Author Interviews, Melanoma, NYU/NYMC / 20.02.2026
Melanoma: NYU Study Outlines Mechanisms Tumors Use to Sustain Blood Supply and Escape Immune Detection
[caption id="attachment_72519" align="alignleft" width="200"] Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
 Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.
Dr. Berico[/caption]
MedicalResearch.com Interview with:
Pietro Berico, M.Sc., Ph.D.
Postdoctoral research fellow
Hernando Lab
NYU Grossman School of Medicine
NYU Langone Health
New York, NY 1001
MedicalResearch.com: What is the background for this study?
Response: “Cutaneous melanoma arises under chronic UV irradiation, which selects for aggressive malignant clones. Paradoxically, its high mutational burden also promotes neoantigen formation and robust immune activation. Consequently, melanoma must establish immune evasion mechanisms from the earliest stages of tumor development. The lack of specific genetic mutational patterns linked to immune escape points toward non-mutational mechanisms, such as epigenetic reprogramming.



 Dr. Jiyoung Ahn[/caption]
MedicalResearch.com Interview with:
Jiyoung Ahn, PhD
Dr. Jiyoung Ahn[/caption]
MedicalResearch.com Interview with:
Jiyoung Ahn, PhD







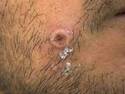
 Dr. Angélica Cifuentes Kottkamp[/caption]
Angélica
Dr. Angélica Cifuentes Kottkamp[/caption]
Angélica

 Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories
Dr. Tsirigos[/caption]
Aristotelis Tsirigos, Ph.D.
Professor of Medicine and Pathology
Co-director, Precision Medicine
Director, Applied Bioinformatics Laboratories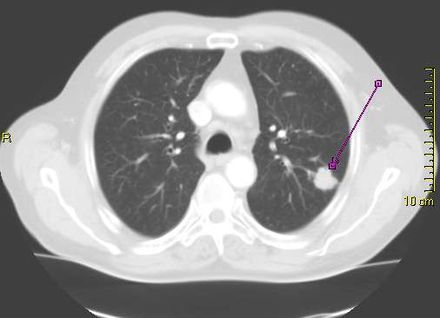
 Dr. Sally Lau[/caption]
Dr. Sally Lau MD
Medical oncologist, NYU Langone’s Perlmutter Cancer Center
Assistant professor of medicine
NYU Grossman School of Medicine
MedicalResearch.com: How big is the problem of
Dr. Sally Lau[/caption]
Dr. Sally Lau MD
Medical oncologist, NYU Langone’s Perlmutter Cancer Center
Assistant professor of medicine
NYU Grossman School of Medicine
MedicalResearch.com: How big is the problem of 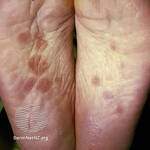









 Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment.
Dr. Bragg[/caption]
Marie Bragg, PhD
Assistant Professor, Department of Population Health on Health Choice
NYU College of Global Public Health
MedicalResearch.com: What is the background for this study?
Response: We know from previous research that children who see food advertisements eat significantly more calories than children who see non-food advertisements. Those studies led the World Health Organization and National Academy of Medicine to issue reports declaring that exposure to food advertising is a major driver of childhood obesity.
What we don’t know is how frequently unhealthy food and beverage brands are appearing in YouTube videos posted by Kid Influencers. Kid influences are children whose parents film videos of the child playing with toys, unwrapping presents, eating food, or engaging in other family-friendly activities. The parents then post the videos to YouTube for other children and parents to view for entertainment. 



