Author Interviews, Gender Differences, Mental Health Research, OBGYNE, Psychological Science / 20.03.2019
How Do Men Express Grief After Pregnancy Loss?
MedicalResearch.com Interview with
[caption id="attachment_48025" align="alignleft" width="150"] Dr. Kranstuber Horstman[/caption]
Haley Kranstuber Horstman, Ph.D.
Department of Communication
University of Missouri
MedicalResearch.com: What is the background for this study?
Response: Miscarriage is a prevalent health concern, with one in five pregnancies ending in miscarriage, which is a pregnancy loss before 20 weeks’ gestation. Past research has shown that women who have miscarried often suffer mental health effects such as heightened grief, depression, loneliness, and suicidality.
Although much of the research on coping with miscarriage has focused on women’s health, many miscarriages occur within romantic relationships and affect the non-miscarrying partner as well. Women in heterosexual marriages report that their husband is often their top support-provider. Past research has shown that husbands suffer with mental health effects after a miscarriage, sometimes for even longer than their wives, but are not often supported in their grief because miscarriage is a “woman’s issue” and they feel uncomfortable talking about it.
Dr. Kranstuber Horstman[/caption]
Haley Kranstuber Horstman, Ph.D.
Department of Communication
University of Missouri
MedicalResearch.com: What is the background for this study?
Response: Miscarriage is a prevalent health concern, with one in five pregnancies ending in miscarriage, which is a pregnancy loss before 20 weeks’ gestation. Past research has shown that women who have miscarried often suffer mental health effects such as heightened grief, depression, loneliness, and suicidality.
Although much of the research on coping with miscarriage has focused on women’s health, many miscarriages occur within romantic relationships and affect the non-miscarrying partner as well. Women in heterosexual marriages report that their husband is often their top support-provider. Past research has shown that husbands suffer with mental health effects after a miscarriage, sometimes for even longer than their wives, but are not often supported in their grief because miscarriage is a “woman’s issue” and they feel uncomfortable talking about it.
 Dr. Kranstuber Horstman[/caption]
Haley Kranstuber Horstman, Ph.D.
Department of Communication
University of Missouri
MedicalResearch.com: What is the background for this study?
Response: Miscarriage is a prevalent health concern, with one in five pregnancies ending in miscarriage, which is a pregnancy loss before 20 weeks’ gestation. Past research has shown that women who have miscarried often suffer mental health effects such as heightened grief, depression, loneliness, and suicidality.
Although much of the research on coping with miscarriage has focused on women’s health, many miscarriages occur within romantic relationships and affect the non-miscarrying partner as well. Women in heterosexual marriages report that their husband is often their top support-provider. Past research has shown that husbands suffer with mental health effects after a miscarriage, sometimes for even longer than their wives, but are not often supported in their grief because miscarriage is a “woman’s issue” and they feel uncomfortable talking about it.
Dr. Kranstuber Horstman[/caption]
Haley Kranstuber Horstman, Ph.D.
Department of Communication
University of Missouri
MedicalResearch.com: What is the background for this study?
Response: Miscarriage is a prevalent health concern, with one in five pregnancies ending in miscarriage, which is a pregnancy loss before 20 weeks’ gestation. Past research has shown that women who have miscarried often suffer mental health effects such as heightened grief, depression, loneliness, and suicidality.
Although much of the research on coping with miscarriage has focused on women’s health, many miscarriages occur within romantic relationships and affect the non-miscarrying partner as well. Women in heterosexual marriages report that their husband is often their top support-provider. Past research has shown that husbands suffer with mental health effects after a miscarriage, sometimes for even longer than their wives, but are not often supported in their grief because miscarriage is a “woman’s issue” and they feel uncomfortable talking about it.



 Dr. Mikkola[/caption]
Tomi Mikkola MD
Associate Professor
Helsinki University Hospital
Department of Obstetrics and Gynecology
Helsinki, Finland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In Finland we have perhaps the most comprehensive and reliable medical registers in the world. Thus, with my research group I have conducted various large studies evaluating association of postmenopausal hormone therapy use and various major diseases (see e.g. the references in the B;MJ paper). There has been various smaller studies indicating that hormone therapy might be protective for all kinds of dementias, also Alzheimer’s disease.
However, we have quite recently shown that hormone therapy seems to lower the mortality risk of vascular dementia but not Alzheimer’s disease (Mikkola TS et al. J Clin Endocrinol Metab 2017;102:870-7). Now in this upcoming BMJ-paper we report in a very large case-control study (83 688 women with Alzheimer’s disease and same number of control women without the disease) that systemic hormone therapy was associated with a 9-17% increased risk of Alzheimer’s disease.
Furthermore, this risk increase is particularly in women using hormone therapy long, for more than 10 years. This was somewhat surprising finding, but it underlines the fact that mechanisms behind Alzheimer’s disease are likely quite different than in vascular dementia, where the risk factors are similar as in cardiovascular disease. We have also shown how hormone therapy protects against cardiovascular disease, particularly in women who initiate hormone therapy soon after menopause.
Dr. Mikkola[/caption]
Tomi Mikkola MD
Associate Professor
Helsinki University Hospital
Department of Obstetrics and Gynecology
Helsinki, Finland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: In Finland we have perhaps the most comprehensive and reliable medical registers in the world. Thus, with my research group I have conducted various large studies evaluating association of postmenopausal hormone therapy use and various major diseases (see e.g. the references in the B;MJ paper). There has been various smaller studies indicating that hormone therapy might be protective for all kinds of dementias, also Alzheimer’s disease.
However, we have quite recently shown that hormone therapy seems to lower the mortality risk of vascular dementia but not Alzheimer’s disease (Mikkola TS et al. J Clin Endocrinol Metab 2017;102:870-7). Now in this upcoming BMJ-paper we report in a very large case-control study (83 688 women with Alzheimer’s disease and same number of control women without the disease) that systemic hormone therapy was associated with a 9-17% increased risk of Alzheimer’s disease.
Furthermore, this risk increase is particularly in women using hormone therapy long, for more than 10 years. This was somewhat surprising finding, but it underlines the fact that mechanisms behind Alzheimer’s disease are likely quite different than in vascular dementia, where the risk factors are similar as in cardiovascular disease. We have also shown how hormone therapy protects against cardiovascular disease, particularly in women who initiate hormone therapy soon after menopause.






 Dr. Kuan-Pin Su[/caption]
Kuan-Pin Su, MD, PhD
China Medical University
Taichung, Taiwan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Delirium, also known as acute confusional state, is a serious disturbance in mental abilities that results in confused thinking and reduced awareness of the environment. Delirium can often be traced to one or more contributing factors, such as a severe or chronic illness, changes in metabolic balance (such as low sodium), medication, infection, surgery, or alcohol or drug intoxication or withdrawal. It’s critically important to identify and treat delirium because some of the contributing factors could be life-threatening. However, there is no sufficient evidence for choice of medication to treat or prevent the symptoms of delirium.
A recent paper, Association of Delirium Response and Safety of Pharmacological Interventions for the Management and Prevention of Delirium A Network Meta-analysis, published in JAMA Psychiatry provides important findings of this missing piece in that important clinical uncertainty. The leading author, Professor Kuan-Pin Su, at the China Medical University in Taichung, Taiwan, concludes the main finding about treatment/prevention of delirium: “In this report, we found that the combination of haloperidol and lorazepam demonstrated the best option for treatment of delirium, while ramelteon for prevention against delirium.
Dr. Kuan-Pin Su[/caption]
Kuan-Pin Su, MD, PhD
China Medical University
Taichung, Taiwan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Delirium, also known as acute confusional state, is a serious disturbance in mental abilities that results in confused thinking and reduced awareness of the environment. Delirium can often be traced to one or more contributing factors, such as a severe or chronic illness, changes in metabolic balance (such as low sodium), medication, infection, surgery, or alcohol or drug intoxication or withdrawal. It’s critically important to identify and treat delirium because some of the contributing factors could be life-threatening. However, there is no sufficient evidence for choice of medication to treat or prevent the symptoms of delirium.
A recent paper, Association of Delirium Response and Safety of Pharmacological Interventions for the Management and Prevention of Delirium A Network Meta-analysis, published in JAMA Psychiatry provides important findings of this missing piece in that important clinical uncertainty. The leading author, Professor Kuan-Pin Su, at the China Medical University in Taichung, Taiwan, concludes the main finding about treatment/prevention of delirium: “In this report, we found that the combination of haloperidol and lorazepam demonstrated the best option for treatment of delirium, while ramelteon for prevention against delirium. 












 Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
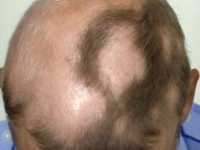
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.
Dr. Vallerand[/caption]
Isabelle Vallerand, PhD
Epidemiologist, MD Student
Department of Community Health Sciences
Cumming School of Medicine
University of Calgary
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: It is well known that patients with alopecia areata, a form of autoimmune hair loss, are at a higher risk of suffering from depression than the general population. But in practice, we often hear patients tell us that they believe their hair loss developed as a result of stress or problems with mental health – certainly the phrase “so stressed your hair is falling out” is something most people have heard of. Despite this, there has actually been very little research investigating the role that mental health may have on development of alopecia areata.
Interestingly, depression has recently been associated with increased systemic inflammatory markers, so there is biologic plausibility that depression could increase the risk of alopecia areata. Our group was interested in addressing this question, and used a large population-level health records database with up to 26 years of follow-up to study it. We ultimately found that not only does depression increase one’s risk of alopecia areata, but that it increases their risk by nearly 90% compared to people who have never had depression. We also found that using antidepressants can significantly decrease the risk of developing alopecia areata in patients with depression. So there appears to be an important link between mental health and development of hair loss from alopecia areata.







