Author Interviews, Brigham & Women's - Harvard, Infections, JAMA, Multiple Sclerosis, Neurological Disorders / 19.03.2024
MS: Harvard Chan Study Further Identified Serologic Response to Epstein-Barr Virus
MedicalResearch.com Interview with:
[caption id="attachment_61454" align="alignleft" width="125"] Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research ScientistDepartment of Nutrition
Harvard T.H. Chan School of Public HealthBoston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: In a study published in Science in 2022, we reported compelling evidence that infection with the Epstein-Barr virus is the leading cause of Multiple Sclerosis. This is a follow-up study to investigate more in depth whether the antibody response to EBV is distinct in individuals with MS compared to individuals without MS and whether there is a part of EBV that the immune response is particularly targeting. For this purpose we assessed the immune response to all protein parts (peptides) of EBV and their association with MS.
Previous studies could only look at parts of EBV and this is the first study looking at all EBV peptides. Antibodies to EBV (especially to a protein called EBNA1) are known to be overall higher in individuals with MS, so we also tested whether immune response overall or the immune response to specific EBV protein parts was more important. If the immune response to a specific EBV protein part (peptide) would be standing out or distinguishing individuals with MS, we hypothesized, it could point to a specific mechanism of how EBV may cause MS, i.e. it could point for example towards “molecular mimicry”, which is when antibodies targeting a pathogen start targeting a body-own structure (for example in the brain) which resembles the protein parts of the pathogen.
Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research ScientistDepartment of Nutrition
Harvard T.H. Chan School of Public HealthBoston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: In a study published in Science in 2022, we reported compelling evidence that infection with the Epstein-Barr virus is the leading cause of Multiple Sclerosis. This is a follow-up study to investigate more in depth whether the antibody response to EBV is distinct in individuals with MS compared to individuals without MS and whether there is a part of EBV that the immune response is particularly targeting. For this purpose we assessed the immune response to all protein parts (peptides) of EBV and their association with MS.
Previous studies could only look at parts of EBV and this is the first study looking at all EBV peptides. Antibodies to EBV (especially to a protein called EBNA1) are known to be overall higher in individuals with MS, so we also tested whether immune response overall or the immune response to specific EBV protein parts was more important. If the immune response to a specific EBV protein part (peptide) would be standing out or distinguishing individuals with MS, we hypothesized, it could point to a specific mechanism of how EBV may cause MS, i.e. it could point for example towards “molecular mimicry”, which is when antibodies targeting a pathogen start targeting a body-own structure (for example in the brain) which resembles the protein parts of the pathogen.
 Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research ScientistDepartment of Nutrition
Harvard T.H. Chan School of Public HealthBoston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: In a study published in Science in 2022, we reported compelling evidence that infection with the Epstein-Barr virus is the leading cause of Multiple Sclerosis. This is a follow-up study to investigate more in depth whether the antibody response to EBV is distinct in individuals with MS compared to individuals without MS and whether there is a part of EBV that the immune response is particularly targeting. For this purpose we assessed the immune response to all protein parts (peptides) of EBV and their association with MS.
Previous studies could only look at parts of EBV and this is the first study looking at all EBV peptides. Antibodies to EBV (especially to a protein called EBNA1) are known to be overall higher in individuals with MS, so we also tested whether immune response overall or the immune response to specific EBV protein parts was more important. If the immune response to a specific EBV protein part (peptide) would be standing out or distinguishing individuals with MS, we hypothesized, it could point to a specific mechanism of how EBV may cause MS, i.e. it could point for example towards “molecular mimicry”, which is when antibodies targeting a pathogen start targeting a body-own structure (for example in the brain) which resembles the protein parts of the pathogen.
Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research ScientistDepartment of Nutrition
Harvard T.H. Chan School of Public HealthBoston, MA 02115
MedicalResearch.com: What is the background for this study?
Response: In a study published in Science in 2022, we reported compelling evidence that infection with the Epstein-Barr virus is the leading cause of Multiple Sclerosis. This is a follow-up study to investigate more in depth whether the antibody response to EBV is distinct in individuals with MS compared to individuals without MS and whether there is a part of EBV that the immune response is particularly targeting. For this purpose we assessed the immune response to all protein parts (peptides) of EBV and their association with MS.
Previous studies could only look at parts of EBV and this is the first study looking at all EBV peptides. Antibodies to EBV (especially to a protein called EBNA1) are known to be overall higher in individuals with MS, so we also tested whether immune response overall or the immune response to specific EBV protein parts was more important. If the immune response to a specific EBV protein part (peptide) would be standing out or distinguishing individuals with MS, we hypothesized, it could point to a specific mechanism of how EBV may cause MS, i.e. it could point for example towards “molecular mimicry”, which is when antibodies targeting a pathogen start targeting a body-own structure (for example in the brain) which resembles the protein parts of the pathogen.



 Dr. Fangqun Yu[/caption]
Dr. Fangqun Yu PhD
Senior Research Faculty
Atmospheric Sciences Research Center University
Albany, State University of New York
Dr. Fangqun Yu[/caption]
Dr. Fangqun Yu PhD
Senior Research Faculty
Atmospheric Sciences Research Center University
Albany, State University of New York
 Dr. Arshad Nair[/caption]
Dr. Arshad Arjunan Nair PhD
Postdoctoral Associate
Atmospheric Sciences Research Center
University at Albany, State University of New York
Dr. Arshad Nair[/caption]
Dr. Arshad Arjunan Nair PhD
Postdoctoral Associate
Atmospheric Sciences Research Center
University at Albany, State University of New York



 Wilson N. Merrell
Ph.D. Student
Wilson N. Merrell
Ph.D. Student
 Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.
Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.
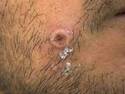
 Dr. Angélica Cifuentes Kottkamp[/caption]
Angélica
Dr. Angélica Cifuentes Kottkamp[/caption]
Angélica
 Dr. Mohyuddin[/caption]
Hira Mohyuddin, PGY-2
Psychiatry Residency Training Program
The George Washington University
MedicalResearch.com: What is the background for this study?
Response: Frailty has become increasingly significant as the global population grows older, as this syndrome is linked with a higher mortality and morbidity in aging. Causes contributing to frailty are poorly understood, but it seems that the role of inflammation is very likely.
While other chronic infections were shown to precipitate and perpetuate inflammation that contributes to the development of frailty, no prior study has previously focused on possible links between Toxoplasma gondii and geriatric frailty. Benefiting from a collaboration with Spanish and Portuguese researchers, we have now tested, for the first time to our knowledge, this possible association.
Dr. Mohyuddin[/caption]
Hira Mohyuddin, PGY-2
Psychiatry Residency Training Program
The George Washington University
MedicalResearch.com: What is the background for this study?
Response: Frailty has become increasingly significant as the global population grows older, as this syndrome is linked with a higher mortality and morbidity in aging. Causes contributing to frailty are poorly understood, but it seems that the role of inflammation is very likely.
While other chronic infections were shown to precipitate and perpetuate inflammation that contributes to the development of frailty, no prior study has previously focused on possible links between Toxoplasma gondii and geriatric frailty. Benefiting from a collaboration with Spanish and Portuguese researchers, we have now tested, for the first time to our knowledge, this possible association.

 Prof. Takeshi[/caption]
Prof. Takeshi Asai
Faculty of Health and Sports Sciences, University of Tsukuba,
Tsukuba Japan
Faculty of Physical Education, International Pacific University
Okayama, Japan
MedicalResearch.com: What is the background for this study?
Response: In the early stages of the COVID-19 pandemic, contact and droplet transmission were considered the main routes of infection. However, it was later demonstrated that airborne transmission is an important route. Therefore, accumulating real-world data on airborne transmission was deemed crucial.
Prof. Takeshi[/caption]
Prof. Takeshi Asai
Faculty of Health and Sports Sciences, University of Tsukuba,
Tsukuba Japan
Faculty of Physical Education, International Pacific University
Okayama, Japan
MedicalResearch.com: What is the background for this study?
Response: In the early stages of the COVID-19 pandemic, contact and droplet transmission were considered the main routes of infection. However, it was later demonstrated that airborne transmission is an important route. Therefore, accumulating real-world data on airborne transmission was deemed crucial.


 Dr. Sood[/caption]
Neeraj Sood, PhD
Verna and Peter Dauterive Hall
University Park Campus
University of Southern California
Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We conducted this study to inform school COVID-19 policies.
The main findings are that the median duration of infectivity after a positive COVID-19 test in children is 3 days. The median duration of infectivity does not vary with vaccination.
Dr. Sood[/caption]
Neeraj Sood, PhD
Verna and Peter Dauterive Hall
University Park Campus
University of Southern California
Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We conducted this study to inform school COVID-19 policies.
The main findings are that the median duration of infectivity after a positive COVID-19 test in children is 3 days. The median duration of infectivity does not vary with vaccination. 
 Dr. Jernigan[/caption]
Dr. John Jernigan, MD MS
Clinical Associate Professor of Medicine
Division of Infectious Diseases
Emory University School of Medicine
Branch Chief
Epidemiology, Research and Innovations Branch
CDC Center for Disease Control
MedicalResearch.com: What is the background for this study?
Response: Staphylococcus aureus commonly causes infections in ICUs. One approach to preventing these infections is using nasal mupirocin plus chlorhexidine gluconate (CHG) bathing for ICU patients. This practice is known to prevent methicillin-resistant Staphylococcus aureus (MRSA) infections and all-cause. bloodstream infections. This practice has been broadly adopted in ICUs in the US, but adoption of mupirocin as a universal topical antibiotic has been slowed by concerns for engendering mupirocin resistance.
This cluster-randomized trial in adult ICUs was conducted to assess whether universal nasal antiseptic povidone-iodine (iodophor), to which minimal S. aureus resistance is expected, was an acceptable alternative to universal nasal mupirocin for reducing S. aureus and MRSA clinical cultures in the setting of daily CHG bathing. Those who received chlorhexidine (CHG) bathing with mupirocin had an 18% reduction in risk of Staphylococcus aureus clinical cultures and a 15% reduction in risk of methicillin-resistant
Dr. Jernigan[/caption]
Dr. John Jernigan, MD MS
Clinical Associate Professor of Medicine
Division of Infectious Diseases
Emory University School of Medicine
Branch Chief
Epidemiology, Research and Innovations Branch
CDC Center for Disease Control
MedicalResearch.com: What is the background for this study?
Response: Staphylococcus aureus commonly causes infections in ICUs. One approach to preventing these infections is using nasal mupirocin plus chlorhexidine gluconate (CHG) bathing for ICU patients. This practice is known to prevent methicillin-resistant Staphylococcus aureus (MRSA) infections and all-cause. bloodstream infections. This practice has been broadly adopted in ICUs in the US, but adoption of mupirocin as a universal topical antibiotic has been slowed by concerns for engendering mupirocin resistance.
This cluster-randomized trial in adult ICUs was conducted to assess whether universal nasal antiseptic povidone-iodine (iodophor), to which minimal S. aureus resistance is expected, was an acceptable alternative to universal nasal mupirocin for reducing S. aureus and MRSA clinical cultures in the setting of daily CHG bathing. Those who received chlorhexidine (CHG) bathing with mupirocin had an 18% reduction in risk of Staphylococcus aureus clinical cultures and a 15% reduction in risk of methicillin-resistant 
 Dr. Stevermer [/caption]
James Stevermer, M.D., M.S.P.H.Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: HIV continues to be a significant public health issue. The good news is that PrEP is a safe, highly effective way to help prevent HIV in people at increased risk. There are now two ways people can take PrEP – as a pill or as a shot. We encourage healthcare professionals to have a conversation with their patients about their individual risk for HIV and determine if they should consider taking whichever form of PrEP would work best for them.
Dr. Stevermer [/caption]
James Stevermer, M.D., M.S.P.H.Vice chair for clinical affairs
Professor of family and community medicine
University of Missouri
Medical director of MU Health Care Family Medicine–Callaway Physicians,
Dr. Stevermer joined the U.S. Preventive Service Task Force in January 2021.
MedicalResearch.com: What is the background for this study?
Response: HIV continues to be a significant public health issue. The good news is that PrEP is a safe, highly effective way to help prevent HIV in people at increased risk. There are now two ways people can take PrEP – as a pill or as a shot. We encourage healthcare professionals to have a conversation with their patients about their individual risk for HIV and determine if they should consider taking whichever form of PrEP would work best for them.

 Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD
Prof. Kaforou[/caption]
MedicalResearch.com Interview with:
Myrsini Kaforou, PhD




 MedicalResearch.com: What is the background for this study?
Response: I became interested in dog's sense of smell several years ago while doing therapy dog demonstrations at the California Science Center in Los Angeles during a special traveling exhibit "Dogs! A Science Tail." (Now at the Orlando Science Center). I did a lot of research on this topic and taught children about it through the Los Angeles Public Library using my Great Pyrenees therapy dogs. Then, COVID broke out and I expanded my research into any work being done to possibly utilize scent dogs for screening and testing for COVID. I found only a few such studies. However, I fortuitously met Heather Junqueira of BioScent, Inc. (in Florida) online and she was beginning to successfully teach her beagles to detect COVID-related odors. She agreed to co-author a peer-reviewed review paper with me. That led to our first paper -
Dickey, T, Junqueira, H. Toward the use of medical scent dogs for COVID-19 screening. J Osteopath Med 2021;1(2): 141-148.
MedicalResearch.com: What is the background for this study?
Response: I became interested in dog's sense of smell several years ago while doing therapy dog demonstrations at the California Science Center in Los Angeles during a special traveling exhibit "Dogs! A Science Tail." (Now at the Orlando Science Center). I did a lot of research on this topic and taught children about it through the Los Angeles Public Library using my Great Pyrenees therapy dogs. Then, COVID broke out and I expanded my research into any work being done to possibly utilize scent dogs for screening and testing for COVID. I found only a few such studies. However, I fortuitously met Heather Junqueira of BioScent, Inc. (in Florida) online and she was beginning to successfully teach her beagles to detect COVID-related odors. She agreed to co-author a peer-reviewed review paper with me. That led to our first paper -
Dickey, T, Junqueira, H. Toward the use of medical scent dogs for COVID-19 screening. J Osteopath Med 2021;1(2): 141-148. 



 Dr. Stephens[/caption]
Dr Jacqueline Stephens MPH, PhD
Epidemiologist & Senior lecturer
Flinders University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: An increase in the volume of evidence published in the peer-reviewed literature on this topic prompted an update of this Cochrane Review.
Dr. Stephens[/caption]
Dr Jacqueline Stephens MPH, PhD
Epidemiologist & Senior lecturer
Flinders University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: An increase in the volume of evidence published in the peer-reviewed literature on this topic prompted an update of this Cochrane Review.
 Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services,
Dr. Gandhi[/caption]
Manoj Gandhi, MD PhD
Senior Medical Director of Genetic Testing Services, 


 Dr. Roca[/caption]
Anna Roca PhD
MRC Unit The Gambia at the London School of Hygiene and Tropical Medicine
Fajara, The Gambia
MedicalResearch.com: What is the background for this study?
Response: Context specific interventions are needed to decrease the high burden of severe neonatal morbidity and mortality in sub-Saharan Africa. Severe bacterial infections are a main cause of neonatal mortality in the continent. Oral intra-partum azithromycin is a cheap intervention easily scalable. Before embarking on this trial, we conducted a proof-of-concept trial that showed the intervention reduced maternal and neonatal bacterial carriage of the most prevalent bacteria causing neonatal sepsis in the continent.
Dr. Roca[/caption]
Anna Roca PhD
MRC Unit The Gambia at the London School of Hygiene and Tropical Medicine
Fajara, The Gambia
MedicalResearch.com: What is the background for this study?
Response: Context specific interventions are needed to decrease the high burden of severe neonatal morbidity and mortality in sub-Saharan Africa. Severe bacterial infections are a main cause of neonatal mortality in the continent. Oral intra-partum azithromycin is a cheap intervention easily scalable. Before embarking on this trial, we conducted a proof-of-concept trial that showed the intervention reduced maternal and neonatal bacterial carriage of the most prevalent bacteria causing neonatal sepsis in the continent.

 Dr. Khullar[/caption]
Dhruv Khullar, M.D., M.P.P.
Director of Policy Dissemination
Physicians Foundation Center for Physician Practice and Leadership
Assistant Professor of Health Policy and Economics
Weill Cornell Medicine, NYC
MedicalResearch.com: What is the background for this study?
Response: From prior research, we know that there are racial/ethnic differences in the acute impact of COVID-19, including higher rates of hospitalization and death among Black and Hispanic individuals compared to white individuals. Less is known about whether there are differences in the rates or types of long COVID by race and ethnicity.
Dr. Khullar[/caption]
Dhruv Khullar, M.D., M.P.P.
Director of Policy Dissemination
Physicians Foundation Center for Physician Practice and Leadership
Assistant Professor of Health Policy and Economics
Weill Cornell Medicine, NYC
MedicalResearch.com: What is the background for this study?
Response: From prior research, we know that there are racial/ethnic differences in the acute impact of COVID-19, including higher rates of hospitalization and death among Black and Hispanic individuals compared to white individuals. Less is known about whether there are differences in the rates or types of long COVID by race and ethnicity.

