Aging, Author Interviews, Environmental Risks, Nature / 30.07.2022
Avoidance of Blue Light Might Be A Good Anti-Aging Strategy
MedicalResearch.com Interview with:
[caption id="attachment_59381" align="alignleft" width="150"] Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
 Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.
Dr. Giebultowicz[/caption]
Dr. Jaga Giebultowicz
Professor Emeritus,
Department of Integrative Biology
Oregon State University
Corvallis, OR 97331
MedicalResearch.com: What is the background for this study? Where is blue light commonly found?
Response: Our study in short-lived model organism Drosophila revealed that cumulative, long-term exposure to blue light impacts brain function, accelerates the aging process and significantly shortens lifespan compared to flies maintained in constant darkness or in white light with blue wavelengths blocked.
Blue light is predominantly produced by the light-emitting diodes (LEDs); it appears white due to the addition of yellow fluorescent powder which is activated by blue light. LEDs has become a main source of display screens (phones, laptops, desktops, TV), and ambient lights. Indeed, humans have become awash in LEDs for most of their waking hours.



 Clare Jensen[/caption]
Clare Jensen
O’Haire Research Team
Center for the Human-Animal Bond
Purdue University College of Veterinary Medicine
MedicalResearch.com: What is the background for this study?
Response: Service dogs for PTSD are becoming more common and the evidence shows they can help improve mental health and quality of life for many veterans with PTSD. However, some veterans benefit more than others. Our research goal was to ask for the very first time: Why?
Clare Jensen[/caption]
Clare Jensen
O’Haire Research Team
Center for the Human-Animal Bond
Purdue University College of Veterinary Medicine
MedicalResearch.com: What is the background for this study?
Response: Service dogs for PTSD are becoming more common and the evidence shows they can help improve mental health and quality of life for many veterans with PTSD. However, some veterans benefit more than others. Our research goal was to ask for the very first time: Why?

 Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
Dr. LeBoff[/caption]
Meryl S. LeBoff, MD
 Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.
Dr. Manson[/caption]
JoAnn E. Manson, MD, DrPH
Professor, Epidemiology, Harvard T.H. Chan School Of Public Health
Michael and Lee Bell Professor of Women's Health, Medicine, Harvard Medical School
Chief, Preventive Medicine, Brigham And Women's Hospital
Co-Director, Womens Health, Brigham And Women's Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Osteoporosis is a major public health problem. Although supplemental vitamin D has been widely used to reduce the risk of fractures in the general population, studies of the effects of vitamin D on fractures, the most important bone health outcome, have been conflicting.
Randomized controlled trials, the highest quality studies, from around the world have shown benefit, no effect, or even harm of supplemental vitamin D on risk of fractures. Some of the trials used bolus dosing, had small samples sizes or short study duration, and co-administered calcium. No large RCTS of this scale tested whether daily supplemental vitamin D (without co-administration with calcium) prevented fractures in the US population.
To fill these knowledge gaps, we tested the hypothesis in this ancillary study to VITAL, whether daily supplemental vitamin D3 reduced the risk of incident total, non-spine and hip fractures in women and men in the US.



 Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.
Joanna Jiang, PhD
Agency for Healthcare Research and Quality
Rockville, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Over the last decade we have seen two trends occurring to rural hospitals – closures and mergers. A hospital in financial distress could likely face closure. But if the hospital affiliates with a multihospital system, it may have access to resources from the system that help shelter the hospital from closure.
That is exactly what we found in this study. System affiliation was associated with a lower risk of closure for financially distressed hospitals. However, among hospitals that were financially stable, system affiliation was associated with a higher risk of closure. This is somewhat puzzling and needs further study to better understand the reason for closure.

 Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
Dr. Midya[/caption]
Dania Valvi, MD MPH PhD
Assistant Professor
Department of Environmental Medicine and Public Health
Co-Director, MS in Epidemiology
Icahn School of Medicine at Mount Sinai
Email: dania.valvi@mssm.edu
MedicalResearch.com: What is the background for this study?
Response: Non-alcoholic fatty liver disease (NAFLD) is the most common liver disease in children in the U.S., Europe and other world regions, currently affecting 1 in every 10 children, and 1 in every 3 children with obesity in the U.S. The rate of pediatric NAFLD has more than doubled in recent decades following the epidemic rates also noted for childhood obesity. There is increasing interest in the role that environmental chemical exposures may play in NAFLD etiology, since several animal studies have shown that prenatal exposures to endocrine-disrupting chemicals (EDCs) cause liver injury and damage; but, until now, the potential effects of prenatal EDC mixture exposures in pediatric NAFLD had not been studied.
 SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
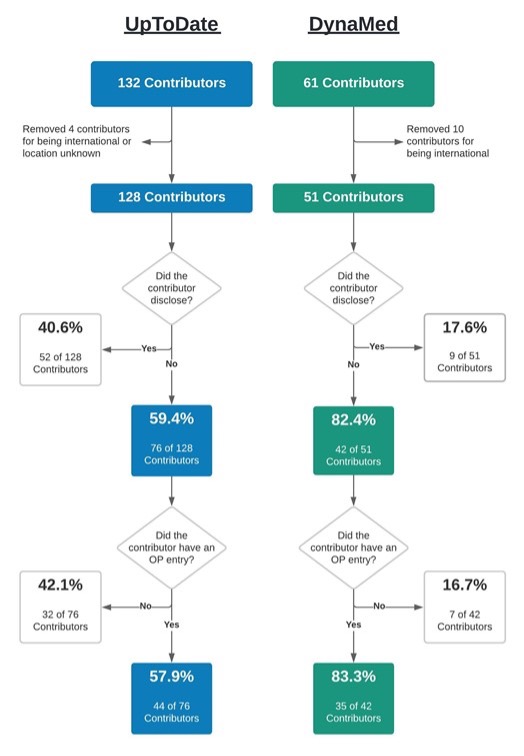
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.
SooYoung VanDeMar[/caption]
SooYoung VanDeMark, MBS
Geisinger Commonwealth School of Medicine
Scranton, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Health care providers utilize subscription-based, point-of-care databases such as DynaMed and UpToDate to provide clinical care guidance and remain current on the latest evidence-based findings. Both of these websites maintain this content through a cadre of physician contributors who write and edit articles for these sites. These physician contributors are required to self-report any conflicts of interest (COI) as outlined by the respective policies on each website. However, prior COI research into similarly self-regulated areas, such as medical and pharmacology textbooks, and clinical practice guidelines, has found both appreciable potential COI and inconsistencies between self-reported and industry mandated disclosures (1-3).
This study (4) explored the accuracy of physician contributors to DynaMed and UpToDate by comparing their self-reported disclosure status with the financial remunerations they received from the healthcare industry (e.g., pharmaceutical companies) as reported to the U.S. Centers for Medicare and Medicaid Services’ Open Payments database. Physician contributors who reported “nothing to disclose” on their respective article topic but had an entry on Open Payments for having received money from industry, were classified as discordant and, thus, as having the potential for a COI. Additionally, total remuneration, gender, and payment category were investigated more in depth for each database.

 Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).
Dr. Soriano[/caption]
Victoria Soriano PhD
Research Assistant/Officer, Population Allergy
University of Melbourne
MedicalResearch.com: What is the background for this study?
Response: Peanut allergy is one of the most common childhood food allergies, and children rarely grow out of it. The only proven way to prevent peanut allergy is to give infants age-appropriate peanut products in the first year of life.
We previously showed there was a dramatic increase in peanut introduction from 2007-11 to 2018-19, following changes to infant feeding guidelines. We wanted to know if earlier peanut introduction would reduce peanut allergy in the general population (in Melbourne, Australia).

 Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .
Dr. Altan-Bonnet[/caption]
Nihal Altan-Bonnet, Ph.D.
Chief of the Laboratory of Host-Pathogen Dynamics
NHLBI
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Enteric viruses such as norovirus, rotavirus and astrovirus are responsible for nearly 1.5 billion global infections per year resulting in gastrointestinal illnesses and sometimes leading to death in the very young, in the elderly and in the immunocompromised. These viruses have been thought to traditionally infect and replicate only in the intestines, then shed into feces and transmit to others via the oral-fecal route (e.g. through ingestion of fecal contaminated food items).
Our findings reported in Nature, using animal models of norovirus, rotavirus and astrovirus infection, challenge this traditional view and reveal that these viruses can also replicate robustly in salivary glands, be shed into saliva in large quantities and transmit through saliva to other animals.
In particular we also show infected infants can transmit these viruses to their mothers mammary glands via suckling and this leads to both an infection in their mothers mammary glands but also a rapid immune response by the mother resulting in a surge in her milk antibodies. These milk antibodies may play a role in fighting the infection in their infants .













 Dr. Duffy[/caption]
Jeanne Duffy, MBA, PhD
Associate Professor of Medicine
Division of Sleep and Circadian Disorders
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: Aging is associated with changes in sleep timing, quality and duration, and even older adults without chronic medical problems have shorter and more disrupted sleep than young adults. Many prescription sleep aids increase the risk of nighttime falls, have
adverse effects on next‐day cognition, and are associated with increased mortality, and so are not recommended for long-term use in older adults. In previous studies, we and others have shown that melatonin, a hormone secreted at night, increases sleep duration in young adults but only when administered during the day when endogenous melatonin levels are low. We wanted to explore whether melatonin could improve the sleep of healthy adults and whether, like young adults, its impact depends on when during the day the person is trying to sleep.
Dr. Duffy[/caption]
Jeanne Duffy, MBA, PhD
Associate Professor of Medicine
Division of Sleep and Circadian Disorders
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: Aging is associated with changes in sleep timing, quality and duration, and even older adults without chronic medical problems have shorter and more disrupted sleep than young adults. Many prescription sleep aids increase the risk of nighttime falls, have
adverse effects on next‐day cognition, and are associated with increased mortality, and so are not recommended for long-term use in older adults. In previous studies, we and others have shown that melatonin, a hormone secreted at night, increases sleep duration in young adults but only when administered during the day when endogenous melatonin levels are low. We wanted to explore whether melatonin could improve the sleep of healthy adults and whether, like young adults, its impact depends on when during the day the person is trying to sleep.




