AHA Journals, Author Interviews, Blood Pressure - Hypertension, Heart Disease, UT Southwestern / 31.10.2018
Home Blood Pressure Readings of 130/80 Has Same Cardiovascular Risks as Office Readings
MedicalResearch.com Interview with:
 Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
 Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population. 



 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
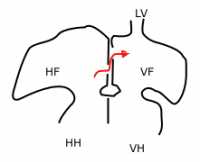
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.






 Dr. Mark Eisner[/caption]
Mark D. Eisner, MD, MPH
Vice PresidentProduct Development Immunology, Infectious Disease and Ophthalmology Genentech
Dr. Eisner discusses the announcement that the FDA has approved XOFLUZA™ (baloxavir marboxil) for the treatment of acute, uncomplicated influenza.
MedicalResearch.com: What is the background for this announcement?
Response: Each year, an estimated 3-11 percent of the U.S. population gets the flu, and it can be very serious, resulting in hospitalization or even death. Since 2010, the Centers for Disease Control and Prevention (CDC) estimates that the flu has resulted annually in 9.2 to 35.6 million illnesses, 140,000 to 900,000 hospitalizations and 12,000 to 80,000 deaths. The severity of last year’s flu season underscores the need for new medical options beyond currently available antivirals.
XOFLUZA was granted Priority Review in June 2018 based on results from the Phase III CAPSTONE-1 study of a single dose of XOFLUZA compared with placebo or oseltamivir 75 mg, twice daily for five days, in otherwise healthy people with the flu, as well as results from a placebo-controlled Phase II study in otherwise healthy people with the flu.
Dr. Mark Eisner[/caption]
Mark D. Eisner, MD, MPH
Vice PresidentProduct Development Immunology, Infectious Disease and Ophthalmology Genentech
Dr. Eisner discusses the announcement that the FDA has approved XOFLUZA™ (baloxavir marboxil) for the treatment of acute, uncomplicated influenza.
MedicalResearch.com: What is the background for this announcement?
Response: Each year, an estimated 3-11 percent of the U.S. population gets the flu, and it can be very serious, resulting in hospitalization or even death. Since 2010, the Centers for Disease Control and Prevention (CDC) estimates that the flu has resulted annually in 9.2 to 35.6 million illnesses, 140,000 to 900,000 hospitalizations and 12,000 to 80,000 deaths. The severity of last year’s flu season underscores the need for new medical options beyond currently available antivirals.
XOFLUZA was granted Priority Review in June 2018 based on results from the Phase III CAPSTONE-1 study of a single dose of XOFLUZA compared with placebo or oseltamivir 75 mg, twice daily for five days, in otherwise healthy people with the flu, as well as results from a placebo-controlled Phase II study in otherwise healthy people with the flu.


 Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.
Faiz Gani, PhD
Postdoctoral research fellow
Department of Surgery
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Firearm related injuries are a leading cause of injury and death in the United States, yet, due to combination of factors, limited data exist that evaluate these injuries, particularly among younger patients (patients younger than 18 years).
The objective of this study was to describe emergency department utilization for firearm related injuries and to quantitate the financial burden associated with these injuries.
In our study of over 75,000 emergency department visits, we observed that each year, over 8,300 children and adolescents present to the emergency department for the treatment / management of a gunshot injury. Within this sub-population of patients, we observed that these injuries are most frequent among patients aged 15-17 years and while these injuries decreased over time initially, were observed to increase again towards the end of the time period studied.
In addition to describing the clinical burden of these injuries, we also sought to describe the financial burden associated with these injuries. For patients discharged from the emergency department, the average (median) charge associated with their care was $2,445, while for patients admitted as inpatients for further care, the average (median) charge was $44,966.
Collectively these injuries resulted in $2.5 billion in emergency department and hospital charges over the time period studied. This translates to an annual financial burden of approximately $270 million.




 Dr. Michael Snape[/caption]
Michael Snape, Ph.D.
Chief executive officer
Chief scientific officer
AMO Pharma
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This is a further analysis of the Phase II Proof of Concept study that was described in March. We have extended the findings from that study by performing further analyses of the data obtained and also commencing an analysis of the relationship between the levels of AMO-02 involved and the clinical response seen.
The main finding is a confirmation that our previously reported conclusions are supported. The concordant trend analysis revealed a clear dose-response relationship that favored the 1000 mg over 400 mg dose for four of the 10 response variables differed in favor of 1000 mg over 400 mg dose on key clinician and caregiver measures, autism scores and grip strength.
Dr. Michael Snape[/caption]
Michael Snape, Ph.D.
Chief executive officer
Chief scientific officer
AMO Pharma
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: This is a further analysis of the Phase II Proof of Concept study that was described in March. We have extended the findings from that study by performing further analyses of the data obtained and also commencing an analysis of the relationship between the levels of AMO-02 involved and the clinical response seen.
The main finding is a confirmation that our previously reported conclusions are supported. The concordant trend analysis revealed a clear dose-response relationship that favored the 1000 mg over 400 mg dose for four of the 10 response variables differed in favor of 1000 mg over 400 mg dose on key clinician and caregiver measures, autism scores and grip strength. 

 Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door.
Prof. Kleiman[/caption]
Prof. Mark A. R. Kleiman PhD
Affiliated Faculty, NYU Wagner; Professor of Public Policy
NYU Marron Institute of Urban Management
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: As state after state legalizes the sale of cannabis, the question of cannabis-impaired driving is getting more attention. There is evidence that the practice has become more common, both because cannabis use - and especially heavy, frequent use - has increased and because a distressingly large fraction of cannabis users believe, falsely, that stoned driving is safe.
The natural response to the problem is to treat cannabis on a par with alcohol: fairly severe criminal penalties for impaired driving, with impairment defined by a specific level of the drug in the body. The paper argues that this would be a mistake, for four independent reasons:
- While cannabis makes driving riskier, it does so by about a factor of two, with no strongly observed dependency on dosage. Alcohol, by contrast, has a steep dose-effect curve. At the legal limit of 0.08% blood alcohol content by weight, the relative risk of drunk driving is at least eight; at 0.15%, which is fairly common, the relative risk has been estimated at 30-50. So there is no justification for punishing stoned driving as severely as we punish drunk driving.
- The lack of evidence of a strong dose-effect relationship suggests that a legal standard based on the content of cannabinoids in blood may not be appropriate.
- Even if a blood standard were valid, the lack of a breath test would make enforcing that standard nearly impossible as a practical matter.
- The long and unpredictable course of cannabis metabolism means that frequent users will be at risk of failing a drug test even when they are neither subjectively intoxicated nor objectively impaired. Worse, they would have no way of judging in advance whether or not driving would be legal. The result would be a re-criminalization of cannabis use through the back door. 

 Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.
Dipender Gill[/caption]
Dipender Gill
Imperial College Healthcare NHS Trust
London, United Kingdon
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Iron status has previously been associated with risk of various types of cardiovascular disease, including stroke. However, the observational research methodologies that identified these associations can be affected by confounding from environmental factors and reverse causation.
We used randomly allocated genetic variants that affect iron status to investigate its effect on risk of different types of ischemic stroke, and found evidence to support that higher iron status increases risk of cardioembolic stroke.



 Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.
Dr. Epling[/caption]
John W. Epling, Jr., M.D., M.S.Ed
Professor of Family and Community Medicine
Virginia Tech Carilion School of Medicine
Roanoke, VA
USPSTF Task Force Member
MedicalResearch.com: What is the background for this study?
Response: Intimate partner violence, often known as domestic violence, can have devastating consequences to one’s health and wellbeing. It can lead to mental illness, substance abuse, unintended pregnancy, and even death. This is a serious public health issue in America: one in three men—and even more women—experience it in their lifetimes. Because this is such an important topic, and the last time we made a recommendation on it was in 2013, the U.S. Preventive Services Task Force reviewed the most recent evidence to determine how clinicians can help prevent the negative health effects of intimate partner violence.

 Sean C. Rose, MD
Pediatric sports neurologist and co-director
Complex Concussion Clinic
Nationwide Children’s Hospital
Assistant professor of Pediatrics
The Ohio State University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The link between sub-concussive head impacts and declines in neurocognitive function has been reported by some studies, yet refuted by others. There is very little evidence that has been collected in children as they are sustaining these head impacts.
We initiated a multi-year study of youth football players to provide a more in-depth look at the question. We measured head impacts using helmet sensors during the 2016 football season. 112 players age 9-18 completed a battery of neurocognitive tests before and after the football season.
We found that neither the total burden of head impacts nor the intensity of individual impacts were associated with changes in testing performance from pre to post-season.
Sean C. Rose, MD
Pediatric sports neurologist and co-director
Complex Concussion Clinic
Nationwide Children’s Hospital
Assistant professor of Pediatrics
The Ohio State University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The link between sub-concussive head impacts and declines in neurocognitive function has been reported by some studies, yet refuted by others. There is very little evidence that has been collected in children as they are sustaining these head impacts.
We initiated a multi-year study of youth football players to provide a more in-depth look at the question. We measured head impacts using helmet sensors during the 2016 football season. 112 players age 9-18 completed a battery of neurocognitive tests before and after the football season.
We found that neither the total burden of head impacts nor the intensity of individual impacts were associated with changes in testing performance from pre to post-season.



 Jennifer Woo Baidal, MD, MPH
Assistant Professor of Pediatrics
Director of Pediatric Weight Management,
Division of Pediatric Gastroenterology, Hepatology, and Nutrition,
Columbia University Medical Center &
New York-Presbyterian Morgan Stanley Children’s Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Childhood obesity prevalence is historically high, with most incident obesity among children occurring before age 5 years. Racial/ethnic and socioeconomic disparities in childhood obesity are already apparent by the first years of life. Latino/Hispanic children in low-income families are at-risk for obesity. Thus, understanding potentially effective ways to prevent childhood obesity, particularly in vulnerable populations, should focus on early life.
Sugar-sweetened beverage (SSB) consumption is a modifiable risk factor for obesity and is linked to other adverse health outcomes. Maternal SSB consumption in pregnancy and infant sugar-sweetened beverage consumption in the first year of life are linked to later childhood obesity.
We sought to describe beverage consumption in a modern cross-sectional cohort of 394 low-income, Latino families, and to examine the relationship of parental attitudes toward sugar-sweetened beverages with parental and infant SSB consumption.
Jennifer Woo Baidal, MD, MPH
Assistant Professor of Pediatrics
Director of Pediatric Weight Management,
Division of Pediatric Gastroenterology, Hepatology, and Nutrition,
Columbia University Medical Center &
New York-Presbyterian Morgan Stanley Children’s Hospital
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Childhood obesity prevalence is historically high, with most incident obesity among children occurring before age 5 years. Racial/ethnic and socioeconomic disparities in childhood obesity are already apparent by the first years of life. Latino/Hispanic children in low-income families are at-risk for obesity. Thus, understanding potentially effective ways to prevent childhood obesity, particularly in vulnerable populations, should focus on early life.
Sugar-sweetened beverage (SSB) consumption is a modifiable risk factor for obesity and is linked to other adverse health outcomes. Maternal SSB consumption in pregnancy and infant sugar-sweetened beverage consumption in the first year of life are linked to later childhood obesity.
We sought to describe beverage consumption in a modern cross-sectional cohort of 394 low-income, Latino families, and to examine the relationship of parental attitudes toward sugar-sweetened beverages with parental and infant SSB consumption.

 Dr. Rothbard[/caption]
MedicalResearch.com Interview with:
Jonathan Rothbard, MA, PhD
Steinman Lab Stanford Medicine
Co-founder
Dr. Rothbard[/caption]
MedicalResearch.com Interview with:
Jonathan Rothbard, MA, PhD
Steinman Lab Stanford Medicine
Co-founder