Author Interviews, Cancer Research, JAMA, Race/Ethnic Diversity / 10.06.2022
Rural Cancer Survival Trails Urban Patients, Especially for Minorities
MedicalResearch.com Interview with:
[caption id="attachment_59246" align="alignleft" width="150"] Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
 Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.
Dr. Lewis-Thames[/caption]
Marquita W. Lewis-Thames, PhD (she/her/Dr.)
Assistant Professor, Department of Medical Social Science
Center for Community Health, Member Researcher
Assistant Directors of Community Outreach and Engagement, Robert H. Lurie Comprehensive Cancer Center
Feinberg School of Medicine, Northwestern University
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Incidence, mortality, and survivorship provide a comprehensive description of cancer for a group of people. Differences in cancer incidence and mortality trends by rural-urban status and race and ethnicity are well documented, but urban-rural cancer survivorship trends by race and ethnicity are unknown. To this end, we examined almost 40 years of racial and ethnic differences by rural-urban status for 5-year survival of patients with lung, prostate, breast, and colorectal cancers.
Using a nationwide epidemiological assessment of 1975-2011 data from the SEER database, we found that 5-year cancer-specific survival trends increased for all cancer types and race and ethnic groups, regardless of rural or urban status.
Generally, rural, and non-Hispanic Black cancer patients had worse survival outcomes than others.






 Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace.
Dr. Rowe[/caption]
Susannah G. Rowe, MD, MPH
Office of Equity, Vitality and Inclusion
Boston University Medical Group
Boston Medical Center
Boston University School of Medicine
Boston, Massachusetts
MedicalResearch.com: What is the background for this study?
Response: We wanted to learn how frequently mistreatment occurs for clinicians at work and how it impacts their occupational well-being. We began to see more anecdotal reports of workplace mistreatment of clinicians even before the pandemic. In the extraordinarily stressful environment we are currently experiencing, with people feeling exhausted and emotionally threadbare on some level, the problem appears to be growing.
We also predicted that the burden of mistreatment would not borne be equally. It has often been said that we are all in the same storm but in different boats – some of us are riding out the storm in comfortable ocean liners, while others are paddling in canoes without life jackets. What we are learning, though, is that we are not in fact experiencing the same storm. For example, the increasing intolerance and erosion of public civility we have seen in recent years might show up as minor annoyances for some of us, and actual threats of violence for others depending in large part on our gender and racialized identities. Our relationship to privilege and oppression affects our experiences, creating protections or additional burdens, so when studying clinician occupational well-being, it seemed important to consider how these disparities play out in the workplace. 
 Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?
Dr. Clarke[/caption]
Megan Clarke, Ph.D., M.H.S.,
Earl Stadtman Investigator
Division of Cancer Epidemiology and Genetics
National Cancer Institute
MedicalResearch.com: What is the background for this study?

 Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
Dr. Ogedegbe[/caption]
MedicalResearch.com Interview with:
Gbenga Ogedegbe, MD, MPH
Dr. Adolph & Margaret Berger Professor of Population Health
Director, Division of Health & Behavior
Director Center for Healthful Behavior Change
Department of Population Health
NYU Langone Health
NYU School of Medicine
Member of the U.S. Preventive Services Task Force
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Heart disease and stroke are the leading causes of mortality in the United States, accounting for more than one in four deaths.
Taking a daily aspirin may help prevent a first heart attack or stroke in some people, but it can also cause some harm, like internal bleeding. The decision on whether or not to start taking a daily aspirin should be based primarily on age, but cardiovascular disease risk, a person’s chances of bleeding, and other factors should also be taken into account.
 Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.
Prof. McManus[/caption]
Richard McManus MA PhD MBBS FRCGP FRCP
Professor of Primary Care
Dr. McManus chairs the Blood Pressure Monitoring Working Party
of the British Hypertension Society
Nuffield Department of Primary Care Health Sciences
MedicalResearch.com: What is the background for this study?
Response: About one in ten people who are pregnant develop high blood pressure and almost half of these go onto to have pre-eclampsia. Many pregnant women and individuals are already measuring their own blood pressure – well over half of those with high blood pressure in a recent large survey in the UK but until recently there were no data to support this.

 Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000.
Dr. Georgiou[/caption]
Archelle Georgiou, MD
Chief Health Officer for Starkey
Starkey Hearing Technologies
Eden Prairie, Minnesota
MedicalResearch.com: What is the background for this study?
Response: In August 2021, Starkey introduced a vaccination incentive program for employees in the U.S. to provide education on COVID-19 and encourage vaccinations. The program encouraged employees to watch and acknowledge online educational information and report their vaccination status. Those fully vaccinated and who submitted proof of vaccination by September 2021, including employees who were vaccinated prior to the incentive announcement, received $1,000. 

 Dr. Cheng-Ying Ho[/caption]
Cheng-Ying Ho, MD, PhD
Associate Professor
Department of Pathology
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study?
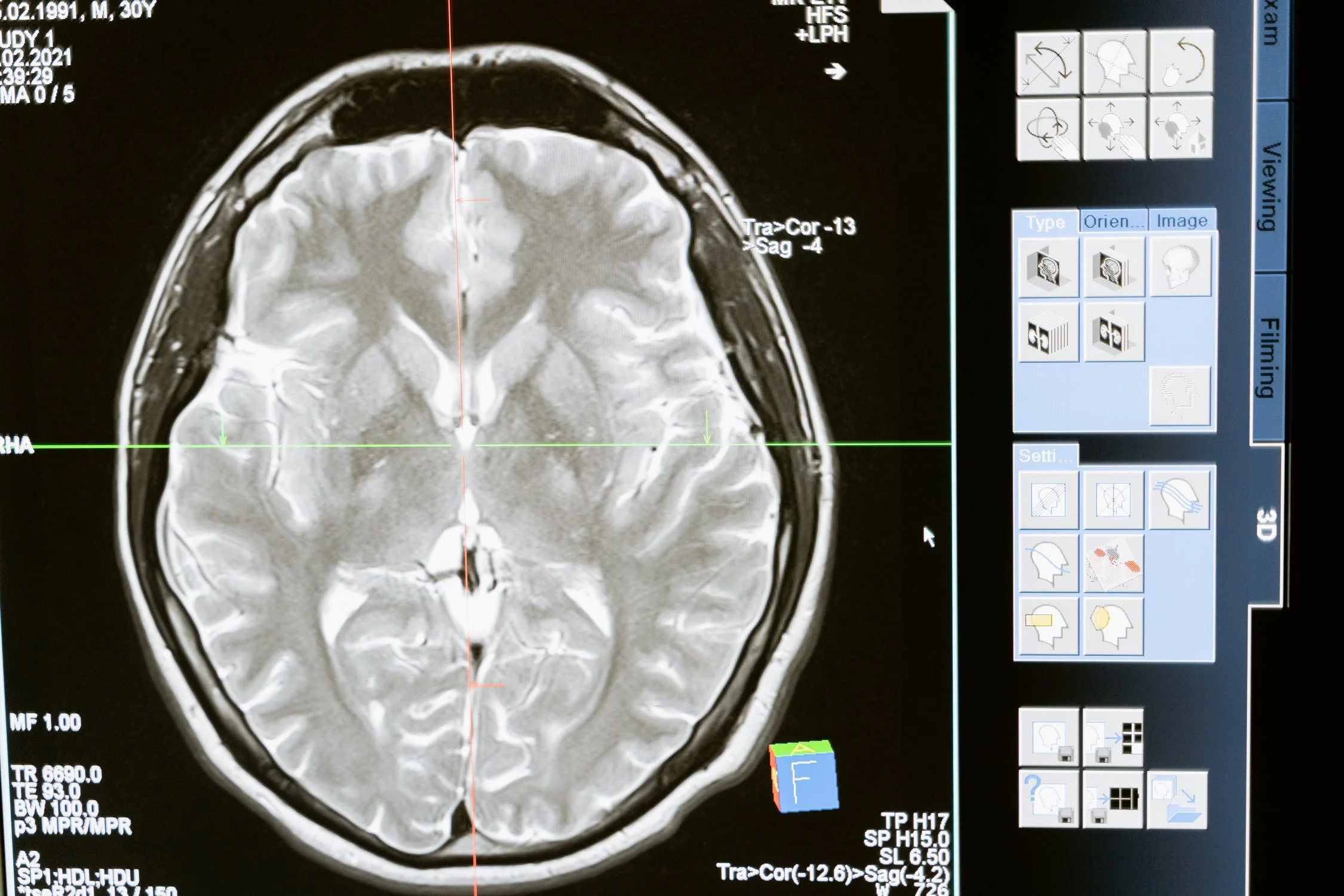
Response: Smell loss is one of the most common symptoms of COVID-19 infection. The mechanism of COVID-19-related smell loss is unclear. Previous studies mainly focused on the effect of the viral infection on the lining of the nasal cavity. We went a step beyond to examine the olfactory bulb, a region that transmits smell-related signals to the brain.
Dr. Cheng-Ying Ho[/caption]
Cheng-Ying Ho, MD, PhD
Associate Professor
Department of Pathology
Johns Hopkins University School of Medicine
MedicalResearch.com: What is the background for this study?
Response: Smell loss is one of the most common symptoms of COVID-19 infection. The mechanism of COVID-19-related smell loss is unclear. Previous studies mainly focused on the effect of the viral infection on the lining of the nasal cavity. We went a step beyond to examine the olfactory bulb, a region that transmits smell-related signals to the brain.
 Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
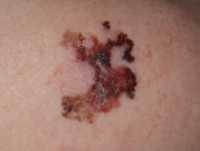
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.
Dr. Ferris[/caption]
Laura Ferris, M.D., Ph.D.
Professor of Dermatology
Director of clinical trials for UPMC Department of Dermatology
University of Pittsburgh School of Medicine
MedicalResearch.com: What is the background for this study?
Response: In this quality initiative at UPMC (a large academic and community health system in Western PA and surrounding areas) Primary Care Physicians were trained to perform annual skin cancer screening examinations of their patients who were aged 35 years and older at routine medical visits.
Over a 5-year period more than 595,000 patients who were eligible to be screened were seen by a UPMC PCP and about 24% of them were screened. We compared the number and thickness (an important indicator of prognosis) of the melanomas diagnosed in those patients who were screened to those who were not screened.



 Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.
Ali M. Fazlollahi[/caption]
Ali M. Fazlollahi, MSc, McGill Medicine Class of 2025
Neurosurgical Simulation and Artificial Intelligence Learning Centre
Department of Neurology and Neurosurgery, Montreal Neurological Institute and Hospital
Faculty of Medicine and Health Sciences
McGill University, Montreal, Canada
MedicalResearch.com: What is the background for this study?
Response: COVID-19 disrupted hands on surgical exposure of medical students and academic centres around the world had to quickly adapt to teaching technical skills remotely. At the same time, advances in artificial intelligence (AI) allowed researchers at the Neurosurgical Simulation and Artificial Intelligence Learning Centre to develop an intelligent tutoring system that evaluates performance and provides high-quality personalized feedback to students. Because this is the first AI system capable of providing surgical instructions in simulation, we sought to evaluate its effectiveness compared with learning from expert human instructors who provided coaching remotely.

 Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
Arman A. Shahriar
Medical Student, University of Minnesota Medical School Research
Consultant, HealthPartners Institute
Minneapolis, Minnesota
 Dr. Wong[/caption]
Susan P. Y. Wong, MD MS
Assistant Professor
Division of Nephrology
University of Washington
VA Puget Sound Health Care System
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Very little is known about the care and outcomes of patients who reach the end stages of kidney disease and do not pursue dialysis. We conducted a systematic review of longitudinal studies on patients with advanced kidney disease who forgo dialysis to determine their long-term outcomes.
We found that many patients survived several years and experienced sustained quality of life until late in the illness course. However, use of acute care services was common and there was a high degree of variability in access to supportive care services near the end of life.
Dr. Wong[/caption]
Susan P. Y. Wong, MD MS
Assistant Professor
Division of Nephrology
University of Washington
VA Puget Sound Health Care System
MedicalResearch.com: What is the background for this study? What are the main findings?
Response: Very little is known about the care and outcomes of patients who reach the end stages of kidney disease and do not pursue dialysis. We conducted a systematic review of longitudinal studies on patients with advanced kidney disease who forgo dialysis to determine their long-term outcomes.
We found that many patients survived several years and experienced sustained quality of life until late in the illness course. However, use of acute care services was common and there was a high degree of variability in access to supportive care services near the end of life.



 Dr. Aris[/caption]
Izzuddin M Aris, PhD
Assistant Professor
Department of Population Medicine, Harvard Medical School
Division of Chronic Disease Research Across the Lifecourse
Harvard Pilgrim Health Care Institute
Boston, MA
MedicalResearch.com: What is the background for this study?
Response: Puberty is a key stage during child development. Previous research indicates that children in the United States are entering puberty at younger ages. These children may be in danger of developing certain diseases, such as type 2 diabetes, later in life. A better understanding of how early life factors affect puberty development is important for combating earlier puberty onset. .
Dr. Aris[/caption]
Izzuddin M Aris, PhD
Assistant Professor
Department of Population Medicine, Harvard Medical School
Division of Chronic Disease Research Across the Lifecourse
Harvard Pilgrim Health Care Institute
Boston, MA
MedicalResearch.com: What is the background for this study?
Response: Puberty is a key stage during child development. Previous research indicates that children in the United States are entering puberty at younger ages. These children may be in danger of developing certain diseases, such as type 2 diabetes, later in life. A better understanding of how early life factors affect puberty development is important for combating earlier puberty onset. .
 Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.
Dr. Kao-Ping Chua[/caption]
Kao-Ping Chua, MD, PhD
Assistant Professor,
Department of Pediatrics
Assistant Professor,
Health Management and Policy
School of Public Health
University of Michigan
MedicalResearch.com: What is the background for this study?
Response: In 2020, most insurers waived the cost of COVID-19 hospitalization for patients. In early 2021, many major insurers started to abandon those waivers. By August 2021, the vast majority of insurers had started billing patients for COVID-19 hospitalizations again.





