Author Interviews, COVID -19 Coronavirus, Nature, Neurological Disorders / 07.04.2022
COVID-19: Neurological Complications May Be First and Only Complication
MedicalResearch.com Interview with:
[caption id="attachment_58991" align="alignleft" width="150"] Dr. Fischer[/caption]
Tracy Fischer, PhD
Associate Professor of Microbiology and Immunology
Tulane National Primate Research Center
MedicalResearch.com: What is the background for this study?
Response: We investigated multiple regions of the brain from SARS-CoV-2 infected Rhesus macaques and African green monkeys for the presence of inflammation and other pathology that may result from COVID-19. Most animals were infected for approximately one month before our investigation, however, two of the African green monkeys developed acute respiratory distress syndrome (ARDS) prior to the study endpoint.
Dr. Fischer[/caption]
Tracy Fischer, PhD
Associate Professor of Microbiology and Immunology
Tulane National Primate Research Center
MedicalResearch.com: What is the background for this study?
Response: We investigated multiple regions of the brain from SARS-CoV-2 infected Rhesus macaques and African green monkeys for the presence of inflammation and other pathology that may result from COVID-19. Most animals were infected for approximately one month before our investigation, however, two of the African green monkeys developed acute respiratory distress syndrome (ARDS) prior to the study endpoint.
 Dr. Fischer[/caption]
Tracy Fischer, PhD
Associate Professor of Microbiology and Immunology
Tulane National Primate Research Center
MedicalResearch.com: What is the background for this study?
Response: We investigated multiple regions of the brain from SARS-CoV-2 infected Rhesus macaques and African green monkeys for the presence of inflammation and other pathology that may result from COVID-19. Most animals were infected for approximately one month before our investigation, however, two of the African green monkeys developed acute respiratory distress syndrome (ARDS) prior to the study endpoint.
Dr. Fischer[/caption]
Tracy Fischer, PhD
Associate Professor of Microbiology and Immunology
Tulane National Primate Research Center
MedicalResearch.com: What is the background for this study?
Response: We investigated multiple regions of the brain from SARS-CoV-2 infected Rhesus macaques and African green monkeys for the presence of inflammation and other pathology that may result from COVID-19. Most animals were infected for approximately one month before our investigation, however, two of the African green monkeys developed acute respiratory distress syndrome (ARDS) prior to the study endpoint.



 Dr. Rathmann[/caption]
Prof. Wolfgang Rathmann MSPH
Prof. of Epidemiology
Deputy Director, Institute for Biometrics and Epidemiology,
German Diabetes Center, Heinrich Heine University
Düsseldorf, Germany
MedicalResearch.com: What is the background for this study?
Response: Diabetes is associated with a poor prognosis of COVID-19. There have been raised concerns about a bidirectional relationship between diabetes and COVID-19. Recent studies raised the possibility that SARS-CoV-2 can cause diabetes. However, there is a lack of studies investigating the incidence of diabetes after recovery from COVID-19 in mild cases.
To provide more evidence, we analyzed electronic health records from 1,171 general and internal medicine practices across Germany between March 2020 and January 2021. This included 35,865 patients who were diagnosed with COVID-19. The incidence of diabetes after COVID-19 was compared with patients, who were diagnosed with an acute upper respiratory tract infection (AURI), matched for sex, age, and comorbidities including obesity, high blood pressure, high cholesterol, heart attack, and stroke.
Dr. Rathmann[/caption]
Prof. Wolfgang Rathmann MSPH
Prof. of Epidemiology
Deputy Director, Institute for Biometrics and Epidemiology,
German Diabetes Center, Heinrich Heine University
Düsseldorf, Germany
MedicalResearch.com: What is the background for this study?
Response: Diabetes is associated with a poor prognosis of COVID-19. There have been raised concerns about a bidirectional relationship between diabetes and COVID-19. Recent studies raised the possibility that SARS-CoV-2 can cause diabetes. However, there is a lack of studies investigating the incidence of diabetes after recovery from COVID-19 in mild cases.
To provide more evidence, we analyzed electronic health records from 1,171 general and internal medicine practices across Germany between March 2020 and January 2021. This included 35,865 patients who were diagnosed with COVID-19. The incidence of diabetes after COVID-19 was compared with patients, who were diagnosed with an acute upper respiratory tract infection (AURI), matched for sex, age, and comorbidities including obesity, high blood pressure, high cholesterol, heart attack, and stroke.


 Johonniuss Chemweno
CEO of VIPStarNetwork
MedicalResearch.com: What is the mission of VIP StarNetwork?
Response: VIP StarNetwork’s mission is to expand access to healthcare services and information, especially in underserved and underprivileged communities. Our comprehensive group of health experts, leading physicians, and healthcare executives are working to create a meaningful and safe environment to ensure that patients have equitable and streamlined access to vaccines and other forms of care.
Johonniuss Chemweno
CEO of VIPStarNetwork
MedicalResearch.com: What is the mission of VIP StarNetwork?
Response: VIP StarNetwork’s mission is to expand access to healthcare services and information, especially in underserved and underprivileged communities. Our comprehensive group of health experts, leading physicians, and healthcare executives are working to create a meaningful and safe environment to ensure that patients have equitable and streamlined access to vaccines and other forms of care.

 Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.
Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.








 Dr. Pollitt[/caption]
Krystal Pollitt, PhD, P.Eng.
Assistant Professor of Epidemiology (Environmental Health Sciences)
Assistant Professor in Chemical and Environmental Engineering
Affiliated Faculty, Yale Institute for Global Health
Yale School of Public Health
MedicalResearch.com: What is the background for this study?
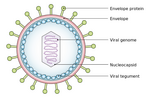
Response: People infected with COVID-19 can release SARS-CoV-2 virus in aerosol and droplets when they exhale. This can be from coughing or sneezing but also when they speaker or just breathe. While the larger droplets can settle to the ground quickly (seconds to minutes), smaller aerosol can remain in the air in longer periods (minutes to hours). SARS-CoV-2 can be transmitted by inhaling aerosol or droplets containing infectious virus. The Fresh Air Clip enables detection of droplet and aerosol containing virus.
Dr. Pollitt[/caption]
Krystal Pollitt, PhD, P.Eng.
Assistant Professor of Epidemiology (Environmental Health Sciences)
Assistant Professor in Chemical and Environmental Engineering
Affiliated Faculty, Yale Institute for Global Health
Yale School of Public Health
MedicalResearch.com: What is the background for this study?
Response: People infected with COVID-19 can release SARS-CoV-2 virus in aerosol and droplets when they exhale. This can be from coughing or sneezing but also when they speaker or just breathe. While the larger droplets can settle to the ground quickly (seconds to minutes), smaller aerosol can remain in the air in longer periods (minutes to hours). SARS-CoV-2 can be transmitted by inhaling aerosol or droplets containing infectious virus. The Fresh Air Clip enables detection of droplet and aerosol containing virus.


 Dr. Deshmukh[/caption]
Ashish A. Deshmukh, PhD, MPH
Associate Professor, Management, Policy & Community Health
Associate Director, Center for Health Services Research
Co-director, Clinical Analytics and Decision Science Lab
UTHealth School of Public Health
Houston, TX 77030
MedicalResearch.com: What is the background for this study?
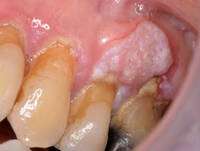
Response: Oropharyngeal cancer is the most common cancer caused by human papillomavirus (HPV) in the United States (US). We know from previous studies that oropharyngeal cancer to be one of the fastest rising cancers in the US. However, trends (i.e., extent of change) in incidence rates among men and women in all 50 US states and trends according to tumor diagnostic characteristics (i.e., stage, size) have not been comprehensively studied. In addition, no prior study evaluated contemporary trends in oropharyngeal cancer mortality (death) rates in the US. Our study provides a comprehensive picture of oropharyngeal cancer incidence and mortality (according to age, stage, tumor size, and state of residence) in all 50 states and DC.
Dr. Deshmukh[/caption]
Ashish A. Deshmukh, PhD, MPH
Associate Professor, Management, Policy & Community Health
Associate Director, Center for Health Services Research
Co-director, Clinical Analytics and Decision Science Lab
UTHealth School of Public Health
Houston, TX 77030
MedicalResearch.com: What is the background for this study?
Response: Oropharyngeal cancer is the most common cancer caused by human papillomavirus (HPV) in the United States (US). We know from previous studies that oropharyngeal cancer to be one of the fastest rising cancers in the US. However, trends (i.e., extent of change) in incidence rates among men and women in all 50 US states and trends according to tumor diagnostic characteristics (i.e., stage, size) have not been comprehensively studied. In addition, no prior study evaluated contemporary trends in oropharyngeal cancer mortality (death) rates in the US. Our study provides a comprehensive picture of oropharyngeal cancer incidence and mortality (according to age, stage, tumor size, and state of residence) in all 50 states and DC.

 Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.
Shuchi Anand, MD MS (she/her)
Assistant Professor in Medicine
Director, Center for Tubulointerstitial Kidney Disease
Stanford University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A majority of people on dialysis who completed vaccination as of September 2021 have had a decline in antibody response to levels that would render them vulnerable to infection. Antibody response immediately after vaccination and circulating antibody response is strongly associated with risk for breakthrough after the initial vaccination series.




 Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
Dr. Dickerman[/caption]
Dr. Barbra Dickerman, PhD
CAUSALab investigator and instructor
Department of Epidemiology
Harvard T.H. Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Early randomized trials showed that the BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna) vaccines were both remarkably effective at preventing symptomatic disease, when comparing each vaccine with no vaccine. However, head-to-head comparisons of these vaccines have been lacking, leaving open the question of which vaccine is more effective.
In this study, we analyzed the VA’s high-quality databases in a way that emulated the design of the hypothetical trial that would have answered this question. Specifically, we used the findings from the original trials to benchmark our methods and then extended them to provide novel evidence for the comparative effectiveness of these two vaccines in a real-world setting and across diverse subgroups and different time periods.
 Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.
Dr. Woodruff[/caption]
Carina M. Woodruff, MD
Department of Dermatolog
University of California, San Francisco
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rigorous hand hygiene has been an important component of the CDC's COVID-19 guidelines. With millions of Americans now using hand sanitizers regularly, we are seeing many more cases of hand dermatitis. Our study evaluated the key product features and most common allergens in the top-reviewed, commercial hand sanitizers sold by major US retailers.
We found that the most common potential allergens were tocopherol, fragrance, propylene glycol and phenoxyethanol. Our study also showed that nearly 1 in 5 marketing claims on these products was misleading. For example, 70% of sanitizers with the marketing claim "hypoallergenic" included at least one common allergen in its formulation.