Author Interviews, Gout, Kidney Disease, NEJM / 24.06.2020
Does Lowering Uric Acid with Allopurinol Slow Progression of Chronic Kidney Disease?
MedicalResearch.com Interview with:
[caption id="attachment_50193" align="alignleft" width="84"] Dr. Badve[/caption]
Sunil Badve MBBS, MD, DNB, FRACP, PhD, FASN
Staff specialist nephrologist | St George Hospital
Conjoint Associate Professor | University of New South Wales
Senior Research Fellow, Acute Kidney Injury and Trials
The George Institute for Global Health
Australia
MedicalResearch.com: What is the background for this study?
Response: Elevated serum urate levels are associated with progression of chronic kidney disease (CKD). CKD patients often have elevated serum urate levels due to decreased excretion.
We conducted this placebo-controlled randomized trial to evaluate if urate-lowering treatment with allopurinol would attenuate decline in estimated glomerular filtration rate (eGFR) over 2 years in patients with CKD. We enrolled 369 CKD patients with high progression risk and no prior history of gout.
Dr. Badve[/caption]
Sunil Badve MBBS, MD, DNB, FRACP, PhD, FASN
Staff specialist nephrologist | St George Hospital
Conjoint Associate Professor | University of New South Wales
Senior Research Fellow, Acute Kidney Injury and Trials
The George Institute for Global Health
Australia
MedicalResearch.com: What is the background for this study?
Response: Elevated serum urate levels are associated with progression of chronic kidney disease (CKD). CKD patients often have elevated serum urate levels due to decreased excretion.
We conducted this placebo-controlled randomized trial to evaluate if urate-lowering treatment with allopurinol would attenuate decline in estimated glomerular filtration rate (eGFR) over 2 years in patients with CKD. We enrolled 369 CKD patients with high progression risk and no prior history of gout.
 Dr. Badve[/caption]
Sunil Badve MBBS, MD, DNB, FRACP, PhD, FASN
Staff specialist nephrologist | St George Hospital
Conjoint Associate Professor | University of New South Wales
Senior Research Fellow, Acute Kidney Injury and Trials
The George Institute for Global Health
Australia
MedicalResearch.com: What is the background for this study?
Response: Elevated serum urate levels are associated with progression of chronic kidney disease (CKD). CKD patients often have elevated serum urate levels due to decreased excretion.
We conducted this placebo-controlled randomized trial to evaluate if urate-lowering treatment with allopurinol would attenuate decline in estimated glomerular filtration rate (eGFR) over 2 years in patients with CKD. We enrolled 369 CKD patients with high progression risk and no prior history of gout.
Dr. Badve[/caption]
Sunil Badve MBBS, MD, DNB, FRACP, PhD, FASN
Staff specialist nephrologist | St George Hospital
Conjoint Associate Professor | University of New South Wales
Senior Research Fellow, Acute Kidney Injury and Trials
The George Institute for Global Health
Australia
MedicalResearch.com: What is the background for this study?
Response: Elevated serum urate levels are associated with progression of chronic kidney disease (CKD). CKD patients often have elevated serum urate levels due to decreased excretion.
We conducted this placebo-controlled randomized trial to evaluate if urate-lowering treatment with allopurinol would attenuate decline in estimated glomerular filtration rate (eGFR) over 2 years in patients with CKD. We enrolled 369 CKD patients with high progression risk and no prior history of gout.






 Dr. Bin Cao[/caption]
Bin Cao, Yeming Wang, Guohui Fan,
Lianghan Shang, Jiuyang Xu, DingyuZhang, Chen Wang
on behalf of LOTUS-China Study Group
China-Japan Friendship Hospital; Wuhan Jintinyan Hospital;
Institute of Respiratory Medicine, Chinese Academy of Medical Science
MedicalResearch.com: What is the background for this study?
Response: In the past two months, the outbreak of Coronavirus Disease 2019 (COVID-19) has been spreading rapidly across the world. Science and technology is the most powerful weapon for human to fight against diseases, especially in such a pandemic setting. Seeking for effective antiviral medication is the most critical and urgent among the many scientific tasks in the pandemic.
At the most critical moment in the fight against COVID-19, Chinese clinical scientists have stepped forward under extremely difficult research conditions to carry out clinical trials in antiviral treatment including lopinavir–ritonavir and remdesivir, in a swift, decisive and effective manner. These trials have attracted worldwide attention.
Recently, the Lopinavir–ritonavir Trial for suppression of SARS-CoV-2 in China (LOTUS-China) has been completed, which, with great clinical significance, can provide strong evidence for the treatment of COVID-19 both in China and around the world.
Dr. Bin Cao[/caption]
Bin Cao, Yeming Wang, Guohui Fan,
Lianghan Shang, Jiuyang Xu, DingyuZhang, Chen Wang
on behalf of LOTUS-China Study Group
China-Japan Friendship Hospital; Wuhan Jintinyan Hospital;
Institute of Respiratory Medicine, Chinese Academy of Medical Science
MedicalResearch.com: What is the background for this study?
Response: In the past two months, the outbreak of Coronavirus Disease 2019 (COVID-19) has been spreading rapidly across the world. Science and technology is the most powerful weapon for human to fight against diseases, especially in such a pandemic setting. Seeking for effective antiviral medication is the most critical and urgent among the many scientific tasks in the pandemic.
At the most critical moment in the fight against COVID-19, Chinese clinical scientists have stepped forward under extremely difficult research conditions to carry out clinical trials in antiviral treatment including lopinavir–ritonavir and remdesivir, in a swift, decisive and effective manner. These trials have attracted worldwide attention.
Recently, the Lopinavir–ritonavir Trial for suppression of SARS-CoV-2 in China (LOTUS-China) has been completed, which, with great clinical significance, can provide strong evidence for the treatment of COVID-19 both in China and around the world.





 Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
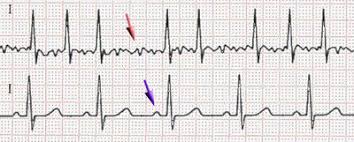
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.
Dr. Kistler[/caption]
Professor Peter M Kistler MBBS, PhD, FRACP
Head of Clinical Electrophysiology Research
Baker Heart and Diabetes Institute
Head of Electrophysiology at The Alfred hospital
Professor of Medicine
University of Melbourne.
MedicalResearch.com: What is the background for this study?
Response: There is a well known association between alcohol intake and atrial fibrillation form population based studies which demonstrate that for every 1 standard drink the incidence of AFib increases by 8%.
This is the first randomised study to determine of alcohol reduction/abstinence leads to a reduction in AFib episodes and time to recurrence.