Accidents & Violence, Author Interviews, Cannabis / 28.10.2018
Should You Get a Ticket For Driving Stoned?
MedicalResearch.com Interview with:
[caption id="attachment_45541" align="alignleft" width="200"] Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.
Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.
 Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.
Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door. 



 Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.
Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.



 Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.
Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.

 Sean C. Rose, MD
Pediatric sports neurologist and co-director
Complex Concussion Clinic
Nationwide Children’s Hospital
Assistant professor of Pediatrics
The Ohio State University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The link between sub-concussive head impacts and declines in neurocognitive function has been reported by some studies, yet refuted by others. There is very little evidence that has been collected in children as they are sustaining these head impacts.
We initiated a multi-year study of youth football players to provide a more in-depth look at the question. We measured head impacts using helmet sensors during the 2016 football season. 112 players age 9-18 completed a battery of neurocognitive tests before and after the football season.
We found that neither the total burden of head impacts nor the intensity of individual impacts were associated with changes in testing performance from pre to post-season.
Sean C. Rose, MD
Pediatric sports neurologist and co-director
Complex Concussion Clinic
Nationwide Children’s Hospital
Assistant professor of Pediatrics
The Ohio State University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The link between sub-concussive head impacts and declines in neurocognitive function has been reported by some studies, yet refuted by others. There is very little evidence that has been collected in children as they are sustaining these head impacts.
We initiated a multi-year study of youth football players to provide a more in-depth look at the question. We measured head impacts using helmet sensors during the 2016 football season. 112 players age 9-18 completed a battery of neurocognitive tests before and after the football season.
We found that neither the total burden of head impacts nor the intensity of individual impacts were associated with changes in testing performance from pre to post-season.



 Jennifer Woo Baidal, MD, MPH
Assistant Professor of Pediatrics
Director of Pediatric Weight Management,
Division of Pediatric Gastroenterology, Hepatology, and Nutrition,
Columbia University Medical Center &
New York-Presbyterian Morgan Stanley Children’s Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Childhood obesity prevalence is historically high, with most incident obesity among children occurring before age 5 years. Racial/ethnic and socioeconomic disparities in childhood obesity are already apparent by the first years of life. Latino/Hispanic children in low-income families are at-risk for obesity. Thus, understanding potentially effective ways to prevent childhood obesity, particularly in vulnerable populations, should focus on early life.
Sugar-sweetened beverage (SSB) consumption is a modifiable risk factor for obesity and is linked to other adverse health outcomes. Maternal SSB consumption in pregnancy and infant sugar-sweetened beverage consumption in the first year of life are linked to later childhood obesity.
We sought to describe beverage consumption in a modern cross-sectional cohort of 394 low-income, Latino families, and to examine the relationship of parental attitudes toward sugar-sweetened beverages with parental and infant SSB consumption.
Jennifer Woo Baidal, MD, MPH
Assistant Professor of Pediatrics
Director of Pediatric Weight Management,
Division of Pediatric Gastroenterology, Hepatology, and Nutrition,
Columbia University Medical Center &
New York-Presbyterian Morgan Stanley Children’s Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Childhood obesity prevalence is historically high, with most incident obesity among children occurring before age 5 years. Racial/ethnic and socioeconomic disparities in childhood obesity are already apparent by the first years of life. Latino/Hispanic children in low-income families are at-risk for obesity. Thus, understanding potentially effective ways to prevent childhood obesity, particularly in vulnerable populations, should focus on early life.
Sugar-sweetened beverage (SSB) consumption is a modifiable risk factor for obesity and is linked to other adverse health outcomes. Maternal SSB consumption in pregnancy and infant sugar-sweetened beverage consumption in the first year of life are linked to later childhood obesity.
We sought to describe beverage consumption in a modern cross-sectional cohort of 394 low-income, Latino families, and to examine the relationship of parental attitudes toward sugar-sweetened beverages with parental and infant SSB consumption.

 Dr. Rothbard[/caption]
MedicalResearch.com Interview with:
Jonathan Rothbard, MA, PhD
Steinman Lab Stanford Medicine
Co-founder
Dr. Rothbard[/caption]
MedicalResearch.com Interview with:
Jonathan Rothbard, MA, PhD
Steinman Lab Stanford Medicine
Co-founder 
 Dr. Smith[/caption]
Gary A. Smith, MD, DrPH
Director, Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: When residential fires happen at night while people are sleeping, deaths are more likely to occur. Smoke alarms are important for preventing these deaths, yet many young children don’t wake up to traditional high-pitch tone alarms. Children sleep longer and deeper than adults and require louder sounds to awaken than adults. For these reasons, children are less likely to awaken and escape a nighttime home fire.
Dr. Smith[/caption]
Gary A. Smith, MD, DrPH
Director, Center for Injury Research and Policy
Nationwide Children’s Hospital
Columbus, OH
MedicalResearch.com: What is the background for this study?
Response: When residential fires happen at night while people are sleeping, deaths are more likely to occur. Smoke alarms are important for preventing these deaths, yet many young children don’t wake up to traditional high-pitch tone alarms. Children sleep longer and deeper than adults and require louder sounds to awaken than adults. For these reasons, children are less likely to awaken and escape a nighttime home fire. 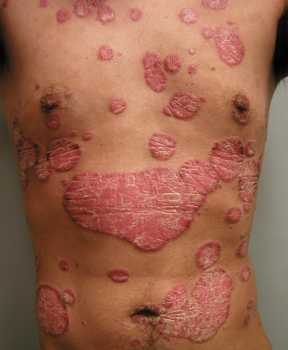
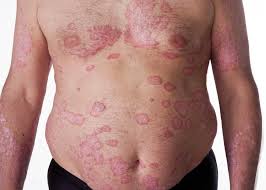 Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease.
Psoriasis[/caption]
Prof Ching-Chi Chi, MD, MMS, DPhil
Department of Dermatology
Chang Gung Memorial Hospital, Linkou
Guishan Dist, Taoyuan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies have shown common genotypes, clinical course, and immunological features shared by psoriasis and inflammatory bowel disease.
However, the relationship between psoriasis and inflammatory bowel disease was largely unclear.
In this study, we found when compared to the general population, psoriatic patients are more likely to have concomitant inflammatory bowel disease. 










 Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (
Dr. Shlipak[/caption]
Michael G. Shlipak, MD, MPH
Scientific Director , Kidney Health Research Collaborative (



 Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).
Dr. Janey Pratt, MD
Clinical Associate Professor, Surgery
Stanford University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In 2013 obesity became recognized as a disease. The rate of pediatric obesity continues to rise. Severe pediatric obesity is rising at a even faster rate than obesity in pediatrics. Despite this Metabolic and Bariatric Surgery (MBS) remains underutilized in the treatment of severe pediatric obesity. There is a significant amount of adult data and now pediatric data about effective treatments for severe obesity. These support the use of MBS as a primary treatment for severe obesity in children. (BMI > 120% of 95th percentile with a comorbidity or BMI > 140% of 95th percentile).

