Author Interviews, Cannabis, Diabetes, JAMA / 06.11.2018
Cannabis May Raise Risk of Diabetic Ketoacidosis
MedicalResearch.com Interview with:
[caption id="attachment_45647" align="alignleft" width="150"] Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.
Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.
 Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.
Dr. Shah[/caption]
Viral Shah, MD
Assistant Professor of Medicine & Pediatrics
Barbara Davis Center for Diabetes, Adult Clinic
School of Medicine
University of Colorado Anschutz Medical Campus
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Cannabis use is increasing in Colorado and many patients with type 1 diabetes (which is an autoimmune form of diabetes that requires life insulin therapy) are using cannabis. Therefore, we surveyed adult patients with type 1 diabetes to study the association between cannabis use and glycemic control and diabetes acute complications (such as diabetic ketoacidosis) in adults with type 1 diabetes.
Main findings of the study: The risk for diabetic ketoacidosis (a serious condition where body produces high levels of acids called ketones in patients with diabetes) was two times higher among adults with type 1 diabetes who reported using cannabis in the past 12 months compared to adults with type 1 diabetes who reported not using cannabis.


 Dr. McLaughlin[/caption]
Ryan J. McLaughlin, PhD
Assistant Professor
Department of Integrative Physiology & Neuroscience
College of Veterinary Medicine
Washington State University
Pullman, WA 99164-7620
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of cannabis during pregnancy is a growing health concern, yet the long-term cognitive ramifications for developing offspring remain largely unknown. Human studies exploring the long-term effects of maternal cannabis use have been sparse for several reasons, including the length and cost of such studies, as well as the fact that experimentally assigning mothers to smoke cannabis during pregnancy is obviously ethically impractical. Animal models of maternal cannabis use have been advantageous in this respect, but they have been limited by the drugs used (synthetic cannabinoids vs. THC vs. cannabis plant) and the way that they are administered. In our study, we used a more translationally relevant animal model of maternal cannabis use that exposes pregnant rat dams to whole plant cannabis extracts using the intra-pulmonary route of administration that is most common to human users. Our preliminary data indicate that twice-daily exposure to a high-dose cannabis extract during pregnancy may produce deficits in cognitive flexibility in adult rat offspring. Importantly, these rats did not experience general learning deficits, as they performed comparably to non-exposed offspring when required to follow a cue in their environment that dictate reinforcer delivery. Instead, deficits were observed only when rats were required to disregard this previous cue-based strategy and adopt a new egocentric spatial strategy in order to continue receiving the sugar reinforcers.
Dr. McLaughlin[/caption]
Ryan J. McLaughlin, PhD
Assistant Professor
Department of Integrative Physiology & Neuroscience
College of Veterinary Medicine
Washington State University
Pullman, WA 99164-7620
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The use of cannabis during pregnancy is a growing health concern, yet the long-term cognitive ramifications for developing offspring remain largely unknown. Human studies exploring the long-term effects of maternal cannabis use have been sparse for several reasons, including the length and cost of such studies, as well as the fact that experimentally assigning mothers to smoke cannabis during pregnancy is obviously ethically impractical. Animal models of maternal cannabis use have been advantageous in this respect, but they have been limited by the drugs used (synthetic cannabinoids vs. THC vs. cannabis plant) and the way that they are administered. In our study, we used a more translationally relevant animal model of maternal cannabis use that exposes pregnant rat dams to whole plant cannabis extracts using the intra-pulmonary route of administration that is most common to human users. Our preliminary data indicate that twice-daily exposure to a high-dose cannabis extract during pregnancy may produce deficits in cognitive flexibility in adult rat offspring. Importantly, these rats did not experience general learning deficits, as they performed comparably to non-exposed offspring when required to follow a cue in their environment that dictate reinforcer delivery. Instead, deficits were observed only when rats were required to disregard this previous cue-based strategy and adopt a new egocentric spatial strategy in order to continue receiving the sugar reinforcers.

 Dr. Verge[/caption]
Danilo Verge MD MBA
Vice President, CVRM Global Medical Affairs
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Dapagliflozin, an SGLT2 inhibitor (sodium-glucose co-transporter 2), has been shown to improve glycemic control by decreasing glucose reabsorption in the kidneys and inducing urinary glucose clearance. SGLT2 inhibitors have also been shown to be effective in lowering albuminuria and stabilizing eGFR (estimated glomerular filtration rate). The effect of dapagliflozin on UACR (urine albumin-to-creatinine ratio) has been shown to vary among patients.
The objective of this post-hoc analysis, based on the pooled data from 11 randomized, placebo-controlled clinical trials, was to assess baseline characteristics and concurrent changes in cardiovascular (CV) risk markers associated with UACR response to dapagliflozin.
Dr. Verge[/caption]
Danilo Verge MD MBA
Vice President, CVRM Global Medical Affairs
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Dapagliflozin, an SGLT2 inhibitor (sodium-glucose co-transporter 2), has been shown to improve glycemic control by decreasing glucose reabsorption in the kidneys and inducing urinary glucose clearance. SGLT2 inhibitors have also been shown to be effective in lowering albuminuria and stabilizing eGFR (estimated glomerular filtration rate). The effect of dapagliflozin on UACR (urine albumin-to-creatinine ratio) has been shown to vary among patients.
The objective of this post-hoc analysis, based on the pooled data from 11 randomized, placebo-controlled clinical trials, was to assess baseline characteristics and concurrent changes in cardiovascular (CV) risk markers associated with UACR response to dapagliflozin.

 Lei Qin[/caption]
Lei Qin MS
Director, Health Economics and Payer Analytics
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Renin-angiotensin-aldosterone system inhibitors (RAASi) are guideline-recommended therapies for patients with chronic kidney disease (CKD), but are commonly prescribed at suboptimal doses, which has been associated with worsening clinical outcomes. The objective of our study was to estimate the real-world associations between RAASi dose and adverse clinical outcomes in patients prescribed RAASi therapies with new-onset CKD in the UK.
Lei Qin[/caption]
Lei Qin MS
Director, Health Economics and Payer Analytics
AstraZeneca
MedicalResearch.com: What is the background for this study?
Response: Renin-angiotensin-aldosterone system inhibitors (RAASi) are guideline-recommended therapies for patients with chronic kidney disease (CKD), but are commonly prescribed at suboptimal doses, which has been associated with worsening clinical outcomes. The objective of our study was to estimate the real-world associations between RAASi dose and adverse clinical outcomes in patients prescribed RAASi therapies with new-onset CKD in the UK.

 Dr. Agrawal[/caption]
Rahul Agrawal MD PhD
VP, Global Medicines Leader
AstraZeneca
MedicalResearch.com: What is the background for this study?
About the study: HARMONIZE Global is a Phase III, randomized, multicenter, double-blind, placebo-controlled trial involving 267 patients with hyperkalemia (mean potassium levels greater than 5.0 mEq/L) in 47 study locations across the Asia Pacific region, which will support registration in Japan, Taiwan, Korea and Russia.
Study design: The trial design of HARMONIZE Global is similar to HARMONIZE (NCT02088073) but evaluated two doses of LOKELMATM (sodium zirconium cyclosilicate) instead of three, as well as patients in different geographical regions.
Dr. Agrawal[/caption]
Rahul Agrawal MD PhD
VP, Global Medicines Leader
AstraZeneca
MedicalResearch.com: What is the background for this study?
About the study: HARMONIZE Global is a Phase III, randomized, multicenter, double-blind, placebo-controlled trial involving 267 patients with hyperkalemia (mean potassium levels greater than 5.0 mEq/L) in 47 study locations across the Asia Pacific region, which will support registration in Japan, Taiwan, Korea and Russia.
Study design: The trial design of HARMONIZE Global is similar to HARMONIZE (NCT02088073) but evaluated two doses of LOKELMATM (sodium zirconium cyclosilicate) instead of three, as well as patients in different geographical regions.


 Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
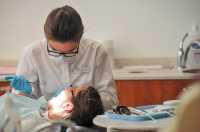
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.
Prof. Thornhill[/caption]
Martin H. Thornhill MBBS, BDS, PhD, MSc, FDSRCS(Edin), FDSRCSI, FDSRCS(Eng)
Professor of Translational Research in Dentistry
Academic Unit of Oral & Maxillofacial Medicine Surgery & Pathology,
University of Sheffield School of Clinical Dentistry
MedicalResearch.com: What is the background for this study?
Response: Infective endocarditis is an infection of the heart valves that has a high death rate (around 30% in the first year). It requires intensive treatment often involving replacement of affected heart valves and frequently results in serious long-term illness and disability in those who survive as well as an increased risk of re-infection and high healthcare costs.
In ~40% of cases, bacteria from the mouth are implicated as the causal organism. Because of this, guideline committees around the world recommended that all those at risk of infective endocarditis should receive antibiotic prophylaxis before undergoing invasive dental procedures. Due to a lack of evidence for efficacy, however, guideline committees started to limit the use of antibiotic prophylaxis. And in 2007, the American Heart Association (AHA) guideline committee recommended that antibiotic prophylaxis should continue for those at high-risk but should cease for those at moderate risk of endocarditis. Most guideline countries around the world followed suite. Except in the UK, where the National Institute for Health and Care Excellence (NICE) recommended that the use of antibiotic prophylaxis should completely stop in 2008.





 Dr. Labrie[/caption]
Viviane Labrie, Ph.D.
Assistant Professor
Center for Neurodegenerative Science
Van Andel Research Institute
Grand Rapids, Michigan
MedicalResearch.com: What is the background for this study?
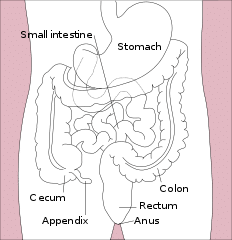
Response: Our lab has an interest in the early events and initiation of neurodegenerative diseases. Parkinson’s disease for a long time was thought to be a movement disorder driven by the destruction of dopamine neurons in a specific area of the brain, the substantia nigra. In the last 10 years it has become evident that Parkinson’s disease is not just a movement disorder but hosts a whole range of non-motor systems. One of the most common non-motor symptoms in Parkinson’s patients is issues with the gastrointestinal (GI) tract. GI symptoms often occur early in Parkinson’s disease; for many patients, GI symptoms precede the onset of motor symptoms by as many as 2 decades. Moreover, the GI is not only involved in the early signs of Parkinson’s but has been proposed to be a place in the body where Parkinson’s disease begins.
The hallmark pathology of Parkinson’s disease in the brain is Lewy bodies, which contains a clumped form of a protein called alpha-synuclein. There is evidence that Parkinson’s disease pathology, this clumped alpha-synuclein protein, is detectable in the GI tract, even many years before the onset of Parkinson’s motor symptoms. Clumped alpha-synuclein is also capable of traveling across nerve cells. There is evidence that clumped alpha-synuclein can travel up the nerve that connects the GI tract to the brain and enter the brain. This could be disastrous because clumped alpha-synuclein can seed and spread in the brain, which has neurotoxic effects and can eventually lead to Parkinson’s disease. In fact, in the brain of Parkinson’s patients, one of the first places where alpha-synuclein clumps are detected is at the terminal where the gut nerve connects to the brain, and this pathology advances from this point to other brain areas as the disease progresses.
This intriguing connection of the GI tract to the early processes of Parkinson’s disease had us interested in trying to understand how the gut could be involved in triggering Parkinson’s. But the GI tract is a very big place, and we first asked ourselves, where should we look to better understand GI involvement in Parkinson’s disease?
Dr. Labrie[/caption]
Viviane Labrie, Ph.D.
Assistant Professor
Center for Neurodegenerative Science
Van Andel Research Institute
Grand Rapids, Michigan
MedicalResearch.com: What is the background for this study?
Response: Our lab has an interest in the early events and initiation of neurodegenerative diseases. Parkinson’s disease for a long time was thought to be a movement disorder driven by the destruction of dopamine neurons in a specific area of the brain, the substantia nigra. In the last 10 years it has become evident that Parkinson’s disease is not just a movement disorder but hosts a whole range of non-motor systems. One of the most common non-motor symptoms in Parkinson’s patients is issues with the gastrointestinal (GI) tract. GI symptoms often occur early in Parkinson’s disease; for many patients, GI symptoms precede the onset of motor symptoms by as many as 2 decades. Moreover, the GI is not only involved in the early signs of Parkinson’s but has been proposed to be a place in the body where Parkinson’s disease begins.
The hallmark pathology of Parkinson’s disease in the brain is Lewy bodies, which contains a clumped form of a protein called alpha-synuclein. There is evidence that Parkinson’s disease pathology, this clumped alpha-synuclein protein, is detectable in the GI tract, even many years before the onset of Parkinson’s motor symptoms. Clumped alpha-synuclein is also capable of traveling across nerve cells. There is evidence that clumped alpha-synuclein can travel up the nerve that connects the GI tract to the brain and enter the brain. This could be disastrous because clumped alpha-synuclein can seed and spread in the brain, which has neurotoxic effects and can eventually lead to Parkinson’s disease. In fact, in the brain of Parkinson’s patients, one of the first places where alpha-synuclein clumps are detected is at the terminal where the gut nerve connects to the brain, and this pathology advances from this point to other brain areas as the disease progresses.
This intriguing connection of the GI tract to the early processes of Parkinson’s disease had us interested in trying to understand how the gut could be involved in triggering Parkinson’s. But the GI tract is a very big place, and we first asked ourselves, where should we look to better understand GI involvement in Parkinson’s disease?



 Dr. Nowell[/caption]
Dr. W. Benjamin Nowell, Ph.D.
Director of Patient-Centered Research
CreakyJoints, study co-author
Co-principal investigator of ArthritisPower
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rheumatoid Arthritis (RA) can diminish patients’ work productivity and increase the risk of long-term disability, economic insecurity and worsening health, but limited research informs these issues. The purpose of our study was to examine associations between patients’ RA disease activity and their productivity and workplace support, using real-world data from the ArthritisPower research registry.
Our study looked at a sample of participants with RA who had a history of or current treatment with non-biologic and/or biologic disease-modifying antirheumatic drugs (DMARD) (n=296). Among the study sample, 74 percent had high disease activity (HDA) as determined by RAPID3 (>12), a common measure of disease activity in RA.
Dr. Nowell[/caption]
Dr. W. Benjamin Nowell, Ph.D.
Director of Patient-Centered Research
CreakyJoints, study co-author
Co-principal investigator of ArthritisPower
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Rheumatoid Arthritis (RA) can diminish patients’ work productivity and increase the risk of long-term disability, economic insecurity and worsening health, but limited research informs these issues. The purpose of our study was to examine associations between patients’ RA disease activity and their productivity and workplace support, using real-world data from the ArthritisPower research registry.
Our study looked at a sample of participants with RA who had a history of or current treatment with non-biologic and/or biologic disease-modifying antirheumatic drugs (DMARD) (n=296). Among the study sample, 74 percent had high disease activity (HDA) as determined by RAPID3 (>12), a common measure of disease activity in RA.

 Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population.
Dr. Wanpen Vongpatanasin, M.D.
Professor of Medicine
Program Director, Hypertension Fellowship Program
UT Southwestern Medical Center in Dallas
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: The new US hypertension guideline places a greater emphasis on out-of-office blood pressure measurement, and maintains that a clinic BP of 130/80 mm Hg is equivalent to the same reading for home BP monitoring or daytime ambulatory BP monitoring. That is based, however, on data from non-US cohorts, primarily from Japanese cohorts and some European populations. None has been studied in the US population until now.
To find out, we analyzed large multi-ethnic studies of primarily young and middle-aged adults in Dallas, Texas, and Durham, N.C., that compared home blood pressure to clinic measurements, using the regression correlation (i.e. regression approach). To confirm the findings, we use another approach called “outcome approach” by determining risks of stroke, MI, and death associated with a clinic systolic blood pressure reading of 130 mmHg from the 3,132 participants in the Dallas study during an 11-year follow up.
Then, we determined the home blood pressure levels that carried the same heart disease risk and stroke risk as the clinic systolic 130 mm Hg reading.
We found that the level of home blood pressure of 130/80 mm Hg actually best correlates with blood pressure taken at the doctor’s office of 130/80 mmHg. This is true for whites, blacks and Hispanic patients in both treated and untreated population. 

 Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
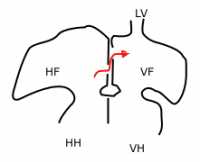
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.
Dr. Elgendy[/caption]
Akram Elgendy MD
Division of Cardiovascular Medicine
University of Florida
MedicalResearch.com: What is the background for this study?
Response: Recent clinical trials have demonstrated that percutaneous patent foramen ovale closure is associated with lower risk of stroke recurrence in cryptogenic stroke patients. However, new-onset atrial fibrillation (AF) has been reported as a safety concern. To better understand the risk of new-onset AF, we performed a meta-analysis of PFO closure trials in patients with cryptogenic stroke and migraine.



