Author Interviews, Cancer Research, Pharmaceutical Companies / 20.05.2022
Glutamine Antagonist Sirpiglenastat (DRP-104) Has Therapeutic Potential in Targeting Lung Cancer, SCCHN, and Prostate Cancer
MedicalResearch.com Interview with:
[caption id="attachment_59179" align="alignleft" width="150"] Dr. Wild[/caption]
Robert Wild, Ph.D
Chief Scientific Officer
Dracen Pharmaceuticals
MedicalResearch.com: What is the background for the development of sirpiglenastat, i.e., would you briefly explain what is meant by glutamine antagonist?
Response: Cancer cells consume and use glutamine for both energy generation and as a source of carbon and nitrogen for biomass accumulation. Many oncogenes and tumor suppressor genes drive large-scale metabolic reprogramming of tumors into glutamine addiction. These highly proliferating tumors create a hostile and immunosuppressive tumor microenvironment (TME), which is nutrient- depleted, acidic and hypoxic in nature.
Sirpiglenastat (DRP-104), is a novel broad-acting glutamine antagonist that inhibits all 10 known glutamine metabolism enzymes. DRP-104 was designed to preferentially inhibit glutamine metabolism in tumors and associated TME and not in normal tissues, providing a large therapeutic window.
DRP-104 demonstrates powerful direct apoptotic (cell death) properties and immune modulatory mechanisms through broad remodeling of the TME to infer DRP-104 impacts immune-metabolism.
Inhibition of glutamine metabolism leads to:
Dr. Wild[/caption]
Robert Wild, Ph.D
Chief Scientific Officer
Dracen Pharmaceuticals
MedicalResearch.com: What is the background for the development of sirpiglenastat, i.e., would you briefly explain what is meant by glutamine antagonist?
Response: Cancer cells consume and use glutamine for both energy generation and as a source of carbon and nitrogen for biomass accumulation. Many oncogenes and tumor suppressor genes drive large-scale metabolic reprogramming of tumors into glutamine addiction. These highly proliferating tumors create a hostile and immunosuppressive tumor microenvironment (TME), which is nutrient- depleted, acidic and hypoxic in nature.
Sirpiglenastat (DRP-104), is a novel broad-acting glutamine antagonist that inhibits all 10 known glutamine metabolism enzymes. DRP-104 was designed to preferentially inhibit glutamine metabolism in tumors and associated TME and not in normal tissues, providing a large therapeutic window.
DRP-104 demonstrates powerful direct apoptotic (cell death) properties and immune modulatory mechanisms through broad remodeling of the TME to infer DRP-104 impacts immune-metabolism.
Inhibition of glutamine metabolism leads to:
 Dr. Wild[/caption]
Robert Wild, Ph.D
Chief Scientific Officer
Dracen Pharmaceuticals
MedicalResearch.com: What is the background for the development of sirpiglenastat, i.e., would you briefly explain what is meant by glutamine antagonist?
Response: Cancer cells consume and use glutamine for both energy generation and as a source of carbon and nitrogen for biomass accumulation. Many oncogenes and tumor suppressor genes drive large-scale metabolic reprogramming of tumors into glutamine addiction. These highly proliferating tumors create a hostile and immunosuppressive tumor microenvironment (TME), which is nutrient- depleted, acidic and hypoxic in nature.
Sirpiglenastat (DRP-104), is a novel broad-acting glutamine antagonist that inhibits all 10 known glutamine metabolism enzymes. DRP-104 was designed to preferentially inhibit glutamine metabolism in tumors and associated TME and not in normal tissues, providing a large therapeutic window.
DRP-104 demonstrates powerful direct apoptotic (cell death) properties and immune modulatory mechanisms through broad remodeling of the TME to infer DRP-104 impacts immune-metabolism.
Inhibition of glutamine metabolism leads to:
Dr. Wild[/caption]
Robert Wild, Ph.D
Chief Scientific Officer
Dracen Pharmaceuticals
MedicalResearch.com: What is the background for the development of sirpiglenastat, i.e., would you briefly explain what is meant by glutamine antagonist?
Response: Cancer cells consume and use glutamine for both energy generation and as a source of carbon and nitrogen for biomass accumulation. Many oncogenes and tumor suppressor genes drive large-scale metabolic reprogramming of tumors into glutamine addiction. These highly proliferating tumors create a hostile and immunosuppressive tumor microenvironment (TME), which is nutrient- depleted, acidic and hypoxic in nature.
Sirpiglenastat (DRP-104), is a novel broad-acting glutamine antagonist that inhibits all 10 known glutamine metabolism enzymes. DRP-104 was designed to preferentially inhibit glutamine metabolism in tumors and associated TME and not in normal tissues, providing a large therapeutic window.
DRP-104 demonstrates powerful direct apoptotic (cell death) properties and immune modulatory mechanisms through broad remodeling of the TME to infer DRP-104 impacts immune-metabolism.
Inhibition of glutamine metabolism leads to:
- Induction of apoptosis in glutamine-addicted tumor cells leading to substantial single-agent activity and tumor regressions
- Rebalance of the TME that enhances immune cell infiltration and function
- Differentiation and modulation of adaptive and innate immune cells toward a highly proliferative, activated and long-lived phenotype for a long-term durable response.





 Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?





 Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
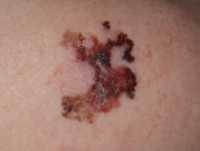
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.
Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.

 Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.
Dr. Sesso[/caption]
Howard D. Sesso, ScD, MPH
Associate Professor of Medicine
Division of Preventive Medicine
Brigham and Women's Hospital
MedicalResearch.com: What is the background for this study? How does the amount of flavanols in the study arm compare to what might be obtained in a typical diet?
Response: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS) is a randomized, double-blind, placebo-controlled clinical trial that tested the effects of two promising dietary supplements on cardiovascular disease (CVD) and cancer in 21,442 older adults. Cocoa flavanols have been shown to have favorable vascular effects in small and short-term clinical trials. The 500 mg/day flavanols tested in COSMOS exceeds that readily obtained in the diet typically from cocoa, tea, grapes, and berries. Of note, flavanol content in not typically listed on food labels.
COSMOS also tested a multivitamin, the most common dietary supplement taken by US adults and previously linked with a potential modest reduction in cancer in a previous long-term trial of men conducted by our research group at the Division of Preventive Medicine at Brigham and Women’s Hospital.
 Dr. Kartal[/caption]
Ece Kartal, PhD
Postdoctoral Fellow
Saez-Rodriguez Group
Universitätsklinikum Heidelberg
Institute for Computational Biomedicine
Heidelberg
MedicalResearch.com: What is the background for this study?
Response: Pancreatic cancer is one of the deadliest types of cancer: although incidence rates are relatively low (only few people develop pancreatic cancer in their lifetimes), it has a high lethality, with a five year survival rate of less than ~5%. Pancreatic cancer symptoms are generally unspecific so that the disease is usually detected very late which further limits therapeutic options. In light of this, earlier detection of pancreatic cancer could dramatically improve prognosis, but there are currently no affordable and non-invasive tests available in the clinic.
For pancreatic ductal adenocarcinoma (PDAC),the most common form of pancreatic cancer, it was previously found that the oral, gut and pancreatic microbiome are risk factors and may affect prognosis .
Dr. Kartal[/caption]
Ece Kartal, PhD
Postdoctoral Fellow
Saez-Rodriguez Group
Universitätsklinikum Heidelberg
Institute for Computational Biomedicine
Heidelberg
MedicalResearch.com: What is the background for this study?
Response: Pancreatic cancer is one of the deadliest types of cancer: although incidence rates are relatively low (only few people develop pancreatic cancer in their lifetimes), it has a high lethality, with a five year survival rate of less than ~5%. Pancreatic cancer symptoms are generally unspecific so that the disease is usually detected very late which further limits therapeutic options. In light of this, earlier detection of pancreatic cancer could dramatically improve prognosis, but there are currently no affordable and non-invasive tests available in the clinic.
For pancreatic ductal adenocarcinoma (PDAC),the most common form of pancreatic cancer, it was previously found that the oral, gut and pancreatic microbiome are risk factors and may affect prognosis .

 Dr. Singh[/caption]
Dr. Saundra Singh M.D., Ph.D.
Founder & CEO/President
Dr. Singh[/caption]
Dr. Saundra Singh M.D., Ph.D.
Founder & CEO/President
 MedicalResearch.com: What is the mission of
MedicalResearch.com: What is the mission of 
 Dr. Deshmukh[/caption]
Ashish A. Deshmukh, PhD, MPH
Associate Professor, Management, Policy & Community Health
Associate Director, Center for Health Services Research
Co-director, Clinical Analytics and Decision Science Lab
UTHealth School of Public Health
Houston, TX 77030
MedicalResearch.com: What is the background for this study?
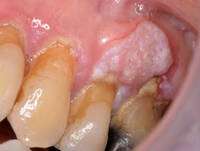
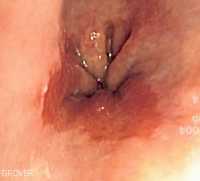
Response: Oropharyngeal cancer is the most common cancer caused by human papillomavirus (HPV) in the United States (US). We know from previous studies that oropharyngeal cancer to be one of the fastest rising cancers in the US. However, trends (i.e., extent of change) in incidence rates among men and women in all 50 US states and trends according to tumor diagnostic characteristics (i.e., stage, size) have not been comprehensively studied. In addition, no prior study evaluated contemporary trends in oropharyngeal cancer mortality (death) rates in the US. Our study provides a comprehensive picture of oropharyngeal cancer incidence and mortality (according to age, stage, tumor size, and state of residence) in all 50 states and DC.
Dr. Deshmukh[/caption]
Ashish A. Deshmukh, PhD, MPH
Associate Professor, Management, Policy & Community Health
Associate Director, Center for Health Services Research
Co-director, Clinical Analytics and Decision Science Lab
UTHealth School of Public Health
Houston, TX 77030
MedicalResearch.com: What is the background for this study?
Response: Oropharyngeal cancer is the most common cancer caused by human papillomavirus (HPV) in the United States (US). We know from previous studies that oropharyngeal cancer to be one of the fastest rising cancers in the US. However, trends (i.e., extent of change) in incidence rates among men and women in all 50 US states and trends according to tumor diagnostic characteristics (i.e., stage, size) have not been comprehensively studied. In addition, no prior study evaluated contemporary trends in oropharyngeal cancer mortality (death) rates in the US. Our study provides a comprehensive picture of oropharyngeal cancer incidence and mortality (according to age, stage, tumor size, and state of residence) in all 50 states and DC.











 Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"]
Dr. Correa[/caption]
Andres F. Correa, MD
Assistant Professor
Department of Surgical Oncology, and
[caption id="attachment_57815" align="alignleft" width="150"] Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
Dr. Bernstein[/caption]
Adrien Bernstein, MD
Second Year Urologic Oncology Fellow
Fox Chase Cancer Center
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, it has been well-established that historically Black Americans experience increased cancer specific mortality compared to white patients. In prostate cancer specifically studies have shown that when access to care is equitable this gap resolves. This suggests that biological factors are not driving these differences but rather the result of the complex interplay of social determinants and systemic inequities in our healthcare system.
Early in the pandemic, multiple studies demonstrated that minority communities disproportionately shouldered poor COVID-19 outcomes. On March 13th 2020, the American College of Surgeons recommended against elective procedures; however, the definition of an elective oncologic case was left to the discretion of the provider. As prostate cancer treatment can be safely deferred up to a year follow diagnosis, management of prostate cancer during the initial lockdown period of the COVID-19 Pandemic provided a useful analysis of the differential restrictions placed on non-emergent health care during the Pandemic.
 MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.
MedicalResearch.com Interview with:
Eleonora Leucci, Ph.D Assistant Professor
Laboratory for RNA Cancer Biology
Department of Oncology
KU Leuven
MedicalResearch.com: What is the background for this study?
Response: Back in 2016, while I was characterising the RNA SAMMSON as essential for mitochondrial translation in melanoma, I noticed that its inhibition was causing cell death across a large spectrum of melanoma cell lines and models, irrespectively of their genetic background and cell state. At that time I still did not know why the effect was so pronounced on melanoma cells, but I knew that antibiotics of the tetracycline family could also block mitochondrial translation and I thought about repurposing them to treat melanoma.