Author Interviews, Cancer Research, HPV / 20.11.2019
Anal Cancer Rates Rise Sharply
MedicalResearch.com Interview with:
[caption id="attachment_52225" align="alignleft" width="133"] Dr. Deshmukh[/caption]
Ashish Deshmukh, PhD, MPH
Assistant Professor
UTHealth School of Public Health
Houston
MedicalResearch.com: What is the background for this study?
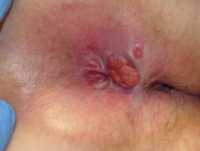
Response: Anal cancer is one of the six human papillomavirus associated cancers. Rates of anal cancer are increasing in the US, but no prior study quantified the contemporary trends (i.e., increase in rates over time) in anal cancer incidence. It was unknown whether the rise is real or driven by increased screening in some high-risk populations. Incidence trends according to age and stage at diagnosis was also never comprehensively studied. Furthermore, it was unknown whether the rise in incidence has led to a rise in mortality. Our objective was to answer these questions.
Dr. Deshmukh[/caption]
Ashish Deshmukh, PhD, MPH
Assistant Professor
UTHealth School of Public Health
Houston
MedicalResearch.com: What is the background for this study?
Response: Anal cancer is one of the six human papillomavirus associated cancers. Rates of anal cancer are increasing in the US, but no prior study quantified the contemporary trends (i.e., increase in rates over time) in anal cancer incidence. It was unknown whether the rise is real or driven by increased screening in some high-risk populations. Incidence trends according to age and stage at diagnosis was also never comprehensively studied. Furthermore, it was unknown whether the rise in incidence has led to a rise in mortality. Our objective was to answer these questions.
 Dr. Deshmukh[/caption]
Ashish Deshmukh, PhD, MPH
Assistant Professor
UTHealth School of Public Health
Houston
MedicalResearch.com: What is the background for this study?
Response: Anal cancer is one of the six human papillomavirus associated cancers. Rates of anal cancer are increasing in the US, but no prior study quantified the contemporary trends (i.e., increase in rates over time) in anal cancer incidence. It was unknown whether the rise is real or driven by increased screening in some high-risk populations. Incidence trends according to age and stage at diagnosis was also never comprehensively studied. Furthermore, it was unknown whether the rise in incidence has led to a rise in mortality. Our objective was to answer these questions.
Dr. Deshmukh[/caption]
Ashish Deshmukh, PhD, MPH
Assistant Professor
UTHealth School of Public Health
Houston
MedicalResearch.com: What is the background for this study?
Response: Anal cancer is one of the six human papillomavirus associated cancers. Rates of anal cancer are increasing in the US, but no prior study quantified the contemporary trends (i.e., increase in rates over time) in anal cancer incidence. It was unknown whether the rise is real or driven by increased screening in some high-risk populations. Incidence trends according to age and stage at diagnosis was also never comprehensively studied. Furthermore, it was unknown whether the rise in incidence has led to a rise in mortality. Our objective was to answer these questions.










 Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
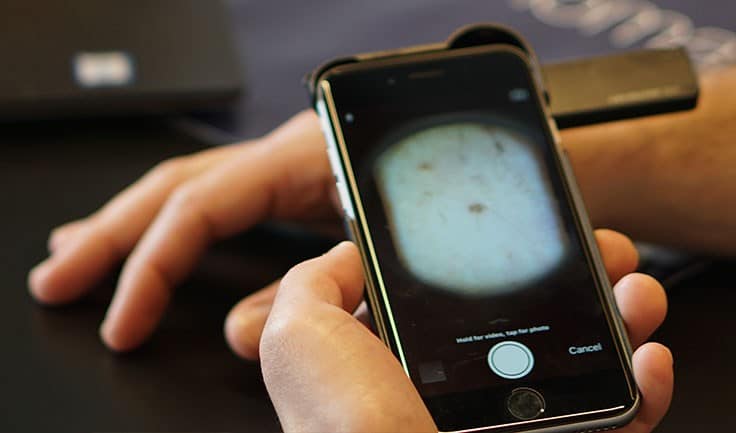
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
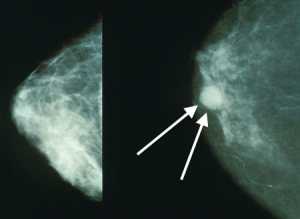
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
Dr. Helen Marsden PhD
Skin Analytics Limited
London, United Kingdom
MedicalResearch.com: What is the background for this study?
Response: In this technology age, with the explosion of interest and applications using Artificial Intelligence, it is easy to accept the output of a technology-based test - such as a smartphone app designed to identify skin cancer - without thinking too much about it. In reality, technology is only as good as the way it has been developed, tested and validated. In particular, AI algorithms are prone to a lack of “generalisation” - i.e. their performance drops when presented with data it has not seen before. In the medical field, and particularly in areas where AI is being developed to direct a patient’s diagnosis or care, this is particularly problematic. Inappropriate diagnosis or advice to patients can lead to false reassurance, heightened concern and pressure on NHS services, or worse. It is concerning, therefore, that there are a large number of smartphone apps available that provide an assessment of skin lesions, including some that provide an estimate of the probability of malignancy, that have not been assessed for diagnostic accuracy.
Skin Analytics has developed an AI-based algorithm, named: Deep Ensemble for Recognition of Malignancy (DERM), for use as a decision support tool for healthcare providers. DERM determines the likelihood of skin cancer from dermoscopic images of skin lesions. It was developed using deep learning techniques that identify and assess features of these lesions which are associated with melanoma, using over 7,000 archived dermoscopic images. Using these images, it was shown to identify melanoma with similar accuracy to specialist physicians. However, to prove the algorithm could be used in a real life clinical setting, Skin Analytics set out to conduct a clinical validation study.
 Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.
Dr. Qing Chen[/caption]
Qing Chen, M.D., Ph.D.
Assistant Professor, Immunology, Microenvironment & Metastasis Program
Scientific Director, Imaging Facility
The Wistar Institute
MedicalResearch.com: What is the background for this study?
Response: We are focusing on how a specific type of brain cells, astrocytes, helps the cancer cells from melanoma and breast cancer to form metastatic lesions.
















