Author Interviews, Herpes Viruses, JAMA, STD, USPSTF / 23.02.2023
USPSTF Statement on Screening For Genital Herpes
MedicalResearch.com Interview with:
[caption id="attachment_59720" align="alignleft" width="133"] Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.
Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.
 Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.
Dr. Stevermer[/caption]
James Stevermer, M.D., M.S.P.H.
Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: Genital herpes is a common sexually transmitted infection (STI) that unfortunately has no cure and cannot accurately be detected in people who do not have signs of the condition. The current screening tests have limitations and there is a high chance that test results will say a person has the condition when they do not. In addition, the available treatments are focused on managing symptoms and preventing the condition from reoccurring. As a result, the Task Force concluded that the harms of screening outweigh the benefits.



 Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.
Kenya Colvin[/caption]
Kenya Colvin, MBS
Department of Medical Education
Scranton, PA
MedicalResearch.com: What is the background for this study?
Response: Vaccine hesitancy is a major driver of COVID-19 vaccination disparities between minority and non-Hispanic White communities. Our goal was to understand what factors influenced vaccine hesitancy among individuals in Eastern Pennsylvania to identify more effective ways to promote vaccine uptake within minority communities.


 Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD
Dr. García Cenoz[/caption]
Manuel García Cenoz MD, PhD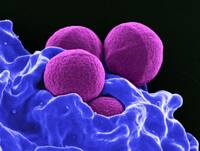

 Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
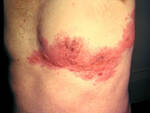
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.
Dr. Curhan[/caption]
Sharon G. Curhan, MD, ScM|
Director, CHEARS: The Conservation of Hearing Study
Channing Division of Network Medicine
Department of Medicine
Brigham and Women’s Hospital
Harvard Medical School
Boston, MA 02114
MedicalResearch.com: What is the background for this study?
Response: Herpes zoster, commonly known as “shingles,” is a viral infection that often causes a painful rash. Shingles can occur anywhere on the head or body. Shingles is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. After a person has chickenpox, the virus stays in their body for the rest of their life. Years and even decades later, the virus may reactivate as shingles. Almost all individuals age 50 years and older in the US have been infected with the varicella zoster virus and therefore they are at risk for shingles.
About 1 in 3 people will develop shingles during their lifetime, and since age is a risk factor for shingles, this number may increase as the population ages. The risk is also higher among individuals of any age who are immunocompromised due to disease or treatment. A number of serious complications can occur when a person develops shingles, such as post-herpetic neuralgia (long-lasting pain), but there was limited information on whether there are other adverse long-term health implications of developing shingles.
There is a growing body of evidence that links VZV, the virus that causes shingles, to vascular disease. VZV vasculopathy may cause damage to blood vessels and increase the risk of stroke or coronary heart disease. Although some previous studies showed a higher risk of stroke or heart attack around the time of the shingles infection, it was not known whether this higher risk persisted in the long term. Therefore, the question we aimed to address in this study was to investigate whether shingles is associated with higher long-term risk of stroke or coronary heart disease.
To address this question, we conducted a prospective longitudinal study in 3 large US cohorts of >200,000 women and men, the Nurses’ Health Study (>79,000 women), the Nurses’ Health Study II (almost 94,000 women) and the Health Professionals Follow-Up Study (>31,000 men), without a prior history of stroke or coronary heart disease. We collected information on shingles, stroke and coronary heart disease on biennial questionnaires and confirmed the diagnoses with medical record review. We followed the participants for up to 16 years and evaluated whether those who had developed shingles were at higher risk for stroke or coronary heart disease years after the shingles episode. The outcomes we measured were incident stroke, incident coronary heart disease [defined as having a non-fatal or fatal myocardial infarction (heart attack) or a coronary revascularization procedure (CABG, coronary artery bypass graft or percutaneous transluminal coronary angioplasty)]. We also evaluated a combined outcome of cardiovascular disease, which included either stroke or coronary heart disease, whichever came first.



 Sean M Hughes MA
Department of Obstetrics and Gynecology
University of Washington
Seattle, WA
MedicalResearch.com: What is the background for this study?
Response: Young women are at elevated risk of getting sexually transmitted infections at the age when they typically start to have sexual intercourse. It’s not known whether this elevated risk is a consequence of behavioral factors (such as choices around use of barrier protection), physiological factors (such as a difference in the immune system) or a combination of both. In this study, we investigated a physiological factor: the immune system in the vagina.
Sean M Hughes MA
Department of Obstetrics and Gynecology
University of Washington
Seattle, WA
MedicalResearch.com: What is the background for this study?
Response: Young women are at elevated risk of getting sexually transmitted infections at the age when they typically start to have sexual intercourse. It’s not known whether this elevated risk is a consequence of behavioral factors (such as choices around use of barrier protection), physiological factors (such as a difference in the immune system) or a combination of both. In this study, we investigated a physiological factor: the immune system in the vagina.

 Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
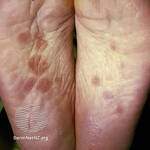
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.
Dr. Ogedegbe[/caption]
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study?
Response: Syphilis has become more common over the past 20 years, after reaching a record low in 2000. The Task Force found that screening people who are at increased risk for syphilis can identify the infection early so it can be treated before problems develop. For that reason, the Task Force recommends screening people who are at increased risk for syphilis infection.


 Dr. Wall[/caption]
Dr Emma Wall
Senior Clinical Research Fellow, UCLH-Crick Legacy study
Consultant Infectious Diseases UCLH
MedicalResearch.com: What is the background for this study?
Response: Since April 2022, both the UK and US have changed their COVID-19 isolation and testing policies. The impact these changes in the guidance and vaccination on community-acquired COVID-19 caused by recent SARS-CoV-2 variants of concern (VOC) has not been fully tested, including infections with BA.2. We aimed to characterise both symptoms and viral loads over the course of COVID-19 infection in otherwise-healthy, vaccinated, non-hospitalised adults, to assess whether current guidance remains justified. All participants were included in the UCLH-Crick Legacy study, a prospective, observational cohort study of otherwise healthy adults who have been taking part in regular workplace testing for SARS-CoV-2 in London
We sent swabs by same-day courier every other day to all adults who reported a positive PCR or lateral flow test to the study team up to day 10 after the start of each infection. We confirmed which variant caused the infection by PCR and sequencing. All participants completed linked symptom diaries.
We compared symptoms and changes in the amount of virus detected in the nose and throat during infection between study participants reporting COVID-19 caused by VOCs Delta and Omicron BA.1 and BA.2. We then analysed how many of our participants would meet current UK/US isolation guidelines.
Dr. Wall[/caption]
Dr Emma Wall
Senior Clinical Research Fellow, UCLH-Crick Legacy study
Consultant Infectious Diseases UCLH
MedicalResearch.com: What is the background for this study?
Response: Since April 2022, both the UK and US have changed their COVID-19 isolation and testing policies. The impact these changes in the guidance and vaccination on community-acquired COVID-19 caused by recent SARS-CoV-2 variants of concern (VOC) has not been fully tested, including infections with BA.2. We aimed to characterise both symptoms and viral loads over the course of COVID-19 infection in otherwise-healthy, vaccinated, non-hospitalised adults, to assess whether current guidance remains justified. All participants were included in the UCLH-Crick Legacy study, a prospective, observational cohort study of otherwise healthy adults who have been taking part in regular workplace testing for SARS-CoV-2 in London
We sent swabs by same-day courier every other day to all adults who reported a positive PCR or lateral flow test to the study team up to day 10 after the start of each infection. We confirmed which variant caused the infection by PCR and sequencing. All participants completed linked symptom diaries.
We compared symptoms and changes in the amount of virus detected in the nose and throat during infection between study participants reporting COVID-19 caused by VOCs Delta and Omicron BA.1 and BA.2. We then analysed how many of our participants would meet current UK/US isolation guidelines.

 Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .
Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .
 Dr. Dryden-Peterson[/caption]
SCOTT DRYDEN-PETERSON, MD
Assistant Professor, Medicine, Harvard Medical School
Research Affiliate, Immunology and Infectious Diseases
Harvard T.H. Chan School Of Public Health
Associate Physician, Medicine, Infectious Diseases
Brigham And Women's Hospital
Research Associate, Botswana Harvard AIDS Institute
MedicalResearch.com: What is the background for this study?
Response: The combination of the antiviral medicine nirmatrelvir and ritonavir (Paxlovid) which boosts antiviral levels was found to reduce the need for hospitalization by nearly 90% among unvaccinated people. Whether nirmatrelvir plus ritonavir can also help vaccinated people was uncertain.
Dr. Dryden-Peterson[/caption]
SCOTT DRYDEN-PETERSON, MD
Assistant Professor, Medicine, Harvard Medical School
Research Affiliate, Immunology and Infectious Diseases
Harvard T.H. Chan School Of Public Health
Associate Physician, Medicine, Infectious Diseases
Brigham And Women's Hospital
Research Associate, Botswana Harvard AIDS Institute
MedicalResearch.com: What is the background for this study?
Response: The combination of the antiviral medicine nirmatrelvir and ritonavir (Paxlovid) which boosts antiviral levels was found to reduce the need for hospitalization by nearly 90% among unvaccinated people. Whether nirmatrelvir plus ritonavir can also help vaccinated people was uncertain.




 Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000.
Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000. 
 Dr. Otter[/caption]
Ashley Otter, PhD
Research scientist within Diagnostic Support
for the rare/imported pathogens laboratory (RIPL)
Public Health England (PHE)
MedicalResearch.com: What is the background for this study?
Response: The SIREN study is a national research project covering all four nations of the United Kingdom. Almost 45,000 healthcare workers from across the UK were enrolled midway through 2020, each providing monthly samples for antibody testing and fortnightly PCR testing. Using samples from participants from this project, we were able to take a snapshot of ~6,000 participants at different stages after they received their vaccination to see how different factors affect their antibody responses.
Dr. Otter[/caption]
Ashley Otter, PhD
Research scientist within Diagnostic Support
for the rare/imported pathogens laboratory (RIPL)
Public Health England (PHE)
MedicalResearch.com: What is the background for this study?
Response: The SIREN study is a national research project covering all four nations of the United Kingdom. Almost 45,000 healthcare workers from across the UK were enrolled midway through 2020, each providing monthly samples for antibody testing and fortnightly PCR testing. Using samples from participants from this project, we were able to take a snapshot of ~6,000 participants at different stages after they received their vaccination to see how different factors affect their antibody responses.
 Dr. Cheng-Ying Ho[/caption]
Cheng-Ying Ho, MD, PhD
Associate Professor
Department of Pathology
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Smell loss is one of the most common symptoms of COVID-19 infection. The mechanism of COVID-19-related smell loss is unclear. Previous studies mainly focused on the effect of the viral infection on the lining of the nasal cavity. We went a step beyond to examine the olfactory bulb, a region that transmits smell-related signals to the brain.
Dr. Cheng-Ying Ho[/caption]
Cheng-Ying Ho, MD, PhD
Associate Professor
Department of Pathology
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Smell loss is one of the most common symptoms of COVID-19 infection. The mechanism of COVID-19-related smell loss is unclear. Previous studies mainly focused on the effect of the viral infection on the lining of the nasal cavity. We went a step beyond to examine the olfactory bulb, a region that transmits smell-related signals to the brain.