journal of Wound Care in February 2019 (https://doi.org/10.12968/jowc.2020.29.Sup2a.S1), under the name "Device-related pressure ulcers: SECURE prevention". The publisher has kindly made this publication freely downloadable and thereby accessible and available to anyone, including all professionals who may need guidance in this regard, including clinicians, industry, regulators and academic researches.
 Dr. Gefen[/caption]
Amit Gefen PhD
Professor of Biomedical Engineering
The Herbert J. Berman Chair in Vascular Bioengineering
Department of Biomedical Engineering, Faculty of Engineering
Tel Aviv University, Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: Although we are witnessing continuous progress in medical technologies, the design of many of the most commonly used medical devices e.g. oxygen masks or cervical collars has changed very little over a period of decades. Not surprisingly, these devices are also the ones which are frequently associated with device-related pressure ulcers (DRPUs). These DRPUs are frequently a hospital-acquired injury which involves risk of infections (including e.g. sepsis and antibiotic-resistant bacteria), scarring with serious psychological consequences, additional and significant healthcare costs and a basis for liability suits and litigation. The problem is massive in Europe and the US and is most frequently encountered in clinical environments where devices are used intensively, such as in operation theatres, intensive care units and emergency care settings (in both adult and pediatric medicine), but also, in elderly care facilities where patients often have fragile skin. With the current pandemic spread of the coronavirus, facilities worldwide are experiencing a considerable rise in usage of emergency and intensive care equipment, which will very likely considerably escalate the incidence of DRPUs.
Early in 2019, a committee of global experts which I have chaired, has met for two days of intensive deliberation in London UK, to start developing the first-ever international consensus document on device-related pressure ulcers . After a rigorous review process by an international review committee of other experts, this consensus report has been published as a Special Edition of the Journal of Wound Care in February 2019 (https://doi.org/10.12968/jowc.2020.29.Sup2a.S1), under the name "Device-related pressure ulcers: SECURE prevention". The publisher has kindly made this publication freely downloadable and thereby accessible and available to anyone, including all professionals who may need guidance in this regard, including clinicians, industry, regulators and academic researches.
Dr. Gefen[/caption]
Amit Gefen PhD
Professor of Biomedical Engineering
The Herbert J. Berman Chair in Vascular Bioengineering
Department of Biomedical Engineering, Faculty of Engineering
Tel Aviv University, Tel Aviv, Israel
MedicalResearch.com: What is the background for this study?
Response: Although we are witnessing continuous progress in medical technologies, the design of many of the most commonly used medical devices e.g. oxygen masks or cervical collars has changed very little over a period of decades. Not surprisingly, these devices are also the ones which are frequently associated with device-related pressure ulcers (DRPUs). These DRPUs are frequently a hospital-acquired injury which involves risk of infections (including e.g. sepsis and antibiotic-resistant bacteria), scarring with serious psychological consequences, additional and significant healthcare costs and a basis for liability suits and litigation. The problem is massive in Europe and the US and is most frequently encountered in clinical environments where devices are used intensively, such as in operation theatres, intensive care units and emergency care settings (in both adult and pediatric medicine), but also, in elderly care facilities where patients often have fragile skin. With the current pandemic spread of the coronavirus, facilities worldwide are experiencing a considerable rise in usage of emergency and intensive care equipment, which will very likely considerably escalate the incidence of DRPUs.
Early in 2019, a committee of global experts which I have chaired, has met for two days of intensive deliberation in London UK, to start developing the first-ever international consensus document on device-related pressure ulcers . After a rigorous review process by an international review committee of other experts, this consensus report has been published as a Special Edition of the Journal of Wound Care in February 2019 (https://doi.org/10.12968/jowc.2020.29.Sup2a.S1), under the name "Device-related pressure ulcers: SECURE prevention". The publisher has kindly made this publication freely downloadable and thereby accessible and available to anyone, including all professionals who may need guidance in this regard, including clinicians, industry, regulators and academic researches.
 Aurika Savickaite[/caption]
Aurika Savickaite RN
Adult Gerontology Acute Care Nurse Practitioner
Bulletproof Coach
University of Chicago Medicine
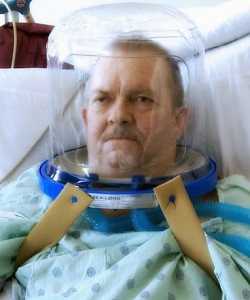
MedicalResearch.com: Would you briefly explain what is meant by helmet-based ventilation? How does it work?
Response: For patients in respiratory failure, noninvasive positive pressure ventilation (NIPPV) is usually delivered through a nasal mask or facemask. Many patients develop pain, discomfort – even claustrophobia -- from using NIPPV systems. The transparent helmet was developed to improve the tolerance of noninvasive ventilation. It allows the patient to see, read, speak and drink without interrupting noninvasive positive-pressure ventilation (NPPV).
The helmet has a sealed connection and a soft collar that adheres to the neck which helps prevent the air leaks that are very common with nasal- or face masks. High positive end-expiratory pressure (PEEP) is vital in treating patients in respiratory failure and thanks to helmets “none to minimum air leak” system, PEEP can be set high (up to 25). NIPPV via a nasal- or full-face mask typically begins to show air leaks when the required pressure exceeds 15-20cm H2O.
Aurika Savickaite[/caption]
Aurika Savickaite RN
Adult Gerontology Acute Care Nurse Practitioner
Bulletproof Coach
University of Chicago Medicine
MedicalResearch.com: Would you briefly explain what is meant by helmet-based ventilation? How does it work?
Response: For patients in respiratory failure, noninvasive positive pressure ventilation (NIPPV) is usually delivered through a nasal mask or facemask. Many patients develop pain, discomfort – even claustrophobia -- from using NIPPV systems. The transparent helmet was developed to improve the tolerance of noninvasive ventilation. It allows the patient to see, read, speak and drink without interrupting noninvasive positive-pressure ventilation (NPPV).
The helmet has a sealed connection and a soft collar that adheres to the neck which helps prevent the air leaks that are very common with nasal- or face masks. High positive end-expiratory pressure (PEEP) is vital in treating patients in respiratory failure and thanks to helmets “none to minimum air leak” system, PEEP can be set high (up to 25). NIPPV via a nasal- or full-face mask typically begins to show air leaks when the required pressure exceeds 15-20cm H2O.




















 Dr. Bin Cao[/caption]
Bin Cao, Yeming Wang, Guohui Fan,
Lianghan Shang, Jiuyang Xu, DingyuZhang, Chen Wang
on behalf of LOTUS-China Study Group
China-Japan Friendship Hospital; Wuhan Jintinyan Hospital;
Institute of Respiratory Medicine, Chinese Academy of Medical Science
MedicalResearch.com: What is the background for this study?
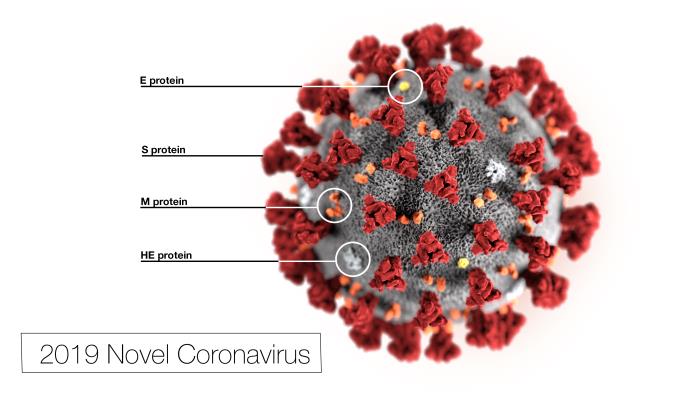
Response: In the past two months, the outbreak of Coronavirus Disease 2019 (COVID-19) has been spreading rapidly across the world. Science and technology is the most powerful weapon for human to fight against diseases, especially in such a pandemic setting. Seeking for effective antiviral medication is the most critical and urgent among the many scientific tasks in the pandemic.
At the most critical moment in the fight against COVID-19, Chinese clinical scientists have stepped forward under extremely difficult research conditions to carry out clinical trials in antiviral treatment including lopinavir–ritonavir and remdesivir, in a swift, decisive and effective manner. These trials have attracted worldwide attention.
Recently, the Lopinavir–ritonavir Trial for suppression of SARS-CoV-2 in China (LOTUS-China) has been completed, which, with great clinical significance, can provide strong evidence for the treatment of COVID-19 both in China and around the world.
Dr. Bin Cao[/caption]
Bin Cao, Yeming Wang, Guohui Fan,
Lianghan Shang, Jiuyang Xu, DingyuZhang, Chen Wang
on behalf of LOTUS-China Study Group
China-Japan Friendship Hospital; Wuhan Jintinyan Hospital;
Institute of Respiratory Medicine, Chinese Academy of Medical Science
MedicalResearch.com: What is the background for this study?
Response: In the past two months, the outbreak of Coronavirus Disease 2019 (COVID-19) has been spreading rapidly across the world. Science and technology is the most powerful weapon for human to fight against diseases, especially in such a pandemic setting. Seeking for effective antiviral medication is the most critical and urgent among the many scientific tasks in the pandemic.
At the most critical moment in the fight against COVID-19, Chinese clinical scientists have stepped forward under extremely difficult research conditions to carry out clinical trials in antiviral treatment including lopinavir–ritonavir and remdesivir, in a swift, decisive and effective manner. These trials have attracted worldwide attention.
Recently, the Lopinavir–ritonavir Trial for suppression of SARS-CoV-2 in China (LOTUS-China) has been completed, which, with great clinical significance, can provide strong evidence for the treatment of COVID-19 both in China and around the world.










 Dr. Jeffrey Smith[/caption]
Jeffrey R. Smith, MD PhD
Department of Medicine, Division of Genetic Medicine
Vanderbilt-Ingram Cancer Center, and Vanderbilt Genetics Institute
Vanderbilt University Medical Center
Medical Research Service
Tennessee Valley Healthcare System, Veterans Administration
Nashville, TN
MedicalResearch.com: What is the background for this study?
Response: Roughly 20% of men with prostate cancer have a family history of the disease, and 5% meet criteria for hereditary prostate cancer. Although prostate cancer has the greatest heritability of all common cancers (twice that of breast cancer), extensive heterogeneity of its inherited causes has presented a considerable obstacle for traditional pedigree-based genetic investigative approaches. Inherited causes across, as well as within families are diverse.
This study introduced a new familial case-control study design that uses extent of family history as a proxy for genetic burden. It compared a large number of men with prostate cancer, each from a separate family with a strong history of the disease, to screened men with no personal or family history. The study comprehensively deconstructs how the 8q24 chromosomal region impacts risk of hereditary prostate cancer, introducing several new analytical approaches. The locus had been known to alter risk of prostate, breast, colon, ovarian, and numerous additional cancers.
Dr. Jeffrey Smith[/caption]
Jeffrey R. Smith, MD PhD
Department of Medicine, Division of Genetic Medicine
Vanderbilt-Ingram Cancer Center, and Vanderbilt Genetics Institute
Vanderbilt University Medical Center
Medical Research Service
Tennessee Valley Healthcare System, Veterans Administration
Nashville, TN
MedicalResearch.com: What is the background for this study?
Response: Roughly 20% of men with prostate cancer have a family history of the disease, and 5% meet criteria for hereditary prostate cancer. Although prostate cancer has the greatest heritability of all common cancers (twice that of breast cancer), extensive heterogeneity of its inherited causes has presented a considerable obstacle for traditional pedigree-based genetic investigative approaches. Inherited causes across, as well as within families are diverse.
This study introduced a new familial case-control study design that uses extent of family history as a proxy for genetic burden. It compared a large number of men with prostate cancer, each from a separate family with a strong history of the disease, to screened men with no personal or family history. The study comprehensively deconstructs how the 8q24 chromosomal region impacts risk of hereditary prostate cancer, introducing several new analytical approaches. The locus had been known to alter risk of prostate, breast, colon, ovarian, and numerous additional cancers.