MedicalResearch.com Interview with:
[caption id="attachment_37907" align="alignleft" width="100"]

Dr. Péault[/caption]
Bruno Péault PhD
Professor and Chair, Vascular Regeneration
Center For Cardiovascular Science
MRC Centre for Regenerative Medicine
Scientific Director, BHF Laboratories
The University of Edinburgh and
Professor, David Geffen School of Medicine at UCLA
Orthopaedic Hospital Research Center
University of California at Los Angeles
Los Angeles, CA 90095-7358
MedicalResearch.com: What is the background for this study?
Response: Kidney, lung, liver, muscle, heart are among the many organs which can be severely affected by fibrosis, a natural scarring process whereby healthy tissues are replaced by a fibrous non-functional substitute. For instance, the billions of cardiac muscle cells that die after a heart infarct, consequently to blood supply interruption, are replaced by a fibrotic scar that cannot contract, reducing the capacity of the heart to pump blood, and leading often to heart failure. There is currently no efficient treatment of fibrotic scars, the basic cellular component of which is the myofibroblast, a cell of unremarkable appearance and unclear origin. The transforming growth factor β (TGFβ) molecule triggers fibrosis development after being activated, via the extra-cellular matrix, by αv integrins, which are adhesion molecules present at the surface of the target cells.
To gain further insight into the cells that drive fibrosis in the heart and skeletal muscle, and explore ways to control this deleterious process, mice were used in which cells expressing the β receptor for PDGF (platelet derived growth factor) have been genetically tagged with a green fluorescent protein, a system previously used by Prof. Neil Henderson to trace fibrosis in the diseased liver (cells naturally expressing PDGFRβ are, in their vast majority, perivascular cells surrounding small blood vessels, as well as some interstitial fibroblasts). Skeletal muscle was injured by a small incision or with a targeted injection of cardiotoxin, a snake venom compound that locally kills myofibers, while the heart was damaged by prolonged infusion of angiotensin II. In both settings, progression of fibrosis was followed over time and contribution of green fluorescent cells – i.e. those expressing PDGFRβ – was assessed.
 Lina Mørch PhD, MSc
Senior Researcher
Rigshospitalet
MedicalResearch.com: What is the background for this study? What are the main findings?
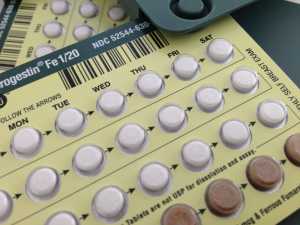
Response: There was a lack of evidence on contemporary hormonal contraception and risk of breast cancer. In particular the knowledge of risk with newer progestins was sparse.
Lina Mørch PhD, MSc
Senior Researcher
Rigshospitalet
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There was a lack of evidence on contemporary hormonal contraception and risk of breast cancer. In particular the knowledge of risk with newer progestins was sparse.
 Lina Mørch PhD, MSc
Senior Researcher
Rigshospitalet
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There was a lack of evidence on contemporary hormonal contraception and risk of breast cancer. In particular the knowledge of risk with newer progestins was sparse.
Lina Mørch PhD, MSc
Senior Researcher
Rigshospitalet
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: There was a lack of evidence on contemporary hormonal contraception and risk of breast cancer. In particular the knowledge of risk with newer progestins was sparse.











 Dr. Jordan[/caption]
Stanley C. Jordan, M.D
Director, Division of Nephrology
Medical Director, Kidney Transplant Program
Medical Director, Human Leukocyte Antigen and Transplant Immunology Laboratory
Cedars-Sinai, Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study is as follows: Patients who are highly HLA sensitized have antibodies to transplant targets create an immunologic barrier to transplant. Currently, there are no approved therapies for elimination of these antibodies. Desensitization is available but is not always successful and most desensitized patients are still transplanted with a positive crossmatch. Thus, many patients are not able to receive life-saving kidney transplants unless newer therapies to remove antibodies are found.
The findings of our study published in the New England Journal of Medicine revealed that the use of the enzyme from streptococcal pyogenes called IdeS® (IgG endopeptidase) is very effective in eliminating donor specific antibodies and allowing transplantation to occur. Antibodies were eliminated from one week up to two months after one treatment with Ides® allowing a safe environment for the transplant to occur. Rejections episodes did occur in some of the patients but were generally mild and easily treatable. Only one patient of 25 lost his allograft during the study. Thus, the study shows promising results for a new approach for elimination of pathogenic antibodies that did not exist before.
Dr. Jordan[/caption]
Stanley C. Jordan, M.D
Director, Division of Nephrology
Medical Director, Kidney Transplant Program
Medical Director, Human Leukocyte Antigen and Transplant Immunology Laboratory
Cedars-Sinai, Los Angeles, CA
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The background for this study is as follows: Patients who are highly HLA sensitized have antibodies to transplant targets create an immunologic barrier to transplant. Currently, there are no approved therapies for elimination of these antibodies. Desensitization is available but is not always successful and most desensitized patients are still transplanted with a positive crossmatch. Thus, many patients are not able to receive life-saving kidney transplants unless newer therapies to remove antibodies are found.
The findings of our study published in the New England Journal of Medicine revealed that the use of the enzyme from streptococcal pyogenes called IdeS® (IgG endopeptidase) is very effective in eliminating donor specific antibodies and allowing transplantation to occur. Antibodies were eliminated from one week up to two months after one treatment with Ides® allowing a safe environment for the transplant to occur. Rejections episodes did occur in some of the patients but were generally mild and easily treatable. Only one patient of 25 lost his allograft during the study. Thus, the study shows promising results for a new approach for elimination of pathogenic antibodies that did not exist before.









