Does Changing Zip Codes Change Your Risk of Chronic Health Conditions?
Time for a Change in Endoscopic Modality of GI Cancer Screening
Which Income Group Linked to More E-Cigarette Purchases?
Who Takes COVID-19 Health Problems More Seriously? Men or Women?
SARS-CoV-2 Can Remain Viable on Surfaces Longer Than Originally Thought
Re-evaluation of Race Multiplier in Estimating Kidney Disease
The original CKD-EPI and MDRD studies showed an association between African-American race with higher measured GFR at the same blood creatinine concentration. However, there have been concerns raised about the application of the race multiplier to all African-American patients. First, there is no clear biological explanation for the association, the identification of Black race was unclear in some of the cohorts used in these studies, and there is vast genetic and ancestral heterogeneity among those who self-identify as black. The use of the race multiplier also ignores the fact that race is a social, not biological construct.
We found that with the removal of the race multiplier, up to one in every three African-American patients would be reclassified as having a more severe stage of CKD, with one-quarter of African-American patients going from stage 3 to stage 4. We also found that with the removal of the race multiplier, 64 patients would have had an eGFR <20, the threshold for referral for kidney transplant, and none of these patients were referred, evaluated or waitlisted for transplant. This is in contrast, to those African-American patients with an eGFR <20 with the race multiplier applied, who had a higher odds of being referred, evaluated or waitlisted for transplant compared to other racial groups (Odds ratio of 2.28, compared to White cohort).
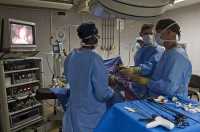
(more…)Surgical Procedures That Generate Aerosols Requiring Enhanced PPE


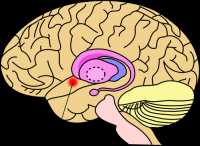
MRI Detects Brain Structure Linked to Increased Weight Gain in Children
Why Do Female Surgeons Perform Less Complex Procedures?
Dopamine Genotype Linked to Walking Speed in Older Adults
President of Transplant Recipients International Discusses Transplantation Experience in Time of COVID-19


Musical Training in Childhood Linked to Improved Attention and Working Memory
TAGRISSO® (osimertinib) in Resected EGFR-Mutated Non–Small-Cell Lung Cancer
Is Exercise Intensity Related to Longevity?
Parents Play Important Role in Whether Kids Smoke or Vape


Global Liver Institute Urges Congress to Fund Fight Against Liver Cancer During COVID-19 Epidemic
DetermaRx™ Stratification Test Identify Patients With Stage I-IIA Non-Squamous NSCLC Who May Benefit From Adjuvant Chemotherapy
- Stage I-IIA non-squamous NSCLC represents ~20% of the lung cancer population and 40,000 patients annually in the U.S.1
- Patients with this diagnosis usually undergo surgical resection and are presumed “cured”. While these patients are presumed “cured”, the recurrence rate in early-stage NSCLC of 30-50%. Usually, these recurrences happen within the first two years after surgery and are likely due to the presence of occult distant metastasis at the time of surgery.2
- Until now, there has not been a validated means of identifying which early-stage patients are at a higher risk of disease recurrence and require adjuvant chemotherapy, versus those patients that are likely cured by surgery alone.
Efficacy of New Exhalation Delivery System with Fluticasone (EDS-FLU) in Patients Who Remain Symptomatic on Standard Nasal Steroid Sprays
Food Insecurity and COVID-19 May Worsen Both Conditions
Adolescents and Young Adults Will Frequently Vape Both Nicotine and Cannabis
Is it More Manly to Get Less Sleep?
E-Cigarette Use Increased in Young Adult Never Smokers
SARS-CoV-2 mRNA-1273 Vaccine: Encouraging Safety and Immunogenicity Data in Older Adults
CDC Study Finds Association Between Marijuana Use and Risky Behaviors in High School Students
SUNRISE 2 Trial: Long-Term Safety and Efficacy of DAYVIGO™ (lemborexant) For Insomnia in Adults
- SUNRISE 2 was one of two pivotal Phase 3 studies evaluated in the U.S. Food and Drug Administration’s approval of DAYVIGO (lemborexant) CIV in December 2019.
- SUNRISE 2 was a pivotal six-month placebo-controlled treatment trial with a 6-month active treatment period including adult patients age 18 or older who met DSM-5 criteria for insomnia disorder.
- Patients were randomized to placebo (n=325), DAYVIGO 5 mg (n=323), or DAYVIGO 10 mg (n=323) once nightly for the first six months of the study (Treatment Period 1).
- The primary efficacy endpoint was the mean change from baseline to end of treatment at six months for subjective sleep onset latency (sSOL; the estimated minutes from the time that the patient attempted to sleep until sleep onset).
- Secondary efficacy endpoints were mean change from baseline to end of treatment at six months subjective sleep efficiency (sSE; the proportion of time spent asleep per time in bed) and subjective wake after sleep onset (sWASO; the minutes of wake from the onset of sleep until wake time). These endpoints were measured by sleep diary.
- At Virtual SLEEP 2020, a post-hoc analysis of SUNRISE 2 was shared in an oral presentation, which looked specifically at the long-term efficacy and safety of lemborexant in elderly adults with insomnia disorder.
- Insomnia disorder, a chronic condition with long-term consequences for health and well-being, is prevalent in older adults.
- This analysis of the SUNRISE 2 data reflects new learnings on the sustained impact of DAYVIGO on sleep onset and sleep maintenance in an older patient population.