Link Between Thyroid Function Genetics and Atrial Fibrillation Grows
 Dr. Salem[/caption]
Joe-Elie Salem, MD, PhD
Associate Professor - MCU-PH, Sorbonne Université - INSERM - CIC, Clinical Pharmacology, Cardio-oncology, APHP, La Pitié-Salpêtrière, Paris, France
Adjunct Associate Professor, Vanderbilt University Medical Center, Cardio-oncology
Clinical Pharmacology, Nashville, TN
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A study by researchers at Vanderbilt University Medical Center has strengthened the link between thyroid function and atrial fibrillation (AF), an irregular heart rhythm that increases the risk of stroke and other heart-related complications.
They phenome-wide association study scanned the medical records of more than 37,000 people for an association between genetically determined variation in thyroid stimulating hormone levels (a measure of thyroid function) and AF risk.
Previous observational studies have found that subclinical hyperthyroidism, an overactive thyroid which does not meet the clinical threshold for diagnosis or treatment, nevertheless can increase the risk of atrial fibrillation. But whether to treat subclinical hypo- or hyperthyroidism to reduce AF risk remains a matter of debate in the medical community.
Dr. Salem[/caption]
Joe-Elie Salem, MD, PhD
Associate Professor - MCU-PH, Sorbonne Université - INSERM - CIC, Clinical Pharmacology, Cardio-oncology, APHP, La Pitié-Salpêtrière, Paris, France
Adjunct Associate Professor, Vanderbilt University Medical Center, Cardio-oncology
Clinical Pharmacology, Nashville, TN
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: A study by researchers at Vanderbilt University Medical Center has strengthened the link between thyroid function and atrial fibrillation (AF), an irregular heart rhythm that increases the risk of stroke and other heart-related complications.
They phenome-wide association study scanned the medical records of more than 37,000 people for an association between genetically determined variation in thyroid stimulating hormone levels (a measure of thyroid function) and AF risk.
Previous observational studies have found that subclinical hyperthyroidism, an overactive thyroid which does not meet the clinical threshold for diagnosis or treatment, nevertheless can increase the risk of atrial fibrillation. But whether to treat subclinical hypo- or hyperthyroidism to reduce AF risk remains a matter of debate in the medical community. Low Sugar Diet Reduced Liver Fat and Inflammation
 Dr. Vos[/caption]
Miriam Vos, MD, MSPH
Associate Professor of Pediatrics and Director
Pediatric Fatty Liver Program
Emory and Children’s Healthcare of Atlanta
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Fatty liver disease has quickly become a common problem in children and adolescents, affecting an estimated 7 million children in the U.S. This study resulted from our previous research demonstrating that fructose increases cardiometabolic risk factors in children with NAFLD in addition to other research that had demonstrated associations between NAFLD and sugar.
Dr. Vos[/caption]
Miriam Vos, MD, MSPH
Associate Professor of Pediatrics and Director
Pediatric Fatty Liver Program
Emory and Children’s Healthcare of Atlanta
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Fatty liver disease has quickly become a common problem in children and adolescents, affecting an estimated 7 million children in the U.S. This study resulted from our previous research demonstrating that fructose increases cardiometabolic risk factors in children with NAFLD in addition to other research that had demonstrated associations between NAFLD and sugar. Changing Attitudes Toward Liver Transplant for Alcohol-Associated Liver Disease
Late post- liver transplantation survival after 5-years is 11% lower for alcohol-associated liver disease (vs. non-ALD). ...
Breast Cancer Survivors More Likely To Develop Subsequent Blood Cancers
 Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.
Dr. Marie Joelle Jabagi, PharmD, MPH
University of Paris Sud, Paris-Saclay University, Paris
Health Product Epidemiology Department
French National Agency for Medicines and Health Products Safety
Saint-Denis, France
MedicalResearch.com: What is the background for this study?
Response: Secondary hematologic malignant neoplasms that develop months or years after the diagnosis of breast cancer may be a consequence of genetic predisposition, environmental factors, previous cancer treatments or a combination of all those factors. These secondary malignant neoplasms are increasingly becoming a concern given that the population of breast cancer survivors is growing substantially. However, their frequency in real life has been poorly investigated to date.
The aims of our research were to estimate the frequency of various types of hematologic malignant neoplasm following a diagnosis of primary breast cancer among women aged 20 to 85 years in France during the past decade, and to compare it to the corresponding frequency in women of the French general population.
Tinnitus: Study of Adoptees Suggests Genetic Predisposition
 Dr. Cederroth[/caption]
Christopher R. Cederroth | Ph.D. Docent
Associate Professor
Experimental Audiology | Department of Physiology and Pharmacology
Karolinska Institutet
Sweden
MedicalResearch.com: What is the background for this study?
Response: Tinnitus is experienced is experienced by a large proportion of the population and affects more than 15% of the population worldwide (estimated 70 million people in Europe). However, for near 3% of the population, tinnitus becomes a chronic bothersome and incapacitating symptom. Severe tinnitus interferes with sleep, mood, and concentration and thus impacts life quality, ultimately leading to sick leave and disability pension. A high cost to society has been reported, and since the prevalence of tinnitus has been predicted to double in Europe by 2050, there is an important need for an effective treatment. And today there are none, with the exception of cognitive behavioral therapy, which helps coping with it but does not remove the tinnitus. There has been a number of innovative treatment approaches, but they are overall not successful and it is now agreed that it is likely because tinnitus is a heterogeneous condition – meaning that we cannot consider tinnitus a single entity but an ensemble of different forms or subtypes, which need to be defined.
Tinnitus has always been considered a condition influenced by environmental factors, but our initial studies suggested the opposite. Adoption studies are excellent in showing the influence of shared-environment effects and establish a genetic basis for a disease or a trait. It allows to test the transmission of a trait between the adoptee and their biological or their adoptive parent. Transmission via the biological parent is expected to be due to a heritable genetic effect, while transmission via the adoptive parent is associated with home-environment, the so-called shared-environmental effect. We used medical registry data to identify tinnitus patients and adoptees.
Dr. Cederroth[/caption]
Christopher R. Cederroth | Ph.D. Docent
Associate Professor
Experimental Audiology | Department of Physiology and Pharmacology
Karolinska Institutet
Sweden
MedicalResearch.com: What is the background for this study?
Response: Tinnitus is experienced is experienced by a large proportion of the population and affects more than 15% of the population worldwide (estimated 70 million people in Europe). However, for near 3% of the population, tinnitus becomes a chronic bothersome and incapacitating symptom. Severe tinnitus interferes with sleep, mood, and concentration and thus impacts life quality, ultimately leading to sick leave and disability pension. A high cost to society has been reported, and since the prevalence of tinnitus has been predicted to double in Europe by 2050, there is an important need for an effective treatment. And today there are none, with the exception of cognitive behavioral therapy, which helps coping with it but does not remove the tinnitus. There has been a number of innovative treatment approaches, but they are overall not successful and it is now agreed that it is likely because tinnitus is a heterogeneous condition – meaning that we cannot consider tinnitus a single entity but an ensemble of different forms or subtypes, which need to be defined.
Tinnitus has always been considered a condition influenced by environmental factors, but our initial studies suggested the opposite. Adoption studies are excellent in showing the influence of shared-environment effects and establish a genetic basis for a disease or a trait. It allows to test the transmission of a trait between the adoptee and their biological or their adoptive parent. Transmission via the biological parent is expected to be due to a heritable genetic effect, while transmission via the adoptive parent is associated with home-environment, the so-called shared-environmental effect. We used medical registry data to identify tinnitus patients and adoptees.
Comparison of Local Public Health Departments Highlights Social Inequities
 Dr. Wallace[/caption]
Megan Wallace, DrPH
Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Baltimore, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Local health departments are often evaluated on a nationwide or statewide basis, however, given diversity among counties that exists even at the state level, we felt there might be a better way to group health departments for evaluation.
In this study, we created county-level clusters using local characteristics most associated with the outcomes of interest, which were smoking, motor vehicle crash deaths, and obesity. We then compared county-level percentile rankings for the outcomes within sociodemographic peer clusters vs nationwide rankings. We identified 8 groups of counties with similar local characteristics.
Percentile ranks for the outcomes of interest often differed when counties were compared within their peer groups in comparison with a nationwide scale.
Dr. Wallace[/caption]
Megan Wallace, DrPH
Department of Epidemiology
Johns Hopkins Bloomberg School of Public Health
Baltimore, Maryland
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Local health departments are often evaluated on a nationwide or statewide basis, however, given diversity among counties that exists even at the state level, we felt there might be a better way to group health departments for evaluation.
In this study, we created county-level clusters using local characteristics most associated with the outcomes of interest, which were smoking, motor vehicle crash deaths, and obesity. We then compared county-level percentile rankings for the outcomes within sociodemographic peer clusters vs nationwide rankings. We identified 8 groups of counties with similar local characteristics.
Percentile ranks for the outcomes of interest often differed when counties were compared within their peer groups in comparison with a nationwide scale. Does Treatment with Vitamin D Reduce Cardiovascular Risk in Hemodialysis Patients?
MedicalResearch.comInterview with:

Tetsuo Shoji, MD, PhD.
Department of Vascular Medicine
Osaka City University Graduate School of Medicine
Osaka Japan
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Vitamin D is known to be associated with health and disease of various organs such as bone, heart, brain, and others. Vitamin D is activated by the liver and kidneys to a hormone called 1,25-dihydroxyvitamin D which binds to vitamin D receptor in cells to exert its functions.
Vitamin D activation is severely impaired in patients with kidney disease requiring hemodialysis therapy, leading to mineral and bone disorder(MBD). Therefore, active form of vitamin D is one of the standard choices of treatment for MBD caused by kidney function loss.
Previous observational cohort studies showed that the use of active vitamin D in hemodialysis patients was associated with lower likelihood of all-cause death, cardiovascular death, and incident cardiovascular disease.Potentially cardio-protective effects of active vitamin D were shown by basic studies using cultured cells and animal models. Then, many nephrologists began to believe that active vitamin D is a “longevity hormone” or a “panacea” for kidney patients requiring dialysis therapy, although there was no evidence by randomized clinical trials.
To show evidence for it, we conducted a randomized clinical trial namedJ-DAVID in which 976 hemodialysis patients were randomly assigned to treatment with oral alfacalcidol or treatment without active vitamin D, and they were followed-up for new cardiovascular events during the four-year period. The risk of cardiovascular events was not significantly different between the two groups. The risk of all-cause death was not significantly different either.
To our surprise, the risk of cardiovascular event tended to be higher in the patients who continued treatment with active vitamin D than those who continued non-use of active vitamin D, although the difference was not statistically significant.
MedicalResearch.comInterview with:
Jac Dinnes PhD, MSc, MA, PGDip
Senior Researcher
Test Evaluation Research Group
Institute of Applied Health Research
University of Birmingham
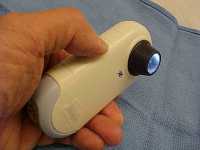
MedicalResearch.com: What is thebackground for this study? Would you briefly explain the benefits of dermoscopy?
Response: This systematic review was one of a series of Cochrane Reviews of studies evaluating different tests for diagnosing skin cancer. Within creasing rates of skin cancer and an increasing number of more specialised tests becoming available in both primary care and in specialist settings, a thorough review of all available evidence was timely.
The diagnosis of melanoma and other skin cancers fundamentally relies on clinical examination, including history taking, and visual inspection of the concerning skin lesion (mole or patch of skin) and surrounding skin (and other lesions). A dermatoscope is a handheld device using visible light (such as from incandescent or LED bulbs), that allows more detailed examination of the skin compared to examination by the naked eye alone.
Knowing the diagnostic accuracy of dermoscopy added to visual inspection alone, across a range of observers and settings, is critical to understanding its contribution for the diagnosis of melanoma and to future understanding of the potential role of the growing number of other high-resolution image analysis techniques.
Using of Big Data to Estimate Prevalence of Defective DNA Repair Variants in the US
MedicalResearch.com Interview with:

Kenneth H. Kraemer,M.D.
Chief DNA Repair Section
Laboratory of Cancer Biology and Genetics, Center for Cancer Research
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Response: At the National Cancer Institute, we have been examining patients with xeroderma pigmentosum (XP), a rare, recessively inherited, cancer-prone disease for many years. Therefore, with the increasing use of exome sequencing, we decided to see how closely"big data" corresponded with our clinical observations.
Chronic Kidney Disease Rate Rising Faster Than Other Noncommunicable Diseases
 Dr. Al-Aly[/caption]
Dr. Ziyad Al-Aly, MD
Associate Chief of Staff for Research and Education
Veterans Affairs St. Louis Health Care System
Institute for Public Health
Washington University, St. Louis MO
MedicalResearch.com: What is the background for this study?
Response: A lot has changed in the US over the past 15 years including aging, population growth, and increased exposure to risk factors such as obesity, elevated blood pressure, etc. With all of these changes, we wondered, how did the burden of kidney disease change in the United States over the past 15 years.
Dr. Al-Aly[/caption]
Dr. Ziyad Al-Aly, MD
Associate Chief of Staff for Research and Education
Veterans Affairs St. Louis Health Care System
Institute for Public Health
Washington University, St. Louis MO
MedicalResearch.com: What is the background for this study?
Response: A lot has changed in the US over the past 15 years including aging, population growth, and increased exposure to risk factors such as obesity, elevated blood pressure, etc. With all of these changes, we wondered, how did the burden of kidney disease change in the United States over the past 15 years.
What are the Patient Preferences that Determine Chose of Bariatric Surgery?
 Dr. Rozier[/caption]
Michael Rozier, S.J., Ph.D.
Assistant Professor, Health Management and Policy
College for Public Health and Social Justice
St. Louis University
MedicalResearch.com: What is the background for this study?
Response: Patients considering surgery for weight loss have several options, which differ in significant ways, such as expected weight loss, risk of complication, modification of diet, effect on other medical conditions, and more. Previous studies have asked patients why they chose one procedure over another.
Instead, we quantified the relative importance of the key characteristics of surgical options. Using a discrete choice experiment, potential patients were given profiles of two weight loss options. They were asked to select one profile based on key characteristics such as out-of-pocket costs, total weight loss, risk of complication, and five other factors.
Dr. Rozier[/caption]
Michael Rozier, S.J., Ph.D.
Assistant Professor, Health Management and Policy
College for Public Health and Social Justice
St. Louis University
MedicalResearch.com: What is the background for this study?
Response: Patients considering surgery for weight loss have several options, which differ in significant ways, such as expected weight loss, risk of complication, modification of diet, effect on other medical conditions, and more. Previous studies have asked patients why they chose one procedure over another.
Instead, we quantified the relative importance of the key characteristics of surgical options. Using a discrete choice experiment, potential patients were given profiles of two weight loss options. They were asked to select one profile based on key characteristics such as out-of-pocket costs, total weight loss, risk of complication, and five other factors.
Stroke: Cerebellar Stimulation Improved Motor Function
 Dr. Koch[/caption]
Giacomo Koch, MD, PhD
Laboratorio di Neurologia Clinica e Comportamentale
Fondazione S. Lucia I.R.C.C.S.
Italy
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We show in this paper that non invasive stimulation of the cerebellum in patients with stroke is able to improve motor functions.
In particular we found that after three weeks of repetitive TMS of the intact cerebellum patients with hemiparesis due to stroke in the cerebral hemisphere remarkably improved their ability to walk and keep their balance, thus highly reducing the risk of fall.
Dr. Koch[/caption]
Giacomo Koch, MD, PhD
Laboratorio di Neurologia Clinica e Comportamentale
Fondazione S. Lucia I.R.C.C.S.
Italy
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: We show in this paper that non invasive stimulation of the cerebellum in patients with stroke is able to improve motor functions.
In particular we found that after three weeks of repetitive TMS of the intact cerebellum patients with hemiparesis due to stroke in the cerebral hemisphere remarkably improved their ability to walk and keep their balance, thus highly reducing the risk of fall.
Serious Mental Illness Raises Risk of 30 Day Readmission
 Dr. Germack[/caption]
Hayley D. Germack PHD, MHS, RN
Assistant Professor, School of Nursing
University of Pittsburgh
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As nurse scientists, we repeatedly witness the impact of having a serious mental illness (i.e. schizophrenia, bipolar disorder, and major depression disorder) on patients’ inpatient and discharge experience. As health services researchers, we know how to make use of large secondary data to illuminate our firsthand observations.
In 2016, Dr. Hanrahan and colleagues (https://www.sciencedirect.com/science/article/pii/S0163834316301347) published findings of a secondary data analysis from a large urban hospital system that found 1.5 to 2.4 greater odds of readmission for patients with an serious mental illness diagnosis compared to those without. We decided to make use of the AHRQ’s HCUP National Readmissions Database to illuminate the magnitude of this relationship using nationally representative data. We found that even after controlling for clinical, demographic, and hospital factors, that patients with SMI have nearly 2 times greater odds of 30-day readmission.
Dr. Germack[/caption]
Hayley D. Germack PHD, MHS, RN
Assistant Professor, School of Nursing
University of Pittsburgh
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As nurse scientists, we repeatedly witness the impact of having a serious mental illness (i.e. schizophrenia, bipolar disorder, and major depression disorder) on patients’ inpatient and discharge experience. As health services researchers, we know how to make use of large secondary data to illuminate our firsthand observations.
In 2016, Dr. Hanrahan and colleagues (https://www.sciencedirect.com/science/article/pii/S0163834316301347) published findings of a secondary data analysis from a large urban hospital system that found 1.5 to 2.4 greater odds of readmission for patients with an serious mental illness diagnosis compared to those without. We decided to make use of the AHRQ’s HCUP National Readmissions Database to illuminate the magnitude of this relationship using nationally representative data. We found that even after controlling for clinical, demographic, and hospital factors, that patients with SMI have nearly 2 times greater odds of 30-day readmission. Alcohol Misuse Raises Risk of Unsafe Firearm Storage
 Erin Morgan
PhD Student | Department of Epidemiology
University of Washington
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Going into this study we were interested in looking at youth exposure to unsafely stored firearms. Unsafely stored firearms in the household, especially those that are stored unlocked, are a known risk factor for adolescent suicide. We were also interested in looking into a population of children and teens who are at particularly heightened risk for suicide and unintentional injury—those living with an adult who misuses alcohol.
Overall, we found that about 30% of those under the age of 18 live in a firearm owning home and among those youth, around 55% lived with a firearm stored in a way other than locked and unloaded. Among those in firearm owning household, we also found that when compared to youth living with a survey respondent that did not report alcohol misuse, those living with an adult that did misuse alcohol were 20% more likely to reside in a home where the firearm was stored unsafely; children were 27% more likely to live in a home reporting unlocked storage, specifically.
Erin Morgan
PhD Student | Department of Epidemiology
University of Washington
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Going into this study we were interested in looking at youth exposure to unsafely stored firearms. Unsafely stored firearms in the household, especially those that are stored unlocked, are a known risk factor for adolescent suicide. We were also interested in looking into a population of children and teens who are at particularly heightened risk for suicide and unintentional injury—those living with an adult who misuses alcohol.
Overall, we found that about 30% of those under the age of 18 live in a firearm owning home and among those youth, around 55% lived with a firearm stored in a way other than locked and unloaded. Among those in firearm owning household, we also found that when compared to youth living with a survey respondent that did not report alcohol misuse, those living with an adult that did misuse alcohol were 20% more likely to reside in a home where the firearm was stored unsafely; children were 27% more likely to live in a home reporting unlocked storage, specifically.Cost-effectiveness of Humanitarian Pediatric Cardiac Surgery
 Dr. Cardarelli[/caption]
Marcelo G. Cardarelli, MD
Inova Children’s Hospita
Fairfax, Falls Church, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Global Humanitarian Medical efforts consume a large amount of resources (nearly $38B in 2016) and donors (Countries, International organizations, WHO, Individuals) make the decisions as to where their funds should be allocated based on cost-effectiveness studies. Most resources go to prevent/treat infectious diseases, sanitation efforts and maternal/child care issues. An insignificant amount of resources is directed to satisfy the surgical needs of the populations in low and middle income countries (LMICs).
The idea behind our project was to find out if it was cost-effective to perform a tertiary surgical specialty (pediatric cardiac surgery) in this context and the answer (at $171 per DALY averted) was an overwhelming yes!
But most importantly, we believe, as many others do, that judging the cost/effectiveness of an intervention in order to decide resources allocation is valid for diseases that can be prevented, but not relevant when it comes to surgical problems that are not preventable.
Instead, we propose the use of another measure of effectiveness, what we call "The Humanitarian Footprint".
The Humanitarian Footprint represents the long term benefits, as measured by changes in the life expectancy, extra years of schooling and potential lifetime earnings of patients treated surgically during humanitarian interventions.
To our surprise and based on the results, the effects on society of at least this particular surgical intervention were greater than we expected. We suspect this measure can be used in many other surgical humanitarian interventions as well.
Dr. Cardarelli[/caption]
Marcelo G. Cardarelli, MD
Inova Children’s Hospita
Fairfax, Falls Church, Virginia
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Global Humanitarian Medical efforts consume a large amount of resources (nearly $38B in 2016) and donors (Countries, International organizations, WHO, Individuals) make the decisions as to where their funds should be allocated based on cost-effectiveness studies. Most resources go to prevent/treat infectious diseases, sanitation efforts and maternal/child care issues. An insignificant amount of resources is directed to satisfy the surgical needs of the populations in low and middle income countries (LMICs).
The idea behind our project was to find out if it was cost-effective to perform a tertiary surgical specialty (pediatric cardiac surgery) in this context and the answer (at $171 per DALY averted) was an overwhelming yes!
But most importantly, we believe, as many others do, that judging the cost/effectiveness of an intervention in order to decide resources allocation is valid for diseases that can be prevented, but not relevant when it comes to surgical problems that are not preventable.
Instead, we propose the use of another measure of effectiveness, what we call "The Humanitarian Footprint".
The Humanitarian Footprint represents the long term benefits, as measured by changes in the life expectancy, extra years of schooling and potential lifetime earnings of patients treated surgically during humanitarian interventions.
To our surprise and based on the results, the effects on society of at least this particular surgical intervention were greater than we expected. We suspect this measure can be used in many other surgical humanitarian interventions as well. Testosterone Treatment May Reduce Depression in Men
 Dr. Walther[/caption]
Dr. Andreas Walther PhD
Department of Biological Psychology, Technische Universität Dresden, Dresden, Germany
Department of Clinical Psychology and Psychotherapy, University of Zurich,
Zurich, Switzerland
Task Force on Men’s Mental Health of the World Federation of the Societies of Biological Psychiatry
MedicalResearch.com: What is the background for this study?
Response: The study situation with regard to endogenous testosterone level and depressive symptoms in men is currently very mixed. There are studies that show no association, but other studies show that low testosterone levels are associated with increased depressive symptoms. That is why several studies have tried to administer testosterone in men to treat depressive symptomatology among other conditions (e.g. erectile dysfunction, cognitive decline).
However, no clear conclusions could be drawn from the studies to date, as some studies reported positive results, while others did not show any effects. Likewise, some studies showed better results in certain subgroups of men such as dysthymic men, treatment resistant, men with low testosterone, which raised the question of relevant moderators.
Dr. Walther[/caption]
Dr. Andreas Walther PhD
Department of Biological Psychology, Technische Universität Dresden, Dresden, Germany
Department of Clinical Psychology and Psychotherapy, University of Zurich,
Zurich, Switzerland
Task Force on Men’s Mental Health of the World Federation of the Societies of Biological Psychiatry
MedicalResearch.com: What is the background for this study?
Response: The study situation with regard to endogenous testosterone level and depressive symptoms in men is currently very mixed. There are studies that show no association, but other studies show that low testosterone levels are associated with increased depressive symptoms. That is why several studies have tried to administer testosterone in men to treat depressive symptomatology among other conditions (e.g. erectile dysfunction, cognitive decline).
However, no clear conclusions could be drawn from the studies to date, as some studies reported positive results, while others did not show any effects. Likewise, some studies showed better results in certain subgroups of men such as dysthymic men, treatment resistant, men with low testosterone, which raised the question of relevant moderators.
Advanced Prostate Cancer: Risk of Mortality with Surgery vs Radiotherapy
 Dr. D'Amico[/caption]
Anthony Victor D'Amico, MD, PhD
Professor and Chief,
Genitourinary Radiation Oncology
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: This study investigated whether surgery followed by the use of adjuvant low dose radiation and short course hormonal therapy as compared to high dose radiation and hormonal therapy could provide an equivalent low risk of death from prostate cancer amongst men presenting with aggressive and not infrequently fatal Gleason score 9 or 10 prostate cancer.
It has been shown previously (https://jamanetwork.com/journals/jama/fullarticle/2673969) and validated in the current study that surgery alone in such cases leads to a more then 2.5-fold increase in the risk of death from prostate cancer as compared to high dose radiation and hormonal therapy.
Dr. D'Amico[/caption]
Anthony Victor D'Amico, MD, PhD
Professor and Chief,
Genitourinary Radiation Oncology
Harvard Medical School
MedicalResearch.com: What is the background for this study?
Response: This study investigated whether surgery followed by the use of adjuvant low dose radiation and short course hormonal therapy as compared to high dose radiation and hormonal therapy could provide an equivalent low risk of death from prostate cancer amongst men presenting with aggressive and not infrequently fatal Gleason score 9 or 10 prostate cancer.
It has been shown previously (https://jamanetwork.com/journals/jama/fullarticle/2673969) and validated in the current study that surgery alone in such cases leads to a more then 2.5-fold increase in the risk of death from prostate cancer as compared to high dose radiation and hormonal therapy. More Pharmacies Willing To Dispense Naloxone Without Prescription
 Clinical Assistant Professor
College of Pharmacy, The University of Texas at Austin
Adjoint Assistant Professor
School of Medicine, University of Texas Health Science Center at San Antonio
Ambulatory Care Pharmacist
Southeast Clinic, University Health System
UT Health Science Center at San Antonio
Pharmacotherapy Education and Research Center
San Antonio, TX 78229
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies in Indiana and New York City, and the similar study in California published alongside ours identified that, despite the fact that laws designed to increase naloxone access had been in place for 2-3 years, patients were still not able to obtain naloxone without first seeing a doctor in many pharmacies.
Our study showed contrasting results to the previous studies, with a much higher proportion of pharmacies stocking naloxone and stating their willingness to dispense without an outside prescription. Among the 2,317 Texas chain community pharmacies we contacted, 83.7% correctly informed our interviewers that they could obtain naloxone without having to get a prescription from their doctor before coming to the pharmacy. We also found that 76.4% of the pharmacies had at least one type of naloxone currently in stock.
Clinical Assistant Professor
College of Pharmacy, The University of Texas at Austin
Adjoint Assistant Professor
School of Medicine, University of Texas Health Science Center at San Antonio
Ambulatory Care Pharmacist
Southeast Clinic, University Health System
UT Health Science Center at San Antonio
Pharmacotherapy Education and Research Center
San Antonio, TX 78229
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Previous studies in Indiana and New York City, and the similar study in California published alongside ours identified that, despite the fact that laws designed to increase naloxone access had been in place for 2-3 years, patients were still not able to obtain naloxone without first seeing a doctor in many pharmacies.
Our study showed contrasting results to the previous studies, with a much higher proportion of pharmacies stocking naloxone and stating their willingness to dispense without an outside prescription. Among the 2,317 Texas chain community pharmacies we contacted, 83.7% correctly informed our interviewers that they could obtain naloxone without having to get a prescription from their doctor before coming to the pharmacy. We also found that 76.4% of the pharmacies had at least one type of naloxone currently in stock.Not All Pharmacies Have Naloxone for Opioid Overdose in Stock
 Dr. Puzantian[/caption]
Talia Puzantian, PharmD, BCPP
Associate Professor of Clinical Sciences,
School of Pharmacy and Health Sciences
Keck Graduate Institute
MedicalResearch.com: What is the background for this study?
Response: Naloxone has been used in hospitals and emergency rooms since the early 1970s. Distribution to laypersons began in the mid-1990s with harm reduction programs such as clean needle exchange programs providing it, along with education, to mostly heroin users. In the years between 1996-2014, 152,000 naloxone kits were distributed in this way with more than 26,000 overdoses reversed (https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6423a2.htm).
We have data showing that counties in which there was greater naloxone distribution among laypeople, there were lower opioid death rates (Walley AY et al BMJ 2013). However, not all opioid users at risk for overdose will interface with harm reduction programs, particularly prescription opioid users, hence more recent efforts to increase access to laypersons through pharmacists. Naloxone access laws have been enacted in all 50 states but very little has been published about how they’ve been adopted by pharmacists thus far. One small study (264 pharmacies) from Indiana (Meyerson BE et al Drug Alcohol Depend 2018) showed that 58.1% of pharmacies stocked naloxone, only 23.6% provided it without prescription, and that large chain pharmacies were more likely to do so.
Dr. Puzantian[/caption]
Talia Puzantian, PharmD, BCPP
Associate Professor of Clinical Sciences,
School of Pharmacy and Health Sciences
Keck Graduate Institute
MedicalResearch.com: What is the background for this study?
Response: Naloxone has been used in hospitals and emergency rooms since the early 1970s. Distribution to laypersons began in the mid-1990s with harm reduction programs such as clean needle exchange programs providing it, along with education, to mostly heroin users. In the years between 1996-2014, 152,000 naloxone kits were distributed in this way with more than 26,000 overdoses reversed (https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6423a2.htm).
We have data showing that counties in which there was greater naloxone distribution among laypeople, there were lower opioid death rates (Walley AY et al BMJ 2013). However, not all opioid users at risk for overdose will interface with harm reduction programs, particularly prescription opioid users, hence more recent efforts to increase access to laypersons through pharmacists. Naloxone access laws have been enacted in all 50 states but very little has been published about how they’ve been adopted by pharmacists thus far. One small study (264 pharmacies) from Indiana (Meyerson BE et al Drug Alcohol Depend 2018) showed that 58.1% of pharmacies stocked naloxone, only 23.6% provided it without prescription, and that large chain pharmacies were more likely to do so.
D-PRESCRIBE: Pharmacist-Led Intervention Can Reduce Inappropriate Medications in Older Adults
 Cara Tannenbaum, MD, MSc
Director | Directrice
Canadian Deprescribing Network
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The D-Prescribe trial was driven by the need to show that seniors can cut down on their medication in a safe and effective manner. Pharmacists intervened in a proactive way to flag patients who were on potentially risky meds such as sleeping pills, NSAIDs and glyburide and to inform them of the risks, using an educational brochure. Pharmacists also communicated with their physician using an evidence-based pharmaceutical opinion to spark conversations about deprescribing. As a result, 43% of patients succeeded in discontinuing at least one medication over the next 6 months.
Cara Tannenbaum, MD, MSc
Director | Directrice
Canadian Deprescribing Network
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The D-Prescribe trial was driven by the need to show that seniors can cut down on their medication in a safe and effective manner. Pharmacists intervened in a proactive way to flag patients who were on potentially risky meds such as sleeping pills, NSAIDs and glyburide and to inform them of the risks, using an educational brochure. Pharmacists also communicated with their physician using an evidence-based pharmaceutical opinion to spark conversations about deprescribing. As a result, 43% of patients succeeded in discontinuing at least one medication over the next 6 months.
Severe Maternal Morbidity Can Be Identified, and Sometimes Prevented
 Dr. Ray[/caption]
Joel Ray MD, MSc, FRCPC
Institute of Health Policy, Management and Evaluation
Faculty of Medicine
University of Toronto, Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many women who die within childbirth or soon thereafter experience rapid onset of morbidity/illness before succumbing. Thus, severe maternal morbidity (SMM) offers a detectable (or set of detectable) conditions that might be dealt with before they progress to a fatality. Even so, severe maternal morbidity alone can be non-fatal, but create disability for a new mother (e.g., a stroke), or prolong separation of mother and newborn.
So, we showed that, as the number of severe maternal morbidity indicators rises, so does the probability of maternal death. This relation was exponential in nature.
Dr. Ray[/caption]
Joel Ray MD, MSc, FRCPC
Institute of Health Policy, Management and Evaluation
Faculty of Medicine
University of Toronto, Toronto
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Many women who die within childbirth or soon thereafter experience rapid onset of morbidity/illness before succumbing. Thus, severe maternal morbidity (SMM) offers a detectable (or set of detectable) conditions that might be dealt with before they progress to a fatality. Even so, severe maternal morbidity alone can be non-fatal, but create disability for a new mother (e.g., a stroke), or prolong separation of mother and newborn.
So, we showed that, as the number of severe maternal morbidity indicators rises, so does the probability of maternal death. This relation was exponential in nature. Brain Metastases: Stereotactic Radiation vs Surgery Compared
 Dr. Weiss[/caption]
Dr. Stephanie E. Weiss MD FASTRO
Chief, Division of Neurologic Oncology
Associate Professor, Department of Radiation Oncology
Director, Radiation Oncology Residency and Fellowship Training Program
Fox Chase Cancer Center
Philadelphia, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Brain metastasis are the most common form of brain tumor.
Historically all patients received whole brain radiation as the primary therapy. Patients required neurosurgery to remove lesions if there was a question of diagnosis, what the diagnosis is and if there was a mass effect not relieved with steroids. Surgery was also indicated for patients with a single brain lesion because this offers a survival benefit over just receiving whole brain radiotherapy.
In 2003 a randomized trial proved that radiosurgery offers a similar benefit. So the question taxing patients and doctors at tumor boards since has been: which is better? If neurosurgery is superior, we are under-treating a lot of patients with radiosurgery. If radiosurgery is superior, we are subjecting a lot of patients to unnecessary brain surgery. Attempts to study this in a head-to-head randomized trial have failed. Patient and physician preference for one treatment or the other has proven to be a barrier to randomization and accrual. The EORTC 22952-2600 trial was originally designed to compare outcomes with and without whole brain radiation for patients receiving surgery or radiosurgery for brain metastasis.
We used this as the highest-quality source data available to compare local control of brain metastasis after surgery or radiosurgery, adjusted for by receipt or not of whole brain radiation.
Dr. Weiss[/caption]
Dr. Stephanie E. Weiss MD FASTRO
Chief, Division of Neurologic Oncology
Associate Professor, Department of Radiation Oncology
Director, Radiation Oncology Residency and Fellowship Training Program
Fox Chase Cancer Center
Philadelphia, Pennsylvania
MedicalResearch.com: What is the background for this study?
Response: Brain metastasis are the most common form of brain tumor.
Historically all patients received whole brain radiation as the primary therapy. Patients required neurosurgery to remove lesions if there was a question of diagnosis, what the diagnosis is and if there was a mass effect not relieved with steroids. Surgery was also indicated for patients with a single brain lesion because this offers a survival benefit over just receiving whole brain radiotherapy.
In 2003 a randomized trial proved that radiosurgery offers a similar benefit. So the question taxing patients and doctors at tumor boards since has been: which is better? If neurosurgery is superior, we are under-treating a lot of patients with radiosurgery. If radiosurgery is superior, we are subjecting a lot of patients to unnecessary brain surgery. Attempts to study this in a head-to-head randomized trial have failed. Patient and physician preference for one treatment or the other has proven to be a barrier to randomization and accrual. The EORTC 22952-2600 trial was originally designed to compare outcomes with and without whole brain radiation for patients receiving surgery or radiosurgery for brain metastasis.
We used this as the highest-quality source data available to compare local control of brain metastasis after surgery or radiosurgery, adjusted for by receipt or not of whole brain radiation. Over 8% of Americans Expressed Distress About Having Difficulty Controlling Their Sexual Urges and Behaviors
 Janna A Dickenson, PhD
Doug Braun-Harvey Postdoctoral Fellow
Program in Human Sexuality
Department of Family Medicine
University of Minnesota Medical School
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Researchers and clinicians have contested the term “sex addiction” in favor of alternative definitions and symptom presentations. Recently, the ICD-11 has characterized compulsive sexual behavior disorder (CSBD) as a persistent pattern that involves failing to control intense sexual urges or sexual behaviors that results in significant levels of distress and/or impairment in one’s functioning.
Janna A Dickenson, PhD
Doug Braun-Harvey Postdoctoral Fellow
Program in Human Sexuality
Department of Family Medicine
University of Minnesota Medical School
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Researchers and clinicians have contested the term “sex addiction” in favor of alternative definitions and symptom presentations. Recently, the ICD-11 has characterized compulsive sexual behavior disorder (CSBD) as a persistent pattern that involves failing to control intense sexual urges or sexual behaviors that results in significant levels of distress and/or impairment in one’s functioning.
Age-Related Hearing Loss Linked to Dementia, Depression, Heart Attacks and Stroke
 Dr. Loughrey[/caption]
David Loughrey PhD
Atlantic Fellow for Equity in Brain Health
Global Brain Health Institute
DeafHear Research Partner
NEIL Programme
Trinity College Institute of Neuroscience
MedicalResearch.com: What is the background for this study?
Response: The World Organisation (WHO) estimate that one-third of older adults aged 65 and over have a disabling hearing loss. Increasingly, research is finding that age-related hearing loss (ARHL) may be associated with other negative health outcomes, including dementia which currently affects 50 million people worldwide.
A study recently published in The Lancet reported that of nine possible modifiable risk factors, addressing age-related hearing loss (ARHL) could potentially lead to the largest reduction in the prevalence of dementia globally.
Dr. Loughrey[/caption]
David Loughrey PhD
Atlantic Fellow for Equity in Brain Health
Global Brain Health Institute
DeafHear Research Partner
NEIL Programme
Trinity College Institute of Neuroscience
MedicalResearch.com: What is the background for this study?
Response: The World Organisation (WHO) estimate that one-third of older adults aged 65 and over have a disabling hearing loss. Increasingly, research is finding that age-related hearing loss (ARHL) may be associated with other negative health outcomes, including dementia which currently affects 50 million people worldwide.
A study recently published in The Lancet reported that of nine possible modifiable risk factors, addressing age-related hearing loss (ARHL) could potentially lead to the largest reduction in the prevalence of dementia globally.
Which Questionnaires Best Reflect Dry Eye Symptoms?
 Jennifer P. Craig, Associate Professor
Department of Ophthalmology
New Zealand National Eye Centre
Auckland, New Zealand
MedicalResearch.com: What is the background for this study?
Response: Dry eye disease is a complex multi-factorial condition, which affects between 5% to 50% of the adult population in different parts of the world. The condition can have profound effects on the ocular comfort, visual function, and quality of life of sufferers. In both clinical practice and academic research settings, validated questionnaires are frequently used to screen for dry eye symptomology, before clinical assessment of tear film homeostatic markers is conducted to make an overall diagnosis of dry eye disease.
Although a large number of validated symptomology questionnaires has previously been developed, the recently convened Tear Film and Ocular Surface Dry Eye Workshop II (TFOS DEWS II) identified that the considerable heterogeneities in the study populations, methodologies, and reference standards used in earlier diagnostic accuracy studies introduced significant challenges when trying to compare the diagnostic performance of these screening instruments.
The current study is the first to offer a direct comparison of five commonly used validated questionnaires within the same study population, and uses the global consensus criteria for tear film homeostatic disturbance developed by the TFOS DEWS II as the reference standard.
Jennifer P. Craig, Associate Professor
Department of Ophthalmology
New Zealand National Eye Centre
Auckland, New Zealand
MedicalResearch.com: What is the background for this study?
Response: Dry eye disease is a complex multi-factorial condition, which affects between 5% to 50% of the adult population in different parts of the world. The condition can have profound effects on the ocular comfort, visual function, and quality of life of sufferers. In both clinical practice and academic research settings, validated questionnaires are frequently used to screen for dry eye symptomology, before clinical assessment of tear film homeostatic markers is conducted to make an overall diagnosis of dry eye disease.
Although a large number of validated symptomology questionnaires has previously been developed, the recently convened Tear Film and Ocular Surface Dry Eye Workshop II (TFOS DEWS II) identified that the considerable heterogeneities in the study populations, methodologies, and reference standards used in earlier diagnostic accuracy studies introduced significant challenges when trying to compare the diagnostic performance of these screening instruments.
The current study is the first to offer a direct comparison of five commonly used validated questionnaires within the same study population, and uses the global consensus criteria for tear film homeostatic disturbance developed by the TFOS DEWS II as the reference standard.
Few Than 10% in Large Study Have Optimal Cardiovascular Health
 Dr. Empana[/caption]
Dr. Jean Philippe Empana, MD, PhD
Research Director, INSERM U970
Paris Cardiovascular Research Center (PARCC) Team 4 Cardiovascular Epidemiology & Sudden Death Paris Descartes University
MedicalResearch.com: What is the background for this study?
Response: In 2010, the American Heart Association (AHA) has emphasized the primary importance of the Primordial prevention concept, i.e. preventing the development of risk factors before they emerge, as a complementary prevention strategy for cardiovascular disease (CVD).
Accordingly, the AHA has developed a simple 7-item tool, including 4 behavioral (nonsmoking, and ideal levels of body weight, physical activity and diet) and 3 biological metrics (ideal levels of untreated blood pressure, fasting blood glucose and total cholesterol) for promoting an optimal cardiovascular health (CVH). The relevance of the concept and of the tool has been several times reported by individual studies and meta-analyses (combining the results of several studies) showing substantial and graded benefit for cardiovascular disease but also mortality, quality of life and even cancer risk with higher level of CVH. However, most studies relied on one measure of cardiovascular health.
In the present work, using serial examinations from the well-known Whitehall Study II, we described change in CVH over time and then quantified the association of change in cardiovascular health over 10 years with subsequent incident cardiovascular disease and mortality. This analysis is based on 9256 UK men and women aged 30 to 55 in 1985-88, and thereafter examined every 5 years on average during 30 years.
Dr. Empana[/caption]
Dr. Jean Philippe Empana, MD, PhD
Research Director, INSERM U970
Paris Cardiovascular Research Center (PARCC) Team 4 Cardiovascular Epidemiology & Sudden Death Paris Descartes University
MedicalResearch.com: What is the background for this study?
Response: In 2010, the American Heart Association (AHA) has emphasized the primary importance of the Primordial prevention concept, i.e. preventing the development of risk factors before they emerge, as a complementary prevention strategy for cardiovascular disease (CVD).
Accordingly, the AHA has developed a simple 7-item tool, including 4 behavioral (nonsmoking, and ideal levels of body weight, physical activity and diet) and 3 biological metrics (ideal levels of untreated blood pressure, fasting blood glucose and total cholesterol) for promoting an optimal cardiovascular health (CVH). The relevance of the concept and of the tool has been several times reported by individual studies and meta-analyses (combining the results of several studies) showing substantial and graded benefit for cardiovascular disease but also mortality, quality of life and even cancer risk with higher level of CVH. However, most studies relied on one measure of cardiovascular health.
In the present work, using serial examinations from the well-known Whitehall Study II, we described change in CVH over time and then quantified the association of change in cardiovascular health over 10 years with subsequent incident cardiovascular disease and mortality. This analysis is based on 9256 UK men and women aged 30 to 55 in 1985-88, and thereafter examined every 5 years on average during 30 years.
Treatment Delays Linked To High Mortality for Head and Neck Cancer
 Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
Dr. Graboyes[/caption]
Dr. Evan M. Graboyes MD
Otolaryngologist: Head and Neck Surgeon
Medical University of South Carolina
MedicalResearch.com: What is the background for this study?
Response: Unfortunately, there is no screening test for head and neck cancer like there is for colorectal, prostate, breast, lung, or cervical cancers. As a result, two-thirds of patients with head and neck cancer (HNC) present with loco-regionally advanced disease, making other aspects of timely treatment that much more critically important. We therefore sought to understand the association between treatment delay at different points along the cancer care continuum and oncologic outcomes for patients with head and neck cancer.
Cannabis May Raise Risk of Diabetic Ketoacidosis
 Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.
Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.Canadians Enjoy High Level of Health and Longevity
 Dr. Justin Lang, PhD
Research Analyst, Public Health Agency of Canada
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study is based on the Global Burden of Disease Study, which is led by the Institute of Health Metrics at the University of Washington. In this study, we present estimates from the Global Burden of Disease Study to describe the major causes of health loss among Canadians, and how these have changed from 1990 to 2016.
In 2016, cancers, cardiovascular diseases, musculoskeletal disorders, and mental and substance use disorders, combined, resulted in over half of the total health loss among Canadians as measured by disability adjusted life years. Disability-adjusted life years is a measure that combines both mortality, through years of life lost, and morbidity, through years lived with disability, into a single measure that allows us to compare health loss from different causes using the same metric.
The all-cause age-standardized years of life lost rate declined 12% between 2006 and 2016, while the all-cause age-standardized years lived with disability rate remained stable (+1%) and the all-cause age-standardized disability-adjusted life year rate declined by 5%.
Finally, between 1990 and 2016, there has been a shift in what contributes to health loss in Canada from premature mortality to disability. In 1990, 45% of total all-cause disability-adjusted life years were due to years lived with disability. By 2016, this proportion grew to 52%.
Dr. Justin Lang, PhD
Research Analyst, Public Health Agency of Canada
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This study is based on the Global Burden of Disease Study, which is led by the Institute of Health Metrics at the University of Washington. In this study, we present estimates from the Global Burden of Disease Study to describe the major causes of health loss among Canadians, and how these have changed from 1990 to 2016.
In 2016, cancers, cardiovascular diseases, musculoskeletal disorders, and mental and substance use disorders, combined, resulted in over half of the total health loss among Canadians as measured by disability adjusted life years. Disability-adjusted life years is a measure that combines both mortality, through years of life lost, and morbidity, through years lived with disability, into a single measure that allows us to compare health loss from different causes using the same metric.
The all-cause age-standardized years of life lost rate declined 12% between 2006 and 2016, while the all-cause age-standardized years lived with disability rate remained stable (+1%) and the all-cause age-standardized disability-adjusted life year rate declined by 5%.
Finally, between 1990 and 2016, there has been a shift in what contributes to health loss in Canada from premature mortality to disability. In 1990, 45% of total all-cause disability-adjusted life years were due to years lived with disability. By 2016, this proportion grew to 52%. 


