Author Interviews, Heart Disease, JAMA, Lipids / 03.07.2024
Lerodalcibep in Patients With or at High Risk of Cardiovascular Disease
MedicalResearch.com Interview with:
[caption id="attachment_62223" align="alignleft" width="150"] Dr. Stein[/caption]
Evan A Stein MD PhD FACC
COO/CSO
LIB Therapeutics
Cincinnati. OH USA 45227
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) remains the main cause of morbidity and mortality worldwide and is increasing in rapidly industrializing countries and is projected to cause more than >20 million deaths annually over the next 15 years. Low-density lipoprotein cholesterol (LDL-C) is well established as a major, easily modifiable, risk factor for CVD. Reductions with statins and, more recently, PCSK9 inhibitors, all agents which directly or indirectly upregulate the LDL receptor and enhance LDL-C clearance, have demonstrated CVD event reductions in cardiovascular outcome trials. Extensive data from these trials, provide a rough estimate that every 40 mg/dL reduction in LDL-C will reduce the risk of major CV cardiovascular events by 22% to 24%. Furthermore, trials with PCSK9 inhibitors added to statins which achieve substantial additional LDL-C reduction show and CVD event reduction remains linear to very low LDL-C levels without signals of adverse events.
Based on this body of evidence, recent revisions to national and international guidelines, now advocate for greater LDL-C reductions and lower LDL-C treatment goals, for patients not achieving these goals on statins alone. The current consensus target goal for LDL-C in patients with CVD, or who are at very-high risk for of CVD, is now less than <55 mg/dL, and <70 mg/dL for those at high risk.
This global trial of over 900 patients with CVD, or at very or high risk for CVD, on maximally tolerated statins assessed the 52-week efficacy and safety of monthly lerodalcibep.
Dr. Stein[/caption]
Evan A Stein MD PhD FACC
COO/CSO
LIB Therapeutics
Cincinnati. OH USA 45227
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) remains the main cause of morbidity and mortality worldwide and is increasing in rapidly industrializing countries and is projected to cause more than >20 million deaths annually over the next 15 years. Low-density lipoprotein cholesterol (LDL-C) is well established as a major, easily modifiable, risk factor for CVD. Reductions with statins and, more recently, PCSK9 inhibitors, all agents which directly or indirectly upregulate the LDL receptor and enhance LDL-C clearance, have demonstrated CVD event reductions in cardiovascular outcome trials. Extensive data from these trials, provide a rough estimate that every 40 mg/dL reduction in LDL-C will reduce the risk of major CV cardiovascular events by 22% to 24%. Furthermore, trials with PCSK9 inhibitors added to statins which achieve substantial additional LDL-C reduction show and CVD event reduction remains linear to very low LDL-C levels without signals of adverse events.
Based on this body of evidence, recent revisions to national and international guidelines, now advocate for greater LDL-C reductions and lower LDL-C treatment goals, for patients not achieving these goals on statins alone. The current consensus target goal for LDL-C in patients with CVD, or who are at very-high risk for of CVD, is now less than <55 mg/dL, and <70 mg/dL for those at high risk.
This global trial of over 900 patients with CVD, or at very or high risk for CVD, on maximally tolerated statins assessed the 52-week efficacy and safety of monthly lerodalcibep.
 Dr. Stein[/caption]
Evan A Stein MD PhD FACC
COO/CSO
LIB Therapeutics
Cincinnati. OH USA 45227
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) remains the main cause of morbidity and mortality worldwide and is increasing in rapidly industrializing countries and is projected to cause more than >20 million deaths annually over the next 15 years. Low-density lipoprotein cholesterol (LDL-C) is well established as a major, easily modifiable, risk factor for CVD. Reductions with statins and, more recently, PCSK9 inhibitors, all agents which directly or indirectly upregulate the LDL receptor and enhance LDL-C clearance, have demonstrated CVD event reductions in cardiovascular outcome trials. Extensive data from these trials, provide a rough estimate that every 40 mg/dL reduction in LDL-C will reduce the risk of major CV cardiovascular events by 22% to 24%. Furthermore, trials with PCSK9 inhibitors added to statins which achieve substantial additional LDL-C reduction show and CVD event reduction remains linear to very low LDL-C levels without signals of adverse events.
Based on this body of evidence, recent revisions to national and international guidelines, now advocate for greater LDL-C reductions and lower LDL-C treatment goals, for patients not achieving these goals on statins alone. The current consensus target goal for LDL-C in patients with CVD, or who are at very-high risk for of CVD, is now less than <55 mg/dL, and <70 mg/dL for those at high risk.
This global trial of over 900 patients with CVD, or at very or high risk for CVD, on maximally tolerated statins assessed the 52-week efficacy and safety of monthly lerodalcibep.
Dr. Stein[/caption]
Evan A Stein MD PhD FACC
COO/CSO
LIB Therapeutics
Cincinnati. OH USA 45227
MedicalResearch.com: What is the background for this study?
Response: Cardiovascular disease (CVD) remains the main cause of morbidity and mortality worldwide and is increasing in rapidly industrializing countries and is projected to cause more than >20 million deaths annually over the next 15 years. Low-density lipoprotein cholesterol (LDL-C) is well established as a major, easily modifiable, risk factor for CVD. Reductions with statins and, more recently, PCSK9 inhibitors, all agents which directly or indirectly upregulate the LDL receptor and enhance LDL-C clearance, have demonstrated CVD event reductions in cardiovascular outcome trials. Extensive data from these trials, provide a rough estimate that every 40 mg/dL reduction in LDL-C will reduce the risk of major CV cardiovascular events by 22% to 24%. Furthermore, trials with PCSK9 inhibitors added to statins which achieve substantial additional LDL-C reduction show and CVD event reduction remains linear to very low LDL-C levels without signals of adverse events.
Based on this body of evidence, recent revisions to national and international guidelines, now advocate for greater LDL-C reductions and lower LDL-C treatment goals, for patients not achieving these goals on statins alone. The current consensus target goal for LDL-C in patients with CVD, or who are at very-high risk for of CVD, is now less than <55 mg/dL, and <70 mg/dL for those at high risk.
This global trial of over 900 patients with CVD, or at very or high risk for CVD, on maximally tolerated statins assessed the 52-week efficacy and safety of monthly lerodalcibep.








 Dr. Guasch-Ferré[/caption]
Marta Guasch-Ferré, PhD
Associate Professor and Deputy Head of Section, Section of Epidemiology
University of Copenhagen
Group Leader, Novo Nordisk Foundation Center for Basic Metabolic Research
Adjunct Associate Professor, Department of Nutrition
Harvard TH Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Olive oil is rich in monounsaturated fats and contains compounds with antioxidant activity that may play a protective role for the brain. Olive oil as part of a Mediterranean diet appears to have a beneficial effect against cognitive decline. Higher olive oil intake was previously associated with a lower risk of cardiovascular disease and mortality. But its association with dementia mortality was unknown.
Dr. Guasch-Ferré[/caption]
Marta Guasch-Ferré, PhD
Associate Professor and Deputy Head of Section, Section of Epidemiology
University of Copenhagen
Group Leader, Novo Nordisk Foundation Center for Basic Metabolic Research
Adjunct Associate Professor, Department of Nutrition
Harvard TH Chan School of Public Health
MedicalResearch.com: What is the background for this study?
Response: Olive oil is rich in monounsaturated fats and contains compounds with antioxidant activity that may play a protective role for the brain. Olive oil as part of a Mediterranean diet appears to have a beneficial effect against cognitive decline. Higher olive oil intake was previously associated with a lower risk of cardiovascular disease and mortality. But its association with dementia mortality was unknown.







 Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist
Dr. Cortese[/caption]
Marianna Cortese, MD, PhD
Senior Research Scientist




 Dr. Di Ciano[/caption]
Patricia Di Ciano, PhD
Dr. Di Ciano[/caption]
Patricia Di Ciano, PhD

 Scott Kaplan PhD
Assistant Professor of Economics
United States Naval Academy
Annapolis, MD 21402
MedicalResearch.com: What is the background for this study?
Response: Sugar-sweetened beverages (colloquially known as SSBs), which include sodas, fruit drinks, sports drinks, energy drinks, and sweetened coffee drinks, are the leading source of added sugars in the American diet, according to the CDC. They are associated with serious negative health outcomes, including type 2 diabetes, obesity, heart disease, kidney disease,
Scott Kaplan PhD
Assistant Professor of Economics
United States Naval Academy
Annapolis, MD 21402
MedicalResearch.com: What is the background for this study?
Response: Sugar-sweetened beverages (colloquially known as SSBs), which include sodas, fruit drinks, sports drinks, energy drinks, and sweetened coffee drinks, are the leading source of added sugars in the American diet, according to the CDC. They are associated with serious negative health outcomes, including type 2 diabetes, obesity, heart disease, kidney disease, 
 Kalli Koukounas[/caption]
Kalli Koukounas, MPH
Kalli Koukounas[/caption]
Kalli Koukounas, MPH


 Dr. Lu Qi[/caption]
Lu Qi, MD, PhD, FAHA
Interim Chair, Department of Epidemiolog
HCA Regents Distinguished Chair and Professor
Tulane University School of Public Health and Tropical Medicine
Director, Tulane University Obesity Research Center
Director, Tulane Personalized Health Institute
New Orleans, LA 70112
MedicalResearch.com: What is the background for this study?
Response: Adding salt to foods is a behavior reflecting long-term preference to salty diets. High sodium intake is a major risk factor for chronic kidney disease.
In our previous studies, we have found that adding salt to foods at the table is related to various disorders including cardiovascular diseases, diabetes, and mortality.
Dr. Lu Qi[/caption]
Lu Qi, MD, PhD, FAHA
Interim Chair, Department of Epidemiolog
HCA Regents Distinguished Chair and Professor
Tulane University School of Public Health and Tropical Medicine
Director, Tulane University Obesity Research Center
Director, Tulane Personalized Health Institute
New Orleans, LA 70112
MedicalResearch.com: What is the background for this study?
Response: Adding salt to foods is a behavior reflecting long-term preference to salty diets. High sodium intake is a major risk factor for chronic kidney disease.
In our previous studies, we have found that adding salt to foods at the table is related to various disorders including cardiovascular diseases, diabetes, and mortality. 
 Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.
Dr. Klompas[/caption]
Michael Klompas MD, MPH, FIDSA, FSHEA
Hospital Epidemiologist
Brigham and Women’s Hospital
Professor of Medicine and Population Medicine
Harvard Medical School and
Harvard Pilgrim Health Care Institute
MedicalResearch.com: What is the background for this study? Can teeth be safely brush in patients who are comatose, intubated or have NG tubes?
Response: Pneumonia is thought to occur when secretions from the mouth get into the lungs. Since there are many microbes in the mouth, there’s a risk that secretions from the mouth that get into the lungs will lead to pneumonia. Toothbrushing may lower this risk by decreasing the quantity of microbes in the mouth.
It is indeed safe and appropriate to brush the teeth of someone who is comatose, intubated, or who has an NG tube. Indeed, our study found that the benefits of toothbrushing were clearest for patients receiving mechanical ventilation.

 Prof. Rong Xu[/caption]
Rong Xu, PhD
Prof. Rong Xu[/caption]
Rong Xu, PhD

 Lisa-Marie Smale, PharmD
Lisa-Marie Smale, PharmD
 Dr. Minneci[/caption]
Peter C. Minneci, MD
Chair of Surgery at Nemours Children’s Health
Delaware Valley
MedicalResearch.com: What is the background for this study? Would you briefly explain the symptoms/course of pilonidal disease?
Response: Pilonidal disease is relatively common and affects up to 1% of the population starting in adolescence and up until young adulthood. Pilonidal disease occurs when cysts or sinuses form between the buttocks. It is believed to be an inflammatory reaction to hair or debris that gets caught in the crease of the buttocks. Risk factors for the condition include a sedentary lifestyle, hygiene and obesity.
[caption id="attachment_61062" align="alignleft" width="150"]
Dr. Minneci[/caption]
Peter C. Minneci, MD
Chair of Surgery at Nemours Children’s Health
Delaware Valley
MedicalResearch.com: What is the background for this study? Would you briefly explain the symptoms/course of pilonidal disease?
Response: Pilonidal disease is relatively common and affects up to 1% of the population starting in adolescence and up until young adulthood. Pilonidal disease occurs when cysts or sinuses form between the buttocks. It is believed to be an inflammatory reaction to hair or debris that gets caught in the crease of the buttocks. Risk factors for the condition include a sedentary lifestyle, hygiene and obesity.
[caption id="attachment_61062" align="alignleft" width="150"]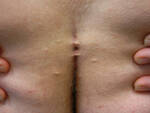 Pilonidal Cyst
Pilonidal Cyst
 Dr. Belloy[/caption]
Michael E. Belloy, PhD
Department of Neurology and Neurological Sciences
Stanford University, Stanford, California
MedicalResearch.com: What is the background for this study?
Response: Apolipoprotein E (APOE)*2 and APOE*4 are, respectively, the strongest protective and risk-increasing, genetic variants for late-onset Alzheimer disease. As such, one’s APOE genotype is highly relevant towards clinical trial design and Alzheimer’s disease research. However, most insights so far are focused on the associations of these APOE genotypes with Alzheimer’s disease risk in non-Hispanic white individuals.
One important aspect of our work is that we really increased sample sizes for non-Hispanic Black, Hispanic, and East Asian individuals, so that we now have better understanding of the associations of APOE genotypes with Alzheimer’s disease risk in these groups. In complement, we also did the largest investigation to date on the role of ancestry on the associations of APOE genotypes with Alzheimer’s disease risk. The scale of our study was thus a critical factor in generating novel insights.
Dr. Belloy[/caption]
Michael E. Belloy, PhD
Department of Neurology and Neurological Sciences
Stanford University, Stanford, California
MedicalResearch.com: What is the background for this study?
Response: Apolipoprotein E (APOE)*2 and APOE*4 are, respectively, the strongest protective and risk-increasing, genetic variants for late-onset Alzheimer disease. As such, one’s APOE genotype is highly relevant towards clinical trial design and Alzheimer’s disease research. However, most insights so far are focused on the associations of these APOE genotypes with Alzheimer’s disease risk in non-Hispanic white individuals.
One important aspect of our work is that we really increased sample sizes for non-Hispanic Black, Hispanic, and East Asian individuals, so that we now have better understanding of the associations of APOE genotypes with Alzheimer’s disease risk in these groups. In complement, we also did the largest investigation to date on the role of ancestry on the associations of APOE genotypes with Alzheimer’s disease risk. The scale of our study was thus a critical factor in generating novel insights.
