Author Interviews, Blood Pressure - Hypertension, Diabetes, JAMA, Race/Ethnic Diversity / 13.09.2021
Medicaid Expansion Linked to Improved in Hypertension and Diabetes Outcomes, especially in Minority Patients
MedicalResearch.com Interview with:
[caption id="attachment_58077" align="alignleft" width="125"] Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
 Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.
Dr. Cole[/caption]
Megan B. Cole, PhD, MPH
Assistant Professor | Dept. of Health Law, Policy, & Management
Co-Director | BU Medicaid Policy Lab
Boston University School of Public Health
Boston, MA 02118
MedicalResearch.com: What is the background for this study?
Response: Under the Affordable Care Act, states were given the option to expand Medicaid eligibility to nonelderly adults with incomes up to 138% of the federal poverty level, where in January 2014, 25 states plus Washington, DC expanded eligibility, with 13 additional states expanding thereafter. State Medicaid expansion decisions were particularly consequential for federally qualified health centers (FQHCs), which serve nearly 30 million low-income, disproportionately uninsured patients across the US.
We know from earlier work that in the shorter-term, Medicaid expansion was associated with improvements in quality of care process measures and FQHC service capacity. However, we conducted the first known nationally representative study to examine how Medicaid expansion impacted key chronic disease outcome measures at FQHCs over the longer-term by looking at changes five years after implementation, including changes by race/ethnicity.









 Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.
Amanda Paluch, PhD
Assistant Professor
University of Massachusetts Amherst
Department of Kinesiology
Institute for Applied Life Sciences
Life Science Laboratories
Amherst, MA 01003
MedicalResearch.com: What is the background for this study?
Response: We wanted to understand the association of total steps per day with premature mortality among middle-aged, Black and White women and men. This study included 2110 adults; age 38-50 years old at the start of this study. These adults wore a step counting device for one week and then followed for death from any cause over the next 10 years.







 Dr. Gary Smith[/caption]
Gary A. Smith, MD, DrPH
Director, Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: Furniture and TV tip-overs are an important source of injury, especially for children younger than 6 years old. Our study found that an estimated 560,200 children younger than 18 years old were treated in U.S. emergency departments for furniture or TV tip-over injuries from 1990 through 2019. In 2019, there were 11,521 injured children, which is an average of one child every 46 minutes.
Dr. Gary Smith[/caption]
Gary A. Smith, MD, DrPH
Director, Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: Furniture and TV tip-overs are an important source of injury, especially for children younger than 6 years old. Our study found that an estimated 560,200 children younger than 18 years old were treated in U.S. emergency departments for furniture or TV tip-over injuries from 1990 through 2019. In 2019, there were 11,521 injured children, which is an average of one child every 46 minutes.







 Dr. Anderson[/caption]
Dr. Weston B Anderson PhD
Postdoctoral Reasearch Scientist
International Research Institute for Climate and Society
The Earth Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We find that while drought continues to be a consistent trigger of food crises in Sub-Saharan Africa, protracted conflict has become relatively more important over the last decade.
We furthermore find that pastoral livelihoods have taken longer to return to food secure conditions following droughts as compared to agricultural livelihoods.
Dr. Anderson[/caption]
Dr. Weston B Anderson PhD
Postdoctoral Reasearch Scientist
International Research Institute for Climate and Society
The Earth Institute
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We find that while drought continues to be a consistent trigger of food crises in Sub-Saharan Africa, protracted conflict has become relatively more important over the last decade.
We furthermore find that pastoral livelihoods have taken longer to return to food secure conditions following droughts as compared to agricultural livelihoods.
 Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
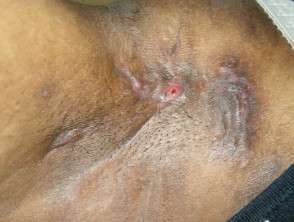
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend
Dr. Albrecht[/caption]
Joerg Albrecht, MD, PhD
Dermatologist, Internist, Clinical Pharmacologist
Division of Dermatology, Department of Medicine
Attending Dermatologist, Chair Division of Dermatology
Chair system-wide Pharmacy & Therapeutics Committee
Cook County Health
Chicago, IL 60612
MedicalResearch.com: What is the background for this study?
Response: The study was stimulated by data that suggested that an unusually large proportion of inpatient with Hidradenitis suppurativa (HS) were African American. HS is an underdiagnosed disease and the total numbers of inpatients with HS in the year we looked at initially seemed small. So we wanted to test whether this finding held up when the period of observation was extended. Point estimates can be unreliable and we had followed another finding in the data that did not hold up when we looked at other years, so we felt one year was not enough to confirm a trend

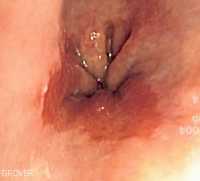
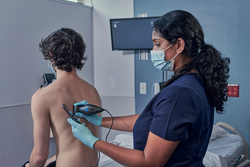
 Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63.
Response: Point-of-care ultrasound is one of the most significant advances in bedside patient care, and its use is expanding across nearly all fields of medicine. In order to best prepare medical students for residency and beyond, it is imperative to begin POCUS training as early as possible. At the Lewis Katz School of Medicine at Temple University, we introduced POCUS education over a decade ago and have expanded it since then.
By providing each student with a Butterfly iQ device, we can augment our curriculum significantly. In addition to our robust pre-clinical sessions, now we will expand into the clinical years highlighting the utility of POCUS with actual patients.
This gift was made possible by the incredible generosity of Dr. Ronald Salvitti, MD ’63. 

 Dr. Mahncke[/caption]
Henry Mahncke, PhD
Chief Executive Officer
Posit Science
Dr. Mahncke earned his PhD at UCSF in the lab where lifelong brain plasticity as discovered. At the request of his academic mentor, he currently leads a global team of more than 400 brain scientists engaged in designing, testing, refining, and validating the computerized brain exercises found in the BrainHQ app from Posit Science, where he serves as CEO.
This week, MedicalResearch.com interviews Dr. Mahncke about a new study, with breakthrough results for service members and Veterans grappling with the signature injury of recent wars.
MedicalResearch.com: What makes this study newsworthy?
Response: As the last troops come home from Afghanistan, the battle is not over for many who served and continue to grapple with the signature injury of recent conflicts — mild Traumatic Brain Injury (or mTBI). Typically, such injures were caused by blasts or concussions, and they’ve been diagnosed in more than 300,000 service members. Most recover within a couple days or weeks, but for many — some estimate fifteen percent — physical, psychological, emotional, and cognitive problems persist for years. Such injuries often go untreated, because treatments focus on in-person, customized, cognitive rehabilitation, which can be helpful, but is costly, time-consuming, requires travel for treatment, and relies on the craft and expertise of the healthcare provider.
Up until now, there’s been no effective intervention that’s highly-scalable and that can be delivered remotely. This study showed that remotely-administered BrainHQ computerized exercises improved overall cognitive performance in a population with very persistent cognitive issues. On average, patients in this study had cognitive issues for more than seven years. That means we finally have a tool shown effective in a gold-standard study that practitioners can employ in treating this large and underserved population, who sacrificed so much to serve our nation.
Dr. Mahncke[/caption]
Henry Mahncke, PhD
Chief Executive Officer
Posit Science
Dr. Mahncke earned his PhD at UCSF in the lab where lifelong brain plasticity as discovered. At the request of his academic mentor, he currently leads a global team of more than 400 brain scientists engaged in designing, testing, refining, and validating the computerized brain exercises found in the BrainHQ app from Posit Science, where he serves as CEO.
This week, MedicalResearch.com interviews Dr. Mahncke about a new study, with breakthrough results for service members and Veterans grappling with the signature injury of recent wars.
MedicalResearch.com: What makes this study newsworthy?
Response: As the last troops come home from Afghanistan, the battle is not over for many who served and continue to grapple with the signature injury of recent conflicts — mild Traumatic Brain Injury (or mTBI). Typically, such injures were caused by blasts or concussions, and they’ve been diagnosed in more than 300,000 service members. Most recover within a couple days or weeks, but for many — some estimate fifteen percent — physical, psychological, emotional, and cognitive problems persist for years. Such injuries often go untreated, because treatments focus on in-person, customized, cognitive rehabilitation, which can be helpful, but is costly, time-consuming, requires travel for treatment, and relies on the craft and expertise of the healthcare provider.
Up until now, there’s been no effective intervention that’s highly-scalable and that can be delivered remotely. This study showed that remotely-administered BrainHQ computerized exercises improved overall cognitive performance in a population with very persistent cognitive issues. On average, patients in this study had cognitive issues for more than seven years. That means we finally have a tool shown effective in a gold-standard study that practitioners can employ in treating this large and underserved population, who sacrificed so much to serve our nation.

 Dr. Lane[/caption]
Scott D. Lane Ph.D.
McGovern Medical School
Vice Chair For Research
Director Of Neurobehavioral Laboratory
Center For Neurobehavioral Research On Addiction
Director Of Research
University of Texas Health Science Center at Houston
Houston, TX
MedicalResearch.com: What is the background for this study?
Response: Addiction science has made considerable progress in understanding how cocaine and other addictive drugs impair the brain. Over time, cocaine can disrupt brain regions that help us think, plan, solve problems, and exert self-control. These disruptions in brain structure can be seen in neuroimaging studies that reveal impairment in the nerve fibers or white matter (WM) tracts in the central and front parts of the brain. We conducted two systematic meta-analytic reviews of the literature to document the robustness of evidence showing alterations in WM integrity of chronic stimulant users relative to healthy control subjects who did not use cocaine or other drugs of abuse (Beard et al., 2019; Suchting et al., 2020). Importantly, WM impairments negatively predict treatment outcome, meaning individuals with greater levels of WM impairment are less likely to benefit from treatment and more likely to experience deficits in attention, working memory, and impulse control.
We reasoned that pharmacological interventions shown to protect WM integrity may help improve cognition and treatment outcomes in patients recovering from cocaine addiction. Pioglitazone, an approved medication for type 2 diabetes, has been shown to reduce inflammation and mediate protection after traumatic brain injury. The therapeutic potential of pioglitazone has prompted investigation of its role in neurodegenerative conditions, such as dementia, Alzheimer’s disease, and stroke. Similar to these brain diseases and injuries, pioglitazone might effectively protect the brain from the inflammatory damage created by cocaine use.
Dr. Lane[/caption]
Scott D. Lane Ph.D.
McGovern Medical School
Vice Chair For Research
Director Of Neurobehavioral Laboratory
Center For Neurobehavioral Research On Addiction
Director Of Research
University of Texas Health Science Center at Houston
Houston, TX
MedicalResearch.com: What is the background for this study?
Response: Addiction science has made considerable progress in understanding how cocaine and other addictive drugs impair the brain. Over time, cocaine can disrupt brain regions that help us think, plan, solve problems, and exert self-control. These disruptions in brain structure can be seen in neuroimaging studies that reveal impairment in the nerve fibers or white matter (WM) tracts in the central and front parts of the brain. We conducted two systematic meta-analytic reviews of the literature to document the robustness of evidence showing alterations in WM integrity of chronic stimulant users relative to healthy control subjects who did not use cocaine or other drugs of abuse (Beard et al., 2019; Suchting et al., 2020). Importantly, WM impairments negatively predict treatment outcome, meaning individuals with greater levels of WM impairment are less likely to benefit from treatment and more likely to experience deficits in attention, working memory, and impulse control.
We reasoned that pharmacological interventions shown to protect WM integrity may help improve cognition and treatment outcomes in patients recovering from cocaine addiction. Pioglitazone, an approved medication for type 2 diabetes, has been shown to reduce inflammation and mediate protection after traumatic brain injury. The therapeutic potential of pioglitazone has prompted investigation of its role in neurodegenerative conditions, such as dementia, Alzheimer’s disease, and stroke. Similar to these brain diseases and injuries, pioglitazone might effectively protect the brain from the inflammatory damage created by cocaine use.